The commission on widening participation in nursing and midwifery education and careers
The aim of the commission was to maximise opportunities to participate in nursing and midwifery education and careers.
2. Evidence and findings
The Commission gathered a range of information regarding Scotland's nursing and midwifery workforce and student population profiles, existing access routes, and policies and measures encouraging access to education and employment (including financial support for institutions, employers and students). The following provides a brief overview and key headlines, with some examples of emerging approaches to widening participation in nursing and midwifery careers being taken forward currently in Scotland.
The chapter also provides summaries of two pieces of work carried out on the Commission's behalf: a rapid review of the international and UK literature, and a survey of students and registered nurses on accessing nurse education through widening participation routes.
2.1 Nursing and midwifery workforce
Nursing and Midwifery Council ( NMC) registration figures [11] show that as of March 2017, there were 618,863 registered nurses and 33,464 registered midwives on the UK register. [12] In Scotland, 68,826 nurses and midwives were on the register in September 2017. [13]
Fifteen per cent of the workforce in Scotland are employed in health and social care, representing over 400,000 staff. Around £6 billion is spent annually on the 162,598 staff employed by NHS Scotland, and 99.6% of all NHS care is delivered by NHS staff.
The nursing and midwifery workforce is the largest staff category for NHS Scotland by some way (42.7%), with almost 60,000 whole time equivalent ( WTE) nursing and midwifery staff in employment in June 2017. Overall, there are more than 3,000 WTE more nursing and midwifery staff working in NHS Scotland compared to five years ago.
Since September 2006, the number of registered nurses and midwives working in NHS Scotland has increased by 5.6%, by 2,314.0 WTE to 43,340.2 WTE. At June 2017, 73% (40,956 WTE) of the NHS Scotland nursing workforce was registered, a proportion that increased by 0.9% over the past decade. Information and Statistics Division ( ISD) figures show that 83% (2,347 WTE) of the midwifery workforce was registered as of September 2016 (a reduction of 5.9% from September 2007, while midwifery support staff WTEs increased by 83% over the same period). Workforce planning requirements in light of a transformed model will be part of the work to support implementation of the Best Start review. This will include the need to consider the role of support staff.
In relation to the social care sector, there were around 6,650 nurses working in the social services sector at the end of 2016, representing about 10% of the nursing workforce in Scotland. The independent sector employs 6,051 (91%) of social care nurses across care home services for adults, housing support and care at home services. Care homes for adults employ 64% of this total. [14] Eleven per cent of the total (registered and support staff) nursing workforce is male, but males account for under 1% of the midwifery workforce. The nursing and midwifery student population is currently 92% female and 8% male, and the proportion of males applying to nursing is falling. The workforce is also ageing.
The National Health and Social Care Workforce Plan Part 1 identifies current and future workforce challenges, including the effects on the nursing and midwifery workforce of issues such as remoteness and rurality, availability of nurses in social care (in particular, care homes), and the potential effects of the UK's exit from the European Union (Brexit). It considers international flows, including the impact of Brexit, on recruitment and retention, and how to make more effective use of international recruitment opportunities. These will take account of developing research across the wider public sector in Scotland of the potential effects of Brexit on international recruitment.
It is not possible to know exactly what effects Brexit will have on the nursing and midwifery workforce at this stage, but registration data show that the number of initial joiners to the NMC register from EU countries reduced from 9,389 in 2015/16 to 6,382 in 2016/17; total numbers of EU registrants nevertheless rose from 34,502 in March 2016 to 38,024 in March 2017. [15]
The National Health and Social Care Workforce Plan Part 1 projects a shortfall of qualified nurses and midwives in the short and medium term unless further measures are taken to enhance supply and manage demand. It commits to an estimated 2,600 additional nursing and midwifery training places by 2021, alongside a wider package of measures to support recruitment and retention of students and existing staff, and measures to widen participation in education and careers. Further work is being undertaken to define nursing and midwifery numbers within the aggregated headline figure.
The National Health and Social Care Workforce Plan Part 1 sets out key recommendations for all of the workforce that relate to:
- testing out new approaches, focusing on promoting and attracting applicants and making health and social care careers more attractive to young people through improved marketing and advertising
- exploring the interface between health and social care and further and higher education to maximise opportunities to recruit and retain staff
- linking student commissioning more closely to recruitment, retention and youth employment, taking account of current trends in supply and demand; this work should also link to career paths and opportunities acros
These recommendations reflect the situation that while NHS workforce numbers have never been higher, the need to take action now to ensure the right numbers of staff with the right skills are available to provide high-quality health and social care services to the people of Scotland now and in the future is urgent.
The Commission noted that efforts to forecast future demands for the nursing and midwifery workforce in capability, competency and capacity terms require further work. This should include the modelling of workforce against future models of care delivery. The concept of a zero-based workforce planning approach was explored and should be tested further.
2.2 Pre-registration nursing and midwifery education
At 31 October 2016 (the last available data at the time of the report's publication), there were 10,239 students in pre-registration nursing and midwifery education, of which 539 were student midwives. [16] The recommended increase in student nursing and midwifery intakes for 2017/18 was 4.7% – the fifth successive rise (following a 5.6% increase in 2016/17, 3.5% in 2015/16, 6.6% in 2014/15 and 4.1% in 2013/14), equating to 3,360 entry places; 60 additional places over and above existing numbers were funded in north-east Scotland to reflect the challenges experienced in remote and rural areas.
Nursing and midwifery pre-registration programmes in Scotland continue to be over-subscribed, but the number of applications per place has fallen in recent years, and Scotland has seen a 10% reduction in applications from males since 2013. There was an aggregated 3.2% reduction in applications to pre-registration nursing and midwifery programmes from students domiciled in Scotland to Scottish universities between 2016 and 2017. By contrast, English universities saw a 22.9% reduction in applications from students domiciled in England during the same period.
Scottish higher education institutions ( HEIs) had the highest median percentage of nursing graduates in sustained employment at one year (75.8%) and three years (68.5%) after graduation compared to all other regions across the UK, and the second highest median percentage of nursing graduates in sustained employment five years (67.1%) after graduation (the highest was East Midlands, at 68%). There are nevertheless significant differences in performance across HEIs and nursing fields.
Scotland is performing well in attracting students over the age of 25, while England in particular has seen a substantial drop (23%). Though the nursing and midwifery student intake is one of the most age-diverse, it nevertheless remains largely under the age of 24. Currently, around 48% of students are under 20, with about 28% between 20 and 24.
HEIs' and further education institutions' ( FEIs') contextual admission targets include objectives against the SIMD (including, for example, SIMD1, representing the 20% most deprived areas of Scotland). The Impact for Access project funded by the SFC that reported in October 2017 [17] showed that 14% of Scottish-domiciled entrants to full-time degree courses in Scotland's 18 HEIs in 2015/16 came from SIMD1 postcodes, suggesting the national 16% target by 2021 is within reach. The percentages differed significantly among institutions, however, for those HEIs offering nursing and midwifery education, they ranged from around 27% to just above 5%. [18] At 3.5 years after starting a nursing programme, there is an approximately 15 percentage point difference in probability of completing between students from the most deprived communities (54%) and those from the least deprived (69%); by five years after starting, this gap has closed to 6 percentage points (77% and 83% respectively).
