Donation and transplantation: plan 2021 to 2026
The Plan sets out our priorities for increasing organ and tissue donation and transplantation over the next five years.
Priority Two – Increasing Organ Transplantation
We want to continue to increase the number of transplants for Scottish patients, reduce waiting times and provide the best possible outcomes for patients.
We aim to support the use of novel technologies and closer joint working between transplant units to increase organ utilisation. We also need transplant units to continue working with all NHS Boards to increase equity of access to transplantation across Scotland, making sure that organ failure is diagnosed early wherever possible and that factors such as where someone lives doesn't affect their chances of being referred for a transplant.
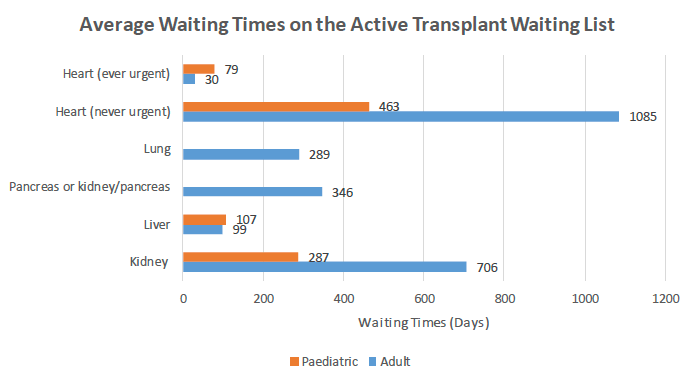
Note - data above provides median waiting times in days on the active transplant waiting list – registration periods vary by organ. For 'ever urgent' hearts, data is for the time the patient was on the urgent waiting list only. Data from NHSBT Transplant Activity Report for 2018-19[4].
As Chart 4 above shows, average waiting times vary significantly by organ and waiting times will also vary depending on how urgently they need a transplant. In many cases, waiting times are still too long and patients risk significant deterioration in their health and even death while they wait. In addition, some groups, such as people from black and minority ethnic communities, tend to wait longer than average as their best chance of a good organ match generally comes from a donor of the same ethnicity.
The new opt-out systems of deemed authorisation (or consent) in both Scotland and England are expected to increase the number of deceased organ donors over the coming years. This provides a real opportunity as more organs are expected to be offered to Scottish transplant units. Therefore, it is important that units are able to make use of all of those organs which are considered suitable for transplant.
While transplant units do receive a lot of organ offers, the majority of these organs are not able to be transplanted. However, the great majority of organs that are declined are not transplanted by any other transplant unit. There are a range of reasons why organs are not accepted by a centre (and in many cases, there may are a combination of reasons, rather than just one factor). However, the most common reasons recorded relate to concerns about the donor or the organ/its function; this could include factors such as the donor's age, BMI or past medical history or evidence from tests (such as X-rays), suggesting the organ does not have good function levels. While many of these factors may always rule out certain donors from ever being suitable to donate particular organs, novel technologies in particular offer the opportunity to allow transplant units to use more 'marginal' organs that may currently need to be declined.
SDTG will continue to monitor reasons for organs being declined and, in particular, consider with units where organs have had to be declined for logistical reasons. Data suggests that relatively small numbers of organs are declined due to hospital issues, such as no beds or operating theatre being available. However, in 60 cases in 2019, records suggest organs had to be declined primarily because the transplant unit was already retrieving or transplanting organs at the same time. As well as needing to consider units' capacity as part of National Services Division's future commissioning planning, this also highlights the potential for machine perfusion technologies to help reduce the need for those organs to be declined in future by allowing a longer time period between the retrieval and when the organ needs to be transplanted.
Increasing the number of viable organs for transplantation and improving transplant outcomes
2.1 We will support the commitments in the UK Strategy to continue to promote developments in perfusion technology and to implement these when there is evidence to support them being sufficiently safe and effective. The Scottish Government has already committed to funding its share of costs of a full UK roll out of use of Normothermic Regional Perfusion (NRP) for abdominal organ retrievals for all donors donating after circulatory death (DCD donors). There is evidence from liver retrievals in particular that using NRP both improves the quality of the organ, thereby reducing the risk of graft failure or complications post-transplant. NRP also increases the number of organs which are transplanted as organs which units would otherwise decline as being too risky can go through a period of assessment. We will work with NHSBT and the other UK governments to try to ensure the use of NRP can be more widely used as soon as practicable.
