Strengthening the Commitment: Living the commitment
This report celebrates the achievements of learning disability nurses across the United
Kingdom and the difference they have made, and continue to make, to the lives and health
outcomes of people with learning disabilities
3 What have we achieved?
Focus on capacity
Accurate information about where learning disability nurses work is important for workforce planning. The challenge set by Strengthening the Commitment was to scope the learning disability workforce, including those working in the independent and voluntary sector and in social care so that strategic workforce development plans could be developed.
Learning disability nurses have a history of working in a wide variety of settings in health and social care. Consequently it can be challenging to obtain accurate figures of where and how many learning disability nurses are working and in what roles. This is particularly so across the independent sector where there are many individual employers and no centrally collected data for numbers employed. Where we have available data we will continue to monitor trends in workforce numbers and settings. It is clear that there continues to be a need to strengthen the numbers of learning disability nurses, particularly as the numbers of people with learning disabilities increases.
The holistic, person-centred skills of learning disability nurses are valued in the prison service, secure services, forensic services, children's services, general practice, social care (where they may not be employed as registered nurses), the police, voluntary sector, the community, and with families, as well as in the acute sector, accident and emergency and neurosciences. Without good information about the location and activities of learning disability nurses it is difficult to move forward.
The four UK health departments, together with key partners, have held three engagement conferences with the independent and voluntary sector. The aim was to establish better understanding of, and planning for, a high quality and sustainable registered learning disability nursing workforce across all sectors. An Independent Sector Collaborative is taking this work forward.
'The issue is not the lack of services but rather the lack of specialist professionals and expertise working within primary and secondary healthcare.'
Carer, mother of adults with learning disabilities
Positive practice (Northern Ireland)
Strengthening capacity: responding to clients with complex needs
A core skill of learning disability nurses is to work with people who have complex needs and who may present with challenging behaviour. When a breakdown happens for such clients, skilled learning disability nurses can work as part of a crisis outreach team to stabilise the client's care and condition so that the individual does not have to be admitted to an acute hospital setting. The following case study illustrates how this vital service has been developed in Northern Ireland.
The challenge
Clients with complex learning disability needs who present with mental ill health or behaviour that challenges need specialist care. The challenge was to provide effective support for individuals to enable them to stay in their own homes and avoid unnecessary admission to hospital where possible.
The journey
The Southern Health and Social Care Trust (SHSCT) developed a Learning Disability Crisis Response Service to effectively support clients with complex learning disability needs to remain in the community. The purpose of the service is to provide short-term assessment, support and treatment for adults with a learning disability and their carers in an effort to effectively support clients to remain in their own home and avoid unnecessary admission to hospital where possible.
The crisis response service was developed by two learning disabilities nurses to provide expert assessment, treatment, care planning and evaluation for adults with a learning disability who present with mental ill health or behaviour that is perceived as challenging. This is a tertiary service, delivered by a small team of professional staff as a part of community based specialist services for adult learning disability.
The service is delivered in the 'home' environment as a viable alternative to hospital admission. The direct intervention in the home allows the adult with a learning disability to use the support of family and social networks during times of distress to aid the process of recovery. It also allows for the identification of precipitating environmental factors that may lead to an episode of mental ill health or behaviours that are perceived as challenging in the environment where they occur. This provides the opportunity for nursing staff to work collaboratively to deliver an intervention aimed at ameliorating or minimising these factors.
Acute inpatient services for adults with a learning disability now consist of one ward of 10 beds for short-term assessment and treatment, located alongside acute mental health beds on the Bluestone site at Craigavon Area Hospital.
The development of this team demonstrates the commitment of SHSCT to the implementation of regional policy recommendations as set out in Transforming your Care (2011) and The Bamford Action Plan (2012-2015). It also effectively demonstrates how the SHSCT has strengthened the capacity of the learning disabilities nurses to meet the needs of clients whilst delivering on the recommendations within Strengthening the Commitment.
Strengthening capacity is evidenced in the following ways.
- This team delivers a specialist service to adults with a learning disability outside of traditional roles and places of work.
- Organisational and decision-making skills of team members are harnessed to deliver interventions that encourage empowerment, participation, shared decision-making and minimise risk.
- Team members have acquired greater skills and knowledge particularly in liaising with other health professionals and stakeholders.
- Enhanced ability of team members to engage in high levels of autonomous decision making, discretion and clinical with support available if required from consultant psychiatrist on-call.
