Community eyecare services: review
Report on how eyecare services are currently delivered, with recommended actions which will lead to improvements to meet patients' needs.
Part I: Context and Developments Since 2006
1. A Ten Year Review
The introduction of the new General Ophthalmic Services ( GOS) regulations in 2006 ( 1) heralded a fundamental change from the testing of sight, to a more patient-led approach. NHS eye examinations became free for everyone, removing an important barrier to care. The emphasis was focussed on managing patients in the community where it was safe to do so, and improving the quality of the referrals that were made to the Hospital Eye Service. Disease prevention and early identification of sight-threatening conditions were also key; improvements were made to develop the case finding/screening for eye disease with the opportunity to recall patients early to reassess or repeat tests or examinations (supplementary examination). Dilating older patients, taking retinal photographs, routinely using binocular indirect ophthalmoscopy, contact (applanation) tonometry and repeating measurements of threshold visual field screening have been key elements to developing the service.
Ten years on from the 2006 Regulations being introduced, the community eye care landscape has developed in line with patient needs and government policy ( 2). More integrated care is being provided in local practices, with community optometry supporting pharmacy, GP, nursing, social care and third sector colleagues to help patients remain within primary care. Many optometrists are caring for more patients within their practices that they would have traditionally referred on to the hospital; referral rates are considerably lower when compared with those in England ( 3). This is coupled with dramatically developing hospital-based care where enhanced treatments are saving sight in more patients and where the demand for age-related ophthalmological procedures continues to rise. It is more important than ever that primary and secondary care professionals are working effectively together to ensure that patient's care is appropriate, timely and personalised ( 4).
Wider integration with social care supports patients in the community with greater needs but despite a universally free service, there is evidence that health inequalities do still need to be addressed ( 5). Local initiatives have developed some excellent community service models ( e.g. NHS Lanarkshire, Grampian and Ayrshire & Arran) enabling care to be shifted into the community where patients are being managed by community Optometry ( Annex B).
With many improvements and developments, a ten-year review of community eyecare services is a timely opportunity to reflect on the achievements and to work to develop more clinically evidenced care. It is also the opportunity to assess how patients' needs have changed and are changing and putting in place a future-proofed service that will continue to be relevant.
2. Scottish Government Policy
Since the introduction of the new General Ophthalmic Services Regulations, the health and social care landscape has changed dramatically. The Scottish Government's 2020 Vision ( 2), set out the Government's strategic vision for delivering quality healthcare services across Scotland, including providing care in a community setting. The publication of the Scottish Government's Chief Medical Officer's 2015 annual report Realistic Medicine ( 4) and the National Clinical Strategy ( 6) have supported this vision. These strategies highlight the changing demographic of Scotland's population, the need to deliver quality care in the community where possible, and reduce unnecessary hospital admissions. This work feeds into the Government's wider primary care transformation agenda of building a multi-disciplinary approach to health and social care, of which optometry will be a key part. The transformational work will explore better ways of working that improve pathways for patients, and ensure that they see the most appropriate healthcare professional in the right place at the right time.
The Scottish Government's Modern Outpatient Programme launched in 2016 ( 7). The intention of this Programme is to shift focus from outpatient appointments in hospital, to empowering patients to manage their own health, and to be able to access appropriate healthcare support when required. This will involve increasing the delivery of care within a primary/community care setting, therefore reducing the need for patients to attend hospital for treatment where appropriate. This will mean those patients that need to be seen in hospital will be seen quicker, while those that can be managed within the community will see the most appropriate healthcare professional. The Programme is currently in consultation phase.
The eyecare review will also form part of the Health and Social Delivery Plan announced in late 2016 ( 8). Optometry is in a prime position to play a key role in managing this plan, by supporting more patients within the community, and reducing the burden on hospitals.
It is not just Scottish Government policy that has changed the landscape of healthcare provision. The Francis Inquiry examined failings at the Mid Staffordshire NHS Foundation Trust ( 9) and recommended that healthcare systems should be open and transparent. It emphasised the need for more patient-centred care within the NHS, and high quality leadership. The tragic court case where an optometrist was found guilty of negligent manslaughter ( 10) has also highlighted the need for good leadership skills within the practice setting, and will influence the training and services provided by locum optometrists. Practices also need to ensure that new and locum optometrists are confident with IT systems before they see patients.
