Scottish Out-of-Hospital Cardiac Arrest data linkage project: 2018-2019 results
Report presenting the latest results of the Scottish out-of-hospital cardiac arrest data linkage project.
Initial rhythm, Bystander CPR and Survival
BOX 2
Initial heart rhythm
The initial heart rhythm recorded on the Electrocardiogram (ECG) on arrival of SAS is important. A patient may have a shockable rhythm (ventricular fibrillation or ventricular tachycardia) treatable by delivering an electric shock using a defibrillator, or non-shockable rhythm (asystole or pulseless ventricular activity and bradycardia). The initial treatment and prognosis depends on presenting heart rhythm, with better survival after OHCA with shockable rhythm.Initial rhythm, Bystander CPR and Survival
In 2018/19, initial heart rhythm data was available for 94.9% of worked OHCA included in the linked dataset. A shockable initial rhythm was recorded in 29.7% of worked OHCA cases. Figure 2 shows how this compares with previous years.
Figure 2: Percentage of worked OHCA cases with shockable initial ECG rhythm
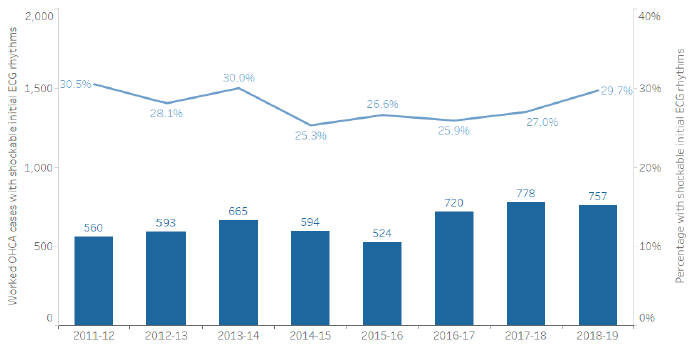
Figure 2: Shows the number of worked OHCA cases with a shockable initial rhythm (ventricular fibrillation or pulseless ventricular tachycardia) recorded on arrival of the Scottish Ambulance Service (blue bars) and the percentage of OHCA cases with shockable initial ECG rhythm (blue line), 2011/12 to 2018/19.
Bystander CPR
Whether or not a member of the public performs chest compressions (CPR) on a patient while awaiting the arrival of the ambulance service is the most important modifiable factor determining survival after OHCA. Promoting bystander CPR is a key element of Scotland’s Strategy for OHCA1. The percentage of OHCA with bystander CPR is therefore a very important metric for tracking progress. In 2018/19 bystander CPR was recorded as taking place on arrival of SAS personnel in 64.0% of cases. Figure 3 below shows the steadily increasing rate of bystander CPR since 2011/12.
Figure 3: Percentage of worked OHCA cases where bystander CPR was performed
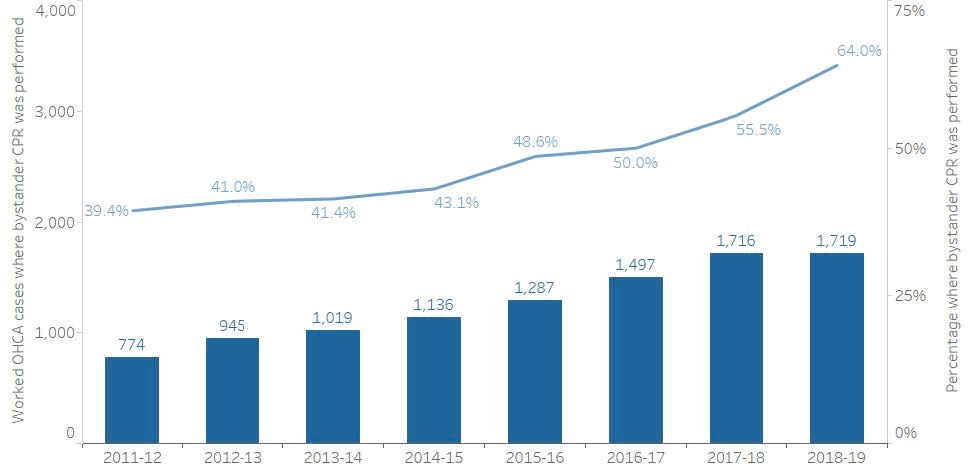
Figure 3: Shows the number of worked OHCA cases where bystander CPR was performed prior to the arrival of the Scottish Ambulance Service (blue bars) and the percentage where bystander CPR was performed (blue line), 2011/12 to 2018/19.