- The team act in an advisory role to adults with learning disability and their families/carers and a diverse range of health professionals and stakeholders during periods of periods of mental ill health or behaviours that challenge.
- Training carers/independent healthcare providers to build capacity in managing emergency or crisis situations.
The results
Outcomes for service users
Outcomes for people with learning disabilities are evidenced through the reduction in the number of admission to acute learning disability hospital beds in the host trust. There has been a 60% reduction in the number of admission in the 21 months since the team was formed.
Innovation/continued professional development
As part of this team's development there will be ongoing review of skills requirements and associated competencies. As the service grows and develops it is anticipated that further continuing professional development opportunities will be identified including those at a postgraduate level to enhance the existing skill set of the team in providing holistic care to meet the bio-psycho-social needs of clients.
Contacts
Gavin Crilly
Crisis Response PractitionerDorsy Unit, Bluestone,
Craigavon Area Hospital
68 Lurgan Road,
Portadown,
BT63 5QQ
Email: gavin.crilly@southerntrust.hscni.net
Bryce McMurray
Assistant Director Mental Health ServicesSouthern Health & Social Care Trust
Bannvale House
10 Moyallen Road
Gilford,
Co Down,
BT63 5JX
Telephone: 02838833240
Email: Bryce.mcmurray@southerntrust.hscni.net
Positive practice (England)
The role of the learning disability nurse across healthcare services: The perspectives of the mother and practitioner
The aim of acute liaison nurses is to improve standards in hospitals and to ensure that reasonable adjustments are made for people with learning disabilities so that they are able to access health services. Learning disability nurses in the role of acute liaison nurses work with general nurses to give them the confidence to work with people with learning disabilities. The following case study presents the views of an acute liaison nurse and the mother of two men both of whom have learning disabilities and highlights the vital role played by the acute liaison nurse.
The challenge
This case involved a mother and her two sons both of whom have profound learning disabilities and complex care needs. Learning disability nursing input had been stopped because the community learning disability nursing team resource was redirected, leaving the mother struggling day to day and with an unclear direction for service implementation. The family's GP had over 1,000 patients and did not have the expertise to support the family.
The mother's view
'The challenge primarily was transition to adult services for my younger son. I had already been through the transition process for my older son, 11 years before. My honest feeling was that if he had an acute admission to an adult ward he would die.
'Both sons had lots of services involved however these were disjointed and we still relied heavily on outreach and short breaks from the children's hospice. We are thankful this had been continued until my son was 21. This time was challenging because of the lack of services for people who can meet the needs of people with profound learning disabilities in healthcare services. The issue is not the lack of services but rather the lack of specialist professionals and expertise working within primary and secondary healthcare. For example there are no specialist acute consultants which is what is provided in paediatric services.'
The practitioner's view
'The mother had to fill in the gaps left by services including invasive treatment that she was told could not be provided in the community. The learning disability nurse (LDN) identified the need for assistance to support the family and ensured their individual needs were met. The lack of engaged service provision was impacting on both sons' health and wellbeing.'
The journey
The practitioner's view
'The mother has provided exceptional care to her sons, the family's resilience has enabled them to meet the challenges thrown at them. The primary liaison LDN identified the sons' health needs through their annual health checks and followed up on identified health needs from their health action plans, as well as implementing identified reasonable adjustments at their GP practice.
'Both sons had hospital admissions during the past year. This time was stressful, but was eased by the assistance of the acute learning disability liaison nurse who ensured the hospital acute staff were meeting the needs of both sons by implementing reasonable adjustments and arranging for their mother to stay at the hospital.
'The LDN also helped the mother in a care coordinator role. Service provision in the community for her sons had been problematic due to the complexity of their needs and the LDN's role was to ensure the sons' health needs were being met in a person-centred way, to advocate for the family, and work strategically to ensure the community services were competent and meeting their needs.'
The mother's view
'This journey has not been easy, especially due to the unpredictability of my sons' health. It means there have been emergency situations that have meant advocating for both my son's more regularly then any parent should have to. I have found services create barriers, which has meant I have had to fill the void.
'I have had vast experience of adult services for people with learning disabilities and often been told I am unlucky due to my older son being ahead of the increasing population of people coming through transition with profound and complex disabilities. However he has been in adult services for more than 10 years and I have not seen the amount of improvement I would have hoped for.'