The Scottish guidance on glaucoma referral and safe discharge ( 11) recommended discharging stable glaucoma patients to be managed in the community, allowing those more serious cases to remain within the hospital eye service. The evidence based guidance supports the safe, high quality community care targeted in the 2020 Vision ( 2).
3. The current and future needs of the population
A key government performance target is that the population will continue to live longer healthier lives ( 12). Current projections suggest that the population of Scotland will rise to 5.7 million by 2039, and that the population will age significantly, with the number of people aged 65 and over increasing by 53% between 2014 and 2039 ( 13). It is also predicted that those aged 90 years and above will have nearly tripled (an increase of 190%).
Since 2006, the number of patients over 60 years old being examined has increased by 34%. With the prevalence of many of the most sight threatening conditions increasing dramatically with age, the "demand for ophthalmology care within Scotland is (already) rapidly out-stripping capacity" ( 14).
Risk Factors
Age
Age is the greatest risk factor for developing sight-threatening conditions ( 15). The revised GOS regulations ( 16) reflect this higher risk group, requiring a more stringent ocular assessment as part of the primary eye examination for those over 60 years, and the option to recall at one rather than two years. The older you are, the greater the risk of developing cataract, glaucoma and macular degeneration, as well as retinal changes due to diabetes. Whilst a cataract can generally be easily managed with surgery, treatment to reduce further visual loss due to glaucoma, and to restore and prevent the progression of macular degeneration and diabetic retinopathy are much more challenging. In many cases, early intervention is key to slowing progression and therefore the optometrist is vital in identifying at the earliest opportunity signs of the developing disease.
Patients with learning difficulties
It is widely accepted that children with learning disabilities are considerably more likely to have a visual impairment ( 17, 18) although estimates vary between 8 and 200 times higher than the general population ( 19). Certainly, levels of refractive error are very high, and the importance of early intervention with the correct spectacle prescription can have a profound effect not only on future vision potential, but on overall social and intellectual development.
Pathways have been established nationally ( 20) and locally e.g. NHS Ayrshire and Arran ( 21) has developed a network of services and trained specialists, and national training is also available from NHS Education for Scotland for optometrists ( 22). SeeAbility's qualitative studies have indicated the importance of allowing additional time and repeat appointments to conduct a patient appropriate eye examination ( 18), something not presently possible under the GOS fee structure ( 16).
The fitting of spectacles on patients with learning difficulties can be challenging and NHS England ( 23) has introduced additional funding for more specialist fitting (special facial characteristics supplement). SeeAbility ( 24) has recommended that adults with learning difficulties are only dispensed spectacles by a registered practitioner as required when dispensing for children and patients who are blind and partially sighted ( 25). This would support a higher quality of care for these vulnerable patients.
Ethnicity
Certain ethnic groups are at a greater risk of developing some sight-threatening ocular conditions. Indeed, in Wales patients who are of "Black or Asian Ethnicity" are entitled to an NHS-funded assessment. Scotland has a lower ethnicity mix than many other parts of the UK with 96% population identified as white ( 13). The Asian population is the largest ethnic minority group at 3%. However, national statistics can be misleading, with small areas within Glasgow in particular, with very high percentages of minority ethnic residents, which are dramatically increasing ( 27, 28).
Lifestyle
Like many systemic conditions, good nutrition is vital to good ocular health. Recent studies have revealed the very strong links between macular disease and nutrition ( 29) driving a large increase in the sale of disease specific supplements.
Poor nutrition frequently leads to obesity which is a growing problem in Scotland ( 30). Obesity has a negative effect on ocular health, with not only an increased risk of retinal vascular disease, but an increase in conditions such as pseudo-tumour cerebri (idiopathic intracranial hypertension) in obese women of child bearing age ( 31).
Smoking has a very negative impact on eye health and under GOS, optometrists are required to ask whether their patient smokes as part of the eye examination ( 1). Macular degeneration has a higher prevalence in patients who smoke; these patients have an increased risk of developing cataract, uveitis, dry eye conditions, and other retinal vascular diseases.
Diabetes
One of the many complications of diabetes is the effect on vision and the eye. Variable visual acuity, retinal bleeds and neovascularisation as well as the increased risk of developing other ocular diseases, highlight the need for these patients to have regular eye examinations.
