Shortage occupations list 2018: call for evidence - our response for health and social care
Response to the UK Migration Advisory Committee call for evidence on the shortage occupation list summarises skills shortages within health and social care sector in Scotland, and details the contribution of international workers.
The Principal Reasons for Acute Shortages
35. The principal job shortages across health and social care in Scotland reflect observable trends both UK wide and internationally, particularly in relation to medical specialists, nursing staff and general practitioners. Nevertheless, these observable market trends are also exacerbated by issues of population demography and the remote and rural context, which is a defining feature of the environment in which we deliver health and social care services.
36. NHS Scotland and social care services are challenged with growing demand resulting from an ageing population, alongside other population health challenges, including an increase in the numbers of young adults living with disabilities. Demographic changes are anticipated to generate a 1% year-on-year, aggregate increase in demand for healthcare. Non-demographic growth, generated by increased public expectations, advances in new technology and service development, have been factored in to Scottish Government projections at 2-2.5% growth year on year. Pressures in the social care sector are likely to be slightly higher for a variety of reasons, including a focus on the very elderly, where demographic pressures are at their greatest. These factors continue to place pressure on training and recruitment, which we are actively addressing through workforce planning, to help ensure that our integrated health and care services have access to a workforce of sufficient size and skill.
Nursing and Midwifery
37. Statistics published by NHS ISD on 04 December 2018, indicate that at 30 September 2018, 3022.2 WTE vacancies existed within the Nursing and Midwifery workforce in NHS Scotland, equating to a vacancy rate of 4.8%. There are over 3,300 WTE more Nursing and Midwifery staff working in NHS Scotland than 5 years ago, with 5 years of consecutive growth. The number of community Nursing and Midwifery staff has increased by 473.1 WTE (4.1%) in the past year alone. Approximately 6,700 nurses work in the social services sector, the vast majority in care home for adult services.
38. An ageing population with a significant proportion of the workforce approaching retirement, will inevitably increase turnover, and is expected to exacerbate existing vacancy issues. This issue is particularly prescient, and most prominent within the Nursing and Midwifery Job Family, as demonstrated in Figure 1, where 19.2 % of the workforce is expected to retire in the next 10 years.
Figure. 1: Demographic composition of NHS Scotland workforce by job family, December 2018[16]
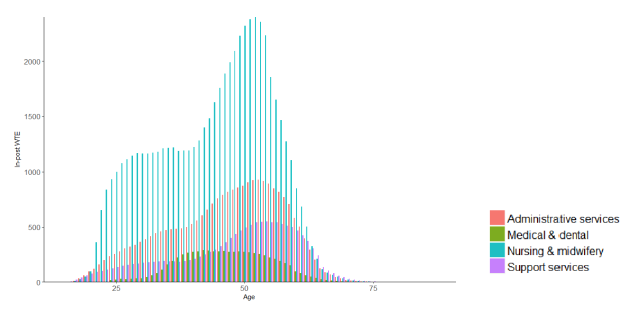
39. Demographic challenges within Nursing and Midwifery are exacerbated by acute supply issues also. Notwithstanding their current exclusion from the cap, nursing staff may not meet with existing Tier 2 minimum salary thresholds, meaning that future changes to immigration rules could stifle supply. This coupled with projected reductions in the movement of staff from within the European Economic Area poses an acute threat. Data from the Nursing and Midwifery Council shows a rapid decline in the numbers of Nurses/Midwives joining the register for the first time following EU withdrawal (9,038 between Oct-14 – Sept-15; 888 between Oct-17 - Sept-18), alongside a notable increase in departures from the register, (1,743 between Oct-14 to Sept-15), as demonstrated in (Figure 2)[17].
