Donation and transplantation: plan 2021 to 2026
The Plan sets out our priorities for increasing organ and tissue donation and transplantation over the next five years.
Priority Three – Reducing Missed Opportunities for Deceased Donation
We want to continue to ensure that, wherever possible, anyone who would have wanted to donate can have that decision respected when they die.
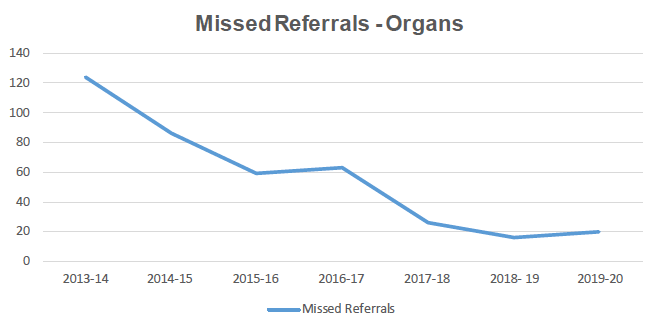
Chart 6
Missed Referrals – Tissue
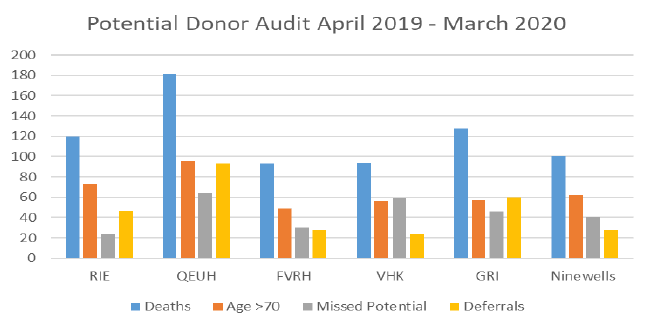
The chart above sets out data on potential donors and missed referrals (in grey) at six main tissue-donating hospitals: the Royal Infirmary of Edinburgh, the Queen Elizabeth University Hospital, Forth Valley Royal Hospital, Victoria Hospital Kirkcaldy, Glasgow Royal Infirmary and Ninewells hospital. Of the 716 patient deaths audited across the five hospitals, 263 patients (36.7%) were considered to be missed potential donors with no documented consideration regarding donation.
Good progress has already been made in reducing missed referrals of potential organ donors, but there is a need to continue working with NHS Boards and their Organ Donation Committees to ensure there are no missed opportunities for either organ or tissue donation. Organ Donation Committees are required to prepare an action plan annually, focussed on any identified areas for improvement, so this should include avoiding missed referrals where this has been an issue. We also need to avoid opportunities for eye donation being missed due to a lack of available retrieval staff; the Scottish National Blood Transfusion Service (SNBTS) is just starting to deliver the eye retrieval service across the central belt, which should enable an increase in eye donation. NHSBT is also continuing to make progress in ensuring that a Specialist Requester or SNOD is always involved in approaches to family members about donation.
It will also be important to ensure that, in line with the opt-out legislation, decisions on whether donation is authorised focus on the decisions made by the potential donor – whether that was to opt in by joining the Organ Donor Register (ODR), to opt out or to do nothing (which, as is being highlighted to households, will also be treated as a decision to opt in in most cases). We anticipate that the new Specialist Requesters who have now started leading approaches to families about organ donation in almost all cases will help to increase authorisation rates in Scotland and to reduce the number of occasions where a potential donor's authorisation decision is overridden by their family.
Authorisation for Organ Donation
3.1 It is anticipated that using the Specialist Requester model will help ensure the best possible chance of delivering improvements in authorisation rates through the introduction of deemed authorisation. As the diagram on page 18 shows, only a small proportion of people die in circumstances where they could donate organs; it is therefore important to ensure as many of these potential donors as possible can proceed if the individual supported donation.
Previously all Specialist Nurses for Organ Donation (SNODs) in Scotland would approach families about the potential of donation, together with hospital staff, as well as taking forward all other parts of the donation process where donation is authorised. It is important to ensure Specialist Requesters (SR) or SNODs are involved in approaches to families as authorisation is much less likely to be given if a SNOD is not involved in the approach. For example, in 2019-20, organ donation was authorised in 71.4% of cases where a SNOD or SR was involved, but in 0% of the cases where no SNOD or SR was present. Using the SR model, a small group of six Specialist Requesters in Scotland will consistently be responsible for leading discussions with family members about donation. These discussions are very sensitive and challenging as they happen at a time when family members have only recently discovered that their relative has died or is about to die. SNODs will still be involved, but will usually take over from the Specialist Requester at the point where it is clear that donation has been authorised.
We will also monitor progress in reducing the number of cases where family members refuse to allow donation to proceed even though their loved one had opted in to donate via the ODR to establish whether Specialist Requesters help reduce these cases by encouraging families to support their family member's decision.