Scotland implemented a national screening programme in 2006 ( 32) with the primary objective of detecting sight threatening changes in patients with diabetes. The Scottish Diabetic Retinopathy Screening ( DRS) collaborative is supported across Scotland by NHS Boards. The screening service has a defined set of standards that are regularly reviewed ( 33). In addition to diabetic retinal screening, diabetic patients are examined as part of GOS for routine eye examinations. Retinal photography frequently makes up part of this examination. Ayrshire and Arran support diabetic patients with their own local solution which uses community optometry as the screeners and graders.
Barriers to eyecare
It is a key part of the Scottish Government's policies, that barriers to care are reduced and ideally removed for those in lower socio-economic groups ( 2). This remains a challenge across health as well as in community eyecare ( 34, 35). Eye examinations in Scotland have always been free of charge to those on the lowest incomes and in this respect the introduction of the GOS eye examination in 2006 had a lesser impact on this aspect of access to service.
Convenient practice locations are clearly important to the uptake of a service. Studies have indicated an even distribution of service location to deprivation index ( 34, 35), with the exception in Scotland of high deprivation areas in NHS Tayside ( 35, 36).
Sir Lewis Ritchie's report Pulling together: Transforming urgent care for the people of Scotland ( 38), set out the need for a multi-disciplinary approach to primary care services, both within and out-of-hours. Optometry is able to play a role in this approach as optometry practices, like pharmacies, are open in the evening and at weekends including Sundays but frequently this is in more urban settings. A recent review of access in optometry ( 5) concluded that:
"the patient access problem is complex and more about patient attitudes and social culture than location of practice."
Indeed, a qualitative study in England has highlighted the general lack of eye health awareness, poor knowledge of the sight test's role in detecting disease, and negative perceptions of optometry when it comes to the sale of spectacles, as key factors for people not accessing the service ( 39).
Blind and Partially Sighted Patients
Sight loss is devastating for any individual. It is frequently associated with co-morbidity ( 40, 41) and impacts on all areas of daily living. It has been estimated that sight loss costs the NHS and the public sector in Scotland a minimum of £194 million a year, plus £434 million more in terms of broader costs to the economy and to society ( 42).
It is estimated that 1 in 5 people aged 75 and over and half of those aged 90 and over, are living with sight loss ( 43). Patients with severe sight loss can be registered as blind or partially sighted. In 2010, 34,492 people in Scotland were registered ( 44). These people require support and assistance to remain independent, to avoid social isolation and to maintain a good quality of life. Such support services, whilst often extremely effective are frequently disjointed, of variable quality and patchy across Scotland ( 45). There is also no clear picture of what such a service should encompass, although it is widely appreciated that it requires a patient-centred approach from a multi-disciplinary team ( 46). One initiative that is making a difference is the introduction of vision support officers, offered in some eye clinics around Scotland. They provide emotional and practical support to people with newly diagnosed sight loss and are making a large difference to patients.
See Hear is Scottish Government's long-term strategy for meeting the needs of people with a sensory impairment ( 47). The strategy, jointly endorsed by COSLA (Convention of Scottish Local Authorities), sets out a commitment that adults and children should expect a seamless provision of assessment, care and support with the same access to public services. It is being implemented through local partnerships of statutory and third sector partners, and local leads have been identified to drive progress across priority areas.
4. The activity and costs in relation to eye examinations since 2006
16.4 million eye examinations have been conducted since the introduction of the new GOS regulations and the number of patients attending for an eye examination has risen each year (Charts 1 and 2).