Figure 2. Nurses and Midwives Joining and Leaving the NMC Register[18]
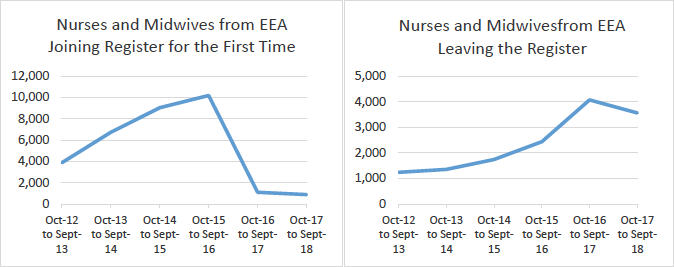
Social Care Services
40. Statistics published by the Care Inspectorate and Scottish Social Services Council (SSSC) in January 2019, taken from 89% of services in Scotland, show that vacancy levels across social services are significant and increasing. 38% of services reported vacancies at the end of 2017, an increase of 2% points on the previous year[19]. This compares to the 20% of all establishments reporting vacancies in Scotland. The rate of whole time equivalent vacancies for all social care services in Scotland is also increasing, up to 5.9% at end 2017 from 5.5% one year earlier. This is higher than the overall vacancy rate for all establishments in Scotland of 3.1%. Problems filling vacancies were reported by 45% of services at end 2017, up from 44% a year earlier. The main reasons reported for problems filling vacancies include :
- Too few applicants with experience (58%)
- Too few applicants (57%)
- Too few qualified applicants (50%)
41. The social care sector benefits extensively from staff from across the EU. Robust estimates of the contribution of EU-nationals to the social services workforce indicate that 5.5% of adult social care staff in Scotland are from other EU countries[20]. However much higher figures are found for specific services and service providers, with stakeholders reporting figures of 11-35% in some services at a recent roundtable discussion with Scottish Ministers.
42. The age profile of the workforce shown in Figure 3 indicates that a significant proportion of the workforce is approaching retirement, which will exacerbate vacancy issues.
Figure 3: Age profile of care service workforce December 2017[21]
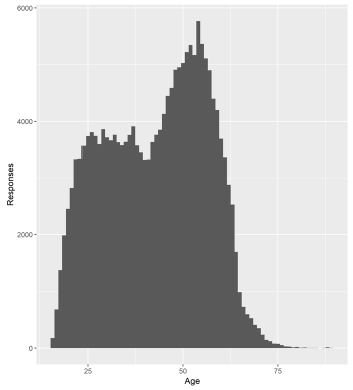
43. Social Workers: The whole time equivalent vacancy rate for social workers in local authorities in Scotland was estimated by the SSSC as 5.7% in December 2017, with highest rates seen for those working with adults (7.6%) and in criminal justice (6.2%). Current shortages may in part be due to an increase in the proportion of social workers approaching retirement. There have also been lower numbers of qualifications and admissions to training programmes in recent years, possibly linked to a reduction in the numbers of qualifying undergraduate programmes.
44. Nurses in social care: 6,700 nurses, equivalent to 10% of NMC-registered nurses in Scotland, work in social care, the majority in care homes for adults. The majority are employed in the independent sector and an increasing proportion (30%) are employed by nursing agencies. The percentages of non-UK EU nationals among NMC-registered nurses in the sector is 7.3%, while the percentage of non-UK EU nationals in nursing agencies is 16.5%. The nurse vacancy rate for care homes for adults was estimated by the SSSC at 14% in December 2017, while Scottish Care (the representative body for independent sector care providers in Scotland) estimated nursing vacancies among their members at 20%, with over 90% struggling to recruit nurses (2017 survey data). The main reason reported was the better terms and conditions available in the NHS. Overall nurse numbers and the ability to recruit from outwith the UK are therefore particularly critical for the social care sector.
45. Care homes for adults care/support workers: Care Inspectorate and SSSC reported data showed that 57% of care homes for adults reported vacancies at the end of 2017, with the same percentage reporting that they found vacancies hard to fill. The most common reasons reported were too few applicants (55%), too few applicants with experience (55%) and competition from other service providers (38%). The rate of WTE vacancies was 5.2%, up from 4.7% the previous year[22]. There are significant numbers of non-UK EU nationals (total number estimated of 3,150), making up 5.9% of staff in care homes for adults. This picture is supported by 2018 data from Scottish Care, covering around 10% of care home staff in Scotland. This showed that 61% of their care home provider members had care worker vacancies, with increasing numbers turning to agencies. 8.1% of staff were from outwith the UK, including 5% from the EU. 42% of services recruited from the EU for care roles.
46. Lack of ability to recruit non-UK nationals poses considerable risks to service provision, with some individual services highly dependent on non-UK EU staff. All care home for adult care workers must register with the SSSC and need to gain the qualification required for their role (at least RQF 3). However, participants in a recent Ministerial roundtable with the sector indicated that with the exception of nurses, salaries would not meet a £30,000 threshold, with average salaries of the order of £18,000. Many service providers are small and a more complex process for recruitment outwith the UK is likely to prove challenging.
47. Care at Home and Housing Support care/support workers: Care Inspectorate and SSSC reported data showed that 60% of care at home/housing support services reported vacancies at the end of 2017, with 57% reporting that they find vacancies hard to fill. The most common reasons reported were too few applicants (71%), too few applicants with experience (56%) and candidates unable to work the hours needed (56%). The rate of WTE vacancies was 7.4%, up from 7.1% the previous year[23]. The number of non-UK EU nationals working in care at home/housing support services was estimated at 2,850 (4.1%) in early 2018[24].
