Transforming nursing, midwifery and health professions roles: education and career development
The fifth in a series of papers on the Transforming Roles programme focuses on education and career development.
Paper 5 - Transforming education and career development in nursing
This series of brief papers on the Transforming Roles programme aims to update stakeholders on the professions' contribution to the wider transformational change agenda in health and social care in Scotland. The fifth paper outlines the education and career development pathways model, which underpins the transformation of nursing roles and was developed during Phase 1 of the programme.
Background
The Chief Nursing Officer ( CNO) is committed to maximising the contribution of the nursing, midwifery and health professions ( NMaHP) workforce and pushing the traditional boundaries of professional roles. The Transforming Roles programme aims to provide strategic oversight, direction and governance to:
- develop and transform NMaHP roles to meet the current and future needs of Scotland's health and care system
- ensure nationally consistent, sustainable and progressive roles, education and career pathways.
Phase 1 of Transforming Roles focused on nursing roles.
Rationale
The vision of the Health and Social Care Delivery Plan [1] is for integrated services focusing on prevention, early intervention and enablement to support people to live well for as long as possible in their own homes and communities. Where hospital care is required, it must be of the highest quality and safety, with the person at the centre of all decisions. The aim is to ensure people get back to their home or community environment as soon as possible, with minimal risk of readmission.
NMaHPs, working alongside professional colleagues in integrated teams, play a critical part in realising this vision. Their roles have developed and expanded to meet new challenges, but scope now exists for transformational change for future roles. This must be supported by targeted post-registration education and continuous professional development ( CPD) that is embedded across career pathways.
NHS Education for Scotland ( NES), a special health board working in partnership with stakeholders to develop and deliver education, training and workforce development for those who work in and with the NHS in Scotland, is working with the CNO and other partners to plan and deliver education, innovation and workforce development to maximise the potential of NMaHP roles in Scotland.
The overall aim of this work is to develop a structured, coordinated and future-focused model for education and development for NMaHPs beyond registration. This will ensure the most appropriate, skilled and flexible workforce is adequately prepared and supported to help deliver necessary innovations in care delivery now and in the future.
As the Nursing 2030 Vision [2] describes, nurses will be working not only in different settings with different teams, but also in different ways – education and CPD will be central to ensuring they are equipped to develop their roles appropriately.
Phase 1 of Transforming Roles has been driven by Setting the Direction [3] , the CNO's review of nurse education. NES is leading on Aim 1 of Setting the Direction, which is to develop a sustainable national approach to post-registration and postgraduate education and CPD that will support nurses and midwives across career pathways, from registration to specialist, advanced and consultant roles.
The education and career development pathways model
The model's main purpose is to establish education and development pathways from registration through to advanced and consultant practice that align with and support changing service needs.
The model is based on key principles that aim to ensure:
- a clear transition from undergraduate to postgraduate education
- a refocused balance between generalist and specialist practice, demonstrating increasing levels of generalist skills from registration through to advanced- and consultant-level practice
- structured career pathways, with specific benchmarks for education and CPD at each stage that reflect increasing complexity and responsibility
- an education and development framework, enabling those on the pathway to gain the necessary skills to meet specific clinical/operational needs at any stage
- flexible approaches to education and learning that allow the acquisition of new and advanced skills.
The model draws on the general principles of the Shape of Training Review [4] , which sets out proposed reforms to the structure of postgraduate medical education and training across the UK. It also aligns with the NES Post-registration Career Development Framework for NMAHPs [5] , which incorporates the four pillars of practice: clinical; leadership; facilitating learning; and evidence, research and development. The framework will help people navigate their way through the pathways.
An outline of the model is shown in Figure 1, which follows the Skills for Health framework.
