Better Heart Disease and Stroke Care Action Plan
Revised strategy for heart disease and stroke in Scotland.
3: PREVENTION - HEALTHY LIFESTYLES AND HEALTH INEQUALITIES
3.1 Scotland's health is improving rapidly but it is not improving fast enough for the poorest sections of our society. Health inequalities remain our major challenge.
3.2 Healthcare in Scotland is shifting from a reactive system of healthcare to one which seeks to anticipate and prevent health problems before they develop. Public health measures relating to tobacco, alcohol and food have a central role in this work.
3.3 A useful survey of the international evidence for the prevention of cardiovascular disease is contained in Healthcare Models for the Prevention of Cardiovascular Disease published by the Health Foundation in April 2009.
Healthy Lifestyles
3.4 Cardiovascular disease ( CVD) covers a spectrum of disorders which includes CHD, cerebrovascular disease, diabetes and peripheral vascular disease. All CVD is associated with a number of potentially modifiable risk factors which can be measured to estimate overall risk. SIGN Guideline 97 on risk estimation and the prevention of CVD therefore covers the prevention of other forms of CVD, not just CHD.
Smoking
3.5 The association between smoking and increased rates of CVD is well understood. Smokers are twice as likely to suffer a heart attack than non-smokers, and smoking is also linked to increased risk of stroke. The Scottish Government's historic ban on smoking in public places in March 2006 led to a reported reduction of 17% in hospital admissions for heart attack when comparing numbers observed 10 months before and after the ban, based on a sample of nine hospitals in Scotland. It is not clear whether there is similar research in relation to strokes. Adult smoking rates increase with increasing deprivation. In 2005-06, smoking rates in Scotland ranged from 11% in the least deprived 10% of areas to 44% in the most deprived 10% of areas. Recent research has also demonstrated that smoking is responsible for a significant reduction in survival after cardiac surgery ( British Medical Journal, 2 April 2009 338; 902 et seq.).
3.6 A survey of Scottish GPs carried out in the autumn of 2008 by the charity HEARTUK found that 24% of those who responded did not refer their patients routinely for lifestyle modification advice and therapy. That finding is confirmed by the EUROASPIRE Study, reported in The Lancet for 14 March 2009 (Vol 373) which suggests that more effective management of lifestyle risk factors is 'desperately needed' in patients with CHD. The study found that adverse lifestyle effects persisted in patients one year after a cardiac event. These trends included smoking. About one-fifth of patients continued to smoke and the proportion of young women smoking actually increased. The Lancet editorial made the point that cardiologists often overlook smoking as a risk factor for CVD when compared to hypertension and hyperlipidaemia, despite the fact that tobacco smoking increases the risk of acute myocardial infarction, sudden cardiac death, aortic aneurysms and peripheral vascular disease. It is likely that these findings would also apply to people who have had a stroke.
3.7 The lack of attention that smoking cessation receives in some primary care and specialist settings is clearly an issue that needs to be addressed, especially as US data suggest that smoking cessation is more cost effective than other preventive cardiology measures. Heart disease and stroke patients should be referred to and have access to community-based smoking cessation services following discharge from hospital.
Action:
All GPs and practice nurses should undertake training in brief intervention/health behaviours and inequalities change, to help them support their patients to make positive lifestyle changes. Greater use could be made of community pharmacists, who should also be included in brief intervention training programmes and trained in the use of CVD risk assessment tools. There is also a role for health coaches, as the Stroke Association work in England indicates.
3.8 In May 2008 the Scottish Government launched Scotland's future is smoke-free, a Smoking Prevention Action Plan with £42m being made available over the next three years (2008-09 to 2010-11) to support a wide-ranging tobacco control programme, including £33m for a range of smoking cessation services. The Action Plan signalled the Government's intention to bring forward new legislation to control the availability and promotion of tobacco by introducing a registration scheme for tobacco retailers and restricting the display of tobacco products in shops. These measures will be taken forward in the Tobacco and Primary Medical Services (Scotland) Bill (published on 26 February 2009) with the main aim of reducing smoking rates by stopping young people starting to smoke.
