Delivering value based health and care: a vision for Scotland
Sets out the challenges our system is facing and how practising Realistic Medicine can deliver a more sustainable system. It includes six commitments on what we’ll do to support health and care professionals deliver care that people value.
3. Realistic Medicine and Value Based Health & Care
It is by practising Realistic Medicine that we will deliver Value Based Health & Care.
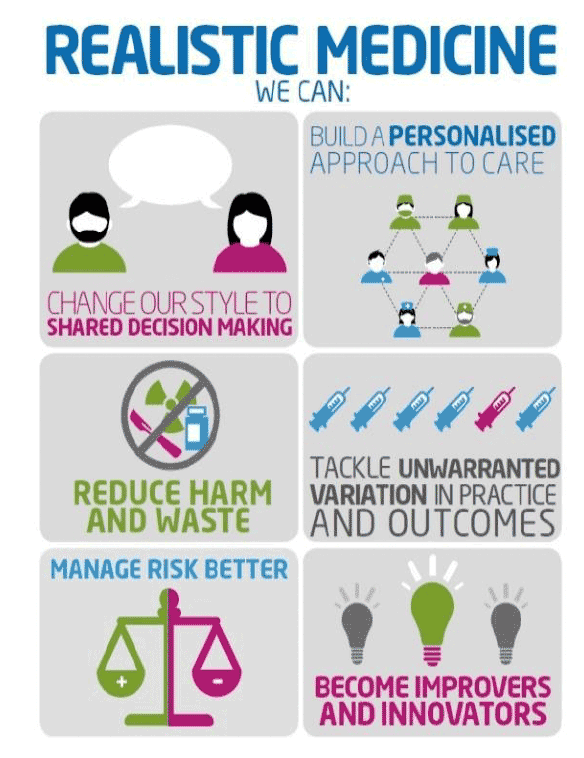
The principles of Realistic Medicine have gained widespread acceptance across Scotland, however there is more to do to achieve its objectives, and help relieve some of the pressures our system is experiencing.
The six tenets outline how we can change the way we deliver health and care in Scotland. By practising Realistic Medicine, we can deliver care and treatment that people value as well as reduce inappropriate care.
Evidence shows that if people are fully informed about the risks and benefits of their treatment options they choose less treatment, or more conservative treatment.
That is why shared decision making sits at the heart of Realistic Medicine. It supports people, and their families, to feel empowered to discuss and consider their treatment options and the associated risks and benefits. This approach can help manage expectations and enables people to make informed choices, based on what matters most to them. In some cases, this may mean they choose different treatments, which offer greater personal value. In other cases, they may choose less or no treatment, which will help reduce wasted resources
Understanding people's preferences does not mean that we always give people what they want, because we know that there are times when it may not be appropriate or practical for us to do so. But we should always consider what matters to them and try to better understand how their health and wellbeing fits into the broader context of their lives.
Realistic Medicine also aims to reduce harm, waste and unwarranted variation, while acknowledging and managing the inherent risks associated with all health and care, and championing innovation and improvement. These principles are essential to delivering a sustainable VBH&C system for the future.
By practising Realistic Medicine, we will deliver Value Based Health & Care, and support a more sustainable health and care system.
That is why we will continue to support health and care colleagues by continuing to provide the tools and learning resources they need to practise Realistic Medicine. In doing so, we will also foster a culture of stewardship across our health and care system where delivery of VBH&C is the norm.