Chart 1 Number of Eye Examinations each year by Patient Age
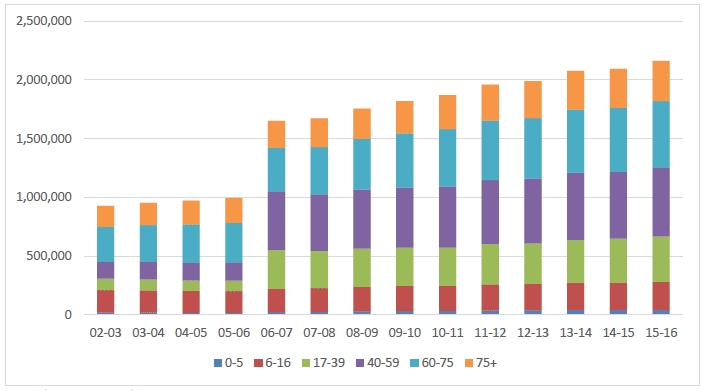
April 1 st until March 31 st each year ( 48)
Eye examinations were available to all from April 1 st 2006
There have been many factors that have driven this increase and these include:
- A free service to patients ( NHS funded for all)
- Optometry is seen as the "First port of call" for all eye disease
- An ageing and increasing population
- An increase in referrals by GPs
- An increase in referrals from other health professionals and social care e.g. pharmacists, community nurses, rehabilitation officers
- Patient education e.g. RNIB campaigns, word of mouth, health promotion, commercial advertising
- More patients being managed and treated within primary care e.g. IP optometrists, local board initiatives
- Occupational requirements e.g. driving, VDU
- Patients discharged from the Hospital Eye Service ( HES) e.g. ocular hypertensives
- Board initiatives and shared care schemes
- Closure of walk-in Accident and Emergency departments ( AEDs)
Changes in 2010 to reduce the frequency of the primary eye examination resulted in a change in balance between a primary and supplementary examination (see Chart 2).
Chart 2 Number of Primary and Supplementary Eye Examinations 2006 - 2016
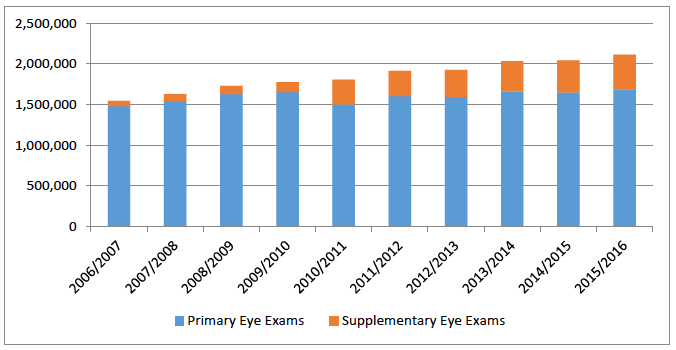
Source: NSS ( 48)
The total spend on eye examinations has risen from just under £40 million when GOS was introduced in 2006/7 to £76 million in 2015/16 ( 48). There was an initial steep cost increase with a phased fee rise over the first four years, but there has been no fee increase for Optometrists since 2010. Recent increases in spend have been due to increased demand by patients and a significant shift in the balance of care from secondary into primary care in line with government policy.
Improved care under GOS
As well as increasing the required assessments conducted within the primary eye examinations especially for older patients, the 2006 contract introduced the supplementary examination. There was previously no mechanism for a patient to be assessed by an optometrist unless a full eye examination (with refraction) was conducted. The optometrist either had to charge privately, or advise the patient to seek care elsewhere. The increase in supplementary exams of over 500% is a clear indication of the additional care undertaken by optometry as a direct result of government policy to provide more community based care ( 2, 49). The main purpose of the supplementary was to fund an assessment outwith the time restricted primary examinations, either on the advice of the optometrists e.g. referral refinement, risk of pathology developing, reviewing treatments implemented, or requested by the patient or another practitioner e.g. loss of vision, recurrent headaches, red eyes, flashes and floaters, ocular injury etc. A post cataract review is a good example of where the supplementary examination has been supporting patients (Case 1). This examination has enabled optometrists to prescribe and treat patients, reviewing and supporting their management. It has also supported the refinement of referrals, particularly for glaucoma, and allows the SIGN glaucoma referral and safe discharge guidance to be followed ( 11). Finally and perhaps often not fully appreciated, this examination allows the optometrist to offer patients piece of mind and support.
Case Study 1 - Cataract Referral and Review
A primary NHS eye examination was conducted on an 80-year-old patient in NHS Lanarkshire. She had binocular cataract and was very aware that her vision was getting worse; she was struggling with the crossword and following knitting patterns. Her family was keen for her to have the surgery, but she had declined referral at her last two appointments.
A dilated examination identified significant nuclear and cortical cataract in both eyes. Fundus and anterior eye checks were both normal. The updated spectacle prescription made no difference to her visual acuity. The optometrist advised that to improve her vision, cataract surgery was now the only option. The procedure, complications and consent issues were discussed and she was now keen to be referred. She was given an information leaflet and an electronic referral via the fast track cataract pathway was sent.
