Chief Medical Officer's Report Part 2: The Health of the Nation
The second section is a report card which presents the surveillance data on the health of the nation. The report contains a summary of the data. These can interpret trends to inform how we continuously improve our management of health and disease
Communicable Diseases
Vaccine Preventable Disease
The Scottish Immunisation Programme continues to develop in response to newly available vaccines and emerging threats.
Since the beginning of 2014, immunisation programme developments include:
- offering seasonal flu vaccine to all children from age 2 years to the end of primary school;
- introducing vaccination against Meningococcal B disease for infants;
- expanding protection against meningococcal disease for adolescents with the introduction of ACWY vaccine for those aged 14-18 years and new university entrants;
- continuing with the phased catch-up programme for herpes zoster (shingles) vaccine for those aged 70-79 years.
These developments mean that over 2 million vaccines are now offered every year to protect the population of Scotland. The programme is delivered by colleagues in Scottish Government working closely with Health Protection Scotland, NHS Boards and primary care. Immense benefits are already being seen and we continue to monitor impact against more recently introduced vaccines.
Meningococcal disease
Meningococcal disease, caused by the bacteria Neisseria meningitidis, is an important cause of morbidity and mortality in Scotland, particularly among children and young people. In the first 6 months of 2015, 38 cases were reported, similar to the same period in 2014, in which 73 cases were reported for the entire year. Serogroup B continues to dominate, but as for elsewhere in the UK, cases of serogroup W have risen markedly, including an outbreak of four cases associated with Scouts returning from an international camp. New vaccination measures against both Group B and W disease have been put in place and are under evaluation.
Healthcare Associated Infections and Antimicrobial Resistance
Healthcare associated infections (HAIs) continue to represent a threat to safe care, wherever that is delivered. HAI place a significant financial burden on NHSScotland with HAI originating in acute care estimated to cost the NHS in Scotland £137 million annually. The recently acknowledged global issue and threat of antimicrobial resistance (AMR) means that prevention and control of all infections is a key continuing requirement in healthcare to minimise the need for antimicrobials, in addition to good stewardship of antimicrobials when required. HPS routinely monitors the incidence of key selected HAI, as follows:
Staphylococcus aureus bacteraemia
During 2014, a total of 1,567 cases of Staphylococcus aureus bacteraemia including 141 (9.0%) meticillin resistant S. aureus (MRSA) were reported. This represented an annual incidence of S. aureus bacteraemia of 30.4 per 100 000 acute occupied bed days (AOBDs). This was not significantly different compared to the previous year.
Figure 1: Overall quarterly S. aureus, MRSA and MSSA bacteraemia incidence rates for Scotland (per 100 000 AOBDs) for the period Q3 2010 to Q2 2015.
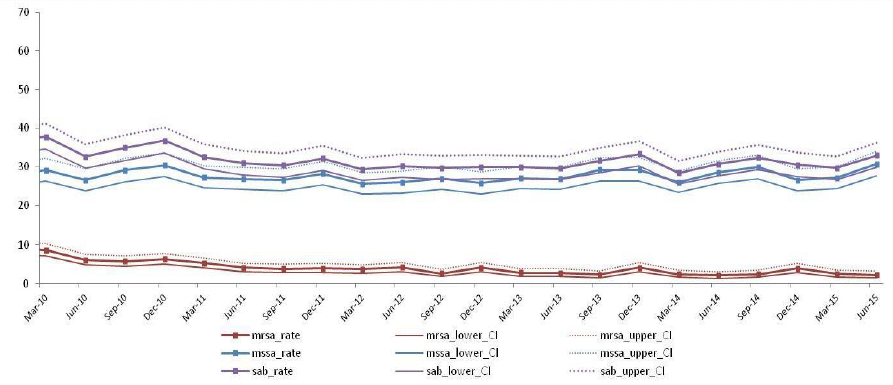
Screening for antibiotic resistant organisms on admission to hospital is one of the key infection prevention activities in acute care. A national MRSA screening policy has been in place in Scotland since March 2012. Compliance with application of the Clinical Risk Assessment is a level 3 HAI Key Performance Indicator, which was introduced in 2013. The compliance, reported between January 2014 and June 2015 was 79%, below the Scottish Government Health and Social Care Directorate (SGHSCD) target of 90%. The current screening policy with this level of compliance remains clinically and cost-effective when compared with universal MRSA screening, due to the added benefits of pre-emptive isolation and significantly lower cost of CRA
Surgical Site Infection (SSI)
The incidence of SSI (inpatient and post discharge surveillance (PDS) to day 10) following Caesarean section surgery decreased from 1.74% in 2013 to 1.41% in 2014 (Figure 2). The SSI incidence has remained unchanged for the first 6 months of 2015 at 1.2%.