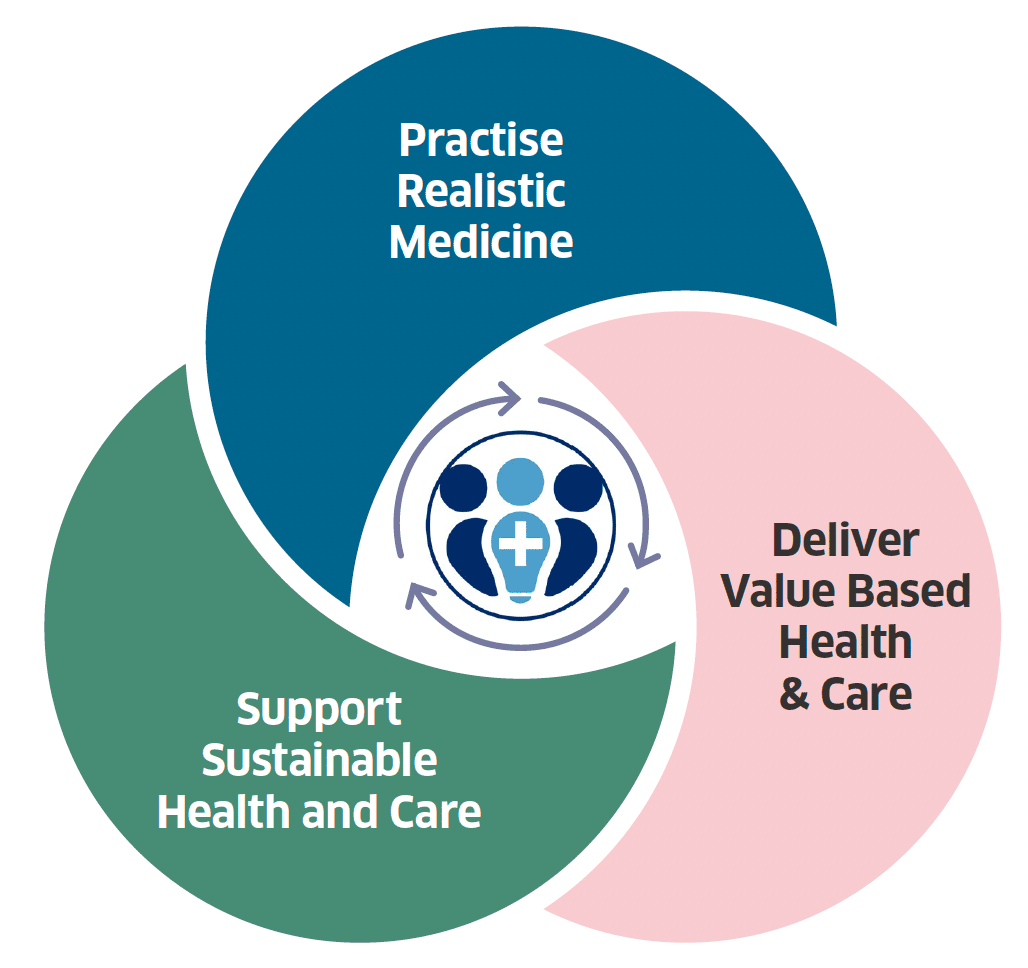
Graphic text below:
Practise Realistic Medicine
Deliver Value Based Health & Care
Support Sustainable Health and Care
What does value mean?
Value can mean different things in different contexts. It is helpful to consider how we as health and care professionals can deliver value, not only for the people we care for, but for our services and society. When we talk about value in health and care, we generally mean achieving the best outcomes at the lowest possible cost.
The European Commission describes four pillars of value upon which VBH&C is built. In practice, value is often achieved across one or more of these pillars, and by assessing the value of an intervention at individual, population and societal levels, we can help to direct resources to where they will deliver the best outcomes.