On gender diversity, there has been a slight reduction in the proportion of male students applying to pre-registration nursing and midwifery courses: 8% of the 2016 student cohort was male. Data has shown women are more likely to complete their courses.
Around 95% of students are UK nationals, with most non- UK nationals coming from European Economic Area ( EEA) countries. In 2017, Scotland was the only UK country to see a rise in EEA students applying to nursing (+3%).
A summary of information on the nursing and midwifery pre-registration student population is shown in Table 1.
Table 1. Pre-registration nursing and midwifery student data in Scotland
| INDICATOR |
Nursing (all fields) |
Midwifery |
|---|---|---|
| Applications (source: UCAS) |
Numbers of applications to nursing HEI courses in Scotland have been fluctuating in recent years: for the years 2013–2016, the number of applications were 14,520, 16,785, 16,465 and 16,400. |
Numbers of applications to midwifery have declined over the same period, from 1,965 to 1,725, a reduction of 12%. |
| Target intakes |
Each year, the Scottish Government recommends target intakes to each field of nursing practice with the aim of ensuring there are enough newly registered practitioners in each field for the future. Target intakes have been rising steadily, from 2,310 in 2012 to 3,149 in 2017. Actual intakes have also been increasing, from 2,605 in 2012 to 3,049 in 2016, an increase of 17%. |
Midwifery targets have increased from 100 in 2012 to 191 in 2017; intakes have increased from 105 in 2012 to 167 in 2016, an increase of 59%. |
| Cohorts by SIMD quintile (source: SFC) |
For the cohorts 2010 to 2015, an average 21% of Scottish-domiciled nursing students came from the 20% most deprived areas ( SIMD1). The percentage in this category varied between 19% and 23% across cohorts. |
For the same cohorts of midwifery students, an average of 13% of Scottish-domiciled students came from the 20% most deprived areas. The percentage varied across cohorts from 9% to 18%. |
| Age |
Nursing students have had a relatively stable age profile in recent intakes. Currently, around 48% of students are in the 16–19 bracket and a further 28% in the 20–24 bracket. |
The midwifery student age profile shows some more variation, but recent intakes have had a slightly higher proportion of students in the 16–19 bracket (around 45%). |
| Completion probabilities |
Looking at completion rates for nursing students on three-year courses in the 2009–2013 cohorts, around 57% complete at three years, 72% at four years and 75% at five years. |
Around 59% of midwifery students from these cohorts also complete at three years, increasing to 80% at four years and 84% at five years. |
| Gender |
The percentage of male nursing students varies slightly across cohorts but is typically between 8% and 10%. |
Midwifery intakes are typically 100% female. Two recent cohorts (2011 and 2014) had a single male student. |
| Qualifications |
Nursing students have a wide range of entry qualification types. In 2016, around 35% had Higher grades/A-levels, around 30% had vocational qualifications 1 and 13% had undertaken an access course. |
Midwifery students are more likely to have Higher grades/A-levels (around 60% in the 2016 cohort). Fewer midwifery students have vocational qualifications 1 and there is no formal access route into midwifery. |
| Nationality |
Nursing students have typically been around 93% from the UK. The percentage of EEA students in the 2016 cohort was 5%. |
Midwifery intakes have tended to have a slightly higher proportion of students from the UK (around 96%). The percentage of EEA students in the 2016 cohort was 4%. |
1 Vocational qualifications are typically Further Education Institute qualifications. In recent cohorts, these are likely to be Scottish Credit and Qualifications Framework ( SCQF) levels 6–7, for example an Access to Higher Education course (Scottish Wider Access Programme ( SWAP)), a Scottish Vocational Qualification ( SVQ), or a Higher National Certificate ( HNC).
2.3 Access routes
Access routes were considered in relation to education generally, and nursing and midwifery specifically.
2.3.1 Access routes to education
Education up to undergraduate level comprises a wide range of types of qualifications that span the Scottish Credit and Qualifications Framework ( SCQF):
- Scottish Qualifications Authority ( SQA)-accredited qualifications, such as the Scottish Baccalaureate in Science, are aimed at candidates in S5 and S6
- Scottish Vocational Qualifications ( SVQs) offer work-based opportunities
- higher national qualifications such as the Higher National Certificate ( HNC) and Diploma ( HND) are college- and practice-based, with some courses offering articulation to relevant undergraduate programmes
- Higher Education Certificate ( HECert) and Diploma ( HEDip) programmes are academic university courses that generally represent year 1 and 2 of undergraduate programmes, meaning articulation for the student may be smooth or, if taken within the same institution, even seamless.
The apprenticeship structure in Scotland has three levels:
- Foundation apprenticeships: offered to young people in S5 and S6, the foundation apprenticeship is seen as a vocational route that can lead directly onto an industry-based modern apprenticeship. From employers' perspectives, it is about developing the talent flow. Funding is provided by Skills Development Scotland ( SDS) direct to organisations such as FEIs.
- Modern apprenticeships: while there are no modern apprenticeships specific to nursing and midwifery, a number are delivered across NHS boards at SCQF levels 6 and 7, including the support worker pathway and non-clinical modern apprenticeships in administration and management. They are available to employees working in the NHS and social care settings. A modern apprenticeship framework should be responsive to employer demand and be oriented around current skills needs. Funding is provided by SDS direct to training providers such as FEIs and employers.
- Graduate-level apprenticeships: these are now in their second year in Scotland and are developed in partnership with HEIs and others. While the orientation is more academic than the other two apprenticeships, they remain employer-led, and are developed in response to clearly defined employer need. Graduate-level apprenticeships, like the other two forms, are completed within employment – in other words, those on the graduate apprenticeship route are in paid employment while they study. Funding is provided by SDS direct to HEIs.
All apprenticeships, and SVQs used by the social service sector, have National Occupational Standards, as developed by the Sector Skills Councils, at their heart.
The Review of the 15–24 Learner Journey programme of work is led by the Scottish Government in partnership with stakeholders and aims to review the effectiveness and efficiency of the learner journey for all 15–24-year-olds. There are two drivers for the review: learner personalisation and choice; and system efficiency. The review will consider the journey from the senior phase (S4–S6) leading to employment, including stages of further and higher education in FEIs, higher education in HEIs, vocational training and apprenticeships. The learning phase of the review did not conclude in sufficient time for the Commission to formally draw on its conclusions in making recommendations, but it is recognised that there will undoubtedly be important parallels between the work of the two reviews.
2.3.2 Access routes to nursing and midwifery (including for support workers)
The integration of health and social care poses challenges in terms of defining a common language across the new environment. The term 'healthcare support worker', for instance, is used commonly in NHS settings, but much less frequently in the context of care homes. Workforce data returns for care homes refer to just over 200 health care support workers/health care assistants/health care workers among over 50,000 care home staff records. In the care home sector, this key staff group would much more likely be referred to as 'support workers'.
The Commission found language differences such as this confusing and unhelpful. The more important consideration, however, is whether the public too finds it confusing and unhelpful. This is an issue that needs to be addressed urgently, and some of the report's recommendations seek to support efforts to make language and terms more simple and consistent across sectors, and to help the public understand what competencies and capabilities groups of workers possess.
