Palliative and End-of-Life Care by Integration Authorities: advice note
An advice note to support the strategic commissioning of Palliative and End of Life Care by Integration Authorities.
Working Definitions of Palliative and End of Life Care and Bereavement.
Definitions for palliative and end of life care are the subject of on-going debate. However, for the purposes of this advice note, the World Health Organisation definition of palliative care [10] is used.
Palliative care is an approach that improves the quality of life of patients (adults and children) and their families who are facing problems associated with life-threatening illness. It prevents and relieves suffering through the early identification, correct assessment and treatment of pain and other problems, whether physical, psychosocial or spiritual.
Again, for the purposes of this note some further explanation may be helpful.
Non-specialist care and support are the types of care which most people will receive as their health and well being declines. Such care is provided to people living in the community, care homes and in hospitals, by professionals across health and social care, and may be an integral part of the fabric of the ‘compassionate communities’ in which people live. Such care, which although frequently not identified as palliative care, can and should be delivered alongside active treatment, where this is appropriate. Such care can be delivered with varying degrees of specialist palliative support throughout the health and social care system.
Specialist Palliative Care can help people with more complex palliative care needs. It is provided by specially trained multi-professional palliative care teams, who are generally based in a hospice, an NHS specialist palliative care unit, or an acute hospital. Specialist palliative care has a particular role in providing support, advice, and education to the rest of the health and care system, without which other forms of care and support would not be sustainable.
End of Life Care – or care of the person living through the dying phase of life - is that part of palliative care which should follow from the recognition that a person is entering the process of dying, and there is a high likelihood of them dying over the next few hours, days or weeks, whether or not he or she is already in receipt of palliative care. This phase could vary between weeks, days or hours, and with less predictability particularly in the context of COPD or other organ failure scenarios in such cases – illness can be unpredictable, and changes can occur suddenly and unexpectedly. It is helpful to address populations’ needs around end of life care, and not assume it is covered by dealing with palliative care.
Bereavement is understood as ‘the entire experience of family members and friends in the anticipation, death, and subsequent adjustment to living following the death of a loved one’ [11] , and bereavement care may be defined as any care provided formally or informally, through statutory or voluntary services or by members of the community to those affected. The needs for support will apply to those affected by both expected and unexpected loss and death.
Four Dimensions of Palliative Care
In assessing needs, and planning how the full breadth of those needs will best be met sustainably, the four dimensions of palliative care should always be considered. Attending to the spiritual, social and psycho-emotional in addition to the physical are not optional extras, and doing so may impact positively on the physical supports a person needs.
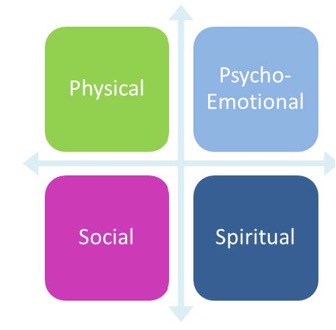
Palliative care involves all these dimensions. Meeting the vision set out in the Strategic Framework for Palliative and End of Life Care, that all who need it should have access to it by 2021 – is not a simple task. Partnerships should also regard palliative and end of life care as encompassing all illnesses, all times (i.e. from diagnosis to bereavement) and all settings. There are many elements of continuity with the services and supports required by people as they become frail or seek to live well with their long term conditions.