48. The challenges arising to this sector from a reduction in ability to recruit from outwith the UK are similar to those outlined above for care homes for adults, with average salaries of the order of £18,000 according to stakeholder estimates. From 2020 all care workers in these services will be required to register with the SSSC and gain the qualification required for their role (at least RQF 3).
Doctors: Consultants
49. The consultant workforce in NHS Scotland is also vulnerable to changes in migration strategy. Much of the medical workforce originates from outside of the UK: 16.6% of all doctors currently practising in Scotland have a primary medical qualification from outwith the UK (3,781/22,740) with 5.7% from the EEA (1,303/22,740)[25]. Figure 4 uses GMC data to give an indication of the exposure of the consultant workforce to both EEA and International staff.
50. Most notably: Vascular Surgery, Orthopaedics and Diagnostic Radiology all rely on intra-European migration, with a significant proportion of the existing workforce having a primary medical qualification from within the EEA[26]. Indications are that the United Kingdom has reduced appeal as a destination for EU migrants, as the UK is perceived as an increasingly hostile destination for immigrants. A British Medical Association (BMA) survey in November 2017 reported that almost a fifth of EU-27 doctors working in the UK have made plans to leave since the referendum vote[27].
51. The international recruitment market for consultants is porous, and an insufficiently flexible approach to the migration of medical professionals going forward would compromise service delivery within NHS Scotland. Given the lengthy training pathways, demand for consultants cannot be met exclusively through the creation of new domestic training places, particularly in the short to medium terms. Given the mobility of fully trained consultants, guarantees cannot be made that trainees will remain in Scotland. The existing Tier 2 system presents logistical and administrative barriers that interfere with the recruitment of consultants to NHS Scotland. It is essential that these are minimised to ensure that we are not competitively disadvantaged.
52. Health Boards surveyed have indicated that in the short-term the most acute problems with recruitment exist in Psychiatry, Radiology, General Surgery, Geriatric Medicine, Histopathology and Gastroenterology. A more detailed discussion of the shortages experienced amongst the medical workforce, alongside current salary information, can be found within the submission from NHS Education Scotland, the sponsor in Scotland for all doctors in training, and in the returns from NHS Lothian and NHS Greater Glasgow and Clyde, which are appended at Annex A.
Figure 4. Origin of Consultants in Scotland on the Specialist Register:
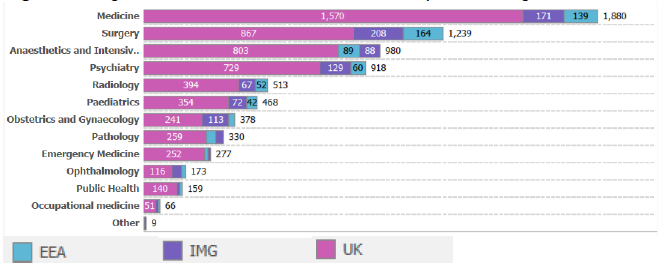
General Practice
53. Recent evidence demonstrates that there is a declining number of registered GPs in practice in Scotland. This comes at a time where the demand on primary care services is steadily increasing due to a combination of an ageing population and rising levels of multi-morbidity. The number of people aged 65 and over is estimated to increase by around 60% from 0.93 million to 1.48 million by 2039, leading to substantial rises in a range of long-term conditions[28]. People with long-term conditions already account for about 50% of GP appointments, placing significant and increasing strain on services. Patients are also demanding more from their healthcare professionals: they rightly expect higher standards of care, more information about their treatment, more involvement in decisions about their care and improved access to the latest treatments.
54. While the headcount number of qualified GPs working in NHS Scotland has increased by around 200 since 2005 to around 4,400, there has been a steady fall in the estimated whole time equivalent[29] since 2013 (Figure 5).
Figure 5: GP headcount and whole time equivalent, 2005-2017[30]
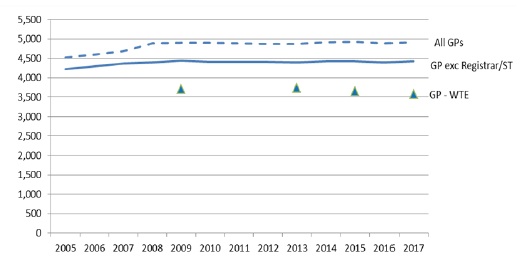
55. The combination of falling capacity and steadily rising demand from an increasing ageing population is placing general practice under significant and unprecedented pressure. This is apparent from the latest Primary Care Workforce Survey[31], which found that:
- Nearly a quarter (24%) of responding GP practices reported current GP vacancies, compared to 22% in 2015, and 9% in 2013.