Figure 2: Incidence of SSI following caesarean section procedures in Scotland (inpatient and PDS to day 10), 2010 to 2014.
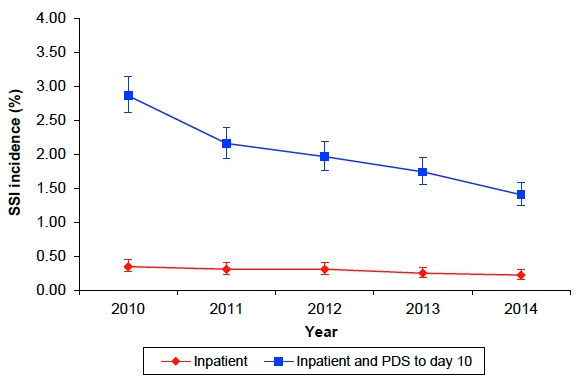
The SSI incidence for hip arthroplasty, for both inpatient and readmission to day 30 remained stable.
Figure 3: Incidence of SSI following hip arthroplasty procedures in Scotland (inpatient and readmission to day 30), 2010 to 2014.
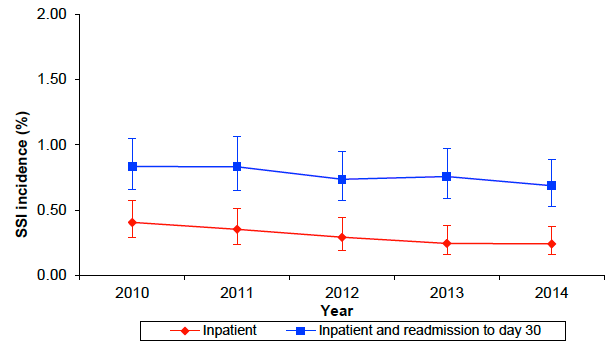
Intensive care unit HAI surveillance
During 2014, 2.5% of patients staying in an intensive care unit for more than 2 days developed an ICU acquired selected HAI. The incidence of bloodstream infection, central venous catheter related infection and pneumonia remained unchanged from 2013.
Clostridium difficile infection (CDI)
The annual incidence rate for 2014, in patients aged 65 and above, was 34.5 per 100,000 total bed days, which is unchanged compared to 2013. In patients aged 15 to 64 years, the annual incidence rate for 2014 was 33.8 per 100,000 acute bed days compared to 35.0 per 100,000 acute bed days in 2013). In the first 2 quarters of 2015, the burden of CDI
Seasonality has been observed in the pattern of quarterly rates over the past 5 years
Figure 4: Overall quarterly CDI incidence rates for Scotland in patients aged 65 years and above (per 100,000 TOBDs) and 15-64 years (per 100,000 AOBDs) for the period Q3 2010 to Q2 2015.
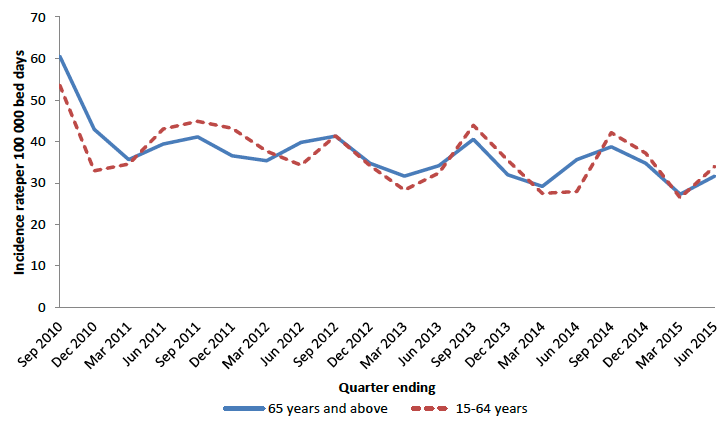
A one-year sentinel study carried out in 2013/14 involving 5 Scottish NHS Boards showed that a substantial proportion of CDI cases (26%) reported in Scotland were community associated (CA-CDI). Historically, CDI has mainly been considered an HAI. Beginning in 2016, HPS will report on the proportion of CA-CDI in national surveillance publications.
