Children and Young People's Mental Health Task Force: recommendations
Recommendations from Children and Young People’s Mental Health Task Force to Scottish Government and COSLA.
Getting it right for every child with mental health support needs: A whole system approach
Most of the time, children and young people should experience good mental health, along with the normal challenges and stresses of growing up. They should benefit from positive and helpful support for their wellbeing at home, in the early years and at school, and they do not require any extra help over and above that from the people they see day to day.
Many children and young people may need extra help at some point and some could need additional or specialist support. This may be because of factors relating to the child's development or health profile or it could be because of the impact of adverse experiences on the child, family or community. If required this help should be delivered in line with the GIRFEC approach and 'National Practice Model'.
Additional support should be provided promptly, wherever possible within universal services and the community, and should be proportionate to the level of need and risk. Where this is not possible there can be no 'wrong door' for children and families who need to receive extra help – they should only have to ask once to access services. Wherever is requested, for example through school or from a GP or Health Visitor, there should be a helpful and appropriate response - bureaucracy or organisational and professional boundaries should not get in the way.
The voice of children, young people and families should be central to the identification and assessment of needs, and in the determination and delivery of the help that is provided. Shared decision-making will increase the likelihood of successful outcomes.
Recommendation 4: The Task Force endorses a whole system approach to addressing children’s mental health needs, ensuring preventative action to reduce need, and a prompt and proportionate response which improves outcomes for all children who need support or treatment.
The Taskforce believes a whole system approach involves addressing the mental health and wellbeing needs of children, young people and families in an integrated way across the groupings shown below.
Workstreams have collaborated in a bid to ensure recommendations meet the needs of children and young people with a range of needs within the whole system, including those at risk of not receiving a service and those with neurodevelopmental support needs.
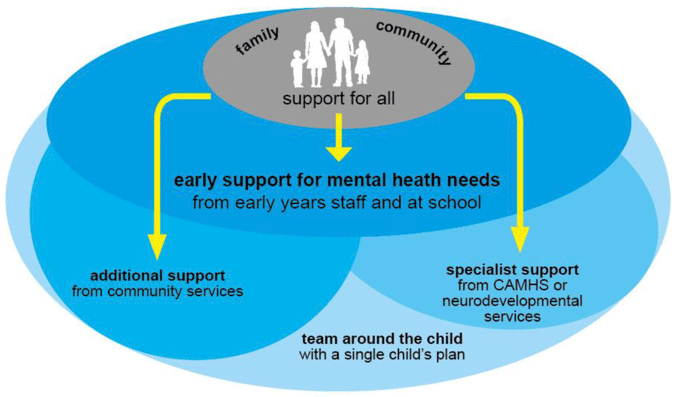
Support for All
Positive mental health and wellbeing is promoted with families and young children throughout the early years. This continues into school, with the focus on health and wellbeing within the Curriculum for Excellence.
Midwives, Health Visitors and other partners work with parents and carers to support the healthy development of the baby and young child. Critically, this includes promoting strong early attachment, involving positive engagement and interaction with the primary carers.
When children go into school, learning in health and wellbeing ensures that they can develop the knowledge, skills and capabilities they need for mental and emotional wellbeing. This includes support for young people to make informed choices to promote their own wellbeing, and to establish a healthy lifestyle that can be sustained into adult life.
A key focus should be on the capacity building of staff who work with and support children and young people.
Early Support
Many children, young people and families experience mild and/or temporary mental health difficulties at some time during childhood that can be responded to early and effectively by GPs, Health Visitors, School Nurses and school staff or other significant adults with whom they have a supportive relationship.
This early support can be in the form of advice and guidance, including signposting families to information or supportive activities. Information can be shared in a way that empowers young people and families to find the best ways of supporting their own mental health and wellbeing. Increasingly, good use can be made of helpful online resources. Good quality support at this stage can help reduce referrals made to other parts of the system, therefore impacting on wait times and helping to prevent emotional distress and mental illness need from escalating.
Health Visitors and education staff can also provide early support through making changes or enhancements to how they support the child and family. This might include one to one activities including counselling or group work, for example with Health Visitors organising a parenting group, or guidance staff organising a group for those who need support.
Additional Support
Some children and young people may require additional support for a mental health or neurodevelopmental need to achieve positive mental health outcomes. This support should be determined by a practitioner with a strong understanding of mental health provision within a community setting, such as; a Primary Care Mental Health Worker, Psychologist, Educational Psychologist, School Nurse or Family Support Worker. It can be provided directly by that practitioner, or by other colleagues within the team around the child – for example, school or social work - and should be evidence based.