- The GP vacancy rate has increased from 1.7% of total sessions in 2013 to 5.6% in 2017.
- The estimated WTE of GPs has decreased by over 4% since 2013.
- Nearly 9 out of 10 practices reported using GP locums in the 12 months preceding the 2017 surveys.
- There has been a continued decrease in the proportion of GPs working eight or more sessions per week: from 51% of GPs in 2013 to 37% in 2017.
- Over a third (36%) of all GPs are aged 50 years or over, with a significant risk these doctors will leave the profession as demand continues to outpace workforce supply.
56. As set out in the Health and Social Care Delivery Plan[32], the Scottish Government's vision for the future of primary care is for enhanced and expanded multi-disciplinary community care teams, made up of a variety of professionals each contributing their unique skills to managing care and improving outcomes. This is accompanied by a clearer whole system quality improvement and clinical leadership for General Practitioners (GPs) via the new General Medical Services (GMS) Contract. Strong primary care services focused on prevention, anticipatory care planning and self-management are fundamental to ensuring the sustainability of the NHS.
57. The recent Nuffield report Shifting the balance of care: Great expectations[33] highlighted the implementation challenges involved in shifting care out of hospital settings to deliver the triple aim of improved population health, better patient care, while reducing costs. It stressed the need to properly resource primary and community care in taking on additional responsibilities as transition is further embedded.
Allied Health Professionals
58. The AHP workforce has increased by over 30% in the last 10 years - from 8,800 in 2006 to around 11,500 in 2017[34]. This reflects a growing need for professionals with a diverse range of specialist skills who can make a vital contribution as first point of contact practitioners for diagnostics, early rehabilitation and enablement. Amongst Allied health professionals, shortages persist within Radiography & Sonography, Prosthetics and Orthotics, and amongst Paramedics, all of whom are present on the current SOL. Other notable shortages have been highlighted within physiotherapy, and occupational therapy.
59. Within physiotherapy, NHS Scotland currently has some 205.6 vacancies, equating to a vacancy rate of 6.7%[35]. These issues are expanded upon within the NHS Lothian return, which has been appended. Additional profiles have been provided within Annex C for several key roles, experiencing acute vacancy (Cardiac Physiology/ Prosthetics and Orthotics/ Physiotherapy).
60. For a significant proportion of Allied Health Professionals international recruitment is contingent on the presence of their occupation on the Shortage Occupations List, in order to meet the Tier 2 salary threshold. Table 1 indicates the proportion of AHPs affected by the £30,000 threshold, as well as the £35,000 settlement threshold, using 2019-20 pay scales.
Healthcare Science Professions
61. Healthcare Scientists are the fourth largest clinical group, and their work underpins over 80% of all clinical diagnoses. Further technological advances will bring many more opportunities for Healthcare Scientists to work across disciplines and NHS Board boundaries. The NHS Scotland workforce covers over 50 different scientific specialities in the three main strands of healthcare science – life sciences, physical sciences and physiological sciences.
62. Demand profiles for cardiac physiology suggests that demand for additional cardiac physiologists could range between 35 and 156 WTE within 10 years, on top of the current shortage of 16 WTE. Additionally, the Academy of Healthcare Science were able to highlight that in Vascular Science 20% of the labs (4 out of 20) say they have unfilled vacancies, but we were unable to collect further evidence within the short time-frames. Other notable shortages have been highlighted within Clinical Physiology; most acutely in Cardiac Physiology and Vascular Science. These issues are expanded upon within the NHS Lothian return, which has been appended. Additional profiles have been provided within Annex C for several key roles, experiencing acute vacancy.
63. The educational pathways for Healthcare Scientists vary in length and complexity, spanning a wide range of professions, with slight deviations in titles representing distinct and strategically significant roles. These job titles have often confounded classification and caused problems with Tier 2 visas particularly within various strands of Physical Sciences including: Medical Physics and Nuclear Medicine, as indicated within the appended return from NHS Lothian. There is currently no process whereby employers are able to appeal decisions, when disagreements with the Home Office occur, and in some cases this has caused considerable uncertainty for applicants.
64. Within Healthcare Science: Vascular scientists; Medical Illustrators; and the Maxillo-facial workforce are reliant on graduates from courses in England, and therefore have limited success in attracting individuals to work in Scotland.
Contact
Email: Niall.Anderson@gov.scot