The Commission took the view that for simplicity, and unless otherwise indicated, the term 'support worker' would be adopted as the default term throughout the report to encompass support staff with direct patient/client contact across the health and social care sector.
A range of routes by which candidates can ultimately gain access to nursing and midwifery degree-level programmes exists currently. They are nevertheless different across the professions. For instance, there is no acknowledged recognised prior learning ( RPL) route for HNC students into the second year of midwifery degree programmes, as there is in nursing: while HNC students are articulating into midwifery education programmes, they are doing so in first year, not second, and are tending to do so in informal ways without guarantees of places. This differs from the situation in nursing, and is primarily driven by the requirements of the NMC nursing standards and NMC midwifery standards.
Figure 1 shows the most common current routes into pre-registration nursing programmes. A more detailed description of routes is provided in Annex 2.
The figure highlights four key groups:
- people who already have a degree and apply directly to an HEI nursing programme; these applications are considered on an individual basis, and while it is conceivable that entry to a Master's programme would be granted, in practice it is very uncommon
- school-leavers: those with the requisite qualifications for HEI entry can join year 1 of an HEI programme; those who do not can enter FEI programmes, depending on their qualifications, where they will acquire appropriate qualifications and work experience, or directly enter the workforce through employment
- adult returners: this represents a wide range of people who may wish to change career or are not currently in employment, and who do not have the requisite qualifications; sometimes they have considerable life and work experience and wish to pursue a career in nursing through accessing an FEI programme (Scottish Wider Access Programme ( SWAP) Access to Nursing, National Certificate ( NC) or HNC, depending on qualifications)
- people currently in employment in health and social care settings: this includes childcare workers, NHS and care home support workers, social services workers and modern apprentices; they do not have the requisite qualifications for entry to HEIs and their common route is the HNC in Care and Administrative Practice, but they can also pursue an Open University ( OU) route.
Figure 1. Current widening participation routes
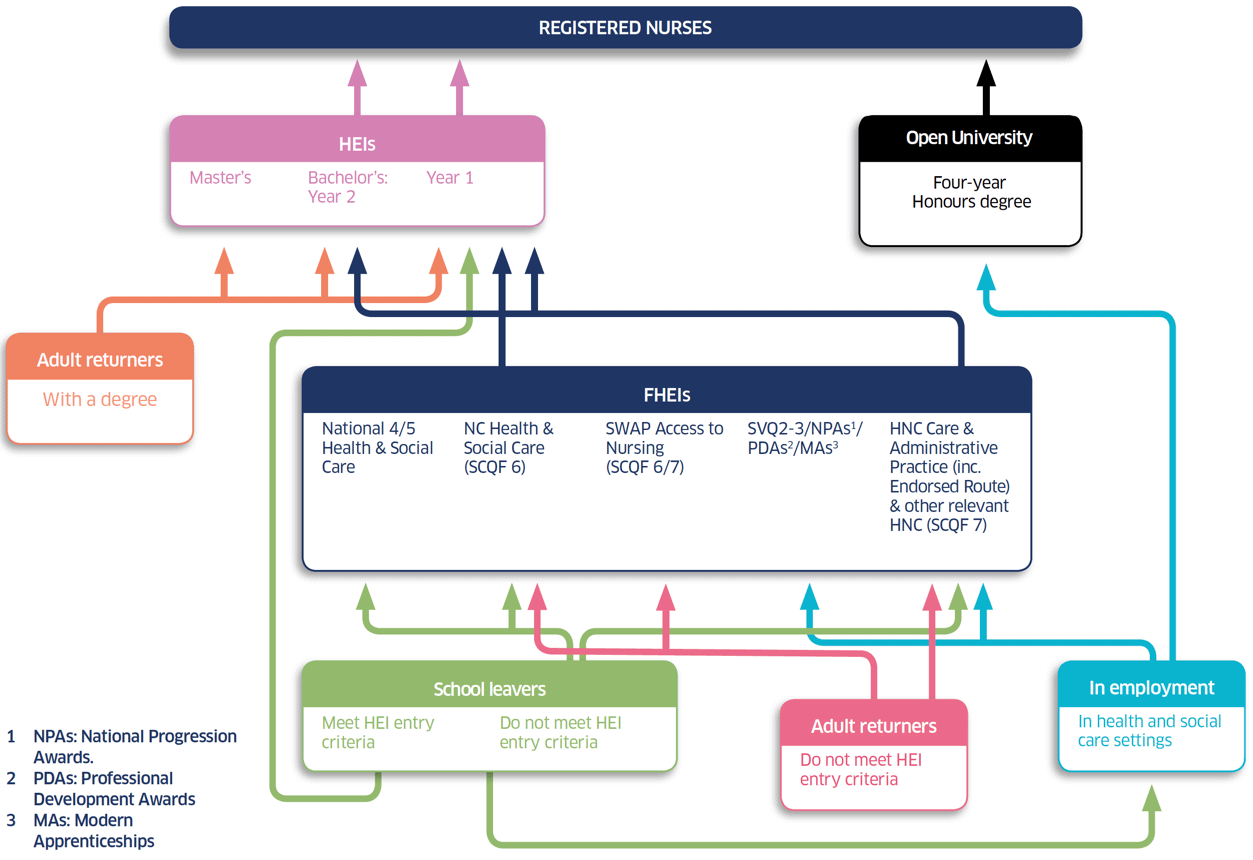
The college-based HNC route – with a number of places funded by the Scottish Government – articulates to year 2 (sometimes year 1) of the degree course, and other qualifications, such as the SVQ and Professional Development Awards ( PDAs), may be eligible for accreditation of prior experience and learning ( APEL), provided they are accredited by the SQA and mapped against the SCQF. Modern apprenticeships may provide significant funding opportunities for NHS boards in the context of the Apprenticeship Levy, though clarity is needed on the mechanisms and eligibility criteria for accessing funding.
There currently are no educational routes through which midwifery support workers can articulate directly to pre-registration midwifery education, which has a significant impact on access to the profession. No shortened courses to participation in midwifery education for qualified nurses are currently available in Scotland, although some are being planned.
Despite the establishment of integrated joint boards to commission and fund care for local populations, approaches to regulation of workers differ depending on their employer and/or their professional/work role. Many groups in the social care workforce, 69% of whom are employed by third or independent sector employers and the remainder by the public sector, are subject to statutory regulation by the Scottish Social Services Council ( SSSC). The SSSC has the role of the sector skills council in Scotland and is a non-departmental public body responsible to Scottish Ministers.
All support workers employed by NHS Scotland since December 2010, however, must sign up to the contractual employer-led model of regulation, which requires them to work to a set of standards and agree to abide by a code of conduct. The code and standards were reviewed in 2017 to ensure they remain fit for purpose in the context of changes to healthcare policy and delivery, including the integration of health and social care. The report from the review is currently going through governance mechanisms prior to wider discussion, but it seems likely that it will include recommendations on supporting access for support workers who wish to enter nursing or midwifery undergraduate programmes.
This issue has also been examined closely by the Commission, which found that support workers in other countries can and, in some cases, must go through an accreditation or certification process before they can practise. These processes may not be very complex, and may only equate to a period of intense induction. The Commission expects that support workers in Scotland must work towards achieving minimum standards defined by their employers prior to entering practice, but believes that integrated regulation for this group of workers needs to be explored further.
