SMASAC Short Life Working Group on Lymphoedema - Lymphoedema Care in Scotland, Achieving Equity and Quality
A Scottish Medical and Scientific Advisory Committee Report. Providing information on the nature and extent of Lymphoedema. Making recommendations for Scottish Government Health and Social Care Directorate, Health Boards, NHS Education Scotland and Healthcare Improvement Scotland
Section 3: Providing a Multi-Agency Service
It is important that the multi-agency service has clearly identified core members with easy access to a much wider group of services that may be required. A named co-ordinator for each team should be identified.
3.1 Patient experience
Patients with lymphoedema experience significant physical and psychosocial burdens which are amenable to management interventions, with early interventions costing less than treatments for advanced lymphoedema. In addition to the provision of clinically effective interventions, reducing the adverse impact on the quality of life of a patient requires ongoing support in the community.
A recent poll of the top ten priorities of people with lymphoedema by Macmillan Lymphoedema Project Scotland (2013) found that patients and their carers place the highest value on:
- Getting the best treatment
- Receiving a prompt diagnosis
- Not having to wait long for my treatment to start
- Being able to access treatment quickly if my condition worsens
- Receiving prompt assessment and treatment if I have symptoms of cellulitis
- Being able to obtain replacement hosiery as required
- Accessing specialist lymphoedema care locally
- My GP knowing about my condition and treatment
- My lymphoedema care provider knowing enough about my condition and treatment and
- Being supported to self manage my lymphoedema.
3.2 Health and social care policy
In terms of health and social care policy in Scotland, the Healthcare Quality Strategy and the Route Map to the 2020 Vision for Health and Social Care state the Scottish Government is committed to "shift the balance of power to, and build upon the assets of, individuals and communities through a focus on achieving social change (more people able to care, volunteer etc.), support for the self management of long-term conditions and personal action (alcohol, exercise, diet and engagement) through working in partnership in Community Planning Partnerships (CPPs) and the new Integrated Health and Social Care Partnerships".
The aims deliver the principles observed by the Christie Commission that "effective services must be designed with and for people and communities" (Scottish Government, 2011). This is supported by the underlying principle of the Public Bodies (Joint Working) (Scotland) Bill 2013, that Health Boards and local authorities must take joint and equal responsibility for the delivery of nationally agreed outcomes for health and well being.
Evidence reviewed by the Health Foundation (2011) suggested that there are potential gains to be made from shifting some acute inpatient and day case services from hospital into the community. Those potential gains include better health outcomes for patients, greater patient satisfaction with services and more cost-effective delivery of treatment.
This shift from hospital to community supports the Long Term Conditions Collaborative Improving Care Pathways resource (Scottish Government, 2010), which promotes ten approaches by partnerships to deliver better outcomes and an enhanced experience of care for people living with long term conditions. Achieving better outcomes for people may involve shifting the location of care, sharing responsibility by empowering a different member of the multi-professional team, or shifting the focus of care through an anticipatory approach that prevents or delays dependency and need for more intensive support.
This approach also includes delivering care closer to home by providing as much care as possible in the community, including general practice and the wider primary care; making home care as safe, flexible, responsive and as enabling as possible; and developing the community hospital role which could be integrated or co-located with social care, housing support and third sector organisations.
3.3 Current service delivery
There is currently a wide variation in the organisation and delivery of lymphoedema services across Scotland. Some Health Boards provide a comprehensive service, whereas others offer services only for patients with cancer. Unfortunately, in some Health Boards there are no services available specifically for lymphoedema. In addition, the teams delivering lymphoedema care range from lone practitioners to small teams, with some or no administrative support, leading to variable waiting times and variable management options. It is also important to consider the location of these services as the location may not be acceptable to patients despite excellent service quality. For example, services located in hospices may not be acceptable to people who do not need palliative care.
The two main components of a comprehensive NHS Scotland service for people with lymphoedema should include:
1. Clinical intervention to manage the condition in addition to raising awareness among health and social care workers, patients, carers and the public. The aim is to improve the quality of life and enable individuals with the condition to function as independently as possible. This requires an integrated multidisciplinary and multiagency team, including the voluntary sector, to address not just the clinical aspects of the condition, but also:
- health improvement, lifestyle and health promoting advice (such as smoking cessation, increasing physical activity, balanced diet and moderate intake of alcohol)
- prevention of ill health (such as prevention and early robust management of cellulitis or other associated conditions such as cardiovascular disease)
- psychological, emotional, psychosocial, educational, and spiritual care support.
This type of service needs to be equitable as well as of a high quality, accessible locally as much as possible, and culturally sensitive.
2. Adopting the model of long term conditions management and supported self management, which is ideally suited for this condition, where the care is delivered mainly in the community and primary care with access to various specialist services and care as appropriate. Mindful of mobility and access challenges for people with these conditions, some of these services could be shared-care with regionally based services such as for complex oedema (Tier 3 - see below and in Figure 2) or nationally for complex resistant lymphoedema; congenital/genetic lymphoedema, complex syndromes or lymphoedema in children; or those who require assessment for a surgical intervention. Shared care could include telehealth and telecare interventions as well as face-to-face interventions. A referral and management pathway for children's services described in Appendix 4.