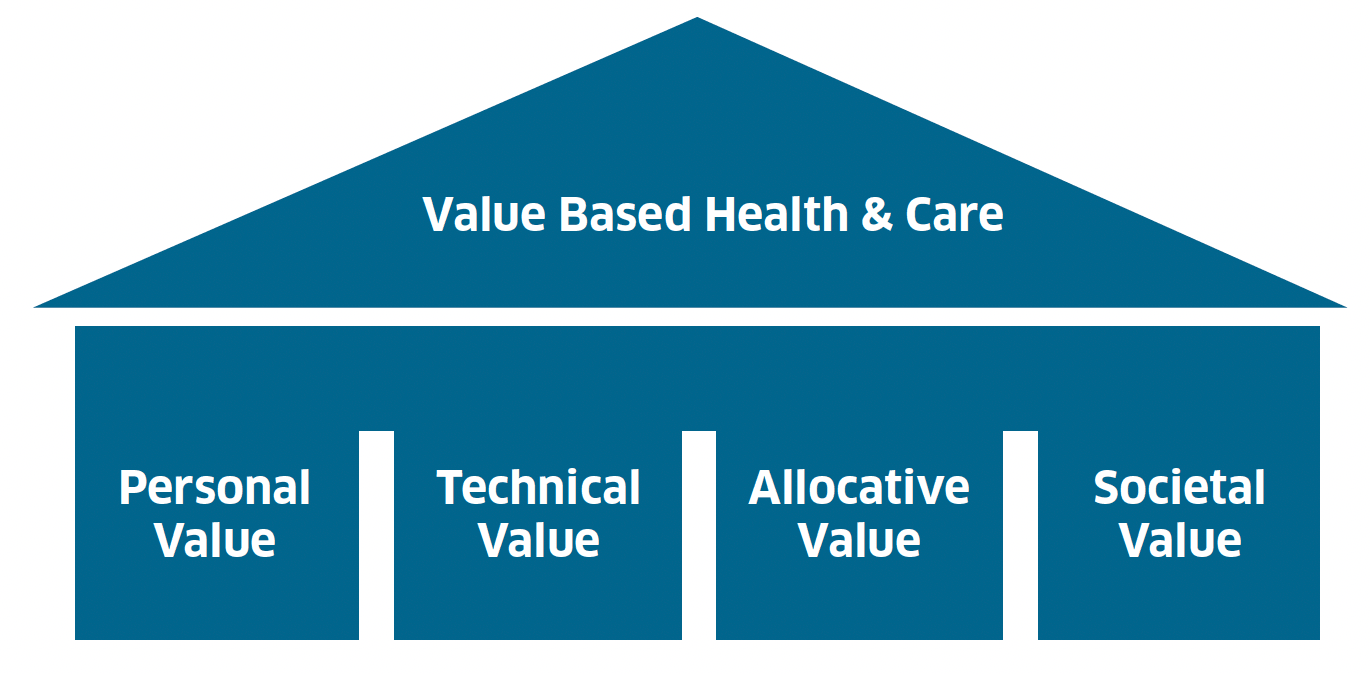
Graphic text below:
Value Based Health & Care
- Personal Value
- Technical Value
- Allocative Value
- Societal Value
Personal value is delivered when the outcome of care for people meets their personal goals. Personal value means people and families are involved in decisions about their care by health and care professionals who understand and respect what matters to them. It is delivered through shared decision making and discussion about the potential benefits and harms of different treatment options, including the option to do nothing. This approach allows people to make an informed choice about the care options that are right for them.
We know if people are fully informed and involved in decisions about their care, they choose less treatment, or consider a more conservative approach. They are also far more likely to value the treatment they choose, and this reduces waste and potential harm. Delivering personal value informs appropriate use of available resources while delivering care that really matters to people.
What matters most
The following case study is an example of delivering personal value:
Case Study: Spending precious time at home
When Robert, a young and newly married man, developed worsening symptoms of heart failure, the team in Forth Valley were ready to offer their care and support. Breathlessness was a problem, especially at night, and the heart failure team helped the young couple to receive a grant from a third sector organisation to buy a specialist bed offering better comfort for Robert.
Frequent admissions to hospital for intravenous therapy were required, at which point Robert asked if he could have his therapy through the day and go home to his own bed at night. Recognising this was what mattered to Robert, the team undertook to develop a new treatment protocol and to deliver the treatment required on a day-case basis, enabling Robert to spend more precious time at home. We were able to time treatment to suit Robert and his wife Donna, including ensuring Robert made as many of his team's football matches as he could.
Listening to what mattered to Robert informed the development and delivery of a service which has now been running for 10 years, reducing length of hospital stay, promoting admission avoidance, and enabling many other patients to spend more precious time at home.
Allocative (or population) value looks at how we distribute resources across our population. Distribution of resources should be equitable and transparent, so that different health conditions, for example, cancer and musculoskeletal problems, are resourced appropriately and fairly according to the needs of the population. When considering allocative value, we must ensure we distribute resources across the pathway of care, including prevention. In this way, allocative value seeks to avoid inequity by disease or need.