Five months later she attended for a supplementary examination having had her surgery 6 weeks previously in Hairmyres hospital, East Kilbride. She was discharged back to her optometrist for the post-op review and refraction. She had completed her course of antibiotic and steroid drops. The entire experience had been trouble free and she was delighted. Her anterior eye was checked and found to have healed well with no complications. Her new refraction enabled her to easily achieve vision better than she'd had in the 10 years of coming to the practice. An electronic referral for the second eye was arranged. She couldn't wait to get back to knitting with her new glasses as her first great-grandson had just recently arrived.
Referrals are made following an eye examination when the optometrist identifies a need for further investigation or treatment, and with the agreement of the patient (Chart 3). In many cases, the referral is made to the Hospital Eye Service ( HES) but other hospital referrals include neurology and the stroke service. Referrals are also made to the GP for general health issues e.g. systemic hypertension, prescribed medication concerns, headaches.
Chart 3 Referrals from optometrists to GPs and the Hospital Eye Service ( HES) in Scotland (red and blue bars), and new patients seen in the HES (green bars)
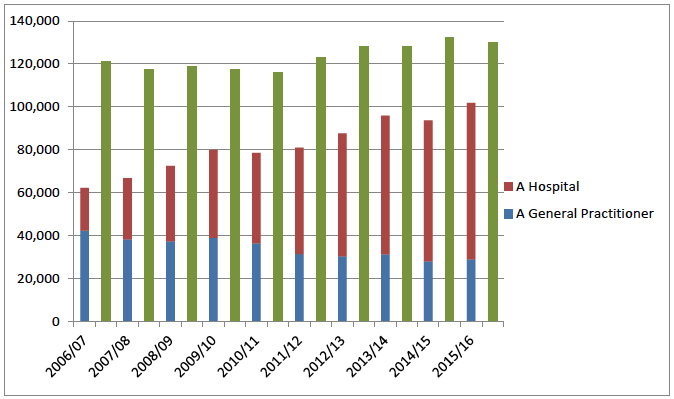
Source: NSS ( 48)
To note: Red and blue bars are the referrals recorded on the GOS 1 form - in some Board areas all optometrist's referrals are direct to the HES whilst in others, some referrals are still via the GP. Therefore, not all GP referrals will be for the HES and may be for the GP themselves.
Green bars are new patients attending outpatient appointments within the HES around Scotland.
There is no routinely collected data on the number of GP referrals to HES.
Other community referrals include to social care (general living issues) or another optometrist (specialist services out-with GOS).
Feedback from the appointment following referral is vital and supports the on-going management of patients within the community ( 46). It is also important to improve the on-going quality and appropriateness of referrals. Of note is the 13% increase in new patients seen at ophthalmology departments in Scotland over the last 10 years, compared with the 32% increase in England ( 3). Whilst fewer patients are referred via their GP, referrals are frequently made for management by the GP, relating to many general health as well as ocular conditions. Close working relationships between general practice and community optometry have been strengthened with no fees as a barrier to care, and referrals from GPs to optometry have increased significantly ( 48).
Optometrists work closely with community pharmacy colleagues ( 49). Two-way referral supports community eyecare and a free to patient service allows swift access to treatment and medication.
5. Ophthalmology
New treatments have had a profound effect on the ability of ophthalmologists to save sight. For example: repeatedly successful retinal detachment surgery, macular disease injections and micro-surgical advances, targeted glaucoma drugs and new trabecular drainage surgery and rapid routine cataract day surgery, dramatically improve sight. Scotland's ageing population combined with these developing treatments results in the continued on-going pressure on hospital services. The annual ophthalmology spend in Scotland is over £145 million ( 50) and has increased by 45% in the last five years (Chart 4). This is despite many initiatives around the country to discharge patients out to community optometry e.g. NHS Lanarkshire and NHS Grampian eye health networks, AEDs closed to walk-in patients in many areas of Scotland and early discharge of post-cataract patients.