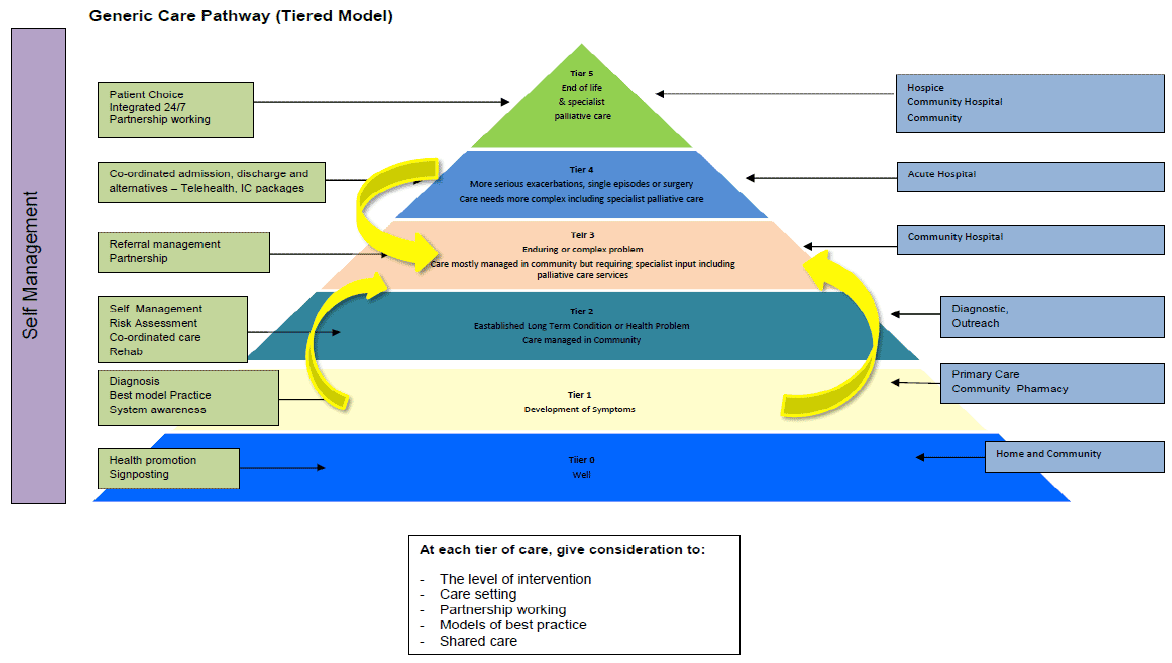
Needs can be usefully assessed according to tiers of care as outlined on page 20. This tiered approach has been adapted from the NHS Forth Valley Generic Care Pathway for long term conditions, which has been designed to promote an integrated and system-wide approach. At each tier of care, give consideration to:
- Where people receive information, including condition-specific information, information about services, and correspondence regarding appointments
- The level of intervention
- Care setting
- Partnership working
- Models of best practice
- Shared care.
Application to Lymphoedema Services
Stages of care
In long term conditions it is good practice to consider patients' needs along various stages of the pathway of care. For lymphoedema, these stages may be described as:
Tier 0: For people who are well
This level describes services provided at home and in community setting with and for people who are well. Services aim to inform and educate the general public about lifestyle choices and self management, raising awareness of how to identify early signs of lymphoedema and how to access services if needed. They may include targeted health improvement for those with higher risk of lymphoedema (e.g. cancer patients receiving surgical or radiotherapy interventions) as well as general health and wellbeing awareness.
Tier 1: Development of symptoms
This identifies those first level services provided to help people, who have developed symptoms, to manage their lymphoedema and maintain their health and wellbeing. The purpose is to enable speedy access to primary care services, facilitation of early diagnosis and staging of the condition where appropriate. Maximising quality of life and independence at home may require additional information and support to manage their condition from family, community and voluntary sector partners.
Tier 2: Established lymphoedema with needs met fully in the community
In this situation, services address the requirements of those individuals where the aim is to support people to manage their lymphoedema and maintain their health and wellbeing through primary care services, delivered with community and voluntary sector partners. Maximising quality of life and independence at home may require additional support from outreach rehabilitation, diagnostic, social care and housing services.
Tier 3: Lymphoedema mainly managed in the community but require specialist input
At this stage services are provided for people who are already supported by the primary care team, but who need additional intermittent and usually intensive support delivered by specialist lymphoedema practitioners. It is important to have effective coordination across multi-disciplinary and multiagency teams. It may useful to consider Anticipatory Care Planning at this stage, and explore carer support needs.
Tier 4: Frequent exacerbations and people with most complex care needs
These services apply to people with serious lymphoedema, with complex needs which may include other underlying long term conditions or difficulties. Services need to be well coordinated with timely access to a range of professionals, across care settings and agencies. As well as increased involvement of specialists based in hospitals or hospices there is a need to deliver effective packages of care and equipment that proactively and continually support people. This requires an integrated approach to care planning (including the appropriate use of telehealthcare), workforce development, and effective information sharing. For people who require inpatient hospital care, such as surgery, referral and admission criteria, should be agreed and known to practitioners. It is essential to have a well co-ordinated discharge plan prior to discharge of the individual into the community.
Tier 5: End of Life Care
Here the services need to address the complex need of patients with advanced disease with palliative care requirements, and the needs of their informal carers. A variety of supportive measures and treatments from specialists, generalists and the voluntary sector may be helpful. The care, which is more appropriately delivered in community or hospice settings in the majority of cases, should be informed by the wishes of the individual and those close to them.
See Figure 2.
Recommendations
| 6 |
Health Boards should support and develop a community-based integrated model of tiered care for people with lymphoedema, including complications such as cellulitis applying the principles of integration. |
| 7 |
Health Board Leads together with regional planning groups should develop a national referral pathway for people with lymphoedema who require assessment for surgery for lymphoedema. |
Figure 2. Tiers of Care. Adapted from NHS Forth Valley LTC Collaborative.
Contact
Email: Diane Dempster