Figure 1. Education and career development pathways model
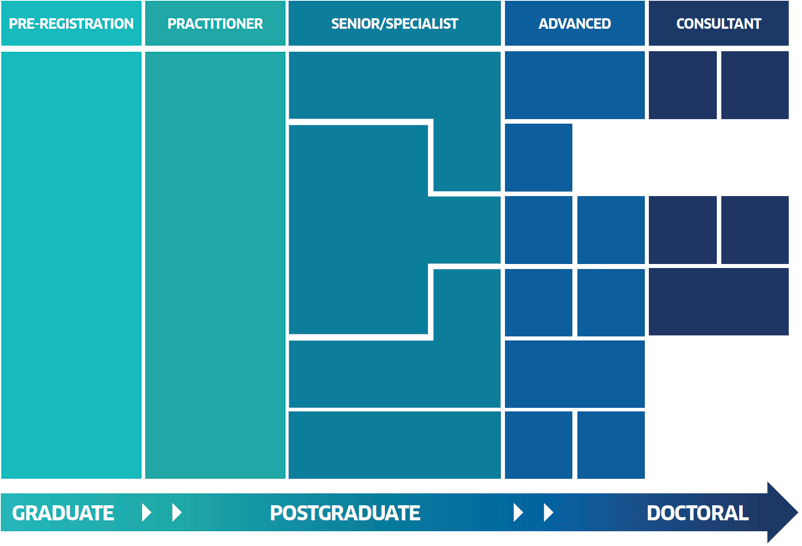
The model shows the transition from undergraduate to postgraduate education. Rather than single specialist education pathways, it advocates broader (but higher-level) core, generalist education components, such as mental health, leadership, prescribing, public health, and clinical assessment and decision-making (illustrated as 'learning' blocks in Figure1). More flexible approaches to gaining knowledge and skill for advanced- and consultant-level practice are in place, allowing the acquisition of new knowledge and skills related to emerging priorities and future innovations in health care.
The model facilitates the delivery of education covering core and role-specific components that will act as a foundation for further development at practitioner level and as a springboard for more specific and higher-level learning required by practitioners as they diversify into more specialised roles or advanced levels of practice to meet the complex needs of people and populations. This will ensure a workforce 'pipeline', attracting practitioners to specific areas of practice linked to service need to ensure succession planning and a sustainable and flexible workforce, and offer practitioners incentives for career development to practice to the full extent of their capability at each level of practice.
Education benchmarks to inform career pathway progression from pre-registration to consultant-level practice are a key feature of the model. An indicative example of benchmark points is provided in Figure 2, reflecting increasing complexity and decision-making across the levels of practice.
Figure 2. Education and career development pathways model: benchmarks [6]
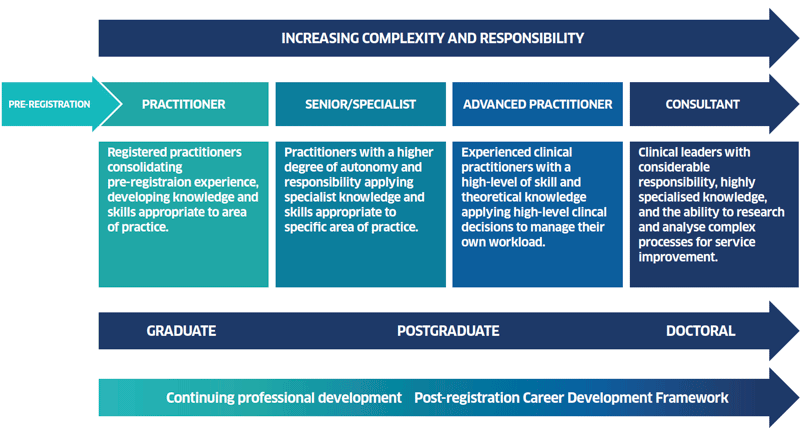
Progress to date: Phase 1
In addition to development of the model, which provides an overarching framework for structured sustainable education and role development pathways from transition at registration through to advanced- and consultant-level practice, a nationally consistent approach to advanced nurse practitioner ( ANP) education has been defined. This is based on the role and expectations identified in the report from the Transforming Nursing Advanced Practice Group. [7]
Scoping of education provision in Scotland that meets the ANP definition and competencies has been carried out with higher education institutions, and service and education needs analyses for ANP roles have been undertaken with NHS boards, integrated joint boards, primary care services, care homes and hospices to identify ANP education required over the next four years. Specific competencies for ANPs in paediatric and neonatal, primary and community care, mental health and acute settings have been defined to shape education in these areas. This will be further supported by the publication of a refreshed ANP toolkit.