Alcohol
3.9 Excess alcohol consumption is related to a wide range of health harms. For those over the age of 40 drinking a small amount of alcohol may have a protective effect against heart disease and stroke. However, for those who drink beyond this low level, and for those under 40 years old who drink any amount, alcohol increases the risk of heart disease and stroke by increasing blood pressure, weight and levels of triglycerides in the blood. In March 2009 the Scottish Government published a discussion document Changing Scotland's Relationship with Alcohol: A Framework for Action, which outlines a range of measures to tackle alcohol misuse, including introducing a minimum price per unit of alcohol, tackling irresponsible promotions, limiting the use of marketing material, placing a duty on licensing boards to consider raising the age of off-sales purchases to 21, and introducing a social responsibility levy. This is backed up by a record investment of over £120m from 2008-09 to 2010-11, to reduce alcohol-related harm.
Action:
NHS Boards, through their cardiac and stroke MCNs, should ensure appropriate referral to community advice and support on alcohol use.
Hypertension
3.10 The Quality and Outcomes Framework of the GMS contract from April 2009 includes two new indicators for primary prevention of CVD in patients with hypertension without confirmed CVD. These require practices to complete a CVD risk assessment on newly diagnosed patients in this category and to give lifestyle advice on an annual basis to all patients diagnosed with hypertension from 1 April 2009. The importance of this issue is underlined by the recent meta-analysis of 150 clinical trials involving blood pressure medication, published in the BMJ (23 May 2009, vol. 338 p1245 et seq.). The results indicate the importance of lowering blood pressure in everyone over a certain age.
Cholesterol
3.11 The report Cholesterol and the ageing population, published in 2008 by HEARTUK claims that cholesterol is the single greatest risk factor for CHD, contributing to almost half the CHD-related deaths in the UK. Cholesterol is also a major risk factor in stroke, and it contributes to the increased risk of CVD associated with diabetes and obesity. The draft NHSQIS clinical standards for prevention and treatment of CHD, currently out for consultation, propose the following priority groups for prevention of CVD:
- Patients with:
- Hypertension without confirmed CVD;
- A first degree relative with premature CVD; and
- A first degree relative with Familial Hypercholesterolaemia ( FH);
- Patients with a personal history of:
- Diabetes (Types 1 and 2) aged 40 and over; and
- Familial Hypercholesterolaemia at any age.
3.12 Population-wide action on cholesterol seems to offer the biggest opportunity for health gains relative to the small scale of effort involved. Whole population approaches should therefore be borne in mind, as indicated in the CVD Guide to Primary Prevention, published in 2005 by Heart Health National Learning Network.
3.13 The specific issues around testing for Familial Hypercholesterolaemia are covered in paragraphs 4.95 to 4.97.
Obesity and Cardiovascular Risk
3.14 Individuals with a BMI >30kg/m 2 have a two- to threefold increased risk of CHD and stroke compared to individuals with a normal BMI. They also have a very dramatic (fortyfold) increased risk of developing diabetes. Central obesity, as measured by waist circumference, is a better predictor of cardiovascular risk than BMI (defined as waist circumference = 102cms in men and = 88cms in women). Scottish Asians are at greater risk of CHD and stroke at lower BMI and waist circumference than non-Asians (= 90cms in Asian men and = 80cms in Asian women).
3.15Healthy Eating, Active Living: An action plan to improve diet, increase physical activity and tackle obesity (2008-2011) was published in June 2008. This document outlines commitments to invest £56m in initiatives aimed at supporting people to make healthier choices in what they eat, to build more physical activity into their everyday lives and to maintain or achieve a healthy weight. This action plan will build on, not replace, the continued delivery of the Diet Action Plan and Physical Activity Strategy.
3.16 The action plan also set out the Scottish Government's intention to develop a long term strategic approach to addressing the current obesity epidemic. This will require cross-departmental and cross-sector collaboration to make deep, sustainable changes to our living environment, from one that promotes weight gain, to one that supports healthy choices by all.