The SSSC's requirement for registration qualifications have work-based learning and adherence to the SSSC codes of practice as a central element; this includes evidence of 'observed assessed practice' and contrasts with NHS boards' educational demands for clinical support roles, creating parallel progression pathways along the largely vocational SVQ route and the more academic NC to HND route (including National Progression Awards ( NPA) and PDAs). While the SVQ qualification route allows RPL in work and from previous training, ideally there should be additional recognition mechanisms in place to facilitate sideways transmissions between these two paths.
The UK Department of Health announced in December 2015 the creation of a new role of nursing associate. The role was developed by Health Education England to address the workforce planning needs of NHS England, and the Department envisages nursing associates working alongside, and bridging a perceived gap in capabilities between, health care assistants and registered nurses. The role is attained through a graduate apprenticeship scheme, with an estimated 2,000 currently in training across 11 pilot sites in England. The first tranche of trainees is due to graduate in January 2019.
All three Devolved Administrations subsequently expressed reservations about introducing a role with a proposed scope of practice almost indistinguishable from that of a registered nurse and, in the absence of a comprehensive risk analysis, resisted statutory regulation on a UK-wide basis at this time. The Devolved Administrations are awaiting evidence of the efficacy and risk presented by the new role before taking a further view on its suitability beyond NHS England.
The principal reason for the introduction of the role in England – bridging the workforce gap between health care assistants and registered nurses – does not exist in such an obvious way in Scotland. The Scottish Government nevertheless recognises that the support worker workforce requires support to develop skills and academic growth to match the requirements of band 3 and 4 roles, and which will enhance their opportunities to articulate to nursing, midwifery, allied health professional or, indeed, social care undergraduate programmes.
Other issues in this area include:
- the SVQ 2 framework is workplace/competency based and requires learners to evidence the underpinning knowledge and values for each element of the SVQ, but people who hold SVQs experience lack of parity of esteem with those undertaking other routes to achieving learning
- while the SSSC has some data on retention rates for the social care sector, there are limited national or regional methodologies for following-up on what happens once people have gained a qualification – where they go and what their experiences are
- there is an appetite for a consistent national pathway of recognised, accredited qualifications; such a system potentially could provide vocational routes for progression and entry, both horizontally and vertically, into continuing education or employment.
2.4 Funding and support
Scotland has a wide range of funding and support mechanisms to enable people to access education and move either into careers generally or those specific to nursing and midwifery.
2.4.1 Education and careers
In relation to Further Education Access funding, the 2017/18 budget for college bursaries, childcare and discretionary funds is over £107 million. Further education students in 2017/18 will be able to receive a non-repayable bursary of up to £97.33 per week.
Scottish Funding Council ( SFC) access funding initiatives include: the Disabled Students' Premium; Access to Rural Communities; Access to High Demand Professions ( REACH); Schools for Higher Education Programme; Scottish Wider Access Programme ( SWAP); and the Widening Access and Retention Fund. Priority 1 of the SFC outcome agreement for 2017/18 states that widening access requires 'learning that is accessible and diverse, attracting and providing more equal opportunities for people of all ages, and from all communities and backgrounds.'
The Scottish Government will receive £221 million in 2017/18 as consequentials from the UK Apprenticeship Levy, which will come to Scotland through the existing Block Grant arrangements. Currently, the levy costs NHS boards in Scotland around £30 million per year.
2.4.2 Nursing and midwifery education and careers
The Scottish Government meets the costs of pre-registration training places through the SFC, providing commissioned HEIs with funding for provision of places. In the 2016/17 academic year, the Scottish Government transferred £56,815,659 to the SFC (unit cost £7,203). A further £1,160,159 was paid to commissioned HEIs to contribute towards Honours degrees (unit cost £1,820).
The Student Awards Agency for Scotland ( SAAS) assesses and pays the Nursing and Midwifery Student Bursary ( NMSB), which is a non-income-assessed, non-repayable personal allowance, and other associated allowances. All eligible Scottish-domiciled nursing and midwifery students can receive a core bursary of £6,578 per annum in years 1–3; for those undertaking an Honours degree, 75% of the NMSB (£4,934) will be paid in year 4, as this element of the programme does not cover the full 52 weeks.
The bursary is distributed to students by SAAS, but is not available to those who have previously undertaken a pre-registration nursing and midwifery course and received the NMSB. The NSMB was offered to 8,915 students in 2016/17, costing £55.1 million – this was 87.9% of all financial support to students. The level of the NMSB is being kept under review going forward; significant updates have been taken forward since the beginning of the review process, with the introduction of the Discretionary Fund (see below) in 2016/17, and measures to enable targeted support for children and dependants via an increase in means-tested associated allowances.
Students in receipt of the NMSB are also entitled to apply for an Initial Expenses Allowance of £60 (paid to 3,065 students in 2016/17, costing £0.2 million, which was 0.3% of all financial support offered), and means-tested allowances are available:
- Dependants Allowance – up to £2,640 for a dependant, and up to £557 for each other dependent child; it was paid to 1,125 students in 2016/17, costing £3.2 million, which was 5.1% of all financial support offered
- Childcare Allowance – up to £1,216 for registered childcare costs (in 2016/17, 805, £0.9 million, 1.4%)
- Single Parents Allowance – up to £1,303 (in 2016/17, 980, £1.2 million, 1.9%).
Following the first stage of the review into the effectiveness of the student support system in Scotland, these allowances were increased substantially from year 2017/18 with a view to ensuring increased support for students with additional responsibilities. Dependants Allowance is now up to £3,640; Childcare Allowance is up to £2,466; and Single Parent Allowance is up to £2,303.
The Disabled Students Allowance is available to students who have a disability or learning difficulty. It is a non-income assessed allowance to cover any extra costs or expenses related to the student's disability. In 2016/17, the allowance was offered to 375 nursing and midwifery students, costing £0.4 million (0.7% of all financial support offered).
Following the UK Government's decision to remove the health bursary and install a loans-based support package for nursing, midwifery and allied health professional students in England from academic year 2017/18, Scotland has withdrawn from the reciprocal agreement with the other three UK countries (r UK). This means that from 2017/18, students from England, Wales and Northern Ireland are no longer eligible to apply for the NMSB. These students from r UK are required to apply to their home country for fee and living-cost support. Students who were in receipt of the NMSB in 2016/17 are not affected by these changes.
Students from Scotland choosing to study in other UK countries will need to have a standard undergraduate package of a fee loan and a living-cost loan. For academic year 2017/18, the Scottish Government has agreed to fund students' tuition fees until systems can be set up in SAAS and the Student Loans Company to accommodate these loans.
A Discretionary Fund of at least £1 million has been set up to provide a 'safety net' for pre-registration nursing and midwifery degree students in most need. The fund is designed to enable them to access and/or continue in higher education and is paid in addition to any other forms of student support. The Discretionary Fund is allocated by Scottish Ministers and administered by individual HEIs.
All r UK nursing and midwifery students are entitled to apply for this fund. The maximum award to individual students is £2,500, but awards above this can be made available in extreme circumstances and with pre-approval by the Chief Nursing Officer Directorate.
