Approved Medical Practitioners - Mental Health (Care and Treatment) (Scotland) Act, 2003 Training Manual
Training material for Approved Medical Practitioners
Section 4. Compulsory Treatment Order ( CTO) - Section 63
Only a MHO can apply for a CTO, once he or she has received two mental health reports. The application would include a proposed care plan and must occur within 14 days of the date of the second of the two medical examinations which gave rise to the mental health report. Doctors should consult the MHO prior to any decision to initiate the CTO application.
Criteria for issuing a compulsory treatment order
- The patient must have a mental disorder.
- Medical treatment is available and would be likely to prevent the mental disorder worsening, or alleviate its effects.
- Significant risk to health, safety and the welfare of the patient, or to the safety of others, exists if medical treatment is not provided.
- The patient's ability to make decisions about his or her treatment is significantly impaired by mental disorder.
- The treatment cannot be provided informally.
The responsible medical officer will provide in the mental health report:
- Confirmation that these criteria have been met, giving reasons to justify each decision.
- A description of the patient's symptoms and consequent effects of the mental disorder.
- The 'measures' that should be authorised under the order.
- The date of the medical examination.
'Measures' authorised through CTOs
'Measures' that could be authorised by the Tribunal following the suggestion of the MHO or mental health report through CTOs include:
- Detention in a specific hospital
- Giving medical treatment
- Requirement to attend at a specified time and place to receive treatment
- Requirement to reside at a specific address
- Requirement to allow home visits by the responsible medical officer, MHO, community psychiatric nurse and appropriate others
- Requirement to inform/obtain approval from of the responsible medical officer to a proposed change of address.
Imposition of community-based 'measures' would only be recommended if they provide a safe alternative to hospitalisation, and voluntary community care had previously failed. The principle of 'least restrictive alternative' of care should remain paramount.
Mental health reports to support a CTO application
Mental health reports for CTOs require that two medical examinations are carried out. Criteria apply to these examinations, which are:
- They must be completed by either two AMPs, or by one AMP and the patient's GP.
- The two medical examinations may occur simultaneously or separately, but no more than five days apart.
- The medical examination should include the assessments noted for an EDC (page 19).
- Consideration of the patient's past psychiatric history and probable success of long-term treatment should be included; advice on these issues should be sought from the MHO and other relevant parties.
- Patients should be able to have their named person and/or an independent advocate with them at the medical examination.
- The two mental health reports should agree on the category of mental disorder.
- The same 'measures' should be specified in the two reports.
- Any doctor who provides a mental health report should be able to attend a Tribunal hearing.
An AMP must also state whether the patient should receive written notice of any CTO application, and whether the patient is capable of arranging representation at a Tribunal. These points should be discussed with the MHO.
CTOs in operation - Section 64
The Tribunal will either:
- Grant the application
- Refuse the application, or
- Authorise an interim CTO.
Granting the application
If the CTO is granted, the stated compulsory 'measures' last initially for six months. The Tribunal may (unusually) specify different or additional compulsory 'measures'.
The Tribunal can also specify 'recorded matters' (Box 2). These are particular types of treatment or services viewed as being essential.
Box 2. Recorded matters The Tribunal records aspects of care from the patient's care plan that are considered to be essential, and notes them as recorded matters. For instance, a sixteen year-old person's need to be cared for in a child and adolescent service may be noted as a recorded matter; if an NHS Board is unable to provide this service to the patient, the Tribunal can refer the issue to the Mental Welfare Commission. The responsible medical officer has a duty to notify ('make a reference to') the Tribunal when a recorded matter is not provided. This must contain the name and address of the patient and named person, as well as the reason for the reference. The patient, named person, MHO, Mental Welfare Commission, and any guardian/attorney must also be notified of the reference to the Tribunal. |
Once the Tribunal has made the CTO, any removal to hospital under the order must occur within seven days.