Developing an integrated community nursing team [8] pathway was a key priority in phase 1. Core and specific education has been identified to support career pathways in community nursing. An example of core components of a community nursing pathway is shown in Figure 3. Role-specific education, such as child protection, would be tailored as necessary to role requirements within integrated community nursing teams.
Figure 3. Career pathway model: example community pathway
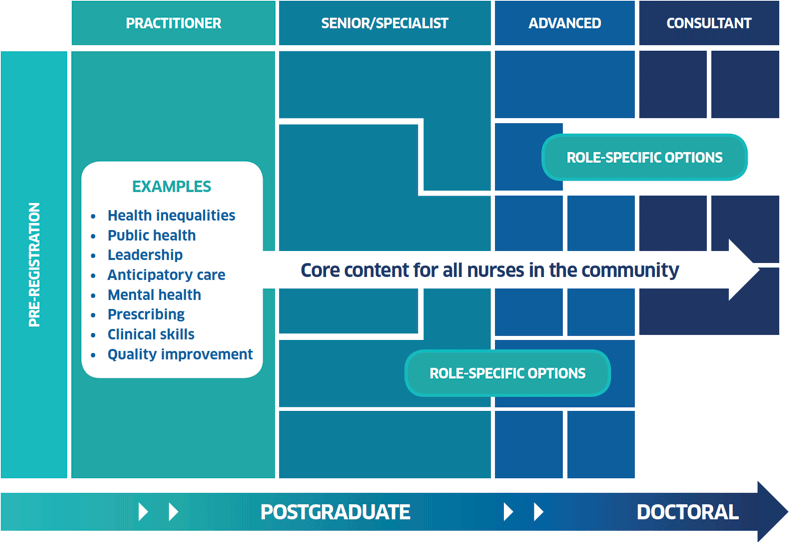
Other NES activity to date includes:
- facilitating a four-day national CPD programme for the wider health visiting workforce that included a focus on the Children and Young People (Scotland) Act 2014 and the Named Person role
- delivering a two-day CPD programme in three Scottish regions to support the wider school nursing workforce to meet the refocused school nursing role
- scoping the education and preparation of other children and young people's nursing roles (such as community children's nurses and looked-after children's nurses).
Moving forward: Phase 2
Moving forward, the education focus is now on widening application to other health professionals, nurses and midwives, and building on the strong education foundation established around transformation of roles. Overseen by a postgraduate education and development group, work in progress includes:
- securing agreement on core and specialist education requirements to support career pathways and populate them in accordance with output from the Transforming Roles programme
- further exploring and agreeing a national approach to strategic education commissioning
- introducing mechanisms for implementing, testing and evaluating role developments to inform future plans and models of provision for post-registration education
- building capacity and capability of those supporting learning in practice
- considering how the pathway model could translate to other roles.
NES will work with NHS boards, integrated joint boards, education providers and other strategic partners to progress the education and/or development required for role transformation, including core course requirements and CPD, to ensure a well prepared workforce pipeline for the future. A new curriculum has been developed for nurses working in schools and with the school-age population.
In light of the priorities of the Health and Social Care Delivery Plan and the emerging workforce plans, structured, coordinated and future-focused education and development beyond registration will be essential to the success of the Transforming Roles programme.
NES will continue to work in collaboration with key stakeholders to lead education development to support the Transforming Roles agenda with the aim of ensuring:
- practitioners are appropriately prepared for new and enhanced roles
- education and commissioning are based on local and regional service needs analyses
- new roles and associated education are configured to support service transformation
- practitioners are enabled to practice to the full extent of their capability
- the objective to recruit, develop and support a highly skilled, effective and professional workforce aligned to service requirements is achieved
- a robust education commissioning plan is in place to ensure best value and sustainability.