NHSBT is trialling the Specialist Requester model in partnership with the Scottish Government for three years. After the initial three year period, progress will be evaluated to assess the effectiveness of using Specialist Requesters in increasing authorisation rates in Scotland. In a number of regions of England, evidence suggests that using Specialist Requesters, particularly where those requesters are experienced and approach families regularly, does increase authorisation rates. If authorisation rates have not increased, further work will be carried out with NHSBT and SDTG to consider what more can be learned from other nations or regions on improving authorisation rates.
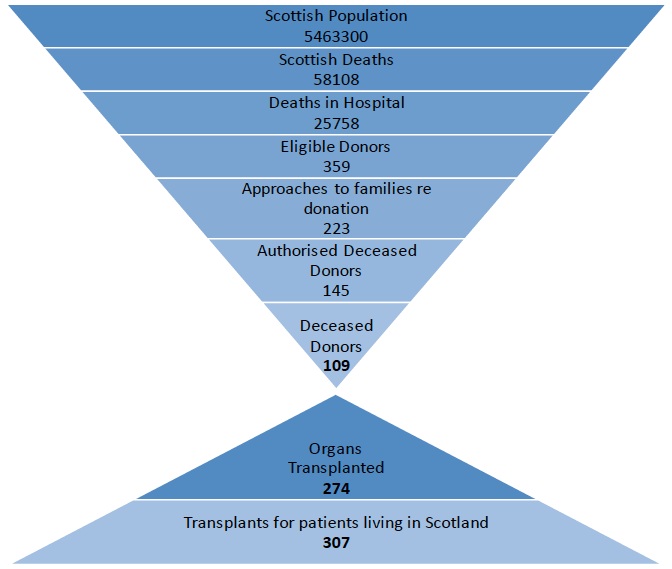
Data from National Records of Scotland, Public Health Scotland and NHSBT. Note – organs transplanted data is based on numbers of transplants from organs donated in Scottish hospitals.
Tissue and Eye Donation
3.2 Both through the introduction of opt out and on a continuing basis, we will support SNBTS to reduce missed opportunities for tissue donation by increasing NHS staff awareness across hospitals and hospices by raising awareness and reminding NHS staff of the importance of considering the potential of tissue donation for all deaths. There will be work carried out with hospitals, hospices and Organ Donation Committees to embed referral of potential tissue donors as part of standard end of life care. Staff in key hospitals will be issued with Tissue Donation cards to attach to a lanyard to help remind them when and how potential donors can be referred. We plan to monitor tissue referral rates and reasons for tissue donation not being authorised to try to consider if there are any further steps which should be taken to increase donation.
In 2019-20, 36% of families approached about tissue donation were not willing to speak to a tissue donor coordinator (TDC); work will therefore be progressed, particularly through the implementation of deemed authorisation, to look at whether there are ways to reduce the proportion of families who decline to discuss donation. The great majority of the families who do agree to speak to a TDC are content for donation to proceed.
Unfortunately eye donation in Scotland has declined in recent years, although there has been no significant decline in demand for cornea transplants. For example, in 2019/20 there were 281 cornea transplants carried out on patients living in Scotland, but only 46 donors in Scotland donated their eyes in that year. We believe that part of the shortfall is due to a lack of suitably trained retrieval staff being available to carry out the retrieval within 24 hours of the patient's death. It is important to ensure a robust eye retrieval service is in place and will work with SNBTS and NHSBT to monitor progress with the aim of ultimately ensuring that there are enough eye donors in Scotland to meet the demand for cornea transplants for patients in Scotland. In addition, to support this work, we aim to work with NHSBT to improve the data available on referrals and the reason why eye donation does not proceed following a referral.
Having better data will help identify key areas for improvement. We will therefore consider further how best to optimise levels of eye donation in Scotland and continue to promote public awareness about the importance of eye donation. While it is likely that reducing missed referrals and improvements in the retrieval service should increase eye donation in Scotland, SNBTS will work with a number of hospices to enable some of those who die out of hospital also to have the opportunity to donate their eyes.
| Key Recommendations | Short term 1 – 2 years Medium term 3 – 5 years | Lead | |
|---|---|---|---|
| 1 | Ensure use of Specialist Requesters to approach families about organ donation in all donating hospitals to help improve authorisation and reduce overrides where the patient was on the ODR. | Short term – implementation already started | NHSBT |
| 2 | Monitor and review use of Specialist Requester model | Medium term | NHSBT and Scottish Government |
| 3 | Via opt out implementation and longer term, increase awareness raising among NHS staff about referring potential tissue donors. | Short to medium term (likely to be ongoing) | SNBTS and Scottish Government |
| 4 | Ensure a robust eye retrieval service for Scotland is in place and continue to monitor and review progress on increasing eye donation. | Short term - for the retrieval service Medium term - for monitoring and reviewing progress in increasing donation | SNBTS and NHSBT |