The results
The mother's view
'This isn't a situation that can be resolved over night, however the involvement of LDNs across the health services has definitely improved access and treatment for my sons. Having a named person to offer support and bridge the gap between services cannot be undervalued. The answer would be more resources but I am aware this is cannot always be relied upon, but it is often professionals skills which are lacking, this could be resolved by standardised training.
'Health services need to understand that people with profound and complex learning disabilities often have multiple health needs so won't fit into generic health structures where one need is addressed at a time, issues need to be tackled collectively. Looking holistically is a key skill of a LDN.'
The practitioner's view
'The LDN's impact across the health services has ensured steps towards a seamless transition across primary and secondary care as outlined in Valuing People (2001). Being proactive in primary healthcare is looking to reduce premature death among people with learning disabilities whilst the role of acute liaison nurses is to meet deficits in service delivery in secondary care. LDNs have a duty to advocate for improvement to health service delivery to ensure the needs of individuals are being met independently.'
Contacts
Daniel Turner
Community NurseClinical Health Team for People with Learning Disabilities
2nd Floor Civic Offices,
St Nicholas Way,
Sutton,
Surrey,
SM1 1EA
Telephone: 0208 770 6433
Mobile: 07816 079828
Graphics created at Strengthening the Commitment event held at the University of Wolverhampton, 2014. Reproduced with thanks to Staffordshire and South Shropshire Foundation Trust and Pen Mendonca www.penmendonca.com
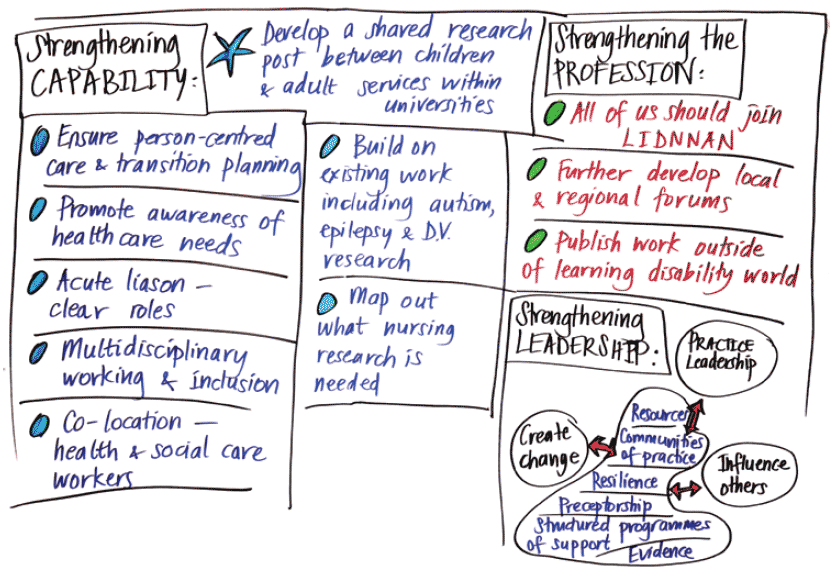
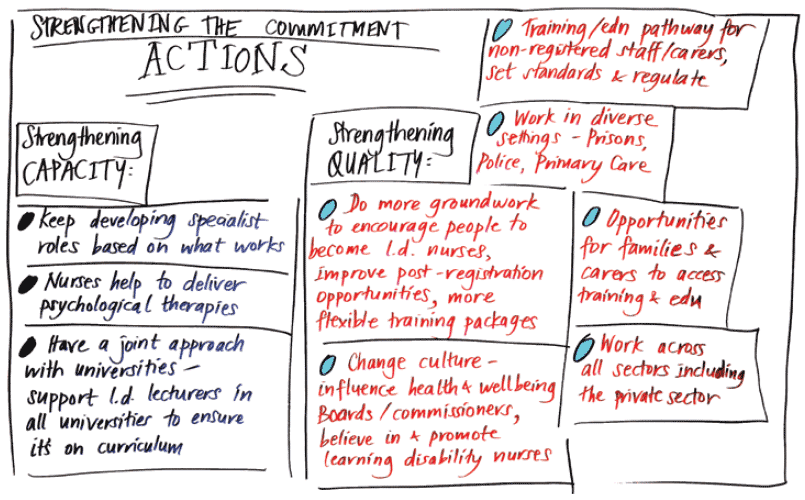
Focus on capability
The challenge set by Strengthening the Commitment was that the skills, knowledge and competencies of learning disability nurses needed to change and extend to reflect the changing needs of people with learning disabilities. Learning disability nurses have an important role to play in supporting timely access to services as well as contributing to preventative and anticipatory care. The following case study relates to strengthening both capacity and capability. It focuses on developing leadership and also enabling experienced learning disability nurses to facilitate learning in practice.
