Better Heart Disease and Stroke Care Action Plan
Revised strategy for heart disease and stroke in Scotland.
6: IMPROVING THE QUALITY OF CARE AND SUPPORT
Information and Communication
6.1 One of the major concerns from the British Heart Foundation's research project to explore the practical, social and emotional implications of living with CHD was a considerable lack of communication and information-giving on the part of the medical profession, leaving patients feeling disempowered, confused and anxious at a time when they particularly need strength, re-assurance and confidence.
6.2 One of the key messages from a survey carried out by Chest, Heart & Stroke Scotland and NHS Tayside during 2006-07 into the emotional impact of stroke was that stroke has a major emotional impact, with feelings of anxiety, frustration and fear of recurrence being common. If not addressed, these can intensify to clinical depression, with substantial detrimental effects on long term recovery and family relationships. Those who had had a stroke recognised the need to be able to talk to someone. One-to-one support from a knowledgeable health professional appeared to be the most widely acceptable intervention.
6.3 These findings are consistent with those in the generic work on long term conditions being undertaken by the Chief Medical Officer and the Long Term Conditions Alliance Scotland. It is essential that the approaches being developed through the Long Term Conditions Action Plan should be applied to people with heart disease and those who have had a stroke, from the time of their first contact with the NHS onwards. That information should include making sure that people have a clear understanding about what has happened to their heart on a physical level, in order to dispel misconceptions. It is also essential that people should be given a satisfactory explanation of the cause of their illness, to pave the way for discussions about the role of their own lifestyle and the acceptance of a degree of responsibility for their own health. People must be signposted to the information and support available from voluntary sector organisations.
6.4 The British Heart Foundation research project referred to above showed that within the medical profession there were weak links of communication between GPs and hospital consultants. This resulted not only in a lack of continuity of care, but also in patients feeling a sense of having been abandoned after discharge from hospital. People were, for example, often surprised at the apparent lack of interest shown by their GP in relation to their hospital treatment. Participants also commented on the compartmentalised nature of the medical system and the lack of the continuity of care necessary for a more patient-centred approach. The same issues have been raised by patients with stroke, and their carers.
6.5 The National Advisory Committee for CHD has supported the development of 'Heart Scotland' a website that contains a patient portal. When completed, it will direct patients and carers to nationally applicable, quality-assured information about all forms of heart disease, their causes, diagnosis, treatment, rehabilitation, and on living with specific manifestations. In addition, 'Heart Scotland' has created a series of 'virtual visits'. These illustrate what to expect in general terms when going for a consultation, test or treatment in a range of care settings, and at the same time highlight the growing role that community care settings such as the GP surgery and community pharmacy are playing in tackling heart disease.
Action:
NHS Boards, through their cardiac and stroke MCNs, need to make concerns about communication issues for heart disease and stroke patients one of their priorities, and develop plans to tackle these concerns locally.
6.6NHS Education for Scotland has a patient elibrary for stroke. NHS 24's website includes information on both heart disease and stroke. Chest, Heart & Stroke Scotland, the British Heart Foundation and the Stroke Association provide public information on their websites also.
6.7 In line with the Scottish Government approach to working in partnership with the voluntary sector, as set out in Better Health, Better Care, the key voluntary organisations - the British Heart Foundation in Scotland, Chest, Heart & Stroke Scotland and the Stroke Association in Scotland - will be fully involved in taking forward the actions in the revised strategy through their representation on the relevant National Advisory Committees. The Scottish Government Health Directorates ( SGHD) will also continue to work with other organisations active in relation to CVD, such as HEARTUK, Diabetes UK Scotland, Scottish HART, the Cardiomyopathy Association and the Arrythmia Alliance. In addition, SGHD will also maintain close links with the recently-formed Parliamentary Cross Party Group on Heart Disease and Stroke.
Self Management
6.8 As with any other long term condition, self management has an extremely important part to play in relation to heart disease and stroke. The principles of self management as set out in the national strategy, Gaun Yersel!, developed by the Long Term Conditions Alliance Scotland ( LTCAS) therefore apply here. They are:
- I am the leading partner in management of my health (I am involved in my own care. I, those who care for me and organisations that represent me, shape new approaches to my care);
- Be accountable to me and value my experience (Evaluation systems should be ongoing and shaped by my experience. They should be non judgemental and focus on more than medical or financial outcomes);
- I am a whole person and this is for my whole life (My needs are met along my life journey with support aimed at improving my physical, emotional, social and spiritual wellbeing);
- Self management is not a replacement for services. Gaun yersel' doesn't mean going it alone (self management does not mean managing my long term condition alone. It's about self determination in partnership with supporters);
- Clear information helps me make decisions that are right for me (Professionals communicate with me effectively. They help ensure I have high quality, accessible information. They also support my right to make decisions).
