Approved Medical Practitioners - Mental Health (Care and Treatment) (Scotland) Act, 2003 Training Manual
Training material for Approved Medical Practitioners
Guide for medical practitioners on the granting of an emergency detention certificate under section 36 of the Mental Health (Care and Treatment) (Scotland) Act 2003
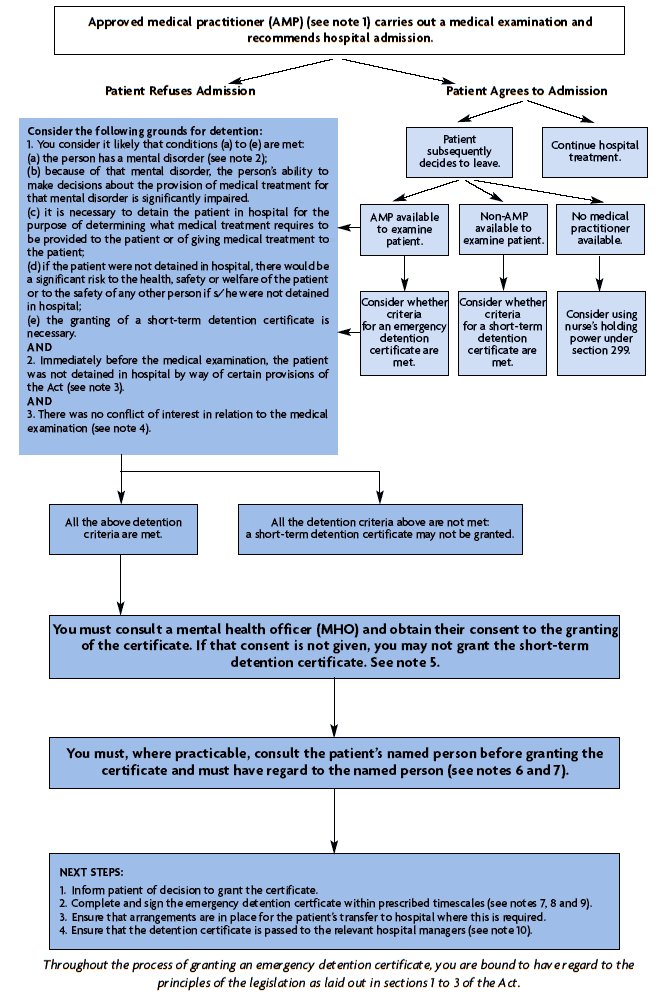
Note 1: Any registered medical practitioner may grant an emergency detention certificate. You do not have to be an approved medical practitioner.
Note 2: Section 328(1) of the Act defines "mental disorder" as "mental illness, personality disorder or learning disability, however caused or manifested". Section 328(2) further states that a person is not mentally disordered by reason only of sexual orientation; sexual deviancy; trans-sexualism; transvestism; dependence on, or use of alcohol or drugs; behaviour that causes, or is likely to cause, harassment, alarm or distress to an other person; or acting as no prudent person would act.
Note 3: The relevant provisions are set out at section 36(2) of the Act and they are: an emergency detention certificate; a short-term detention certificate; an extension certificate issued under section 47 of the Act pending an application for a CTO; section 68 of the Act (i.e. the extension to the detention period authorised once a CTO application has been submitted to the Tribunal); a certificate granted under sections 114(2) or 115(2) of the Act (i.e. a certificate issued subsequent to a patient's non-compliance with the terms of a community-based interim CTO or a CTO). [ DN - Add something in about definition of "immediately before"? (depending on content of Code on this point)]
Note 4: [ DN - conflict of interest material to be added once regs/Code of Practice material have been finalised]
Note 5: The medical practitioner must consult and seek the consent of an MHO to the granting of the certificate. All reasonable efforts should be make to contact an MHO. However, where the urgency of the situation is so great that it would not be practicable for this consultation to take place then it is permissible for the practitioner to grant the EDC without consent. [ DN - Add in best practice material about consulting and discussing the situation with other members of the multi-disciplinary team depending on what the final version of the Code says.]
Note 6: Best practice would be that if one MHO refuses to grant consent, then .... [ DN - revise according to the final version of the Code]
Note 7: A valid emergency detention certificate can be issued on any document if form [x] is not available. However, it is strongly recommended that form [x] be used in all circumstances. If form [x] is not used, the emergency detention certificate must state the practitioner's reasons for believing the conditions mentioned at points 1 and 2 on the blue box overleaf to be met and must be signed by the medical practitioner.
Note 8: The emergency detention certificate must be completed either by the end of the day on which the medical examination takes place (if the examination takes place before 8pm) or within 4 hours of the medical examination being completed (if it takes place after 8pm).
Note 9: The emergency detention certificate authorises, first, the patient's transfer to hospital within 72 hours of the certificate being granted; and, secondly, the patient's detention in hospital for 72 hours.
Note 10: Section 36(7) of the Act states that the patient's detention in hospital is only authorised is the emergency detention certificate is given to the managers of the hospital before the patient is admitted to hospital under the authority of the certificate. If the patient is already in hospital when the certificate is granted, then the certificate must be given to the hospital managers as soon as practicable after it was granted [ DN - clarification of "hospital managers" required? depends on final content of Code on this point].
The purpose of this leaflet is to act as a guide only. It does not provide full and comprehensive coverage of everything you ought to know about emergency detention. For fuller information, please consult the Act and its Code of Practice.