Positive choices: Together we are better
Positive Choices is the only national conference designed to give student nurses the freedom to celebrate the contribution they make to the lives of people with a learning disability. Established before the publication of Strengthening the Commitment, the core Positive Choices team have worked closely with the UK Strengthening the Commitment Steering Group to support implementation and to facilitate the leadership event for 3rd year students. It relies on the goodwill of five universities, speakers who give their time and talents freely, and organisations including the Department of Health, learningdisabiltynursing.com, RCN Learning Disability Practice, who sponsor the event each year.
'Invigorating'
'Supports and inspires'
Positive practice (Scotland)
Developing leadership and facilitating learning in practice
The challenge
The right support is key to enabling people to live meaningful and fulfilled lives. The skills, attitudes, knowledge and confidence in supporting people are central to getting the support right. Service commissioners and providers face a major issue in providing effective, efficient and equitable services for people with a learning disability who present with challenging behaviours. There may be serious consequences for people with a learning disability and behaviours perceived as challenging, including risk of placement breakdown, neglect, abuse and social deprivation, and staff play an invaluable role in supporting them.
The journey
NHS Education for Scotland recognised the role of support workers in supporting people with learning disabilities and wanted to roll out their educational resource: Improving Practice: Supporting people with learning disabilities whose behaviour is perceived as challenging. An educational resource for support workers.
The leadership role of learning disability nurses was recognised and NES recruited experienced learning disabilities nurses from all over Scotland to act as trainers. Trainers attended a series of five workshops to work through a trainer's toolkit that accompanied the resource. Each of the workshops concentrated on a unit from Improving Practice:
- Day 1 Value based care and getting orientated
- Day 2 Positive behavioural support and communication
- Day 3 Active support plans and skills development
- Day 4 Reactive and restrictive practice
- Day 5 Future facilitation and evaluation
These workshop enabled trainers to become familiar with the resource, Improving Practice, and explore how to make best use of the trainer's toolkit. Trainers then worked through the units with their support workers. The fifth workshop concentrated on future facilitation and evaluation.
The results
Trainers gained tremendously from the group work and the networking. One trainer observed the impact that the Improving Practice resource had for the support workers that she facilitated.
'Whilst working through Improving Practice with my two support workers I became aware of a change in their values, their motivation and their interactions with the tenants they were working with. They learnt the skills necessary for planning person-centred care and gained the confidence to implement it, sometimes without the support of the entire staff team. The tenants are being enabled to participate in more active lives and, for one of them, a simple thing like a cup of coffee and a chat with staff before bed has become an integral part of ending the day in a positive way.'
Yvonne Maclean, community learning disability nurse
Support workers also identified the major changes to their attitudes and practice as a result of participating in the programme.
'Doing this course has opened my eyes to how much the individual was capable of doing for himself. Skills have been lost over time as staff were doing for him and not with him. The activity plan now in place enhances his life and builds on his skills. He is a much happier person.'
Marie White, support worker
'From the start of the course my values have changed and the way I work has changed. I look at the individual now, putting them at the centre of everything that I do and try to encourage them to take part in their own lives more.'
Lesley Robinson, support worker
Improving Practice: Supporting people with learning disabilities whose behaviour is perceived as challenging. An educational resource for support workers. Published by NHS Education for Scotland in 2004. This resource is freely available to staff throughout Scotland.
Contacts
Elaine Kwiatek
Education Project Manager Learning DisabilitiesNursing, Midwifery and Allied Health Professionals
2nd Floor, 102 West Port,
Edinburgh
EH3 9DN
Telephone: 0131 656 4268
Email: Elaine.Kwiatek@nes.scot.nhs.uk
Positive practice (England)
Strengthening capability, quality and care: empowering people with learning disabilities
The health and social care organisations in England are delivering a major programme to transform the care of people with learning disabilities. This includes a commitment to redesign care models and services which reduce the need for in-patient beds and support people in a place they call home. As part of this work, new staffing models will be developed and the role of the registered learning disability nurse will be vital to ensure safe, compassionate and competent care in whatever setting.