The responsible medical officer must prepare a care plan. The care plan will reflect the 'proposed care plan' (proposed by the MHO for the Tribunal) and will contain details of:
- The medical treatment
- Community services
- Any other services or treatment to be given.
Interim CTO
An interim CTO is authorised by the Tribunal when it is felt additional information is required before it can determine the application. The interim order lasts for up to 28 days.
Best practice dictates that a care plan be developed and implemented during an interim CTO. The responsible medical officer can revoke the interim order if detention criteria are no longer met under its duration, but must give written reasons to the patient, named person, MHO, Tribunal, Mental Welfare Commission, and any guardian/attorney.
No more than two interim CTOs with a total of 56 consecutive days can be authorised.
Reviewing the CTO
The criteria applied during review are the same as those applied during application. The presumption applied is that the criteria are no longer being met - the responsible medical officer must therefore be able to demonstrate that the criteria are still being met to justify continuation.
Mandatory review must occur during the last two months of the order, bearing in mind that an initial order lasts for six months. Extensions last another six months, and thereafter for 12 months.
Mandatory review for a CTO occurs two months prior to expiry of the order and must consist of:
- Medical examination of the patient, including a determination of whether criteria for compulsion are met.
- Consultation with the MHO, relevant service providers, and other appropriate individuals.
Best practice suggests that a mandatory review should involve a case conference. Further (less formal) reviews are mandatory 'from time to time'.
Following review, the responsible medical officer may:
1 Revoke the CTO (Section 82). If the responsible medical officer revokes the order using Section 82, written notification giving reasons for revocation must be sent to several parties (Box 3).
Box 3. Notification list for revocation or variation of a compulsory treatment order
|
2 Apply to the Tribunal to vary the compulsory measures or recorded matters
(Section 95) in the order. This is done after review and consultation with the MHO and other relevant service providers lead the responsible medical officer to believe that a variation in the CTO terms is required. The intention to vary the order must be communicated to several parties (Box 3). The Section 95 application will contain: the name and address of the patient and named person; the details of the modification to the compulsory measures and/or recorded matters being sought; and whether or not the MHO is in agreement with the application. The most recent draft of the patient's care plan and mental health report should accompany the application.
The care plan should state:
- Which compulsory measures have been granted
- Which recorded matters have been specified
- When the next mandatory review of the order is due.
3 Extend the order, with (Section 92) variation in the compulsory measures and/or recorded matters. When the responsible medical officer wishes to extend the CTO but vary its terms he or she must notify the MHO beforehand, usually at least two weeks prior to expiry. The other parties who need to be notified about a Section 92 application are shown in Box 3.
The Section 92 application to the Tribunal must take account of the MHO's and any other relevant service providers' views. It must state: the name and address of the patient and named person; what modifications of compulsory measures or recorded matters are being sought, with accompanying reasoning; and whether or not the MHO consents to the application. The responsible medical officer should also provide the most recent draft of the patient's care plan alongside the Section 92 application, and the MHO will also provide a report.
4 Extend the order without (Section 86) variation in the compulsory measures and/or recorded matters. The responsible medical officer must notify the MHO if he or she wishes to extend the order under Section 86 without a variation in terms, usually two weeks before expiry. The responsible medical officer's record of determination to extend the CTO must contain: the reasons for the extension; a note of what type of mental disorder exists; and whether or not the MHO agrees to the extension. This record goes to the parties shown in Box 3. The responsible medical officer is allowed to withhold the record from the patient only if significant harm to the patient or others would ensue. If the record is withheld, the reasons must be noted.
The Tribunal does not need to review the responsible medical officer's Section 86 determination unless:
- There is disagreement between the RMO and the MHO on the need for extension.
- The MHO has failed to inform the responsible medical officer of whether or not he or she agrees to the extension or with the original order.
- No Tribunal hearing has been held on the CTO for two years.
Rights of Appeal
The patient or named person can appeal to the Tribunal for revocation of a Section 86 (extending order) or, at least three months after the imposition of a CTO, Section 92 or 95.