Diet
3.17 Currently, a wide range of actions is under way in relation to the provision of a healthier diet for the general population, all of which have the potential to make a positive long term and sustained impact on the incidence of CVD. Reductions in levels of salt, fat and sugar in food are particularly relevant to tackling CVD. Measures targeted at early years, such as a £19m investment over three years to improve the nutrition of women of childbearing age, pregnant women and children under 5 in disadvantaged areas, and measures to increase the proportion of babies who are exclusively breast fed at 6-8 weeks, are key to success in this area. The Schools (Health Promotion and Nutrition) Scotland Act 2007 will also ensure better access to nutritionally healthier foods in schools.
3.18 The National Food and Drink Policy for Scotland aims to create a healthier Scotland by changing individual behaviour and attitudes about diet and food choices by:
- improving the nutritional quality, safety and freshness of food on offer in institutions and the catering sector; and
- supporting Scottish food manufacturers and retailers to take the initiative in driving forward consumer demand for more affordable, healthier food options.
Physical Activity
3.19 The link between physical activity and health is now firmly established, with clear evidence showing that regular activity has both preventive and therapeutic effects on many chronic conditions, including CHD and stroke.
3.20 Scotland's physical activity Strategy Let's make Scotland more Active, published in 2003, remains the key Scottish Government policy document in this area. The Strategy sets a target for 50% of adults and 80% of children to meet recommended levels of physical activity by 2022. In recognition of the fact that these are challenging targets, over the three years (2008-11) the physical activity budget will double from £2m to £4m a year. This is over and above spending in other Government areas which impact directly on physical activity, for example sustainable transport, the active schools programme, etc. The key implementation settings for the next three years will be schools, workplaces, communities and homes.
Equally Well
3.21Better Health, Better Care emphasised the importance of identifying and prioritising practical actions to reduce 'the most significant and widening health inequalities in Scotland'. Equally Well, the report of the Ministerial Task Force on Health Inequalities, sets out the joint Government and local authority plan to tackle Scotland's health inequalities. Evidence shows that those individuals and families from our most deprived communities are most likely to have risk factors associated with poor health outcomes, including CVD. By offering tailored services, focussed on preventative action, which meet the specific and differing needs of our most deprived individuals, Equally Well aims to reduce the gap in health outcomes between most and least deprived.
3.22 Research suggests that CHD, hypertension and diabetes originate early in life during fœtal development. If intrauterine growth is restricted, for example due to inadequate maternal energy intake, there is an increased risk of low birthweight which can have a permanent effect on long term health. Studies suggest that low birthweight babies are more likely to suffer from cardiovascular disease later in life.
Anticipatory Care: targeted high risk primary prevention
3.23 Improving rates of premature mortality from CHD in our most deprived areas is therefore a key objective for Government. This is reflected in the National Performance Framework indicator 'to reduce mortality from CHD among under 75s in deprived areas' and in the 'Keep Well' HEAT target, 'to deliver an agreed number of inequalities-targeted health checks with a focus on CHD'.
3.24 The 'Keep Well' and 'Well North' Programmes provide anticipatory care for those at higher risk of CHD, stroke and diabetes. They invite 45-64 year olds, initially within deprived communities, to attend a health check and offer those found to be at higher risk medical treatment and support to tackle smoking, poor physical activity and other health-related behaviour.
3.25 As the mechanisms for targeting and engaging with 'at risk' populations become more refined, Boards are expected to broaden out their focus to include other key groups that are vulnerable to premature mortality from CVD, such as the South Asian community, offenders, and deprived people living in remote and rural areas.
3.26 The delivery of this service has significant implications for the NHS, local authority services and the third sector, and 'Keep Well' will be fully evaluated with lessons/best practice learned used to influence the future shape of healthcare services.
'Life Begins' Checks
3.27Better Health, Better Care committed the Scottish Government to developing a programme of 'Life Begins' checks. NHS 24 is therefore currently developing a robust online self assessment programme, complemented by telephone-based assistance. This programme will invite people reaching the age of 40 to conduct a web-based self assessment through which they can identify which, if any, personal, family and lifestyle issues could pose a risk for their future health and wellbeing. Where needed, people will be signposted to sources of help and given the option of a telephone consultation with a health adviser. There will be a facility to inform practices of the outcome of the self assessment, if the person agrees. The programme should be 'equalities checked' and it will be important to ensure that those who do not respond are followed up.