Save a Life for Scotland
A key driver of the increase in bystander CPR is the activity of the Save a Life for Scotland (SALFS). The SALFS partnership is composed of emergency services, third sector organisations, community responder groups, Scottish Government and academic partners.
Increasing the incidence of bystander CPR is the cornerstone of improving outcomes as prompt bystander CPR can increase the likelihood of survival after OHCA by as much as three times. As part of Scotland’s 2015 OHCA strategy, the SALFS partnership aimed to tackle Scotland’s low bystander CPR rate by equipping the Scottish public with CPR skills. CPR familiarisation has been rolled out across schools, communities and workplaces by the partner organisations, who have successfully reached the Strategy aim of familiarising 500,000 people with CPR skills - a year earlier than planned. Figure 4 demonstrates the increasing number of people equipped with CPR skills by the SALFS partnership since 2015. (Further information on the SALFS partnership and how to get ‘CPR ready’ can be found at www.savealife.scot).
Figure 4: Number of people receiving face-to-face CPR familiarisation from Save a Life for Scotland
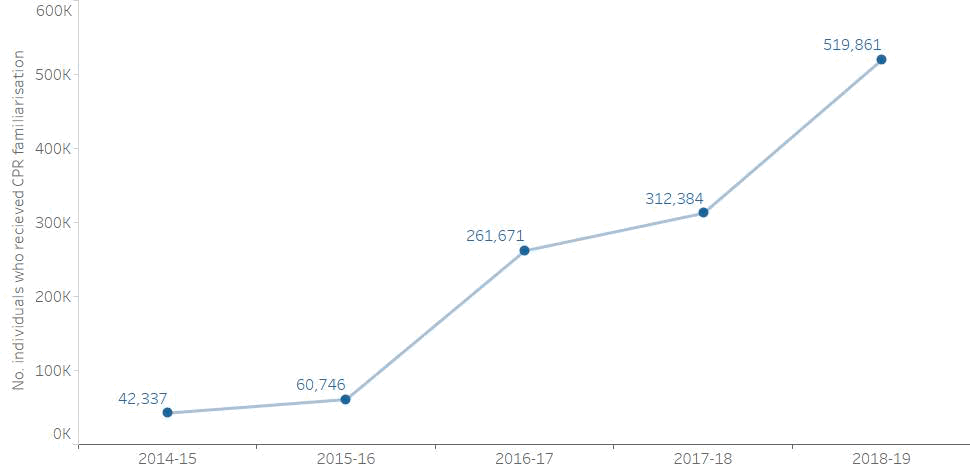
Figure 4: Shows the number of people receiving face-to-face CPR familiarisation from the Save a Life for Scotland partners since its inception in October 2015
Public Access Defibrillators
The use of public access defibrillators (PAD) by members of the public prior to the arrival of the ambulance service can reduce the time to delivery of a defibrillator shock and increase chance survival4. Although PADs are very effective when deployed in a timely fashion, international experience is that most OHCA patients do not have PAD applied. Bystander defibrillator usage as low as 1.74% have been observed in the literature5. The updating of the Scottish Ambulance Service electronic patient record in 2017 allowed improved capture of data reflecting PAD use by the public. Figure 5 shows the number of recorded uses of PAD at worked arrests during 2018/19 with a trend towards increased PAD deployment over time.