The following case study provides an example of allocative value:
Case Study: Tonsillectomy in NHS Grampian
The problem
In work carried out as part of the precursor to the Atlas of Unwarranted Variation, ISD (now PHS) published data suggesting NHS Grampian was an outlier in tonsillectomy, performing more surgeries than other NHS Boards. NHS Grampian reviewed the data locally. Their practice appeared to conform to SIGN guidelines and at first glance, there was no clear reason why NHS Grampian had high rates of tonsillectomy.
What happened next
NHS Grampian were keen to understand how they could address this high rate of tonsillectomy. Were they performing too many tonsillectomy procedures or were other NHS Boards performing too few?
They consulted with the ENT Scotland group. Initial thoughts were that demographics had an impact but the was no association with deprivation and tonsillectomy rates. They wondered whether the vetting process and GP awareness of SIGN guidelines might be a factor. Working with GPs, NHS Grampian sought to standardise their process by revisiting guidelines and introducing advanced clinical referral triage with one ENT consultant. They also worked to develop a patient decision-aid and participated in national research into tonsillectomy versus conservative treatment.
Results
NHS Grampian now has more robust standardised referral and vetting process.
NHS Grampian now has one of the lowest rates of tonsillectomy in Scotland.
PHS went on to develop an Atlas of Variation for tonsillectomy and using this data the ENT surgical community in Scotland have concluded that tonsillectomy should not be offered for the treatment of tonsil stones alone. This reduces the harm and waste from unnecessary surgeries.
Technical value considers how well our resources are invested for a particular subgroup of the population, defined by a specific care need or health condition. Technical value requires a close match between the needs of service users and the provision of service. Where there is overuse of a treatment or service, we are not providing value since people do not benefit from care they do not need and may be exposed to harm.
We are also concerned with underuse, where treatments and services which would be beneficial are not used. Equity of access is required for good technical value, where all of the people living with a condition and who will benefit have access to appropriate care and treatment. The Scottish Atlas of Healthcare Variation considers unwarranted variation and helps us to examine potential areas of overuse or underuse of services. It creates an opportunity for NHS Boards to review current policy and practices to identify better value treatment options. A refreshed version of the Scottish Atlas of Healthcare Variation has been published.
Here is an example of providing technical value:
Case Study: The Care Home Continence Improvement Project
The Care Home Continence Improvement project, developed by NHS National Procurement has improved outcomes and delivers better value for not only patients but also the wider health and social care system.
National Procurement developed the Care Home Continence Improvement project in partnership with NHS Lanarkshire after noticing a year-on-year rise in the purchasing of incontinence products. They started digging deeper to look at how the various products in selected care homes were being used. They found that care home staff were confused about which products to use and there was no systematic approach to choosing the right one.
The project found that by introducing a bundle of care (from the available evidence) they could reduce harm in the care homes. They incorporated improvements, for example, steps like encouraging people to drink, which had seemed like a 'risk' to effectively managing incontinence and were understandably challenging for care workers, at first. However, when they delivered this step alongside the other improvements, the NHS Lanarkshire team found there were fewer episodes of incontinence.
Over a year, the project was able to promote continence in care home residents, improve patient safety and reduce patient distress. The pilot care homes also saw a significant reduction in falls, skin damage and hospital admissions for falls and urinary tract infections. In the projects first year product usage and waste were reduced, contributing to £250,000 of savings for the NHS.
In addition, because there were so many fewer accidents, frontline staff were able to spend more time on higher value activities like talking to patients and delivering personalised care. The latter was also delivered by the fact that carers were able to ensure they were choosing the right product to meet the needs of the individual.
The success of this project has been widely recognised with the team winning a number of awards since completion of the pilot project.
Societal value takes account of the wider impact of health and care services on society. These can be very positive, for example, health and care services can support local communities by providing opportunities for employment and promoting social cohesion. On the other hand, our health and care services also have an impact on the environment – the NHS is a major contributor to climate change through its greenhouse gas emissions. For this reason, our vision for VBH&C is closely aligned with the NHS Scotland climate emergency and sustainability strategy: 2022-2026 which seeks to improve societal value through the delivery of sustainable care.