To improve understanding of CDI mortality trends in Scotland, CDI case patient data from the national surveillance programme were linked to hospital episode and mortality data between 2009 and 2013. The results showed there was a decrease in 30-day all-cause mortality among patients with CDI from 19.8% to 17.0% between 2009 and 2013, with a year on year decrease of 5.6%. Thirty-day mortality was higher in patients with healthcare-associated CDI.
These results may suggest improvements in the quality of care received by CDI patients in recent years; however, the observed decline may be indirectly linked to overall improvements in mortality among the general population of Scotland, which needs to be assessed.
HAI Outbreaks
From January 2014 to September 2015, a total of 69 health-care associated outbreaks were reported to HPS of which: 17 were of the highest category Hospital Infection Incident Assessment Tool (HIIAT) red, 35 were HIIAT amber and 16 were green. One outbreak was ongoing at the time of this report, thus final HIIAT assessment was not complete.
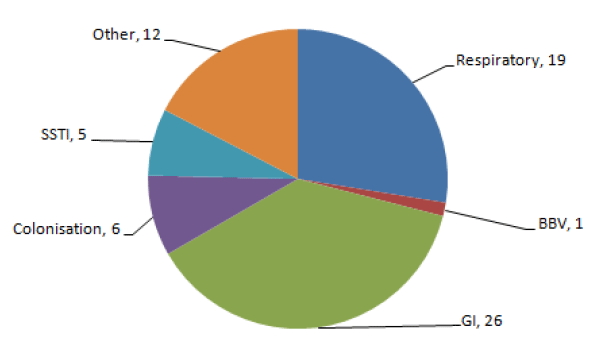
Figure 5 shows the infection types that arose in healthcare related outbreaks reported from January 2014 to September 2015. The most commonly reported outbreaks involved respiratory and gastrointestinal infections similar to findings in 2013. The most common organism causing gastrointestinal outbreaks was Norovirus (n=13) and Clostridium difficile (n=13). The most common organism causing respiratory outbreaks was influenza (n=9).
Figure 5: Types of HAI outbreaks and incidents (n=69) reported to HPS, January 2014 to September 2015.
Norovirus outbreaks continue to be the most common cause of ward closures within NHS boards. Figures are reported from mid-year to mid-year due to the seasonality of norovirus. Reported ward closures for season 2014/2015 were higher (n=222) compared with the previous season 2013/2014 (n=116). This may be due to a decrease in bay closures for season 2014/2015 (n=17) compared with season 2013/2014 (n=117).
Escherichia coli and its antimicrobial susceptibility
In Scotland, Escherichia coli (E. coli) is the most common pathogen implicated in bacteraemia in community and healthcare settings. During 2014, there were 4,539 cases of E. coli bacteraemia in Scotland compared to 4,321 in 2013. The incidence increased from 69.8 per 100,000 bed days in 2010 to 88.2 per 100,000 bed days in 2014. There have been 2,645 cases of E coli bacteraemia between January and June of 2015. A national E. coli bacteraemia programme is being established to monitor the burden of E.coli bacteraemia and to inform interventions/changes in practices.
Antimicrobial susceptibility among E. coli bacteraemias has remained stable since 2011. Non-susceptibility to co-amoxiclav in continues to occur at a very high frequency, (32.6%), and potentially could compromise infection management. Prescribing policies leading to the restriction of broad-spectrum agents in general (in particular carbapenems), IVOST (IV switch to oral therapy) and de-escalation initiatives may have driven the increased use of co-amoxiclav. The proportion of extended-spectrum beta-lactamase (ESBL) producers among E. coli bacteraemias has remained stable since 2011.
Carbapenemase Producing Organisms
Multidrug resistance among Gram-negative organisms continues to be a major threat to public health and patient safety. In particular, the emergence of carbapenemase producing bacteria is concerning as this leaves few options to treat severe infections. In 2014, a total of 43 carbapenemase-producing organisms (CPO's) were reported to HPS from the Antimicrobial Resistance and Healthcare Associated Infection (AMRHAI) Reference Laboratory at Public Health England (PHE). This was an increase compared to 2013 (n=22), however this increase could reflect ascertainment bias due to better awareness and implementation of screening in high risk populations rather than a genuine increasing incidence. For the first 6 months of 2015, there have been a total of 25 CPO's reported.
Controlling Antimicrobial Resistance in Scotland (CARS)
Established in 2015, the Control of Antimicrobial Resistance in Scotland (CARS) team in HPS is leading Scotland's strategic response to control of antimicrobial resistance (AMR) in line with the UK five- year antimicrobial resistance strategy 2013-2018.