6.9 It is essential that people with a heart condition or who have had a stroke are made aware of all the relevant sources of information and support that could be made available to them, whether provided by the NHS, local authorities or the voluntary sector. Much of this work will be achieved through the NHS Health Information Service being launched formally in autumn 2009.
6.10 Voluntary organisations active in the area of CVD will be able to apply for grants from the Self Management Fund administered by LTCAS in order to promote the development of self management amongst those with a cardiac condition or who are recovering from a stroke. The Fund is being supported through £2m funding from the Scottish Government in each of 2009-10 and 2010-11. Details are available from the LTCAS website ( www.ltcas.org.uk).
Managed Clinical Networks
6.11 The 'Voices Scotland' project supports the Scottish Government's vision of a mutual NHS by ensuring that chest, heart and stroke patients' and carers' views are represented, and their voices heard, and that they have the opportunity to be involved in a meaningful way in the work of NHSScotland. 'Voices Scotland' aims:
- to provide people affected with chest, heart or stroke conditions, and their carers, with the skills and confidence to work alongside the NHS;
- to empower patients and carers through access to information, training and support;
- to develop a supportive network of chest, heart and stroke patients and carers; and
- to encourage partnership working between the NHS and the voluntary sector.
6.12 The project, which is run by Chest, Heart & Stroke Scotland and the British Heart Foundation, has trained more than 250 people so far, across all but one NHS Board. Those who have been through the training have been able to take part in relevant work by SIGN, NHS Quality Improvement Scotland, NHS Education for Scotland and the 'Living Better' project, as well as taking part in the consultations on the revision of the CHD and Stroke Strategy and the Patients' Rights Bill.
6.13 One of the core principles of all MCN developments is that they should include strong patient and voluntary sector participation. 'Voices Scotland' helps to strengthen the patient and carer voice in the work of the cardiac and stroke MCNs. Given the central role intended for these Networks in taking forward this Action Plan, it is essential that the 'Voices Scotland' project should continue to provide the training needed. It is particularly important that those with communication difficulties following a stroke should be able to make their voices heard, and the development of training suited to their specific needs should form part of the next phase of the project. 'Voices Scotland' will also help to provide representation on the National Advisory Committees from those with a heart condition or who have had a stroke.
Quality and safety of care
6.14 The NHS Quality Improvement Scotland CHD Improvement Management Programme, issued in June 2009, represents the first nationally co-ordinated quality improvement programme for heart disease in Scotland. It complements and builds on existing work of the cardiac MCNs. The programme provides linkage between evidence-based practice, patient safety and patient-centred care. It is based on genuine partnership with health professionals and voluntary organisations involved in heart disease.
6.15NHSQIS will work with the NHS, principally the cardiac MCNs and patient representative groups, to:
- harness the individual discrete functions of NHSQIS to deliver a proactive, integrated and supportive approach;
- ensure alignment and integration of work with the Scottish Patient Safety Programme ( SPSP);
- work with other agencies as required;
- provide the appropriate resources, tools and mechanisms that will support the service in ongoing improvement;
- build capacity and capability to support service improvement;
- provide a structured approach and support for a sustained programme of implementation; and
- demonstrate the quality of care throughout NHSScotland.
Measurement for Improvement
6.16 A national audit programme is under way which is directly linked to the NHSQIS standards. The work is overseen by a Clinical Audit and Indicators Steering Group and supported by sub-groups covering heart failure, acute coronary syndromes, atrial fibrillation and cardiac rehabilitation. Audits will begin in 2009. Formal reporting mechanisms are also being put in place to ensure that local and national results are communicated widely, to drive improvement.
6.17 Clinical indicators will be developed, within the programme for CHD, informed by the results of audit activity. Work on developing measures of quality and safety in primary care will also be included within this work stream. It is envisaged that a small, focussed suite of indicators will provide the ongoing mechanism by which NHS Boards can monitor local activity and highlight where improvement may be required. Responsibility for this element of the CHD work programme falls within the remit of the Clinical Audit and Indicators Steering Group.
6.18NHSQIS will ensure that emerging results and issues associated with this programme of work are shared between parallel work programmes, e.g. long term conditions and primary care to capitalise on the 'knowledge brokering role' and to ensure that the maximum benefits for people with or at risk of heart disease are realised.
6.19NHSQIS will be developing and piloting Patient Reported Outcome Measures as part of the programme. This work will commence in late summer of 2009.