To ensure nurses and midwives are fully equipped to undertake their placement experiences, funding is provided for placement expenses, uniforms, disclosure checks and health checks. Expenditure for 2016/17 was as follows: clinical placements, £1,690,000; uniforms, £197,660; disclosure checks, [19] £184,000; and health checks, £941,600. The Scottish Government has agreed to fund these expenses for r UK students choosing to study in Scotland in academic year 2017/18, but not thereafter.
In partnership with NHS boards, the Scottish Government provides support to widen participation for support workers, who traditionally may not have pursued careers in nursing, to enhance their skills and experience and further their careers if they wish. Specific programmes that aim to widen participation are spearheaded by the HNC Care and Administrative Practice, which has replaced the HNC in Healthcare as the national HNC qualification for gaining entry into year 2 of nursing degree programmes. Funding allows support workers to attend an HNC course at a local FEI on a part-time basis, while still being in employment. After year 1, if the support worker chooses to undertake an HEI degree in nursing, the following options are available:
1. the support worker may resign from her or his post and become a student in an HEI, gaining access to the NMSB (£6,578 per year), with the option of joining a bank or pool to earn money possibly being available
2. the support worker may resign from her or his post but agree an honorary contract with the employer and be paid an £8,000 NHS bursary; again, the option to join a bank or pool to earn money may be available
3. the NHS board chooses to continue to pay the support worker her or his normal salary for the period of the programme and the Scottish Government provides £8,000 per student to offset costs (£4,000 backfill per year for part-time students).
In 2016/17, 189 support workers undertook this route into nursing (118 new intakes on the HNC course and 71 continuing with the nursing degree). The breakdown of funding for the course from April 2016 to March 2017 is: HNC year 1, £576,000; and HNC years 2 and 3, £546,000 (total, £1,122,000).
These opportunities are advantageous to the student and the host board. The intended outcome is that students will maintain links with their host board throughout the programme and then work for them as registered nurses on completion. Presently, the route can only be accessed by NHS support workers, but it would be beneficial to widen access to include support workers from other sectors.
Feedback from some NHS boards that do not participate in this initiative highlights that the funding package, which has increased minimally since 2003 from £7,500 to £8,000 per student, is insufficient.
Support workers also have opportunities through a Scottish Government-funded Open University ( OU) programme that offers support workers in remote and rural areas the opportunity to undertake pre-registration nursing courses on a distance-learning basis.
Currently, the OU delivers a pre-registration programme for 91 nursing students in partnership with nine NHS boards and two GP practices (25 new students and 66 continuing students). One student is with Borders Council and seven work in four care homes.
Funding by Scottish Government is £10,000 backfill per OU student, plus costs incurred for tuition fees at £402 per month per student (teaching costs, support from practice tutors (including face-to-face meetings) and module materials). Total expenditure for OU training in 2016/17 was around £898,500. OU students do not have access to the NMSB with associated allowances for child care and dependants, however, and cannot access the Discretionary Fund. Due to the geographical location of most OU students, this may cause unnecessary barriers to a nursing career: the package of financial support for these students should therefore be reviewed.
The Scottish Government has commissioned the OU to take forward a care-home pilot in which support workers from care homes have access to the same pre-registration courses. Each care-home pilot student is supported by £5,000 of Government funding. To date, seven support workers are undertaking a nursing pre-registration course.
The Scottish Government remains committed to a national Return to Practice Programme, with a minimum £450,000 investment over three years to enable former nurses and midwives to retrain and re-enter employment. Returnees will have their HEI programme fees (£1,500) fully paid. To date, around 364 former nurses and midwives have taken up the opportunity to retrain, exceeding the initial target of 75 places per year.
All newly qualified nurses and midwives continue to be guaranteed one year of employment once they complete their studies, a commitment which is not offered anywhere else in the UK.
2.5 Rapid review of international and UK approaches
A rapid review of literature focusing on experience in Australia, New Zealand, United States, Canada, r UK and Ireland was conducted on behalf of the Commission by Dr Maria Pollard and colleagues from UWS and NES.
The review confirmed that many countries are facing similar issues to Scotland, particularly around recruiting and maintaining a nursing and midwifery workforce that is educated and reflects the population. Globally, there is a shortage of nurses and midwives due to demand being greater than supply. This is further exacerbated by an ageing workforce and increasing age of the population, which add complexities to health and social care planning and delivery.
Areas that require consideration in addressing this challenge, the review suggests, include: retaining nurses and midwives in the workforce; ensuring fair reward; improving the work environment; promoting flexible working patterns; providing clarity of access routes; recruiting from a broad and diverse population (including mature workers, ethnic minority groups, men, those with work-based vocational qualifications and non-traditional learners); encouraging return to practice; and recruiting internationally.
Australia, New Zealand, United States, Canada and Ireland regulate registered nurses, who are expected to be degree-educated. Australia, Canada, Ireland and New Zealand also have clear structures for recognising prior learning.
In England, as in Scotland, registered nurses are degree-educated and registered with the NMC. Care assistants have no registration, although a care certificate has been introduced. The Shape of Caring review (Raising the Bar), published in March 2015, [20] recommended the development of more innovative work-based learning routes and proposed a pathway for care assistants to enter nursing.
One to One, a community case-loading service commissioned by NHS England, has recently announced funding for nurses who wish to undertake the 'Midwifery short programme' – a 78-week programme giving nurses registered in the adult field the opportunity to undertake the pre-registration midwifery programme by an accelerated route and register with the NMC as a midwife.
The rapid review concluded that the Commission should promote:
- the development of clear definitions of target groups for widening access to pre-registration nursing and midwifery programmes to influence recruitment strategies
- mapping of current access routes to pre-registration nursing and midwifery programmes
- a review of alternative entry qualifications and admission processes of HEIs
- understanding of the current provision of flexible/non-conventional programmes (such as part-time).
The full report from the rapid review is reproduced at Annex 3.
2.6 Survey among students and registered nurses
The survey was carried out on behalf of the Commission, with the report compiled by Dr Rosie Stenhouse of the University of Edinburgh.
The purpose was to enhance the Commission's understanding of key areas relating to the choice of nursing as a career, information and accessibility of access routes/pre-registration nursing degree programmes and the interface between FEIs and HEIs from the perspective of students who had experienced entry into nursing via widening access routes, or aspired to enter nursing and were currently taking courses in FEIs.
Participants were current pre-registration students (n=20, including eight OU students), registered nurses (n=2) who had entered nursing through widening access routes (two male participants comprised this very small sample), and current students in FEIs (n=150) who aspire to enter pre-registration nursing degree programmes and are undertaking either the HNC Care and Administrative Practice or Access to Nursing courses in FEIs in a range of areas, including Highland, Perthshire, Glasgow, Edinburgh and Lothian. The sample therefore represents the student journey pre-, intra- and post pre-registration education.
Data was collected from focus groups and online surveys; the focus groups were run by FEI and HEI staff, and virtual focus groups were organised by the OU using their virtual learning environment. All data were collated and themes identified across the data set for each group of participants.
While the survey was small and cannot be claimed to be representative, it nevertheless sheds light on key issues from students' perspectives that influenced the Commission's focus as its work progressed.