ASSIGN Risk Calculator
3.28ASSIGN was developed as part of SIGN Guideline 97 on Risk estimation and prevention of cardiovascular disease. It is being implemented and assessed initially through GP practices involved in the Keep Well programme. While based on the Framingham risk score, it includes a measure of social deprivation - the Scottish Index of Multiple Deprivation - as well as family history. This means that for the first time Scottish people at risk of CVD can have a full assessment of that risk, taking account of the influence of both deprivation and family history (as a proxy for ethnic background). This is particularly important in terms of the Scottish South Asian population, who are at greater risk of CHD at lower BMI and younger age than the rest of the population.
3.29ASSIGN is the preferred CVD risk calculator in use across Scotland. It is available throughout primary care as a web-based tool, and will be due course be integrated into primary care IT systems. In this context, it is helpful that in the new QOF indicators for primary prevention ASSIGN is one of the acceptable risk assessment scores for the achievement of the indicator.
Action:
ASSIGN should be promoted more actively within primary care by NHS Boards and their cardiac MCNs, and integrated with current GP systems (see paragraph 7.17). ASSIGN must be available easily, in a variety of formats, to all clinicians dealing with CVD.
3.30 The 'polypill', a tablet combining the different drugs available to treat many of the cardiac risk factors, is thought to be capable of reducing heart disease by 80% ('Can the polypill save the world from heart disease?', The Lancet, Vol 373 18 April 2009, pp 1313-14). The results of the Indian Polycap Study ( TIPS) showed that each of the components of the polypill did what was intended: the statin reduced cholesterol, the three antihypertensives reduced blood pressure and aspirin reduced the clotting ability of blood. Tolerability for the polypill was good. The paper concluded, however, that a large trial with longer follow-up is however needed to assess the true feasibility of this strategy.
Health Promoting Health Service
3.31NHS Boards are making good progress with implementing the seven actions outlined in CEL(2008)14 on the Health Promoting Health Service ('Every healthcare contact is a health improvement opportunity'). All of the actions, which are focussed on the acute sector, will make a contribution to further reducing rates of CHD and stroke in Scotland.
3.32 Given the proportionately greater use of acute services by patients from deprived communities, this initiative offers a major opportunity to improve health and reduce health inequalities across a whole range of disease areas, not just CHD and stroke. The Scottish Government, in conjunction with NHS Health Scotland, is planning a national conference in autumn 2009 to demonstrate and build on progress to date with the CEL actions.
Action:
The Scottish Government Health Directorates should use the outputs from the 2009 national conference to further develop the Health Promoting Health Service concept, and issue a follow-up CEL by spring 2010.
3.33A Force for Improvement: The Workforce Response to 'Better Health, Better Care' further develops the role of NHS staff as ambassadors for improving health and promoting the benefits of preventative action and measures of self care for patients and the public across a range of health issues.
Mental Health
3.34 People with serious mental health problems are more likely to suffer from CVD before the age of 55, and once diagnosed have poorer survival rates. Those affected by anxiety and depression are less likely to engage in lifestyle change. Interventions to change behaviour will therefore have to address psychological issues. Further actions should include: better screening for depression; improved access to psychological therapies in acute settings and cognitive behavioural therapy; and motivational interviewing, all of which can help improve physical function, mood and treatment compliance. The QOF already incentivises annual screening for depression for those patients with diagnosed CHD and/or diabetes. Addressing anxiety and depression within 'Keep Well', through access to mental wellbeing supports for stress, and the Living Better programme (see box over) will have a positive impact on those with poor mental health.
'Living Better'
'Living Better' aims to improve the mental health and wellbeing of people with diabetes and Coronary Heart Disease. It is funded by the Scottish Government and runs from January 2008 to November 2010. Research indicates that approximately one in three people with diabetes and one in 5 with CHD experience depression. There is evidence that providing treatment and support for depression and other mental health problems can bring a range of physical and psychological benefits. It is estimated, however, that 50% of people with mental health problems go undiagnosed in primary care.