The prescription of a medicine is the most common intervention in the NHS and the use of medicines and chemicals account for 20% of the carbon footprint of the NHS in England, yet up to 50% medicines are either not taken correctly or not taken at all. A VBH&C approach to over-prescribing and inappropriate prescribing, using shared decision making and outcomes which matter to patients, can reduce waste and harm associated with medicines and reduce the impact of the NHS on the environment.
Enhancing value usually requires a multi-faceted and multi-professional approach and may necessitate working with organisations not traditionally associated with health and care. This case study from Deep End Practices exemplifies this approach.
The following case study is an example of how societal value can be delivered:
Case Study: Deep end project
Setting the scene
John is a 33-year-old man who lives with his pregnant partner, Julie, and three young children. John was brought up in foster care from the age of five years, left school at 16 years with no formal qualifications and spent time in prison for drug-related offences. He now lives with his family in a small flat and is registered at one of Scotland's Deep End GP practices. He is in financial difficulty and struggling with basic essentials. John has had poor mental health for most of his life exacerbated by drug and alcohol use. He has been diagnosed with diabetes which is poorly controlled with frequently missed appointments.
John presents at reception of his general practice, as he has no credit on his phone. He appears angry and frustrated. One of the receptionists finds a private space and establishes he is struggling with his mental health. She books him in for a face-to-face GP appointment.
Interventions of value
John shares that he has been feeling depressed and suicidal at times. He's worried about his diabetes. Previous hospital clinic appointment letters did not arrive, and he was removed from the waiting list. His financial stresses are a significant concern and he's drinking more.
His GP makes a plan to become John's 'named' GP with planned appointments. She refers him to their Community Links Worker, who involves him with a local volunteering project, and their Welfare Advisor, who helps John with debt and benefits advice. He is also referred to the Primary Care Alcohol Nurse, for support with his low mood and alcohol use. Adopting the learning from the Govan SHIP project, John and his family are discussed at the Practice multi-disciplinary team (MDT) meeting and they agree about how they might best support the family. For continuity and consistency between MDT members, out-of-hours GP and A&E services, John consents to a 'key information summary' care plan electronically sharing details of his main problems and 'what matters to him'. John agrees to a social work referral for additional support. The diabetes clinic receives an 'alert' referral highlighting John's vulnerability and risk of non-attendance which asks the clinic to inform the Practice and link worker of appointment details so they can support his attendance.
Outcomes of importance
Over the following months with planned, longer appointments, a relationship of trust and understanding builds between John and his GP. He feels more able to accept, and engage with, his care. This enables his self-caring ability and appointment attendance. Low mood and anger management issues improve, and his alcohol intake reduces with support from his alcohol nurses. His financial stresses ease with assistance from his welfare advisor. Family energy costs and rent are supported with access to the correct benefits. He is able to attend his hospital diabetes clinic aided by the community link worker who joined his first appointment and helped him arrange transport for subsequent appointments.
Culture of Stewardship
A culture of stewardship is one which recognises and prioritises the importance of best use of our health and care resources, which not only includes equipment, diagnostics and treatment, but also our health and care colleagues' skills and time. If we can work across specialties with the people we care for, using Evidence Based Practice, we can guide people to make informed choices about the treatment and care that is right for them. By doing so, we provide care that really matters to people, optimise value, minimise waste and tackle inequity by supporting those who need our help the most.
Creating a working environment in which a culture of stewardship can flourish is vital if we wish to deliver more sustainable care as well as help tackle the climate emergency.
VBH&C encourages and supports health and care colleagues to take responsibility and be accountable for increasing value in health and care. This requires working in partnership with people, communities and health and care systems to disinvest from low value care and focus on high value care. VBH&C seeks to foster and promote a culture of stewardship across health and care.
Value Based Health & Care in practice
The following case studies show how the aspects of VBH&C that we have outlined can be put into practice to deliver better outcomes for the people we care for, provide greater equity of care and a more sustainable system.
Case Study : Use of Patient Reported Outcome Measures (PROMS) in polypharmacy medication reviews
The care of patients with multi-morbidity (multiple medical conditions) is one of the greatest challenges now faced by the health service, as it can create overly complex health care for some of the most vulnerable in society. The vast majority of medical research, guidelines and contractual agreements have focussed on single targets for single disease states, whereas in reality most patients have multi-morbidities, requiring multiple treatments.