2.6.1 Promoting the professions' attraction
The attraction for many of a career in nursing and midwifery was based on a rational recognition of the career opportunities presented in and outside the NHS. It also reflected a desire to make a positive impact on society, rather than following a vocational 'calling'. When asked ' What attracted you to a career in nursing or midwifery?', the most prevalent reasons were personal experience, perceived educational and career opportunities, and a desire to help/make an impact on society. FEI participants focused on helping on an individual patient basis, talking about 'want[ing] to help others', while those from HEIs and registered nurses spoke of 'making a difference' on a much wider, and possibly more political, level.
Participants identified the negative image of nursing often portrayed through news media and films/ TV and the impact this has on motivations to join the profession. One said:
'I think that media can show nursing in such a negative way, portraying poor wages and long working hours … [There needs to be] better advertising through social media as well as TV, targeting all ages, gender and ethnic minority.'
A need to promote the different routes into the professions to ensure wider understanding was also raised. Participants discovered these through a range of formal and informal means. There was a sense that more formal information needed to be made available: some participants identified that they had only found out about courses through word of mouth, or by being in the right place at the right time.
The diversity of roles and contexts in which nursing occurs was identified by many participants as attractive. One said:
'Nursing is a rewarding and challenging job and could provid[e] exciting and varied opportunities. It also offers routine and structure. The skills used in nursing can be used in a wide variety of formal and informal situations.'
Some felt that more needs to be done to promote this side of the profession, including the fact that nursing is not provided exclusively in the NHS. For example:
'Advertise the wide range of jobs on offer once qualified such as the forces, cruise ships or simply the different jobs that can be done within the NHS itself … I'm sure many people don't realise what is available.'
Participants spoke of the need to move beyond the concept of nursing being for young women and wanted institutions actively to promote diversity in nursing through a greater emphasis on advertising to men and older male/female students, rather than pursue exclusively its perceived heavy focus on younger school-leavers. They also talked about the need to promote a realistic view of nursing, suggesting this could be achieved through offering work-experience opportunities, advertising and ensuring that TV programmes that involve nurses are realistic. One said:
'When it comes to young students tell them what to expect on placement, tell them how much work it takes so they know where [they] stand. Show the best parts of nursing too, the thankfulness that patients show and how rewarding the profession is.'
Identified barriers to entering nursing and midwifery education and careers included:
- financial, particularly for mature students who may have family responsibilities and perhaps had to give up paid employment to become students; other financial issues, such as travel costs to get to HEIs and limited employment opportunities while studying, were also considered important barriers
- self-doubt and lack of confidence in negotiating HEIs' admission procedures
- inappropriate home circumstances with inadequate opportunities for study (lack of good wi-fi access in rural communities, for example)
- the gendered nature of nursing, with men not perceiving nursing and midwifery as 'male' professions
- inconsistent information about the qualifications required, particularly around numeracy, and more generally a lack of (or inaccurate) information in schools and colleges.
Summary
- Students made choices to undertake nursing and midwifery education based on opportunities offered.
- Information was gained through formal and informal routes.
- Prospective students had a particular focus on the diverse contexts of nursing and midwifery.
- Wanting to make a difference remains a strong driver for students.
- Concerns about the financial impacts of being a student were identified as a barrier.
- The gendered perception of nursing and midwifery was seen as a barrier to male applicants.
2.6.2 Application processes
Responses identified either that participants felt supported when making their application and it was therefore a positive experience, or that it was a positive experience because they found the process straightforward. Those who had difficult experiences had found themselves lacking confidence, or there had been a lack of clarity/consistency in the available information. Some identified that lack of consistency in entry requirements between HEIs made the application process more challenging; additionally, some had been required to undertake numeracy tests, but found this process anxiety-provoking due to lack of clarity and communication.
Most of the current pre-registration students and registered nurses felt well supported in the application process, finding college staff helpful when completing Universities and Colleges Admissions Service ( UCAS) forms; having an articulated place onto year 2 of a nursing programme was considered a positive impetus for students' work at college.
In relation to improving the ease with which people can apply to HEIs, some students found that having previous healthcare experience helped at interview stage, but were unsure about its effect overall in the application process. Despite HEIs and the NMC supporting the RPL process, no participants identified that previous experience had been taken into account in lieu of academic qualifications or enabled accelerated access into pre-registration nursing degree programmes. One respondent identified that despite having experience in caring, it was not taken into account because it was not in the same field of nursing to which the person was applying.
Summary
- Generally, students who came through the FEI system felt supported in making UCAS applications.
- The UCAS system was easy to follow.
- The diversity of entry requirements for individual HEIs was difficult to navigate when applying.
- There is a need for consistent information, particularly around numeracy.
- Despite many participants citing extensive experience in healthcare settings, none identified that this was formally recognised
2.6.3 The journey to higher education
A number of FEI students who had undertaken a module aimed at supporting the transition into higher education felt the design, alignment and coherence of their learner journey – their experience of moving into higher education – was well supported, as did one who had been a pupil of the Advanced Higher Hub prior to moving into nurse education. The access and HNC courses were identified as providing relevant graded content (such as Highers) as well as practice placement experience. One participant noted:
' HNC prepares you greatly by giving you underpinning knowledge, simulation sessions and placements.'
Some participants pointed to the support experienced through various schemes to bridge the gap between school/ FEI and HEI. One commented:
'Some students felt having a summer placement transition module help[ed] them prepare more for the complexities of practice and they felt that the lines of communication between the colleges and the HEI were good.'
The ability to re-enter an educational context, enabling students not only to regain academic skills but also to develop other skills required to manage the learning experience, was also appreciated by some participants.
Others, however, felt less prepared and supported, particularly in relation to preparation for academic writing and other study skills (a participant noted: 'College did not teach correct essay writing skills or adequate referencing skills'), and one did not feel the HNC course provided adequate preparation for transitioning into the second year of a BSc course. One of the registered nurses suggested that increased contact with practice education facilitators during the HNC course might have better supported transition to year 2 of the degree programme, and proposed more flexible and reduced contracts with the NHS while students are undertaking their studies.
Barriers to progress once on programmes included financial pressures, difficulties accessing funding for those coming from care homes, anxieties about course content triggering cathartic reactions to events in their personal lives, self-doubt and problems meeting demands for study, work, family/friends and recreation.
Participants found themselves juggling a range of responsibilities and demands on their time. Their comments included:
'Health, family and domestic difficulties can impact at different levels throughout your time on the programme.'
'Barriers for me are mostly time management v working. I think I may have to spend more time on my assignments as I can spend a lot of time reading. I also work full time which I require to pay bills etc.'
Participants were asked how they had overcome these barriers. Their responses were scattered across a range of individual strategies, such as developing a routine and planning ahead, learning time-management skills, asking for help from tutors and managers, and increasing the amount of paid work they took on. Interestingly, the students' perceptions of means of reducing barriers did not include any actions by HEIs – all involved changes to their own approaches.
FEI students identified the high relevance of their HNC/access experiences in terms of giving them what they needed to get into nursing and midwifery courses, particularly in relation to issues such as promoting understanding on how to deal with people in different situations, recognising diversity and treating each person as an individual. These experiences also helped them to develop their academic skills and provided access to care placements. The students felt the reputation of the HNC as a stepping stone to university, and the success of previous HNC students on HEI courses, was very encouraging to them.