'Living Better' is being piloted on six sites, and starts from the position that people with diabetes or CHD deserve a holistic assessment of their needs, both physical and mental, matched by appropriate services. In order to achieve this, the project team is working with GPs, Community Health Partnerships, people with CHD and diabetes and their carers, to improve the detection of mental health problems and improve the support people receive.
3.35 If people are worried about their life circumstances, they will be less ready to change their behaviours. This is particularly relevant given the current recession, and could be tackled through initiatives such as direct NHS referral to welfare rights services, ideally in healthcare settings, assisting people with managing debt, improving their housing situation and reducing fuel poverty.
Action:
Once evaluated, the lessons from 'Living Better' pilots should be rolled out by NHS Boards and their cardiac and stroke MCNs.
3.36 A paper in The Lancet for 3 January 2009 (Vol 373, 82-93) reported that current data suggest that obstructive sleep apnoea ( OSA) increases the risk of developing CVD and that its treatment has the potential to diminish such risk. Large-scale randomised trials are however needed to determine, definitively, whether treating OSA improves cardiovascular outcomes.
Inequalities in CVD Prevalence
3.37 As noted at paragraph 2.1, over the past 10 years Scotland has seen a steady fall in the mortality rates of the cardiovascular diseases ( CVD) of Coronary Heart Disease ( CHD) and stroke. Behind these population trends, however, there remains a worrying gap in cardiovascular health between the more affluent and the more deprived people of Scotland. This is clearly illustrated by Figures 3 and 4, taken from the Chief Medical Officer's annual report for 2007.
Figure 3: Coronary Heart Disease standardised mortality ratios by SIMD deprivation decile,
2002-06
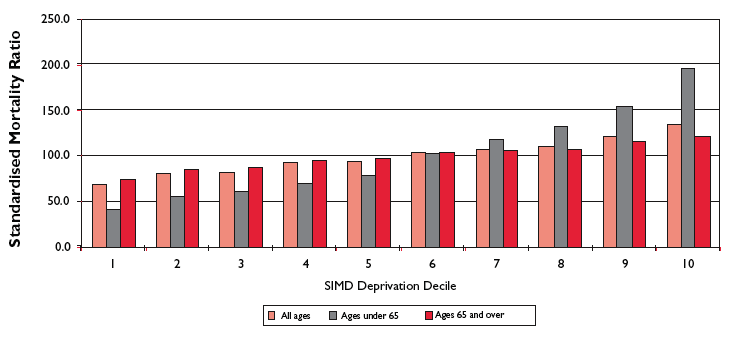
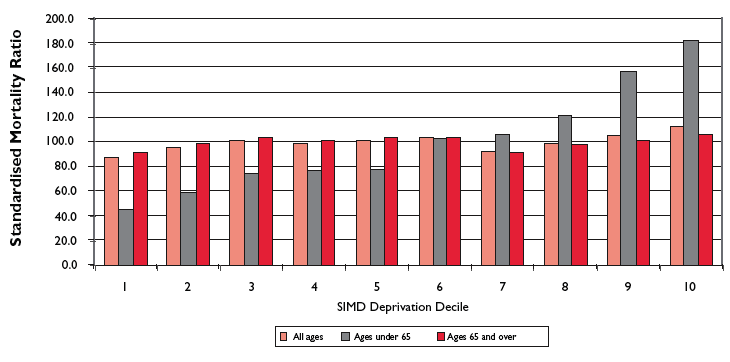
Figure 4: Cerebrovascular disease standardised mortality ratios, by SIMD deprivation decile, 2002-06
3.38 According to recent published research ('Effect of financial incentives on inequalities in the delivery of primary care in England', The Lancet 2008; 372: 728-36), there has been a narrowing of differences in the QOF achievement for practices in areas of relatively high and low deprivation in the years following its introduction against a background of overall rising achievement. The QOF therefore has the potential to continue to contribute to the reduction of health inequalities.
3.39 The Public Health Service ( PHS) component of the community pharmacy contract is being used to target resources to tackle inequalities. Community pharmacies, located where people live, are well placed to help provide patients and the public with personal care closer to home, including measuring weight, calculating BMI, measuring total and HDL cholesterol, blood pressure and blood glucose monitoring. Some NHS Boards have local initiatives to allow some community pharmacies to provide blood pressure monitoring. The introduction of the Chronic Medication Service may provide an opportunity for developing a national approach.