The resulting polypharmacy (use of multiple medicines) can be appropriate or inappropriate and the key healthcare aim for the individual patient is to ensure the safe and effective use of their multiple medicines.
Polypharmacy becomes inappropriate when the medication risks begin to outweigh the benefits for an individual. The National Polypharmacy Guidance aims to address this by helping to identify people at greatest risk of harm, and to agree a medication regimen that is tailored to their changing needs and expectations.
PROMS questionnaire
To support implementation of the polypharmacy guidance, the Scottish Government Effective Prescribing and Therapeutics Division has worked with the Digital Health & Care Innovation Centre to use the national decision support platform – the Right Decision Service – and the expertise of knowledge services staff to deliver a national web and mobile decision support app for polypharmacy. The "Questions for my Review" section within the patient and carer toolkit in the polypharmacy app comprises two sets of questions, designed through research and consultation to gather Patient Reported Outcome Measures before and after medicines review.
The questionnaires can be completed in various ways including directly via patient to healthcare professional, in collaboration by a patient and carer, healthcare professional asking the patient the questions and filling in the answers on their behalf or non-clinically trained staff (e.g. community connectors, link workers, care home and care at home workers), supporting the patient to complete the questionnaires.
The completed questionnaires are emailed to the healthcare professional as a record and to provide a person centred focus for shared decision making within the medicines review.
Outcomes
This work aims to develop an optimal, sustainable and scalable approach to use of medications for people with multiple morbidity. A key aspect of the study is enabling patients to live healthy and active lives by supporting them and their healthcare professionals to define goals for medicines treatment that reflect the outcomes that matter to them.
Case Study : NHS Lanarkshire Health Promotion Health Service (HPHS).
NHS Lanarkshire's Realistic Medicine team recognised the opportunity to align with Health Promoting Health Service (HPHS). HPHS adopts a personalised approach to care by utilising a Holistic Needs Assessment (HNA) encouraging patients and staff to discuss what matters most to them, what support or guidance they require and how best they can be supported to maintain their health and wellbeing.
In one case, a patient with frequent admissions for falls underwent multiple CT scans, yet no diagnosis as to the cause of the falls was found. The potential of wider underlying issues being the cause prompted referral to the Health Improvement Senior (HIS) for HPHS.
Using a person centred conversation and personalised approach to care using the HNA, the patient disclosed aspects of their home-life and health anxieties. The HNA was used to understand where those issues were in relation to home-life, what mattered most to the person and how these could be supported. External supports were put in place to support discharge. For example, the patient missed having a dog and being no longer fit to look after one, visits from a local pet charity were arranged for when the patient was discharged.
Exploring the root cause of the anxieties around their health culminated in the patient admitting that they were worried their pacemaker might malfunction as the battery was due for replacement later. The patient lived alone and was concerned that should the battery malfunction, there would be no help available. This was the underlying worry and what mattered most to them.
Ward staff were made aware and asked if this could be changed earlier than planned as the potential driver for repeat admissions. The battery was changed and post-procedure, there have been no further hospital admissions following discharge. This has generated an efficiency gain of £62,564.25 if the pattern of admission and discharge were to continue.
This case study demonstrates improved patient outcomes as the patient felt able to share their anxiety, leading to high value care that meets the needs of the individual in a shared decision making and personalised approach to care.
Our Vision
Our vision for Realistic Medicine has not changed:
'By 2025, we will support the Health and Social Care workforce to practise Realistic Medicine, thereby enabling the delivery of high quality and personalised care to the people of Scotland.'
We remain committed to ensuring that health and care colleagues can access the tools and learning resources they need to practise Realistic Medicine and deliver VBH&C.
However, in order to ensure we are delivering VBH&C, we need to be able to measure the outcomes that matter to the people we care for and we will need to consider how we support health and care colleagues to do this. That's why we have a new, longer-term vision for Value Based Health & Care in Scotland:
Vision
By 2030 all health and care professionals will be supported to deliver Value Based Health & Care. This will achieve the outcomes that matter to people and a more sustainable system.
The following strategic aims will help us achieve our vision for Value Based Health & Care in Scotland.
Contact
Email: RealisticMedicine@gov.scot