Building on the successful antimicrobial prescribing work led by the Scottish Antimicrobial prescribing Group (SAPG) in Scotland under the existing AMR strategy (SCOTMARAP 2); a number of work streams have been developed with a focus on:
- Surveillance - CARS is working with Scottish Microbiology and Virology Network (SMVN) and other partners to further standardise and improve AMR data systems to improve AMR monitoring and provide an early warning of new types of resistance threats.
- Animal health - Working with partners, the CARS team is ensuring that measures to prevent animal infection and to optimise animal prescribing are in place across all animal health sectors, particularly those which are important in relation to the development of AMR.
- Research- working with partners to develop a strategic approach to AMR research including scoping out research priorities, approaches, collaborations and funding opportunities.
- Education and engagement- working with NES and other partners to ensure that AMR is a component of the education of all relevant professional groups including those working in animal health.
Summary
Health Protection Scotland continues to coordinate the national leadership in tackling HAI and AMR and whilst some improvements have been seen in selected SSI there remains a burden of HAI requiring further reduction. Key initiatives introduced in the last year include: evidence reviews to inform infection prevention and control guidance, decontamination monitoring, guidance for endoscopes and equipment used at the patient bedside, establishing the CARS programme and campaigning to prevent the risk of norovirus. In addition HPS has provided expertise to support outbreak preparedness within NHS boards and utilised the national reference laboratory intelligence to inform our work. Newly established enhanced surveillance and research studies will add to this intelligence to inform future strategies for prevention of HAI.
Blood Borne Viruses and Sexually Transmissible Infections
A new Sexual Health and Blood-Borne Virus (SHBBV) Framework (2015-2020) was published by the Scottish Government in September 2015. The framework is a natural progression, rather than a reworking, of the previous SHBBV Framework 2011-2015. It combines areas of work surrounding Sexual Health, HIV, hepatitis C and hepatitis B and is a multi-agency, cross agenda approach based on 5 high level outcomes.
Hepatitis C Virus Infection
New national guidance on the treatment of Hepatitis C virus (HCV) was released in Scotland in August 2015 following a review of clinical evidence by expert stakeholders. The new guidance advises Sofosbuvir-based regimens as the first-line prescribing choice for treating the majority of patients with genotypes 1, 2 and 3.
In the first quarter of 2015/16, over 400 individuals commenced treatment for chronic HCV infection, almost three-quarters of whom were being treated with a sofosbuvir-containing regimen. Challenges relating to the identification of HCV infected individuals, particularly those with advancing disease, and the accessing of funds to pay for the therapies, remain.
Complementary guidance on treatment prioritisations, in terms of timing only, was published in the SHBBV Framework as above; targets of at least 1,500 people being treated annually from 2015, and a 75% reduction in end stage liver disease by 2020, were set.
In recognition of Scotland's pioneering work in the field, the inaugural World Hepatitis Summit was held in Glasgow in September 2015. The summit, co-sponsored by WHO and the World Hepatitis Alliance, was hosted by the Scottish Government in association with HPS and Glasgow Caledonian University. The aim was to help countries enhance action to prevent viral hepatitis infection and ensure that people who are infected are diagnosed and offered treatment. Policymakers, patient groups and other key stakeholders attending the summit issued The Glasgow Declaration on Hepatitis promoting the elimination of viral hepatitis as a public health concern and urging governments to work with WHO to define and agree on global targets for prevention, diagnosis and treatment.
HIV
At the end June 2015, over 5,000 people are estimated to be diagnosed and living with HIV in Scotland. An estimated further 1,600, however, remain undiagnosed and novel methods are required to promote HIV testing in a variety of settings. Following a change in the law in April 2014, the first licensed HIV self testing kits, based on a finger prick blood sample, went on sale at the end of April 2015. This approach, where the individual can read their own test result within 15 minutes, increases the options for HIV testing as part of the prevention toolkit. These kits are available online and it is expected that these will also be available to purchase over the counter in due course. Furthermore, developments in laboratory testing now mean that all new HIV diagnoses are subjected to a supplementary new test, the avidity antibody test, developed by the BBV specialist testing laboratory in Glasgow. The results of this test are used to determine the proportion of those who have recently acquired their HIV infection, that is, within the previous 3 to 4 months. This service was implemented across all NHS board areas during 2014 and the most recent data up to the end September 2015 indicate that over one third of newly diagnosed men who have sex with men (MSM) have recently acquired their HIV infection. This is the highest proportion among all risk groups tested and suggests that the majority of HIV transmission in Scotland is occurring among this group. This test has also been helpful in outbreak situations.