People with learning disabilities suffer a higher incidence of ill health than the general population. In the following case study a team approach succeeded in reducing the numbers of individuals reaching crisis point.
The challenge
There is a higher prevalence of ill health among people with learning disabilities partly because people with learning disabilities and their carers often do not recognise a deterioration in health until the situation has become serious. The intensive health outreach team in Cheltenham recognised that referrals often reached crisis level because of unmet basic health needs such as malnutrition and dehydration. The team also recognised that practitioners needed to have appropriate resource readily to hand in an accessible form to respond to referrals.
The journey
The team identified the need to link care planning with care pathways incorporating the Health Equalities Framework together with the resources related to the determinants of health inequality. Following a series of workshops, nutrition and hydration were identified as factors in the majority of the referrals. The team also recognised that information was not always stored in an organised way to enable practitioners to access it quickly and effectively.
Claire James, administration manager, created a flow chart for nurses and health care assistants which linked resources for care staff and service users. As the flow chart developed, additional resources were created for use by practitioners.
For example, carers often did not understand how to judge the amount of fluids an individual was having during the day. The team created a fluid chart in the form of an image of a jug which carers could mark to show daily intake as the jug 'filled up'. In addition a nutritionist worked with the team to identify foods that were nutritious and hydrating.
The flow charts, linked to the electronic pathway, enabled practitioners to locate relevant resources in a timely way when called out to referrals in residential settings, supported living environments and even over the weekend.
The outcomes
- Electronic care pathways support timely access to services i.e. right person, right place, right time as well as contributing to preventative and anticipated care.
- The care pathways improve safety and increase the productivity of the learning disability nurse through preparation and the ability to access the resources needed for reasonable adjustments and partnership care planning in a timely and responsive manner.
- They enable non-registered nurses to have access to reliable, evidence-based resources in the absence of senior staff thus enabling registered nurses to use their skills to the utmost while spreading their knowledge to all sectors.
- The resource includes easy-read and health information to aid proactive and preventative literature that increases health literacy and prevents unnecessary admissions and improves safety for service users and allows the nurses to respond in a timely fashion so aiding the productivity of the team as a whole.
- The journey to implement solutions has helped staff look at the relationship between health inequalities and the care provided and to recognise that basic healthcare and preventing ill health needed to be embedded in the social care environment before a crisis occurs.
- Staff are more productive in relation to releasing time to care, the independent care providers receive valuable resources to increase health literacy and are better able to offer preventative solutions themselves.
- Service users experience greater consistency of care and advice from learning disabilities and care providers. Students are able to follow the pathways which reinforced their knowledge of using validated procedures, and enable them to provide guidance in a structured systematic approach.
- Health literacy among people with learning disabilities and their carers improved alongside their ability to recognise a deterioration in health before a crisis occurs.
- The approach offers staff clarity and validity and allows them to work to minimise health inequality by using their unique skills while also transferring skills and information to other care sectors.
- The culture has moved from reactive and crisis-led to a more preventative strategy that is also responsive and measurable.
- The resources linked to the electronic pathway provide easy-read and template care plans and visual aids that can be saved and personalised for the individual. These bespoke examples of care planning empower the individual and carers thereby assisting and promoting a move from a culture of exclusion to one of inclusion.
Contacts
Intensive Health Outreach TeamRoom CR 027
Charlton Lane Centre,
Charlton Lane,
Cheltenham
Gloucestershire,
GL53 9DZ
Telephone: 01242 634 175
Email: Consultant nurse: Crispin.Hebron@glos.nhs.uk
Email: Administration manager: Claire.James@glos.nhs.uk
Email: Clinical nurse specialist: Marc.Pratt@glos.nhs.uk
Positive practice (Wales)
Strengthening capability in forensic care in the independent sector
Many learning disability nurses work in the independent sector. This case study is an example of partnership working between statutory services and an independent sector provider (Public Health Wales, 2013) who up until that time had had no previous experience of working with high-risk offenders. It demonstrates the added value brought to the service by a learning disability nurse.
The challenge
A small independent provider specialising in supporting individuals with learning disabilities and serious challenging behavior, including high risk offenders, values the skills of learning disability nurses in working with these individuals to deliver evidence based treatment programmes.