6.20 The Managed Clinical Networks ( MCNs) are pivotal in taking the CHD Improvement Management Programme forward. NHSQIS will work closely with a range of key stakeholders but particularly the MCNs to ensure the success of the Programme. Accreditation of local cardiac MCNs will form part of this work, and the Programme will support MCNs to achieve accreditation.
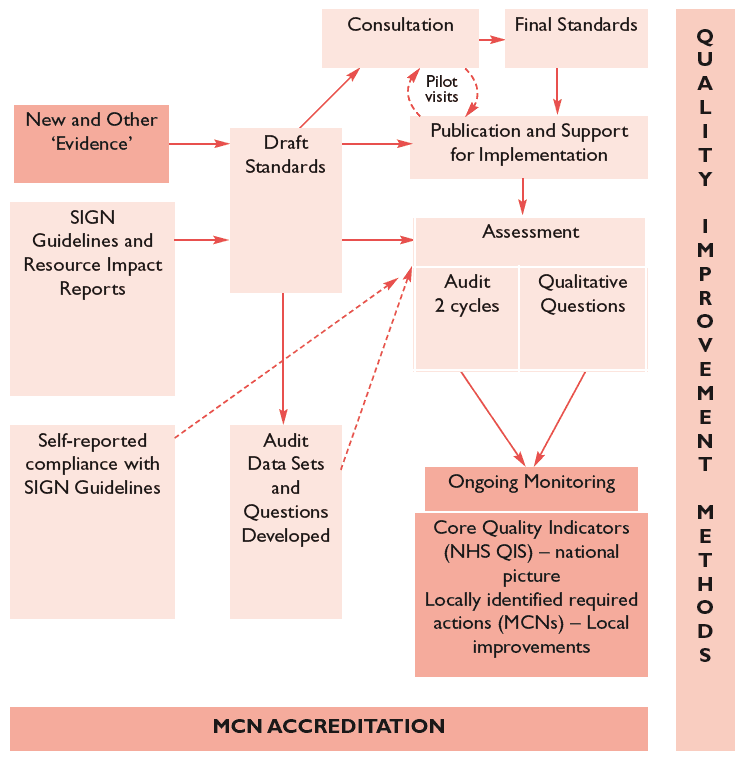
NHS Quality Improvement Scotland CHD Improvement Programme 2007-2010
Stroke
Clinical Guidelines
6.21SIGN 13, 'Management of patients with Stroke I: Assessment, investigation, immediate management and secondary prevention', and SIGN 14, 'Management of patients with Stroke II: Management of carotid stenosis and carotid endarterectomy', have been updated and amalgamated into a single guideline entitled: 'Management of patients with Stroke or TIA: assessment, investigation, immediate management and secondary prevention'. This was published in December 2008 as Guideline 108 on the Management of patients with stroke or TIA: assessment, investigation, immediate management and secondary prevention. A patient version of the Guideline has been developed in collaboration with Chest, Heart & Stroke Scotland.
6.22SIGN is currently working on a selective update of SIGN 64, 'Management of patients with Stroke: rehabilitation, prevention and management of complications, and discharge planning'. This will cover the issues involved in longer term support in the community following discharge from hospital dealt with in Chapter 5.
Clinical Standards
6.23NHSQIS first developed stroke standards in 2004, covering the care of the patient in the acute setting. As a result of the publication of SIGN Guideline 108, NHSQIS has revisited and updated the 2004 standards on a selective basis. The revised standards were published in draft form in December 2008 and will be finalised, following consultation, later in 2009.
Practice Development
6.24 The NHSQIS Practice Development Unit ( PDU), which forms part of the new Implementation and Improvement Support Directorate, conducted a scoping exercise in 2007 with allied health professions ( AHPs) to identify potential contributions to improving practice to patients with a stroke. Following this scoping, different programmes of work have been completed, including programmes of improvement support and NHSQIS reports, as follows:
- a 'Stroke' Master Class for AHPs in 2007 to share best practice and update knowledge;
- the NHSQIS response to the Aphasia in Scotland report including a self-assessment tool to facilitate local evaluation of aphasia services (published 2008);
- an Easy Access Version of the NHSQIS Response to Aphasia in Scotland (published in February 2009) and specifically developed for people with aphasia;
- a programme of implementation and improvement support provided by the NHSQIS Practice Development Unit at six demonstration sites, The report Road to Recovery - Easier to Swallow (published April 2009) describes the programme which was given to nurses and AHPs in the management of the patient with dysphagia; and
- The Road to Recovery - One Step at a Time report (2007) outlines a review of issues relevant to AHPs and nurses in the management of ankle-foot orthoses following acute stroke. As a result of this work a Best Practice Statement on Ankle-Foot Orthoses Following Acute Stroke has begun, and will be completed in July 2009.