An increase in the number of people who inject drugs (PWID) diagnosed with HIV infection in Glasgow is currently under investigation. Between January and August 2015, 36 HIV infections had been diagnosed, including 10 with evidence of recent infection. Glasgow typically records around 10 new cases of HIV related to injecting drug use each year. Control measures including awareness raising of the risk of HIV among PWID and services in contact with this population, and reminding PWID not to share injecting equipment and to use condoms for sexual intercourse, have been implemented. Foil for smoking heroin is available as an alternative to injecting, and provision of injecting equipment including water is widely available with PWID not limited in the volume they can access. Control measures also include increasing HIV testing by a variety of services in contact with those at risk and measures to engage cases in HIV treatment.
Sexually transmitted infection
Evidence from the monitoring of laboratory positive diagnoses of sexually transmitted infection (STI) indicate that the incidence of STIs among the young heterosexual population and MSM through unprotected sexual intercourse remain a problem in Scotland: challenges for control and prevention continue. Thus, this remains a priority area for the Scottish Government as outlined in the SHBBV Framework 2015-2020. In this respect, chlamydia testing policy has been an area of review and the Scottish Government commissioned a cost effectiveness study. HPS, in conjunction with other clinical and research partners, notably modelling experts at the University of Bristol, published the results of the cost-effectiveness analysis in January 2015. The model was sensitive to several parameters, particularly the health state utility values for pelvic inflammatory disease and tubal factor infertility, however, based on conservative modelling assumptions, current testing activities in Scotland do not appear to be cost-effective. The study highlighted areas where cost effectiveness could be improved and this information will be used to inform the guidance around testing practice.
HIV infected Health Care Workers and Exposure Prone Procedures
In January 2014, the CMO distributed a letter communicating changes to policy in Scotland (and across the UK) in relation to the practice of exposure prone procedures (EPPs) by healthcare workers living with HIV. The letter briefly summarised the conditions for being cleared to perform EPPs based on viral load and treatment regime and also explained the requirement of healthcare workers to be registered on a confidential national register, the UKAP-OHR (UK Advisory Panel for Healthcare Workers Infected with Blood-borne Viruses - Occupational Health Monitoring Register for BBV Infected HCWs). This change reflects accumulated evidence that shows there is an extremely low risk of transmission from an infected HCW to a patient, and has benefitted a number of healthcare workers who are living with HIV in Scotland.
Accompanying this policy change is an updated guidance document from Public Health England describing the management of HIV infected HCWs who wish to perform EPPs https://www.gov.uk/government/publications/hiv-infected-healthcare-workers-and-exposure-prone-procedures.
Gastrointestinal and Zoonoses Infections
Verotoxin-producing E. coli
In 2014, there were 263 faecal culture positive cases of E. coli O157 notified to HPS in 2014. This represented an increase on the 167 cases reported in 2013. The reasons for the increase observed in 2014 compared to 2013 were due in part to the fact that the number of cases reported in 2013 was the lowest annual total for 5 years and substantially below the annual average for that period (221 cases per annum). Nine general outbreaks of verotoxin-producing E. coli (VTEC) were reported to HPS compared to three in 2013. Of these 9, 7 were identified as serogroup O157, one was serogroup O125 and one was both serogroup O157 and O103. Further information on these outbreaks is contained in the HPS Weekly Report on general outbreaks of infectious intestinal disease in 2014. (http://www.hps.scot.nhs.uk/ewr/redirect.aspx?id=64290)
The consistently high rates of VTEC infection reported in Scotland as compared to other UK countries, and indeed the increase in outbreak cases observed in 2014, underlines the need for the continued and comprehensive application of the wide range of existing control measures embedded in food safety and other guidance in Scotland. In addition it highlights the importance of a comprehensive multi-agency approach to tackling VTEC in Scotland as set out in the VTEC Action Plan for Scotland; more information on the VTEC Action Plan can be accessed at: http://www.scotland.gov.uk/Publications/2013/11/8897/0.
The VTEC Action plan was published in November 2013 and contained 86 recommendations designed to tackle VTEC/ E.coli O157 in Scotland. Scottish Government requested that HPS take responsibility for monitoring and coordinating the implementation of the actions plan.
Recommendations were divided into 8 areas of work (animal attractions, clinical, communications, environmental, Food Standards Scotland, private water supplies, public water supplies, research & surveillance). It was recognised that communications will crossover a wide range of work streams. It is anticipated that the working groups will complete their actions by 2017.