Chart 4 Total Ophthalmology Spend in Scotland*
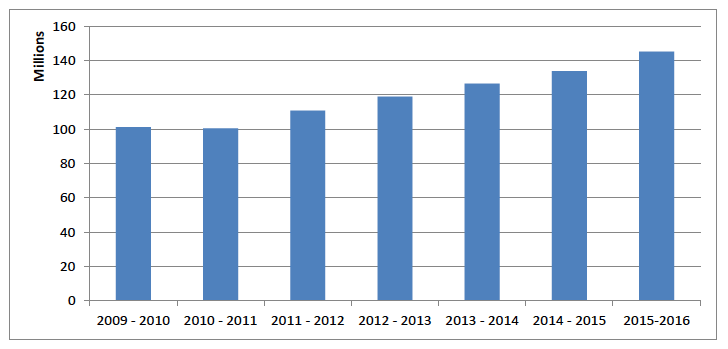
NSS(50) *inpatient and outpatient activity
6. Service Developments
a) National developments
E-Health
The referral of a patient with an ocular condition was expedited in 2006. The regulations facilitated the routine referral of patients from the community directly to the hospital eye service ( HES), thus reducing the administrative burden on the GP. In 2010, the Scottish Government approved a national optometry programme to deliver electronic payment and electronic referrals for the optometry community, called the Eye Care Integration Programme ( 51). The electronic referral of patients between optometrists and hospitals is crucial to supporting patient care ( 52) and aimed to deliver the following benefits:
- enhanced patient safety - so those that require sight-saving treatments are seen quickly
- a reduced burden on general medical services ( GMS)
- improved ophthalmology waiting time targets
- electronic feedback to optometrists upon receipt of the electronic referral
- better data quality meaning fewer errors
- reduced paperwork
Chart 5 Percentage of e-referrals by NHS Health Board
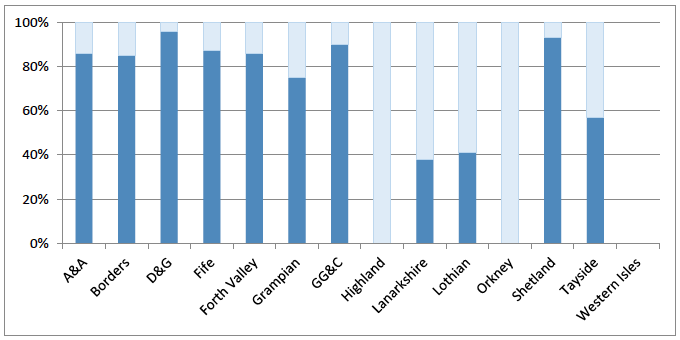
Source: NSS (December 2016)
Electronic referrals have gone live with varying degrees of uptake (chart 6). Work continues to improve uptake and address the issues affecting the programme.
The electronic transmission of General Ophthalmic Services ( GOS) claims for payment provides an important cost saving exercise across NHS Services Scotland ( NSS). It also supports:
- the validation of a claim while the patient is still available to answer any queries that may arise
- clerical issues resolved at source, reducing the burden on practice resources to correct and re-submit forms that have been rejected
- more robust check of patient entitlement reduces the time to process payment claims
- faster payment of claims to community practices.
Case Study 2 - A Patient Managed within Primary Care
A 72 year old male who had cataract surgery in summer 2016, returned in November to his IP Optometrist in NHS Tayside. He was complaining of a pain over the left side of his head and a red eye which had been a problem for a few weeks. He was booked for an NHS supplementary examination the following day.
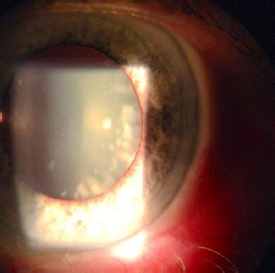
An external ocular assessment revealed a small mass on the white of his eye (Figure 1). Using a 25 gauge needle the optometrist found that it was a piece of debris that had become embedded. This was carefully removed and the patient was given antibiotic drops with a NHS Prescription. On review the eye had returned to normal and the patient was asymptomatic.
This case demonstrates the importance of the NHS supplementary test in the community. The patient was examined by an optometrist who knew him well, he was seen without delay and his problem was managed in a professional and straight forward manner.
Figure 1. Before
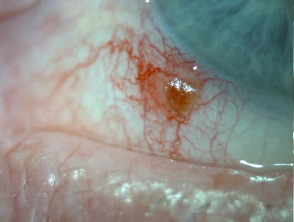
Figure 2. After
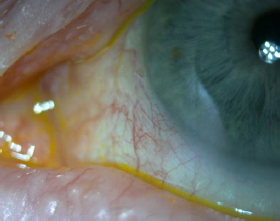
The e-payment system has now rolled out with 50 practices submitting claims via a web form, totalling approx. 5,000 claims a month. Two software suppliers are currently developing solutions to allow their customer base to submit claims electronically, and it is hoped uptake will increase over the coming months.