We will also monitor the progress of the current three year initiative funded by NHSBT and NHS England to enable the retrieval of more hearts from DCD donors. If this is effective in increasing heart transplant access for Scottish patients, we will consider with NHSBT and the other UK governments the potential for a longer term roll out of a DCD heart donation programme. Alongside this, the impact of retrieving hearts from DCD donors for potential solid heart transplant on the availability of heart valves in Scotland will also be monitored. At the present time, it is considered unlikely that there will be a significant impact on heart valve donation numbers as we expect that only a small proportion of DCD donors will be suitable heart donors (Priority Three sets out other actions to help increase the numbers of heart valves donated).

Picture of NRP machinery – courtesy of NHS Lothian
Alongside similar work in the UK Strategy, we will support work to increase the use of ex-vivo Normothermic Machine Perfusion (NMP) which allows organs to be perfused after they have been removed from the donor and kept oxygenated for longer before transplant. We will consider with transplant units and National Services Division (NSD) the feasibility of an organ reconditioning hub for Scotland (known as an Assessment and Recovery Centre or ARC) to centralise abdominal ex-vivo organ perfusion services. An ARC would hopefully help increase the number of transplantable organs and enable units to stagger the timing of their transplants better. Subject to the outcomes of the feasibility study, in due course, a proposal to trial reconditioning of livers at the Scottish National Blood Transfusion Service's (SNBTS) headquarters will be considered. If successful, this ARC could also be used for the management of kidneys, pancreata and lungs in due course. This work is still at a fairly early stage, but it would have the potential to provide a service for a number of transplant units. SNBTS has already developed expertise in the field of Advanced Therapy Medicinal Products (ATMPs) and may be able to use this expertise in the future to use cell and gene therapy to help regenerate organs for transplantation.
Work to ensure a sustainable, patient-centred transplant service in Scotland
2.2 National Services Division's (NSD's) future commissioning plans will look at ensuring transplant units have the capacity to deliver the anticipated gradually increasing numbers of transplants over the coming five years. SDTG will continue to work with NHSBT to monitor organ utilisation in Scotland and in particular the reasons for any organs being declined due to lack of capacity. We will support the UK Strategy in continuing to monitor and discuss with units any significant variations in practice on organ utilisation (where these are not explained by some units using novel technologies) to try to encourage good practice.
To support this, we propose that NSD should work with the transplant units to explore options for the sharing of services and resources and increased collaboration between Scottish units. Work to explore increased collaboration has already begun between the Edinburgh and Glasgow adult renal units. This could also help ensure transplant units learn from one another's experiences and potentially support each other to ensure equity of access to transplant services across Scotland.
With the potential increase in the number of viable organs for transplantation, the Scottish Government and NSD also need to support transplant units and the British Transplantation Society in their work to ensure sufficient and sustainable staffing levels in future. In addition, we also need to work with NHS Boards to ensure appropriate, secure IT is in place to allow both transplant units and referring clinicians to be able to access and share patient information more easily. This can be an issue for both adult and paediatric services. While clinicians can access patient records for patients living in their own NHS Board area, it is often more difficult, particularly out of hours, to get the necessary access to records of patients living in other Board areas.
Ensure that all patients likely to benefit from transplantation are offered the opportunity
2.3 We will seek to increase equity of access to transplantation services across Scotland by reviewing current and projected need for referral to transplant units, in particular looking at any significant variations in referral rates between NHS Boards. Transplant units in partnership with NHS Boards will be asked to continue to increase awareness of transplant services with referring clinicians across Scotland, particularly focussing on any areas with referral rates significantly below the Scottish average. Clinicians and NHS Boards should be encouraged to ensure they proactively identify and discuss transplantation with any patient who may be eligible for and benefit from a transplant. We will explore the potential for developing a network of clinicians who can support improvements within Boards and ensure key staff are kept up to date with developments in the field of transplant.
| Key Recommendations | Short term 1 – 2 years Medium term 3 – 5 years | Lead | |
|---|---|---|---|
| 1 | Increase the number of viable organs for transplantation by using novel technologies, such as rolling out use of machine perfusion. Subject to the findings of initial feasibility work, consider moving ahead with development of a Scottish Assessment and Recovery Centre. | Medium term | NHS Lothian/ SNBTS, NHSBT and Scottish Government |
| 2 | Work to ensure sustainable, patient-centred transplant services, including exploring options for increased shared services between renal units, in particular to avoid the need for patients to miss out on any suitable organs offered for them. | Short to medium term | NSD and Transplant Units |
| 3 | Raise awareness among relevant staff across NHS Boards to seek to ensure all those patients who would be likely to benefit from a transplant are offered the opportunity. | Short term | Transplant Units, NHS Boards, supported by SDTG |