Hepatitis E
Over the past few years Hepatitis E has emerged in Scotland and elsewhere in the UK as a pathogen of increasing importance. Until recently Hepatitis E was considered mainly travel-related among those returning from Hepatitis E endemic areas; however, indigenous cases are now recognised as an important component of infection in Scotland. Since 2011, there has been an increase in laboratory reports of Hepatitis E from 13 in 2011, to 78 in 2012, 95 in 2013 and 161 in 2014, more than ten-fold the number four years earlier. In response to this increase HPS has established a Hepatitis sub-group of the SHPN-GIZ group. The Hepatitis E group is a multi-agency group with representatives from Food Standards Scotland, NHS Board Health Protection Teams, virologists, clinicians, veterinary consultant, Public Health England, SNBTS and academia. The group aims to work to achieve a better understanding of the epidemiology of hepatitis E in Scotland to help inform public health action to reduce the incidence of disease.
Imported infection and travel abroad
As part of its remit to protect the health of the Scottish public, Health Protection Scotland (HPS) provides advice and guidance to health professionals and members of the public on:
- risks associated with travelling abroad
- assessment of emerging risks abroad and imported infections
In 2014 to fulfil these responsibilities the Travel & International Health team (TIHT) of HPS continued to carried out surveillance of travel-related infectious disease imported in Scotland, surveillance of outbreaks and incidents abroad, in particular by supporting the risk assessment for the 2014 Commonwealth Games, and also playing a central role the Scottish public health response to the Ebola outbreak in West Africa.
In 2014 [1], there were approximately 3.9 million journeys abroad from Scotland, representing 6% of total journeys from the UK. This was an increase of 9% over the previous year's figure. In 2014 Europe (78%) was the most visited destination followed by North America (8%), Asia (4%), Africa (3%), Central, South America and the Caribbean (2%) and Australia and New Zealand (1%) (Figure 6).
Figure 6. Travellers from Scotland[1]
![Figure 6. Travellers from Scotland[1] Figure 6. Travellers from Scotland[1]](/binaries/content/gallery/publications/report/2016/01/chief-medical-officers-report-part-2-health-nation/00492631.gif)
Forecasts indicate further increases in Global and UK travel abroad, along with the ever present risk of emerging infections of high pathogenicity and/or transmissibility (refs), and incursion of infections into new geographical areas (refs). HPS strives to intelligently translate the various data through risk assessment into tools for planning, management, advice and guidance. Recent work carried out during the Commonwealth Games, has helped build the capacity in HPS to accurately assess the plethora of data available.
TIHT maintain 2 evidence-based, travel health advice websites. TRAVAX (www.travax.nhs.uk) is aimed at health professionals and assists with pre- and post-travel assessment, and fitfortravel (www.fitfortravel.nhs.uk) directly speaks to the travelling public. Both sites highlight developing issues and rely on competent assessment of real-time data on risks abroad, along with clinical and epidemiological evidence, to produce timely and appropriate advice and recommendations for actions.
Surveillance of Imported infection
Surveillance of key imported infections is one indicator HPS uses to assess wider public health risk. Those infections which are reported to HPS as imported are included in the annual totals of travel-related infection authored by TIHT in January each year since 2013. [2]
In 2014, 203 episodes of schistosomiasis were reported, making this the most frequently reported travel-related infection. This disease is transmitted through contact with affected fresh water particularly in sub-saharan Africa. School visits to countries where Schistosoma sp and other pathogens are endemic are now commonplace. In response to this HPS has developed guidance specifically for school groups [3] and continues to advise that travellers who bathe in fresh water in endemic countries are tested for infection on their return home.
In terms of infectious risks to travellers, we know that food and water-borne diseases resulting in travellers' diarrhoea and similar illnesses are amongst the most common affecting travellers. Non-viral gastrointestinal infections were among the most frequently reported by the laboratories to HPS as travel-related during 2014, the most common being Giardia spp (36) followed by Cryptosporidium spp (31) and Shigella spp (22). It is highly likely, however, that the real incidence of these infections is much greater.
Cyclospora cayetanensis is a protozoan parasite that causes diarrhoea, particularly in developing countries. In July 2015, Health Protection Scotland (HPS) identified an unusual increase in Cyclospora infections in travellers to Mexico and informed Public Health England (PHE), who identified additional cases. C. cayetanensis was identified in 21 returned Scottish travellers from the Riviera Maya region of Mexico between 1 June 2015 and 22 September 2015. In total, 176 cases were reported of which 79 cases were reported from the UK and 97 in Canada. An outbreak control team managed the UK investigation. Patients were interviewed about travel history, food consumption, clinical symptom details and demography using a questionnaire.