Summary
- Students on access and HNC routes perceived these courses as being designed to gain them access to a pre-registration nursing degree programme, but competition for places on pre-registration programmes was demotivating.
- The lack of clear articulation routes into year 2 of pre-registration programmes increases financial pressure on students who repeat the year they spent on the HNC.
- The journey into higher education can be smooth if students are supported and prepared, particularly in relation to academic skills.
- It is not, however, possible to assume that HNC or other college courses adequately prepare students for study at higher education level.
- Financial and time pressures put students’ progress at risk.
2.6.4 Income sources
Most of the students received the NMSB, but some had concerns that it was too little, especially when childcare and other costs were factored in and when the fact that some mature students had had to give up paid employment to undertake their programme was considered. Comments included:
'It would be very difficult to rely on the bursary alone – I still work part time all year round to cover the costs of things.'
'Childcare – not enough funding to cover cost of hours in college and placements.'
'Mature students with children giving up jobs don't receive enough funding from colleges to cover costs.'
The need to earn money over and above the NMSB was a commonly cited pressure, compounded by difficulties fitting in paid work around the demands of an intensive degree programme. As one participant noted:
'Fulltime nature of the programme makes it difficult to e.g. over the summer to earn money to make yourself more financially prepared for the next year as you are on placement over the summer unlike other programmes.'
This pressure was not experienced by OU students, who identified that they were paid during their time as students, but they experienced difficulties getting time to study due to lack of support from colleagues.
The students were nevertheless aware that the situation in Scotland is different from the rest of the UK and that they were fortunate to receive the bursary, which provided them with a significant sum of money. Additional funding sources were also recognised and accessed; some participants had received support that included hardship money and income support.
There was a suggestion of funding disparities between those coming into nursing and midwifery education from the independent sector and those from the NHS, with one student with a care home background saying that she was made to feel 'second-rate': this student was denied access to computers at a local hospital and told she could only borrow books while on placement 'because I was from a care home'. She called for future students to be 'encouraged, not segregated, because [they] work in a care home.' OU students who were employed in care homes were aware that the money received by the homes to cover their training was lower than what was paid to the NHS, and that there were other inequalities between the sectors. One commented:
'What I am concerned about is the lack of funding available to private care homes compared to the NHS. I didn't realise that until we did the Induction Day. So I'm disappointed in that – are we not worth as much?'
Overall, students found the SAAS funding process helpful and informative and were paid on time. This reduced financial stresses, although delays were experienced by some, particularly for travel costs when on placement. Some participants from FEIs, however, reported difficulties with their funding and stressed that late payments could result in applicants having to withdraw from programmes:
'Having to chase SAAS means some drop out as [they] cannot manage the first few weeks without money.'
It is worth noting, however, that SAAS operates a guarantee date: where an application is received before 30 June, funding will be in place for the start of the course.
SAAS has further reported to the Commission that it successfully processed an increased percentage (96%) of bursaries within 21 days over the agreed targets in 2016/17.
Summary
- The main source of income was the NMSB.
- The NMSB does not meet participants’ living costs. Childcare costs and increased costs of mature students with dependants are particular pressures.
- While the number of respondents was small, some FEI students reported experiencing later payments from SAAS than their colleagues on pre-registration nursing programmes.
2.6.5 Conclusion
The survey concluded that there needs to be a focus on:
- developing positive but realistic public perceptions of nursing and midwifery, including its gendered nature
- promoting diversity of nursing and midwifery roles and opportunities in careers
- addressing students' financial burden, particularly for mature students and those with dependants
- continuing to learn from good practice in supporting transitions between FEIs and HEIs
- ensuring clear and accessible information about routes into nursing and midwifery and that there is parity of esteem with direct-entry students
- supporting articulation into the second year of programmes for those coming via FEIs.
2.7 Examples of emerging approaches and pilots
Work is already underway in different parts of Scotland to put in place initiatives aimed at widening participation in nursing and midwifery education and careers. The Commission recognises this work and sees it as a solid platform from which to launch its observations and recommendations. Some examples of current initiatives are presented below.
2.7.1 Nursing access courses – OU pilot
The Scottish Government provided over £27,500 funding in October 2017 for a pilot in Grampian to widen participation in nursing education and help increase development opportunities for clinical support staff. The OU pilot is supporting 24 NHS Grampian support worker staff to undertake access courses in literacy and numeracy to enable them to achieve qualifications that may assist in applications for further study at HNC or degree level.
The numeracy qualification ( SCQF level 5) for the pilot will be undertaken through the North East Scotland College ( NESCOL) and the SCQF level 7 'Introduction to Health and Social Care' (K101) course with the OU in Scotland. This will enable staff to develop in their careers, irrespective of their educational and social background.
The pilot will be evaluated with the intention of widening the opportunity to support workers in the broader health and social care sector.
Clinical support staff are attracted into this route for a number of reasons, including:
- the accessibility of the distance learning model, particularly for those living and working in more remote and rural areas and people with caring responsibilities
- the part-time route of study offered, which is viewed as providing a better option for people who are otherwise unable to access full-time FEI- and HEI-based study routes
- maintaining security of employment, particularly where family commitments or financial constraints have prevented support workers from considering the HNC Care and Administrative Practice route to nursing.
2.7.2 Primary 7 schoolboys' taster day – Robert Gordon University ( RGU)
The RGU School of Nursing and Midwifery hosted a taster day for Primary 7 schoolboys from five feeder schools linked to a Fraserburgh secondary school. The initiative represents one aspect of RGU's wider gender work.
Seventeen boys attended. They spent the morning in the skills lab learning basic life support skills and getting experience of taking temperatures and blood pressures, bandaging, working with the robotic manikin and examining equipment. In the afternoon, they had a one-hour session with mental health nurses.
The day was supervised by male nurses from the School with backgrounds in adult, children and young people, and mental health nursing and who have diverse professional experiences. The boys had opportunities to ask questions when they first arrived and throughout the day. They were interested, vocal and inquisitive, asking about issues as diverse as pay, career structure, 'best and worst bits', death and negative public perceptions.
The session evaluated positively; all the boys said they enjoyed the day and had learned a lot about nursing. The head teacher and accompanying staff said they had also learned about nursing as a career and felt better equipped to advise pupils in the future.
Most interesting to RGU staff was that the head teacher said more boys had wanted to come to the day, but some parents had been reluctant to sign the consent form, perhaps highlighting the challenge nursing faces as a career choice for males in rural communities.
RGU hopes to be able to link with these schoolboys again in the future. Third-year pupils from a city secondary school are also invited to take part in the delivery of two modules in the School, and children comprise part of the interview selection panel for the children and young people's field programme.
2.7.3 Attracting men into nursing – University of Dundee
The recruitment rate for males into undergraduate nursing education at the University of Dundee currently is 8%. Attracting more males into nursing is part of the School of Nursing and Health Sciences' action plan, and staff have instituted a number of strategies aimed at increasing the proportion of males to 25% and, ultimately, achieving gender parity.