Action:
The Scottish Government should consider extending the community pharmacy contract to include blood pressure monitoring, phlebotomy and ECGs where appropriate.
'Hearty Lives'
The British Heart Foundation's 'Hearty Lives' is a programme of work across the UK in communities with high rates of heart disease. ' BHF Hearty Lives Dundee' will include extending the 'Keep Well' health checks to 40-44 years and to particular at-risk groups of staff, further exploiting the potential for opportunistic health checks and exploring new ways of delivering services to those who are reluctant to access them.
3.40 As noted at paragraph 3.14, in the UK there is a high rate of CVD among South Asians ( i.e. people who have ancestral origins in the Indian subcontinent). Compared with the rest of the population, mortality rates in Indian subcontinent-born populations are 50-60% higher than the standard population. The incidence of acute myocardial infarction in South Asians living in Scotland is 60-70% higher than in the standard population. Developing primary care programmes to identify and manage cardiovascular risk in high-risk populations such as these should be part of strategies to reduce CHD. People from specific ethnic groups such as Asian, black and Afro-Caribbean, are also at greater risk of experiencing a stroke.
3.41 Recording of ethnicity status of newly registering patients in the GP record has been part of the QOF since April 2006. In November 2008, a Directed Enhanced Service ( DES) was introduced extending this to all registered patients, with the aim of 80% of patients having ethnicity status recorded by April 2011. This DES also included the recording of the need for an interpreter, including sign language.
3.42 A study on myocardial infarction in South Asians, reported in Biomed Central Public Health 2007, 7:142, concluded that it was worrying that South Asians in Scotland are at greater risk of heart attack than a Scottish population notorious for its susceptibility to heart disease. The clinical and epidemiological challenges for prevention, control and rehabilitation of CHD in South Asians are therefore formidable, although survival after AMI in South Asians seems to be comparatively good.
3.43 The Kush Dil (Happy Heart) project was set up in Edinburgh in 2002 to manage cardiovascular risk in South Asians. An assessment of its impact was published in the Journal of Public Health (Vol 29, No 4, pp 388-397) in August 2007. It developed and tested methods for a locally-based, culturally sensitive CHD prevention and control service for South Asians. The project led to a reduction in cardiovascular risk factors amongst participants, who also reported a shift in their motivational status, increasing the likelihood that diet and lifestyle changes are maintained. A further report on the project will be written up by Community Food and Health (Scotland) to share with others in the third sector learning on working with BME communities.
3.44 Future initiatives should adopt the key features of this programme: a targeted community approach that is grounded in a practical understanding of the high-risk group, and one that is culturally sensitive, flexible and accessible (run in a familiar environment) and which fosters good relationships with the at-risk community. For such services to be implemented nationally, on a larger scale, further evaluations are needed to provide rigorous data on effectiveness and cost-effectiveness.
'Community Heart'
The Tayside Cardiology unmet needs project, known as 'Community Heart', which ran from April 2006 to December 2008, aimed at improving access to specialist cardiology services which are normally hospital-based by offering cardiology clinics in deprived areas of Tayside. This was achieved by using a variety of venues including a mobile clinical unit, non- NHS anti-poverty centres and places of worship, such as the mosque. Some people were identified for specialist review from hospital database searches, but the majority were identified by self-presenting opportunistically for a heart health check. During this assessment, the specialist nurses considered symptoms which might be consistent with undiagnosed or sub-optimally managed CHD. The project illustrates the opportunities which can exist for cardiovascular assessment and specialist cardiology follow-up in community areas such as gala days, mosques, bingo halls and shopping centres.
Action:
Cardiac and stroke MCNs should jointly develop plans for adopting this type of flexible, culturally-sensitive approach in other areas of Scotland by March 2010.
Conclusion
3.45 Having considered these issues relating to prevention, in particular healthy lifestyles and health inequalities, we now look at the services needed by those with established heart disease, or who have