This increase in cyclosporiasis in the UK and Canada occurred in people returning from 32 hotels on the Riviera Maya coast of Mexico. No formal epidemiologic study was conducted. Drinking water was an unlikely source as several different water networks supply the resorts. Geographic and temporal associations suggest the outbreak was related to a consumed product(s) distributed throughout the region rather than hygiene deficiencies in individual hotels. Close collaboration with the Scottish Parasite Diagnostic and Reference Laboratory were crucial in the early identification of this rare pathogen. This outbreak has now been published in Eurosurveillance: http://www.eurosurveillance.org/ViewArticle.aspx?ArticleId=21284.
Supplementing routine laboratory reports, HPS also receive information from NHS Boards on potential outbreaks of infectious intestinal disease believed to have been acquired abroad[4] In 2014, information was circulated concerning 30 potential outbreaks of infectious intestinal disease in persons returning to Scotland from abroad. Most commonly mentioned countries were Turkey (7 outbreaks), Spain (7 ), Egypt (3) and Tunisia (2) which are all popular tourist destinations.
Vector-borne diseases remain a risk for travellers and HPS provide guidance on prevention, prophylaxis and treatment via TRAVAX and fitfortravel. Malaria was the most commonly reported vector-borne disease in Scotland in 2014 with 76 reports: representing less than 5% of the UK total. [5] Those visiting friends and relatives (VFRs) abroad represented the greatest proportion of cases with 18 reports (28%). Africa contributed 91% of the 75 reports where region of transmission was recorded; West Africa alone contributed 53% (40) of the reports. In line with the region of transmission 83% (63) of the reports were due to infection with Plasmodium falciparum, with P.vivax (9, 12%), P malariae (5, 7%) and P ovale (1, 1%) providing the remainder; 2 were mixed infections. Risks faced by travellers may be linked to travel at short notice with lack of preparation and appropriate advice. In particular VFR travellers may have a belief in innate immunity or the safety of their destination and fail to take adequate precautions. The possibility should always be considered in a febrile individual arriving from a country where malaria is endemic.
Of the other vector-borne infections reported in 2014, dengue virus (28) was most common although 13% lower than in 2013 (31) followed by 6 reports of chikungunya virus, compared to 2 in 2013. In 2014 imported West Nile virus cases were reported in Scotland for the first time with 3 reports. While there is significant public health concern over the establishment of vector-borne diseases in Europe, particularly in Southern Europe, opportunity for the establishment of such infections in Scotland is limited by climate. Nonetheless as the distribution of such vector-borne infections continues to increase, the risk of disease for travellers from Scotland may increase as a result.
Surveillance of outbreaks across the world
As in previous years, during 2014 HPS continued to monitor and assess international occurrence of infectious diseases of global importance such as Middle East Respiratory Syndrome Coronavirus (MERS-CoV), influenza, measles and poliomyelitis.
Two events in 2014 raised the profile of the international nature of disease transmission for Scotland being 1) the Glasgow Commonwealth Games and 2) the Ebola outbreak in West Africa.
Commonwealth Games
In 2014 the 20th Commonwealth Games was held in Glasgow between 23 July 2015 and 3 August 2015. This was the largest sporting event ever to be held in Scotland with 6500 athletes from 70 countries taking part across sites in Glasgow, Edinburgh and Perthshire, with an estimated 600,000 individuals visiting Games-related events.
In preparation HPS reviewed and enhanced its routine surveillance. The international component of this was carried out by TIHT who stepped up routine surveillance activity, and added in daily contact with colleagues from the European Centre for Disease Prevention and Control (ECDC) to ensure completeness in risk identification.
Eighty-eight new incidents were identified through this enhanced surveillance system as having the potential to be imported and transmitted during the Games, mainly measles (14) and cholera (11). Incidents originated in Asia (23), Africa (15), Europe (15) and Oceania (12). Seventy six of these events were identified by HPS with a further 13 arising as a result of ECDC activity. All were categorised as being very low risk to the Games.
While risk assessments carried out were generally straightforward the report of the Ebola outbreak in West Africa required a more thorough assessment based on reviews of pathology, natural history and epidemiology. Even this was assessed as being very low risk to the Games.
In addition to ensuring safety of public health and integrity of the Games, a key objective in carrying out this extended Epidemic Intelligence was to allow application of lessons learned and help develop a legacy for surveillance of emerging infections and other hazards in Scotland. In 2015 HPS has applied these lessons to ensure systematic methods for assessing the risks of emerging diseases and other hazards.