The journey
A detailed risk assessment using a forensic Structured Assessment of Violence Risk in Youth (SAVRY) risk assessment (Webster, Douglas et al, 1997) enables the multidisciplinary team to work with individuals with high risk behavior including sexual offences to reduce the possibility of a recurrence (Lindsay et al, 2004). A review of the relevant literature (Lindsay and Taylor, 2005) demonstrates the potential benefits of this approach for individuals and the protection of public safety.
The learning disability nurse, who is also the forensic lead, leads and develops the organisation to become knowledgeable and skilled in working with this cohort of complex individuals. Interventions involve a treatment-based approach using adapted material from validated and recognised pathways (Craig et al, 2010) and which may include weekly sessions at the person's place of residence in conjunction with the clinical psychologist from the local learning disability team. The Good Lives Model (Ward, 2011) is promoted to ensure a rich, fulfilling and meaningful lifestyle.
The results
Individuals have a safe therapeutic space for their treatment and are able to discuss their thoughts and beliefs and how they are affected by them. They are then able to understand how thoughts can become actions and actions are offences which have consequences. They also learn coping strategies and gain in confidence.
The benefits for staff are also considerable. The forensic lead ensures staff have clinical supervision and attitudes, confidence and competence have improved as staff now understand the context of how the offence cycles for these individuals have developed over time and how their learning disability impacts on the choices they have made. They now have a healthier, positive relationship with high risk individuals which has helped in the growth of self-esteem.
The organisation recognises the added value that having someone with a learning disability nursing background can bring to a service. They understand that working with people with complex presentations is more than just challenging behaviour and that people are people first and the behaviours they exhibit are in a context which needs to be understood.
Through demonstration, direct work and clinical supervision the organisation has been strengthened in its ability to work with offenders with a learning disability. The added value that having a person employed with a learning disability nursing background has helped to strengthen the service capacity issue and has increased the local options available to commissioners through evidence-based practice, in partnership with statutory services and the independent sector.
Contacts
Paul Baker
Forensic Lead,Procare Wales and Honorary Lecturer (University of Wales - Bangor)
54 -56 Kinmel Street,
Rhyl,
Denbighshire,
North Wales
LL18 1AW
Telephone:01745 369005
Email: PaulB@procarewales.co.uk
Focus on quality
Strengthening the Commitment highlighted that learning disability nurses need to embrace the movement towards quality improvement and demonstrate impact through measurable outcomes and evidence based interventions that improve safety, productivity and effectiveness alongside traditional person-centred approaches. The following case study demonstrates how learning disability nurses were empowered to modernise their practice and to improve the health experience of people with learning disabilities.
'Learning disability nurses help someone to have the best life they could have.'
Annie Norman, RCN
Positive practice (Scotland)
Strengthening our Practice
The challenge
Strengthening the Commitment set out a number of challenges for learning disability services in Scotland. The learning disabilities nursing team in NHS Lanarkshire has played an active part in taking forward the modernisation agenda set out in the report. The majority of the team are involved in one or more sub-group of the Local Implementation Group.
The journey
One working group carried out a scoping exercise to collect base-line information about the role of the learning disability nurse from people with learning disabilities, their carers, learning disability nurses, other healthcare professionals and other agencies. This information was the driver for the project 'Strengthening our Practice'. The overall aim of the project was to empower the learning disability nurses to modernise their practice and improve the healthcare experience of people with learning disabilities. The project supported the implementation of the Moulster and Griffiths learning disability nursing framework into practice.
The project links to three of the principles of Strengthening the Commitment.
- Capability will be strengthened by maximising the skills, knowledge and competencies of learning disability nurses within a range of settings, including community, in-patients and the independent sector. The framework highlights the values and rights based aspect of learning disability nursing.
- Quality is being addressed through the use of the Moulster and Griffiths model which includes an outcomes focused measurement framework to allow nurses to demonstrate the effectiveness of their nursing process. The project addressed future quality issues by involving student nurses and university lecturers.
- The learning disability nursing profession will be strengthened with a focus on incorporating research, reflection and evidence base into everyday practice.
The main challenge for this project was the struggle experienced by learning disability nurses with their desire to improve and modernise their practice while experiencing the pressures of increasing clinical demands. The joint support of senior nurses and managers was pivotal in addressing the challenges. It was important that the nurses understood and appreciated some of the gaps in their practice and were made aware of the policies and guidance that supported the proposed change.