Non-compliance with a CTO
Non-compliance is a serious issue. The responsible medical officer has the authority to have a non-compliant patient taken into custody and conveyed to hospital on the grounds that:
- Efforts to contact the patient have failed.
- It is urgent and likely to prevent a significant deterioration in the patient's mental health.
The relevant sections of the 2003 Act involved are:
- Section 112 (non-compliance with 'attendance requirement')
- Section 113 (detention for 72 hours in hospital)
- Section 114 (non-compliance with a CTO)
- Section 115 (non-compliance with an interim CTO).
Sections 112 and 113
Where the only lack of compliance is with the 'attendance requirement' of the CTO, the responsible medical officer can invoke Section 112, after MHO consent has been obtained.
Section 112 allows the patient to be conveyed to the place of treatment, or hospital, and be detained there for up to six hours to allow administration of medical treatment under Part 16 of the 2003 Act.
Section 112 should be used in preference to Section 113, where appropriate, consistent with the principle of least restrictive alternative. Once the patient is in hospital, detention of 72 hours under Section 113 is allowed. Once the initial 72 hours has expired, further detention can be authorised through invoking Section 114 or 115.
Sections 114 and 115
After the initial 72 hours has expired following actioning of Section 113, further detention of 28 days can be authorised through the responsible medical officer completing a Section 114 for a CTO, and a Section 115 for an interim CTO.
Section 114 is granted and signed by the responsible medical officer. It must state his or her reasons for believing that a significant deterioration in the patient's mental health is likely if he or she is not further detained in hospital.
Detention under Section 114 would start at the point when the certificate was granted, and would last a further 28 days if the following criteria apply:
- The patient is currently under Section 113 (that is, within the 72 hours specified).
- The patient has been examined by the responsible medical officer or another AMP.
- The responsible medical officer is considering whether the specified compulsory measures need to be varied, such as making a Section 95 application to the Tribunal.
- The patient's MHO consents.
- The responsible medical officer has consulted the patient's named person, where practicable.
The criteria for Section 115 (non-compliance with an interim order) are as above.
Once Sections 113, 114 and 115 are in place, the specified compulsory measures of the CTO are suspended, except for those relating to the administration of medical treatment.
Comparisons of the conditions and effects of CTOs between the 1984 and 2003 Acts are shown in Tables 6 and 7.
Table 6. Compulsory treatment order/Section 18 - order conditions
2003 Act Part 7 (Section 57-129) |
1984 Act (Section 18-23 and Section 27-34) |
MHO application, which specifies compulsory measures sought, medical treatment proposed, other |
MHO application which states need for detention in hospital for treatment |
Two mental health (medical) reports, one MHO report and a proposed care plan ( PCP) |
Two medical reports, MHO application One AMP (Section 20) and one GP or, if exceptional, two AMPs |
Two AMPs or one AMP and one GP or one AMP and one GP |
|
Both medical reports must specify at least one of the same types of mental disorder |
Specify same mental disorder |
Treatment likely to prevent mental disorder worsening or alleviate symptoms or effects |
Treatment likely to alleviate or prevent deterioration in condition |
Significant risk to health, safety or welfare of patient or safety of any other person, decision-making ability re medical treatment is significantly impaired and order is necessary |
Necessary for health or safety of patient or for protection of other persons that he should receive medical treatment in hospital |
Mental health reports must specify compulsory treatment measures |
No measures specified |
Dispense with notice to patient if notice is likely to cause significant harm to patient or other person |
Dispense with service on patient if likely to prejudice health or treatment |
