Transforming Outpatient Services: Patient Reminder Services Change Package
Package of information and resources providing details re how to plan, adopt, implement and monitor effectiveness of patient reminder services and includes evidence base, resources, information and contacts for NHS teams to use.
Aim, vision and making it happen
Transforming Outpatient Services is aimed at supporting NHS Boards and local partnerships to move care closer to home and enable more people to receive the right care, from the right person, at the right time, in the right place.
It supports teams working together with patients and the public to understand and diagnose system issues, design and innovate and use continuous improvement to deliver high quality person centred care and best value for money.
Healthcare teams, working with patients and public representatives, have developed Towards Our 2020 Vision a picture of how the services that we currently call outpatient services will need to change for patients and staff as we move towards 2020. (Towards Our 2020 Vision is available in poster format from QuEST.)
Now all NHS Boards working with partners are beginning to take the strategic actions necessary to create the contextual, cultural and leadership conditions to enable staff, practitioners and patients to achieve their 2020 vision. Some Boards have already formalised outpatient transformation as a strategic priority. In other Boards specialties, or teams are undertaking improvement led by enthusiastic service managers, or clinicians who may or may not have been given support and resource.
Four NHS Boards have been commissioned (2012-2014) to use three different improvement methodologies: invention and innovation through technology, benchmarking to improve utilisation of appointment resources and clinic space, and rapidly testing changes and contributing to change packages that help spread reliable improvements.
During year 2013/14 Chief Executives of all NHS Boards agreed to support rapid adoption and spread of five evidence based, high impact change concepts. Adopting and spreading systematic use of reliable patient reminder services is one of these. (See the Transforming Outpatient Services Driver Diagram.)
Are we making the right changes?
The rationale for providing reminder services is that more people will arrive for their planned appointment and where appointments need to be cancelled the appointments are made available for other people to use. There are many reasons that contribute to people not attending outpatient appointments. Deprivation, age and clinical specialty are factors. People may feel that their condition has improved, or do not receive the right information. More efficient use can be made of available resources. The average cost of a traditional outpatient appointment in 2013/14 is £115.
What's the purpose of the change package?
The change package describes in detail the steps needed and how to plan for, how to adopt, how to implement and how to monitor effectiveness of patient reminder services. It includes evidence base, resources, information and contacts for teams to use.
The package is the result of webex and face to face learning sessions and workshops (from April to September 2013) involving people who have day to day responsibility for managing and providing safe, effective and person centred appointment booking processes and colleagues in NHS Special Boards.
How do we use the change package?
1. Familiarise yourself with change package, sustainability guidance, resources & experiential learning from other Boards
2. Form a multidisciplinary project team with enough autonomy to implement change: ensure public and senior management buy-in
3. Assess readiness & understand current state: apply the principles of improvement methodologies (e.g. DCAQ, process map)
4. Identify changes you will make: consider the factors that first need to be addressed to help build sustainable change
5. Implement your changes: apply the principles of improvement methodologies (e.g. PDSA cycles)
6. Maintain your improvement: evaluate, sustain, modify (as required) and spread
Spread and sustainability
The concept of providing patient reminder services incorporating telephony and digital systems has moved beyond the innovation phase. Prototype services and systems have been tested in a range of Boards, sites and specialties and some spread has taken place. This has enabled us to amass evidence and information about creating the right conditions including leadership for change, intended and unintended consequences, costs and benefits and factors affecting reliability. This change package will guide teams through the decision to adopt and implementation phases. Sustainability although depicted as the final stage of the framework below should be planned for from the very early stages.
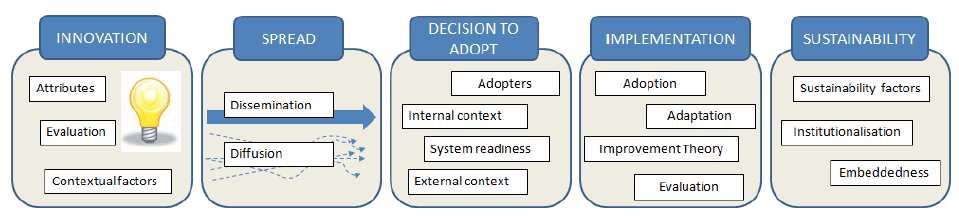
(Health Improvement Scotland Spread and Sustainability Framework)
The usefulness of this change package has been tested. However, we aim for it to be a live document that incorporates new findings and examples from research and experience as knowledge develops.
Any feedback is very welcome. Please contact gillian.borthwick@scotland.gsi.gov.uk
| Change Concept | Change Package | Essential Resources |
|---|---|---|
| Reduced DNAs by utilising reminder systems (PRS) Outcome: 2016: Reduction in DNAs to 7% (Represents achievement of 2013 upper quartile). 2016: Review and reset See the Transforming Outpatient Services Measurement Plan for definitions and more detail. Rationale:
There are many reasons that contribute to people not attending outpatient appointments. Deprivation, age and clinical specialty are factors. People may feel that their condition has improved, or do not receive the right information. Non-attendance at clinics can cause system inefficiencies, as teams tend to respond by overbooking. This can lead to bottle necks in the system. Several methods aimed at increasing the number of people who attend a planned appointment have been researched. These include text, telephone, email and letter reminders. Research demonstrates that these approaches decrease the number of 'failed to attends'. For example, reductions of 29-39% from the baseline DNA rate. NHS 24 provides evidence of reduction in DNA rates associated with use of their propensity model and focussed reminder services for those most likely to fail to attend. Success of the reminder service has been shown to be linked with the appointment booking and confirmation processes being used. Healthcare Improvement Scotland literature reviews: |
Communication and engagement
|
Local media (press & radio) Signs /posters/leaflets/ stickers for: NHS Board Outpatient Departments GP surgeries Patient letters
|
Capture and communicate current demographics, additional needs and preferred mode of communication
|
||
Design Patient Reminder Service and select system provider(s)
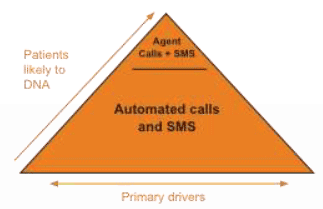 * Ref: NHS 24 |
Factors to Consider when choosing provider(s) (Chronos 360, Netcall and NHS 24) Data
(Methods (channels) can be stand alone or blended)
Economic evaluation of propensity model. (to follow) Contact logistics
|
|
Implement Patient Reminder Service
|
|
|
Review demand and capacity management at the start and on an on-going basis
|
||
On-going communication and review
|
Post-implementation publicity suggestions:
|
Contact
Email: Fiona Bernardis