Such support should be part of an integrated approach to help the child, based on assessed need, and set out in a child's plan. It should be asset based, building on strengths in the family and other local networks, and should be clear on what a successful outcome would look like.
Specialist CAMHS Support
A small number of children and young people experience mental illness or other mental health needs that require focused, evidence based assessment and interventions from specialist Child & Adolescent Mental Health teams. This includes children, young people and families who would benefit from a range of interventions, including specialist community treatment and/or in-patient services.
Once again, such support should be provided as part of an integrated approach, with a team around a child, and with the interventions set out within a child's plan. Given the nature of the needs and interventions, and the key role families play in their treatment and recovery, it may be necessary for some aspects of the plan to remain confidential to the child and family and a core group of practitioners.
It should always be clear what outcomes are being sought, and what additional services will be required once the child no longer requires a specialist service.
Core components of the whole system approach
There are five core components of a whole system approach to meeting the mental health needs of children and young people:
1. Clear points of contact for children, young people, families and practitioners who have concerns regarding a child's mental health through the Health Visitor, School or GP to where advice or access to support is available.
2. An early response to the first concerns or signs of distress, with prompt, proportionate and informed assessment that determines the response, without unnecessary delay or bureaucracy.
3. A clear pathway through services, with a focus on prevention and early intervention within the community, and an accelerated path to additional, higher level or specialist support or treatment whenever that is required.
4. Children, young people and their families at the centre, empowered to express their views regarding their needs and services, and to have these views acknowledged and recorded.
5. Mental health needs integrated into any support for other needs that a child may have, as part of a single plan with a team around the child that is co-ordinated by a lead professional.
This approach must be underpinned by local partnerships. Every local partnership should ensure this whole system approach to meeting mental health needs within GIRFEC, that incorporates agreed service standards and involves:
- Collaborative management and professional leadership of mental health interventions and services, from universal to targeted provision.
- Easy to access, clear points of contact for children, young people, families and practitioners who have a concern about a child or young person's mental health, where advice or access to support is available.
- Early support for children and young people who experience distress, delivered in universal services and by those who know children and young people.
- Dedicated support for children and young people who require community based mental health services as part of additional and integrated support from a range of partners.
- Prompt access to CAMHS and Neurodevelopmental services for children whose needs cannot be met without more specialist support.
- The organisation of a child's plan for all children who require co-ordinated multi-disciplinary support, by a lead professional.
Partnerships should also ensure that support is available to children and young people who may be excluded from mental health services, such as children with neurodevelopmental profiles and support needs, or those who are facing multiple challenges in their lives in addition to their mental health needs.
What does this look like in practice?
Integrated working based on a common language built around the whole system model.
- Use the SHANARRI wellbeing indicators to describe needs.
- Use the National Practice Model, with clear points of contact for children and families, and co-ordinated support and planning from the lead professional.
- Ensure appropriate information sharing, wherever appropriate with consent of the young person and/or family.
- Ensure a high level of respect and confidence for and from practitioners from other disciplines.
- All children receive prompt and appropriate mental health support to meet their needs, including those with neurodevelopmental profiles who require support and those who are facing multiple challenges in their lives, where traditional treatment approaches may not be considered effective.
- Practitioners share the accountability and responsibility when managing risk.
- Mental Health Impact Statements are included when decisions are made in multi-disciplinary meetings e.g. looked after and adopted child's meetings.
Mental wellbeing, and early and community based support are prioritised.
- Focus on active prevention and health promotion strategies.
- Support children, young people, parents and carers to have conversations around mental health and neurodiversity with practitioners they already have a relationship with.
- Encourage evidence based parenting programmes and family support, a whole-family focus, which can be delivered by a range of practitioners.
- Promote whole system, multi-disciplinary support for children who require additional support.
- Provide accessible 'one-stop' integrated services in communities where young people would make use of them.
- Facilitate early help seeking and collaborative intervention strategies that consider professional, self-help, peer support and community interventions.
Children, young people and families are involved in shared decision making around their own mental health and wellbeing.
- Emphasise the range of self and community approaches that do not involve the input of mental health professionals.
- Prioritise shared decision making which actively engages children and parents/care givers.
- Build interventions around collaboratively agreed plans.
- Discuss and monitor the outcomes that are being sought from the outset.
- Develop agreed approaches to reduce the level of support and intervention.
Contact
Email: Hannah.Broadley@gov.scot