Response to Ebola
In March 2014 the world became aware of a developing outbreak of Ebola Virus Disease (EVD) which occurred for the first time in West Africa; previous outbreaks of EVD, first identified in 1976, had occurred in Central and East Africa usually lasting for weeks to months. It is likely the outbreak was initially caused due to consumption of bush meat but it was sustained due to local burial practices and the rural nature of the cases. A further complication was that the outbreak initially involved 2 countries. Attempts by local health authorities and the WHO failed to contain the outbreak and the infection was soon spread to Sierra Leone.
Soon after the outbreak escalated and on 8 August 2014 WHO declared a Public Health Emergency of International Concern (PHEIC). In response to this declaration the UK and Scottish CMOs issued letters giving guidance to NHS volunteers who wished to support the WHO-led response. Volunteers began to leave in November as part the UK component of the international response. In early 2015 the outbreak began to show initial signs of decreasing incidence and increasing control.
As of 25 October 2015 in Sierra Leone, Guinea and Liberia 28,539 confirmed, probable and suspected cases had been reported and 11,298 deaths. Small numbers of cases were continuing to be identified and WHO has not declared the PHEIC to be over. A total of 21 possible cases and one confirmed case presented in Scotland.
Prior to March 2014 HPS had already been applying lessons learned as the result of 2012 Crimean Congo Haemorrhagic fever case who was cared for in Glasgow before being transferred to the Royal Free High Level Isolation Unit in 2012.
From March during the early stages of the outbreak and prior to the Glasgow Commonwealth Games HPS reviewed the data from the area on a daily basis and kept travellers and health professionals informed via TRAVAX, fitfortravel and HPS websites.
A key early HPS action was the establishment of a multi-disciplinary VHF working group. This group met in order to ensure thorough discussion, planning, preparation and exercising, Scotland could be placed in a confident position to respond to any EVD case in Scotland.
From July during the Commonwealth Games period HPS provided guidance to health professionals, raising awareness, and responding to an increasing number of enquiries seeking advice. In addition HPS engaged well with the media during this high profile period, while maintaining confidentiality of two possible Games presenting in the Commonwealth Games Village.
Staff from Scottish agencies including, NHS, Scottish Government and NGOs, went to Sierra Leone to help control the outbreak there and prevent further international spread. PHE established coordinated means of identifying deployed volunteers to facilitate risk management both in West Africa and on return. A total of 112 returning workers were processed, of whom 36 were military.
A critical element of HPS response was in guidance production. This included guidance on the transfer, diagnosis and management of possible Ebola cases identified in the community and in healthcare facilities and infection control precautions for VHF for hospitals, primary care and, the Scottish Ambulance Service (in collaboration with SAS). Guidance was also produced for non-healthcare settings such as schools and universities, as well as guidance on port health. This guidance was updated in real time to ensure alignment with other public health organisations such as PHE, WHO and CDC. Evidence was also produced on waste management, decontamination and procurement.
HPS published guidance on suitable personal protective equipment (PPE) products and how they should be worn, enabling local ICTs to purchase sufficient PPE for their Board By December every board had at least the minimum number of coveralls required.
HPS collaborated with NES to produce a training video 'Viral Haemorrhagic Fever (VHF) - The correct order for donning and the safe order for removal and disposal of Personal Protection Equipment (PPE)' as well as posters and checklists for donning and doffing PPE.
On 29 December 2014 the first case of Ebola to be diagnosed within the UK was confirmed in Scotland by the Scottish National Viral Haemorrhagic Fever Test Service (SNVTS). The patient was a healthcare worker who had recently returned from Sierra Leone to Glasgow via London Heathrow. While the case was managed clinically by Greater Glasgow and Clyde NHS Board, HPS carried out contract tracing on passengers who had been on the flight she had taken from London, identifying 76 possible contacts. By 31 December 2014 all of these had been contacted, interviewed, given advice and, where appropriate had ongoing monitoring arranged.
Following confirmation of Ebola infection, the case was managed in the Brownlee Centre prior to transfer to the Royal Free HLIU . Appropriate staffing levels, PPE, and isolation facilities were deployed in the Brownlee and there was no onward transmission of Ebola infection. Review of the process involved indicated that they were safe and effective.
Management of possible cases included the presentation, isolation, transfer and testing of a possible case in a remote region of Scotland. The majority of possible cases were returning healthcare or aid workers from West African countries affected by the Ebola outbreak.
Contact
Email: Diane Dempster