First port of call for all eye conditions
In line with policy, many GPs no longer see patients with eye problems but direct them to optometry. This is helping to reduce the burden on general practice.
"Whatever your eye problem your first port of call should be an optometrist." NHS Lanarkshire website
"Community optometrists are now recognised as the first 'port of call' for eye problems. If you have any problems with your eyes, make an appointment with an optometrist." NHS Greater Glasgow and Clyde website and posters in NHS facilities across the Board area.
Awareness of this change is beginning to be understood by the public but there are still issues about getting the message to the wider population ( 33, 53). Case 2 is a good example of a patient now fully managed within the community.
All optometrists should be competent to treat basic ocular conditions e.g. dry eye, allergic and bacterial conjunctivitis, blepharitis. Some further training has been provided nationally to more appropriately manage acute ocular conditions and locally in boards where this initiative has been most widely developed e.g. NHS Lanarkshire and NHS Grampian ( Annex B).
In parallel with the comprehensive independent prescribing ( IP) qualification, local schemes support some treatments with PGDs (patient group directions) and agreements with GP colleagues. Regular audits have shown considerable success and widespread patient satisfaction of these schemes ( e.g. 54-56 )
b) Local Developments of the national service (funded under GOS)
There are 14 territorial NHS Boards that are responsible for the protection and the improvement of their population's health and for the delivery of frontline healthcare services. Whereas General Ophthalmic Services is a national eye care service, Boards can enhance and develop local care. For example, NHS Ayrshire and Arran has developed extensions and pathways to support GOS. These include:
- Smoking cessation
- Transient Ischemic attack pathway
- Falls prevention
- Routine enquiry supporting victims of domestic abuse
c) Enhanced Local Services (funded by the Board)
There are several enhanced optometrist-led services in current operation scattered across different Health Boards in Scotland (see Annex B). These services have been developed and funded by individual Health Boards to meet a clinical need for their population. By the very nature of the processes involved in implementing these services, they are not standardised across the whole country. This means that patients will be accessing varying levels of service, available from different providers across Scotland.
- Diabetic Retinopathy Screening (national DRSS, NHS A&A)
- Low Vision Services
- Post-operative cataract review (only NHS A&A is an enhanced service, all other boards run under GOS)
- Care for patients with learning difficulties ( NHS A&A)
- Clinically required contact lenses (various)
- Grampian Enhanced service contract for eye treatments e.g. Case 3
- Glaucoma Shared Care (Grampian)
Case 3 - NHS Grampian Eye Health Network management of Marginal Keratitis
A 64-year-old patient in Dyce lives just around the corner from her local optometrist. She attended for an emergency supplementary appointment with a painful red eye. She was very stressed and upset. On slit-lamp examination she was diagnosed with marginal keratitis and treatment with antibiotic eye drops was started immediately. A faxed referral was made to her GP to co-prescribe a steroid eye drop based on the Grampian Eye Health Network protocols ( 57).
The follow up was booked in the practice two days later and there was a marked improvement in her symptoms. She was discharged at the 1 week review appointment. The patient was extremely grateful. She was happy with the convenience of being seen "just around the corner" and with an appointment to suit her.
7. The workforce
There are 1,453 optometrists and 3 ophthalmic medical practitioners listed with a Health Board in Scotland ( 58). There is no central NHS Ophthalmic list of Optometrists and Ophthalmic Medical Practitioners ( OMPs); all lists are held with each Health Board. OMPs conducted less than 0.1% of the eye examinations in 2015/16 ( 48).
410 qualified dispensing opticians ( DOs) are registered in Scotland ( 59) but they are not listed with the NHS. They are a regulated profession who specialise in the dispensing of spectacles and with additional qualifications, the fitting of contact lenses. Spectacle fitting on children is a restricted function ( 60) and DOs rather than the optometrist, conduct this task in some practices. Their specialist training and considerable knowledge of ocular pathology also supports their wider role in triage in community practice, and their own role in case finding should not be overlooked.
The issuing of spectacle prescriptions is restricted to medical practitioners and optometrists. The Opticians Act 1989, links an ocular assessment with a refraction, but technology is enabling self-refraction and on-line spectacle ordering, which is soon going to support dispensing of spectacles without the need for a professional refraction ( 61).