A pop-up stall was held in September 2017 in a local shopping centre involving male nursing students, lecturers, and staff from the local hospital and FEI who could advise about access programmes for applicants who lacked the necessary qualifications for HEI entry. The event was run in conjunction with a social media campaign using the hashtag #MenDoCare. The publicity from #MenDoCare led to further exposure on radio and in newspapers, and an online article on men in nursing written by one of the HEI lecturers has created much interest.
Two focus groups have been held with local male nursing students to explore facilitators and barriers to embarking on a nursing education route. Results are being analysed to inform future plans.
A male nursing student, admissions lecturer and a member of staff from the local FEI attended an event for guidance teachers in September 2017 to promote nursing as a career option for a wider group of potential school-age applicants, including males.
Staff from the Developing the Young Workforce programme have met with the HEI to discuss its campaign to encourage more male school-leavers into jobs in care. There is an enthusiasm to develop joint interventions in schools at S2/3 and revisit them in S3/4, and in exploring a primary school intervention.
A collaborative project co-led by one of the School's midwifery lecturers and involving the University of Edinburgh, UWS and RGU is currently applying for funding from NES to explore the influences and causes of underrepresentation of men in nursing in Scotland, with a view to recommending ways of influencing recruitment and planning.
2.7.4 Nursing and midwifery summer school programme – RGU and NHS Grampian
The summer school programme for senior secondary school pupils aged 16 and over is designed to provide interested young people with a realistic and comprehensive experience of nursing and midwifery education to inform their decisions about whether they represent the right career choice for them. The programme is not a hands-on work experience, but is one of a range of local initiatives designed to address pre-registration education recruitment and retention challenges.
The educational experience enables participants to:
- explore what the professions are
- learn and practice some core skills in the clinical skills centre
- undertake some simulated practice with volunteer 'patients'
- observe healthcare work in real clinical settings
- interact with nurses and midwives in clinical settings
- experience higher education and healthcare provision at first hand.
Applications are invited through guidance teachers in the Grampian and Moray areas. Twenty students were selected from Grampian and eight from Moray for the 2017 programme: it is very popular with pupils and is oversubscribed, so a reserve list is held.
The programme has evaluated well, both verbally and through a final day exercise. When asked 'What surprised you?' about the experience, responses from participants on the 2017 programme included:
- 'That I enjoyed the adult hospital and would now consider it as a career'
- 'The different specialties in nursing and the number of pathways you can take'
- 'Hearing a lot about mental health conditions and hearing the interesting stories and facts about it'
- 'How strongly I'm stuck on wanting to study children's nursing'
- 'That I decided what career path I wanted to take … finally'.
In addition to highlighting interest in clinical areas such as oncology, mental health, paediatrics, theatre and maternity, responses to a question on what they found most interesting in the experience revealed that participants appreciated:
- 'Seeing how the different types of nursing were similar and different'
- 'How much experience you can get on placement'
- 'The range of career paths available in nursing'.
A retrospective study of outcomes from participants at the summer schools in 2015 and 2016 found that of the 28 participants at each programme, 11 were studying nursing or midwifery at RGU.
2.7.5 The Health and Social Care Academy
The Health and Social Care Academy, the only academy of its kind in Scotland, has been running for the last four years for young people in S5 and S6. An initiative of Queen Margaret University, Edinburgh, and Edinburgh and Borders College, the overarching title is the South East Scotland Academies Partnership ( SESAP). It includes young people from Edinburgh, East Lothian, West Lothian, Midlothian, Borders and Dumfries and Galloway.
Young people gain a qualification on completion of study (National 5 after one year and Higher grade after two). Students can start the National 5 in either S5 or S6, but those taking the Higher need to start in S5. The academy is an option within school curricula, with young people attending the FEI for two afternoons per week and the HEI for four sessions in the year.
The approach focuses on heightening young people's awareness of the range of career opportunities available in health and social care, including nursing, midwifery and the allied health professions. The academy enables them to acquire knowledge and relevant work experience to prepare them for study and work in health and social care. The aim is to help the young people develop transferrable skills that will make them attractive to future further and higher education providers and employers and also help to smooth the transition between school, FEI/ HEI and employment. At the end of the course, graduates are in a good position to pursue a health-related course in an FEI or HEI or apply for work in health and social care.
A recent survey of academy students found they acknowledged the positive influence of the academy on their social, communication and independent learning skills. It was seen as providing a potential way to widen access to higher education and help students make more informed choices, increase their achievement and lower dropout rates in HEIs.
2.7.6 Modern apprenticeships in NHS Lothian
NHS Lothian has started to recruit modern apprenticeships into the nursing service. Twenty-two band 2 posts were advertised in two rounds across the mental health and learning disability service and Royal Hospital for Sick Children (outpatients, medical ward and paediatric intensive care unit). Thirteen posts were appointed in round 1, with interviews for remaining posts to be held in November.
The recruitment process adopted a partnership approach and involved a range of activities, including 1:1 interviews and group values exercises. It was based on a 'future potential and personal attribute and values' approach, with no education requirements set. Advertising focused on social media (Twitter, Facebook, NHS Lothian Career Pages) and partnerships with youth groups to spread the word.
The response was unprecedented for the board, with 39 applications submitted in one night. Applications closed early due to the response (150 applications in three days, with 95,000 hits on Facebook, 800 shares and 300 comments all tagging friends to the advert).
The modern apprentices started in mid-November, with education delivery starting in March/April following completion of induction and some job experience. The aim is to complete the apprenticeship in 12 months from employment.
This level of response contrasts with a steep drop-off in applications currently seen for band 5 posts in the board and suggests that modern apprenticeships may offer an important route for widening access.
2.7.7 University of the West of Scotland – MSc Midwifery
The MSc Midwifery with registration was validated in 2013, representing the only midwifery programme underpinned by master's-level education in Scotland at this time. It is an exciting and unique postgraduate pre-registration three-year midwifery programme run in conjunction with the BSc Midwifery at UWS and enables students to become highly educated midwives with the potential for management, leadership, consultancy, education and research roles.
The programme was developed in accordance with the NMC Standards for Pre-registration Midwifery Education. Students with a first degree can apply for the programme, which comprises 50% theory and 50% practice over a three-year period. All modules are core and a dissertation is undertaken in year 3.
The programme offers the opportunity for practice learning experiences across wide geographical and specialty areas, ranging from large tertiary consultant-led units to remote and rural community midwifery units. It has a dual exit qualification, with the educational level at MSc and a NMC professional qualification with entry to the register as a Registered Midwife.
The midwifery programme acknowledges the centrality of professional practice to the midwife's role and that providing care for women with both normal and complex pregnancy and childbirth can be highly challenging. It addresses current challenges facing maternity services, including vulnerable groups, sexual health, mental health, obesity and social inclusion, and seeks to produce inquisitive, innovative thinkers who understand, develop and enhance concepts of person-centred, compassionate care for childbearing women and their families.
Delivery of knowledge includes teaching at a more advanced scholarship level using a planned programme of additional tutorials and seminars to facilitate greater breadth and depth of the student's experience. This includes a wider perspective on issues such as management, leadership, clinical governance, education, research and development of new insights. The programme aims to prepare students to consider post-doctoral studies as well as project management and leadership, postgraduate teaching and learning, and specialist consultant clinical midwifery roles.