Funding was sourced from NHS Education for Scotland (NES) to provide a development day for the learning disability nurses in NHS Lanarkshire and the independent sector. There was also representation from student nurses, higher education institutions and a user/carer group.
The day was facilitated by Gwen Moulster who provided an overview of the theory behind the Moulster and Griffiths model and provided practical exercises to complement the implementation. The development day was evaluated extremely positively and was the main driver behind the nurses' motivation to use the model.
The framework is being implemented using the small test of change model: Plan, Do, Study, Act (PDSA). A practice development nurse and two community senior charge nurses have formed an implementation support team. They have re-designed the framework paperwork to meet the requirements of NHS Lanarkshire, set up drop-in support sessions for learning disability nurses involved in the project, and arranged one to one visits to their bases for additional support.
The project is due for completion in May 2015, but initial results are very positive. The project is addressing Strengthening the Commitment priorities for the future by raising the profile of learning disability nurses within NHS Lanarkshire and other agencies and is also helping to build relationships with the independent sector through collaboration.
The results
Initial feedback from the learning disability nurses involved in the project is positive. There is already evidence of a culture change as the nurses are aiming to be more outcome focused in their approach and are more aware of the need to seek out the evidence behind their interventions. They feel more confident in having a unified approach across the service, however it will take some time for them to get used to what they perceive as an increase in paperwork. Improved electronic systems may help to address this in the future. The benefits of documenting reflection on a case-by-case basis was initially viewed with doubt, however nurses have been able to see the positive impact, both on care planning and also as a basis for clinical supervision. It can also be used as a means to evidence, revalidation requirements set out by the Nursing and Midwifery Council.
Feedback from carer groups has been positive and the project has been taken to service user groups for consultation. A collective advocacy group has agreed to offer ongoing support to the project.
Contacts
Norah Arnott
Practice Improvement and Development Nurse,NHS Lanarkshire,
Resource Centre,
48-54 Roberts Street,
Wishaw
ML2 7JF
Telephone: 01698 354029 or 07854 671 545
Email: norah.arnott@lanarkshire.scot.nhs.uk
Team members involved:
Johnann Wilson, Senior charge nurse
Fiona Gibney, Senior charge nurse
Focus on strengthening the profession
Effective, strong leadership was highlighted by Strengthening the Commitment as being essential to ensuring that networks for learning disability nurses across the UK provide a powerful platform from which to celebrate, promote and develop their unique contribution. The following case study highlights the leadership programme developed for learning disability nurses in Northern Ireland.
'My client trusts and relies on me … I'll do my best for him.'
Amy Hodkin, student
Positive practice (Northern Ireland)
Learning disability leadership programme
The challenge
Increasing demand for learning disability services, complexity of need and the recommendations of various regulatory and inquiry reports pointed to the need to build the relevant set of leadership and practice development knowledge and skills within the learning disability nursing workforce in Northern Ireland. This challenge was set within the context of Strengthening the Commitment. A bespoke regional leadership programme has been developed to equip the profession to meet these demands and to identify and support a cohort of confident, competent leaders to support the learning disability nursing profession, now and into the future. The need for this programme has been recognised and endorsed at ministerial and Chief Nursing Officer level.
The programme has been developed and delivered by the Royal College of Nursing (Northern Ireland).
The journey
The programme focuses on strengthening the profession and aims to help participants develop their leadership knowledge and skills necessary to ensure the delivery of safe and effective care in all learning disability settings. The content has been designed to deliver the learning outcomes concerned with the responsibilities of being a senior nurse working within learning disability services, with a particular focus on effective leadership behaviours, understanding whole systems working, managing the health versus social care conflict, positive performance management culture and the principles of working in and leading effective teams.
At its heart the programme seeks to build leadership capacity and capability to ensure visible leadership for the profession within Northern Ireland now and into the future.
In the context of Strengthening the Commitment this leadership programme has focused on helping participants develop competencies and skills in a number of key areas, including:
- leading for change
- practice development methodology
- problem based learning
- root cause analysis.
At a fundamental level the leadership programme will be an important mechanism to support succession planning and raise the profile of learning disability nurses and nursing in Northern Ireland.
In nurturing and developing new and aspiring leaders who are equipped (individually and collectively), Northern Ireland is aiming to transform the culture of service provision for individuals with a learning disability, to raise and improve nursing standards, to develop and role model strong clinical leadership and professionalism within the profession and ultimately to develop and ensure a better future of high quality nursing care for people with learning disabilities throughout their lifespan.