A good practice team is vital to high quality and safe patient care. Whilst the NHS listed practitioner is often examining patients in the testing room, he/she is reliant on the wider practice staff to attend to patient queries, correctly triage patients and support anxious patients. Optical assistants frequently are conducting delegated functions e.g. visual field assessments, retinal photography and spectacle fitting on children. Staff who are well trained, understand their role and appreciate when to ask for guidance are crucial. Thus, the optometrist needs to have good leadership and management skills within the practices ( 62).
Chart 6 Community IP optometrists in Scotland by NHS Health Board
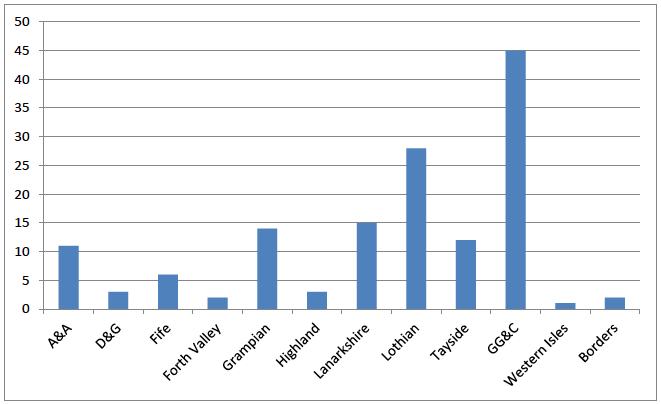
( NSS ( 48))
Independent Prescribers
142 community optometrists are qualified independent prescribers (chart 6); 35% UK IP optometrists are in Scotland ( 59). Prescribing patterns indicate a very conservative approach, with lubricants by far the most prescribed preparation. There is huge intra-professional variation in prescribing rates which is likely to reflect the variation in experience, with a number of practitioners having been prescribing for many years e.g. under the Glasgow Integrated Eyecare Service ( GIES). A national audit of prescribing data is required to further develop and highlight the service that is being provided within the community.
Locum Optometrists
There are 417 optometrists listed on part 2 of the Ophthalmic List as locum practitioners ( 58). In 2010 the GOC commissioned a report to consider "Risks in the Optical Profession" ( 63). The issue was raised by various stakeholders that "locums could pose a risk to patient health and safety". The report found no available data to support this concern. The role of the locum could be one of reduced accountability, but one also of greater experience from working in many different environments. The GOC report concluded that any risk was largely down to the individual practitioner and not necessarily their role as a locum ( 63). Similar risks have been highlighted in medicine ( 64), and in light of the locum optometrists found guilty of gross negligence manslaughter ( 10), this group of practitioners may well require additional attention.
Developing the Workforce
A dramatic increase in postgraduate education has also been a factor in raising the standard of community eyecare. All optometrists were initially required to undertake training to reach a minimum standard of competence ( 2). Any practitioner taking two years away from practice is required to be re-trained and if an optometrist wishes to move to practice in Scotland, they need to attend training. Further, clinical placements, interactive workshops, e-learning and peer discussion groups are all available to support community practitioners. The profession has been enthusiastic in taking on additional responsibility and keen to develop their skills. Nearly 30% of the profession are either qualified, or on their way to becoming Independent prescribers ( IP). This qualification supports more community care, with practitioners being able to prescribe treatment for a huge range of ocular conditions reducing both the burden on general medical services and referrals to the hospital eye service. Programmes are also available for dispensing opticians and optical assistants to support the care provided to NHS patients by all practice staff.
Optometry Practices
There is a fair distribution of practices providing GOS across Scotland ( 58). The average distance to a practice was 3.4km which related to a drive time of 5.3 minutes. Almost two thirds of the population were within 5 minutes' drive time of their nearest practice. In Highland, Shetland, the Western Isles, the Borders and Dumfries & Galloway however, many population centres were at distances of 10km or more from local practice ( 36).
8. Looking Ahead
It is vital that community eyecare services continue to improve and develop over the next few years to meet the changing needs of the Scottish population. There has already been huge progress with an increase in the range of care that is now being provided; Many more patients are being treated and managed successfully. Evidence to support good practice will allow further developments and enable patients to continue to access a high quality, safe community service.
Contact
Email: Liam Kearney
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG