See Hear
A strategic framework for meeting the needs of people with a sensory impairment in Scotland
7. The development of care pathways
7.1. Another way of identifying the response that should be made to sensory loss is to consider an individual's journey or pathway through care and their requirement for appropriate and timely interventions from statutory agencies and service providers.
7.2. Care pathways are increasingly seen as a means of ensuring that local partnerships and services have clearly identified and agreed ways of placing the person at the centre, and assisting the individual to move through and across services for particular conditions. Not only does this provide a more integrated and positive experience for the individual, but it is also a way of optimising resources and systems for agencies to provide the most efficient service patterns and respond to changing needs. They provide a structure to guide interventions and to prompt actions and communication between and within agencies and services.
7.3. Every person's needs are different and there can be no typical journey, but the diagram below has been designed to show the main component parts of most people's journey in relation to sensory impairment. Again people may enter at different stages, particularly in relation to the nature/timing of the onset of a sensory impairment.
7.4. Many people can be dealt with through effective mainstream service provision. If these services are accessible and service staff have an awareness of the needs of people with sensory loss and appropriate skills/training to deal with these needs, then a wide range of these staff should be able to not only identify needs relating to sensory impairment, but also assess and provide simple solutions. It also recognises, however, that there will be some people whose sensory loss or complexity of need is such that specialist provision will always be required.
7.5. Parents, carers and other family members can often be the first to recognise a sensory loss in a family member. As such they are a valuable source of knowledge and expertise. Recognising the challenges of sensory loss, parents/carers can also be assisted to support people with a sensory loss if they are aware of the implications of that loss and, where appropriate, are provided with information that can assist them in their role. In many instances the person themselves will be able to relay this information, but in other instances it would be helpful if this could be done either directly with the parent/carer, or with both the person themselves and their parent/carer.
7.6. Meeting the communication needs of people with a sensory impairment is fundamental to ensuring that they can engage with the care pathway, and is an essential element in their everyday lives.
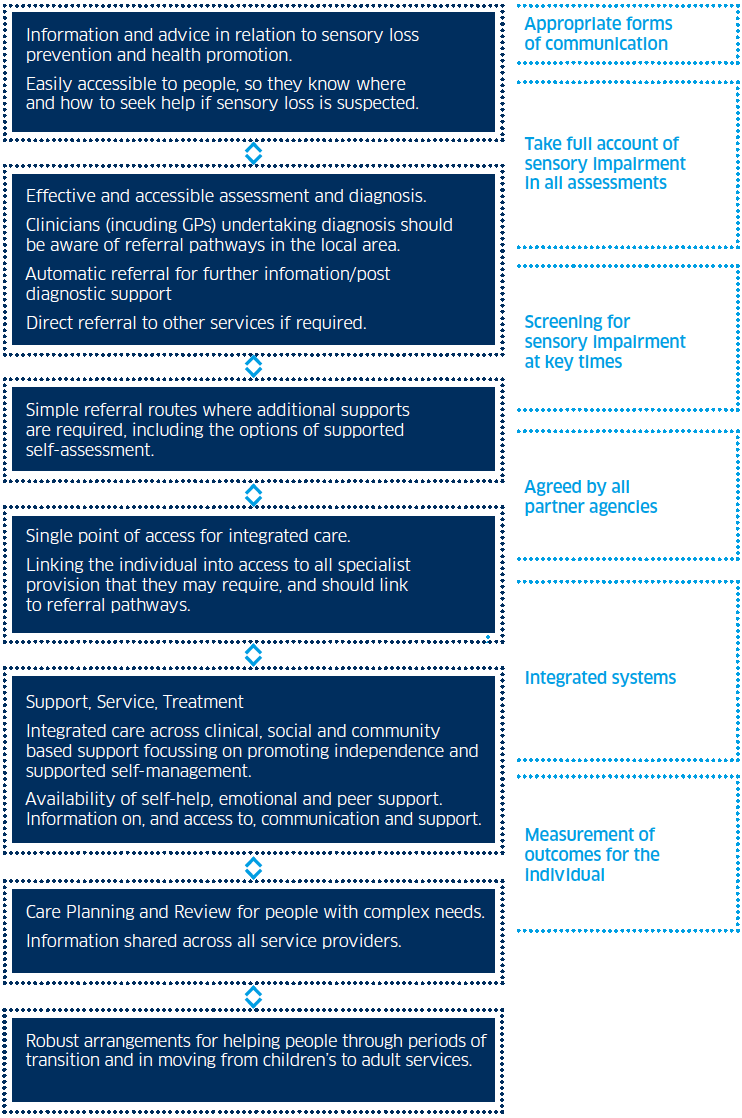
Key factors in care pathways
7.7. To ensure that pathways work as effectively as possible for people with a sensory impairment, they must be confirmed at a local level to take account of local circumstances, demographic and ethnic profiles and a number of key factors must be considered:
- For the majority of people, the point of diagnosis will be undertaken primarily through NHS audiologists, ophthalmologists, optometrists or optometry practitioners. Others will first become engaged through their paediatric services or GP. It is important that referral routes into support services are clear to those undertaking diagnoses, and that information is available in appropriate formats to the individuals themselves and their parents/carers;
- It remains a cause for some concern that there is no standard requirement in relation to maintaining information on people with the various diagnoses of sensory impairment. Such information is basic to understanding the prevalence of impairment and then being able to monitor the reach of services, engage with service users and carers, identify and learn from best practice, and identify gaps and opportunities for service improvement;
- A commitment to the consideration of sensory impairment being included in a range of health and social care assessments;
- The development of integrated service provision that actively promotes opportunities for assessment and service delivery across the different types of sensory loss and also the agencies involved;
- Agencies and disciplines should have robust, coordinated arrangements for information sharing and a commitment to local care pathways to best meet the needs of local service users;
- Agencies and disciplines should be aware of the opportunities offered by their distinct legal and practice frameworks, and to take advantage of any such opportunities to provide person centred solutions for individuals;
- A commitment to maximise basic sensory impairment checks which can readily be undertaken by non specialist staff, with onward referral where there is an indication of sensory loss. This could be done at GP surgeries when the person
reaches an agreed age, or at key times of engagement, e.g. assessment for other community care services or admission to a care home; - A commitment to a single point of access wherever possible, including for ongoing contact. This places a responsibility on services and agencies to work together effectively and reduce duplication and confusion for the individual. For children this will be addressed by the Named Person role, a core component of the Getting It Right For Every Child approach. The Children and Young People (Scotland) Bill proposes to make the availability of a Named Person for every child in Scotland a statutory provision;
- A clearly developed set of local sensory impairment care pathways that are agreed by key stakeholders and understood by all clinicians, assessors, service providers and, most importantly, the person themselves. This should address the needs of people with an identified sensory impairment, people at risk of sensory loss, and people who may be living with a hidden sensory loss, and should reflect the importance of prompting the outcomes based approach outlined earlier;
- A commitment from statutory agencies to seek to agree the maximum possible consistency of approach across Scotland, and ensure similar access to services across Scotland;
- A commitment to awareness raising training for front line staff who may have to deal with people with sensory impairments;
- An awareness of existing mechanisms which may facilitate the achievement of the above, for example, the Managed Clinical Network (MCN), Visual Impairment Network for Children and Young People (VINCYP), which aims to improve services to children and families by providing evidence-based guidance, information and pathways for children identified as having a visual impairment.
Contact
Email: Alan Nicholson