The results
The first cohort of learning disability nurses completed the programme in March 2015 and there will be follow up evaluation to establish the impact on practice and the development of leadership skills and behaviours. However, it is also the intention and responsibility of the Northern Ireland Regional Collaborative for the Northern Ireland Action Plan to ensure that we support and assist in the development of these individuals in a leadership context.
Contacts
Rita Devlin
Head of Professional Development DepartmentRoyal College of Nursing, Northern Ireland
17 Windsor Avenue
Belfast,
BT9 6EE
Telephone: 028 90384600
Email: Rita.Devlin@rcn.org.uk
Frances Cannon
Senior Professional Officer
Northern Ireland Practice and Education Council for Nursing and Midwifery (NIPEC)
79 Chichester Street
Belfast,
BT1 4JE
Telephone: 0300 300 006
Email: frances.cannon@nipec.hscni.net
Positive practice (Wales)
Raising the profile of learning disability nursing
One of the challenges facing learning disability nursing is the perception of the profession among other nurses, the public and prospective students. Too often we hear reports that learning disability nursing is viewed negatively or that parents of newly diagnosed babies or children with a learning disability do not realise that learning disability nurses are there to support them. The following case study illustrates an approach to introducing young people to learning disability nursing.
The challenge
Merthyr Tydfil is an area in South Wales where people with learning disabilities are mainly cared for by their own families in the family home. One of the day opportunities provided locally is in the college. The Independent Living Skills (ILS) department provides educational opportunities to a client group who have additional health needs alongside their learning disability, therefore recognising that health and social outcomes are interdependent. The lead nurse based in the local health team for adults with learning disabilities recognised that a working partnership was needed between the college and the health team.
The college also provides education to young adults who are embarking on their career paths; some are working towards qualifications to enter nursing. This was felt to be a good opportunity to raise the profile of learning disability nursing and a proposal was offered to the college to deliver a half-day session to a group of students studying on the health and social care module.
One of the challenges was to create a session that would be meaningful, memorable and delivered in a manner to create engagement. The other was to gain positive feedback from all students. While it was not expected that all students would leave the session wanting to become a learning disability nurse, the aim was to raise the profile of the profession and to enlighten potential student nurses.
The journey
The nurses led a session with a group of college students on International Disability Day, promoted by the United Nations. The aims of the session were to promote an understanding of disability issues and mobilise support for the dignity, rights and wellbeing of people with disabilities whilst celebrating the provision of Merthyr College.
The session was made up of:
- a presentation on disability awareness focusing on disability issues and attitudes
- a treasure hunt game to reinforce disability issues and celebrate the college provision. Students were invited to explore the college and locate particular reasonable adjustments that the college provides
- college students from the ILS department being invited to talk about their college course and their experiences in the college. The aim was to bring together the two departments as nursing students may be on a work placement in the ILS department and this would help build bridges
- a presentation on the role of the learning disability nurse describing examples of work, places to work and demonstrating that learning disability nursing is a promising career
- a question and answer session led by learning disability student nurses about their own experiences in university and what the course had to offer. A video created by the university has also been added to the presentation.
The results
Feedback has been positive and appears to have stimulated an interest among students for learning disability nursing and a greater understanding of the role played by learning disability nurses.
'I found this morning very interesting and the opportunity of this session has made my career path clearer. Thanks'
'I found the morning really interesting, it also made me think of different jobs I would possibly like to do.'
'Today's talk was very interesting and helpful, I would like to be a learning disability nurse, thank you very much.'
The session has been repeated to another group of students this year, and it is planned to continue to deliver the session on an annual basis. The aim is to continue raising the profile of learning disability and assist in strengthening the capacity of learning disability nurses.
Contacts
Elizabeth Fair
Lead NurseAMBU LHB
Merthyr Community Learning Disability Team
Keir Hardie Health Park
Aberdare Road
Merthyr Tydfil,
CF48 1BZ
Telephone: 01685 351277
Email: Elizabeth.fair@wales.nhs.uk
Persons involved in the project:
Elizabeth Fair - Lead nurse (project leader)
Rhiannon Smith - Community nurse
Rebecca Thomas - 3rd year student
Jessica Bamwell - 2nd year student
Contact
Email: Scott Taylor