No more than five days between mental health reports |
No more than five days between medical reports |
No conflict of interest in relation to medical examination |
No pecuniary interest or relationship with patient |
Separate medical examinations unless consent from patient (if capable) or named person/guardian/welfare attorney (if incapable) |
Separate medical examinations unless consent |
Notification by MHO to patient, named person and Mental Welfare Commission |
MHO informs nearest relative unless impracticable |
MHO informs patient of right to advocate and helps patient access these services |
|
MHO prepares report and PCP |
|
Application to Tribunal within 14 days of second mental health report for detention in hospital or treatment in community |
Application to Sheriff within 14 days of MHO interview and seven days of of later medical report. For detention in hospital |
Tribunal hearing. Right to attend for patient, named person, Guardian or Attorney, MHO, doctors, primary carer, curator ad litem, anyone else with an interest in the application |
Sheriff Court hearing. Right to attend for patient, nearest relative, patient's representative, mental health officer |
Tribunal can make order sought in whole or in part and can specify measures other than those set out in the application |
Sheriff can grant or refuse application |
Emergency and short-term detention extension certificate extends detention for three working days (from date of issue for emergency detention and from end of 28 days for short-term detention) |
Section 26 extended for up to five working days |
Detention under short-term and/or extension certificate extended by five working days once application for CTO made |
Sheriff court hearing within five working days (Section 21.) Section 26 extended until application determined |
Tribunal decision before end of five working-day extension period. |
|
Removal to hospital or specified place of residence within seven days of CTO |
Removal to hospital within seven days |
Table 7. Compulsory treatment order/Section 18 - order effects
2003 Act |
1984 Act |
|---|---|
The CTO lasts initially for six months |
Lasts initially for six months |
Tribunal can make interim order for up to 28 days. The total length of the interim order may not exceed 56 continuous days |
No interim orders, but Section 26 extended until final determination |
No interim order without opportunity for patient to be heard |
|
|
Order authorises detention in hospital but leave of absence with or without conditions possible later for specified maximum periods of time |
Responsible medical officer duty to review interim and final compulsory treatment order, within two months of end of order. Duty to consult MHO and others |
Responsible medical officer duty to review within two months of end of Section 18. Duty to consult those involved with treatment |
Mental Welfare Commission power to evoke CTO |
Mental Welfare Commission power to discharge detailed patients |
Responsible medical officer duty to make care plan (Section 76) |
|
Responsible medical officer power to extend by six months and then by 12 months. Consent of mental health officer must be sought |
Responsible medical officer power to extend by six months and then 12 months |
Appeal to Tribunal against extension |
Appeal to Sheriff against renewal |
Failure of a community-based patient to attend for treatment gives responsible medical officer or authorised representative power to take patient to hospital or specified place and keep him or her there for up to six hours to give treatment or to determine whether capable of consenting to treatment |
Absence without leave or failure to comply with conditions of leave of absence gives mental health officer hospital staff, constable and persons authorised by managers of hospital power to take patient back to hospital |
Failure to comply generally with CTO in community gives responsible medical officer or authorised person power to take patient to hospital for up to 72 hours for examination and for further 28 days if considering variation or application to Tribunal. MHO consent needed. Patient can apply to Tribunal to revoke |
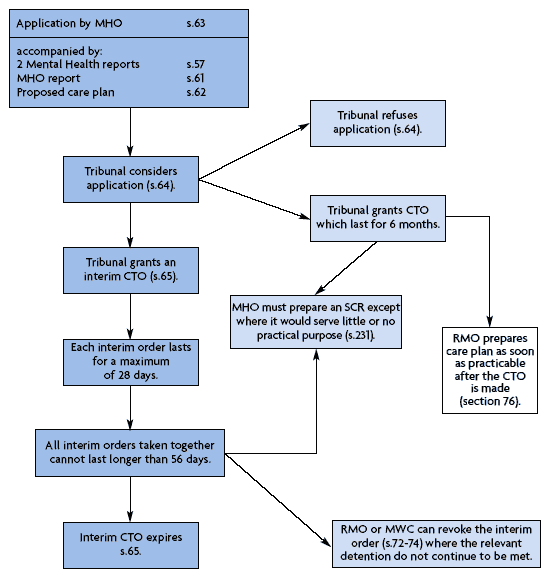
Consideration of a Compulsory Treatment Order Application - Flowchart