Figure 5: Percentage of worked OHCA cases where a Public Access Defibrillator was used
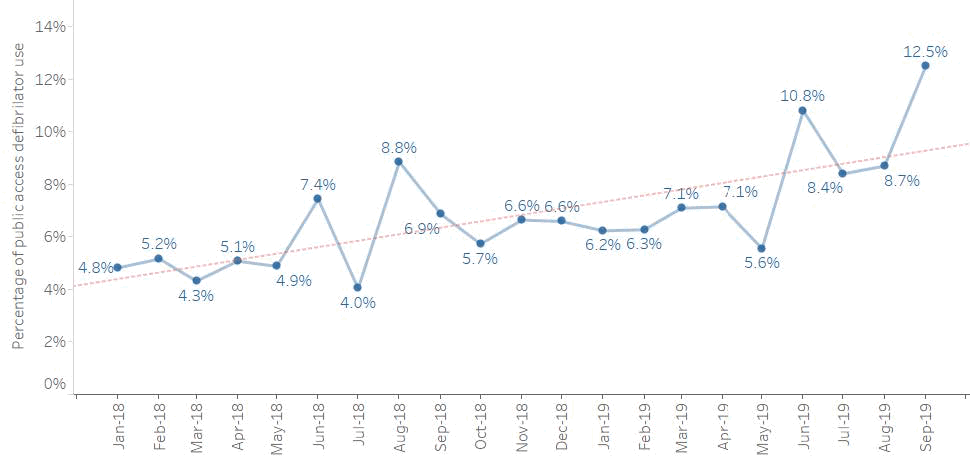
Figure 5: Shows the percentage of OHCA worked arrests where SAS recorded that a Public Access Defibrillator had been used, January 2018 to September 2019.
ROSC and Survival
The key clinical outcome after OHCA is long term patient survival. An important precursor to this is Return of Spontaneous Circulation (ROSC).
BOX 3
Return of Spontaneous Circulation (ROSC)
Definitions for ROSC vary. The Scottish Ambulance Service record ROSC if a patient regains a palpable pulse which is sustained until arrival at the Emergency Department. This is sometimes referred to as ‘survival to hospital’ or ‘number of hearts restarted’. ROSC does not equate to survival.
BOX 4
Survival
The definition of ‘survival’ used in this report is survival to 30 days after the date of the OHCA. We have counted survival as the percentage of worked arrests where patients were still alive at 30 days. Worked arrests which were not linked to outcome data have been assumed to be deaths and included in the denominator when calculating survival rates. A more detailed discussion of the methodology we have used can be found here2 6.
In 2018/19 ROSC occurred in 30.3% of worked OHCA cases, with 10.2% of these patients surviving to 30 days. This is shown in Figure 6.
Figure 6: Percentage of worked OHCA cases with ROSC, and the percentage of people who survived to 30 days
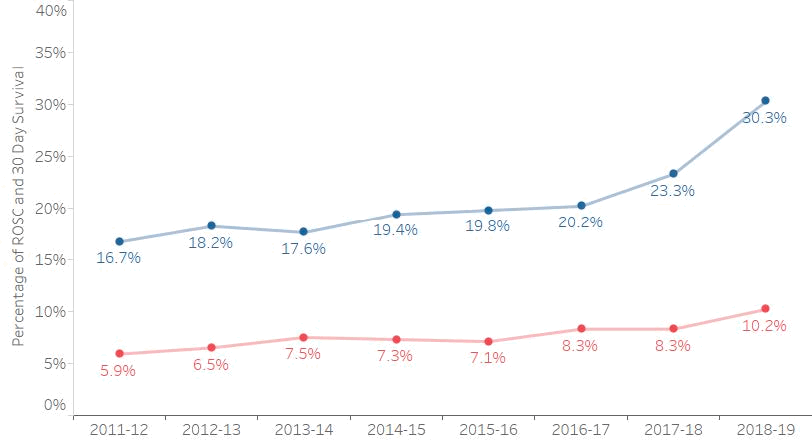
Figure 6: Shows the percentage of worked OHCA cases where the patient had ROSC (blue line) and those who survived to 30 days (red line) , 2011/12 to 2018/19.
Survival for shockable versus non-shockable rhythms
BOX 5
The Utstein Comparator
The Utstein templates aim to provide uniformity to OHCA data definitions. Analysis of the ‘Utstein comparator group’ (bystander witnessed cardiac arrest with an initial shockable heart rhythm) attempts to allow some adjustment for case mix7.
Appendix 1 contains tables showing a comparison of bystander CPR rates, ROSC rates and survival for patients with shockable versus non-shockable rhythms. In 2018/19 the ROSC rate for the shockable rhythm cohort rose to 47.0% from 39.1% the previous year. Survival to 30 days was 25.9% in the Utstein Comparator group in 2018/19, up from 21.9% in 2017/18.
Figure 7: Number of worked OHCA cases with a shockable initial ECG rhythm, and the percentage of which survived to 30 days
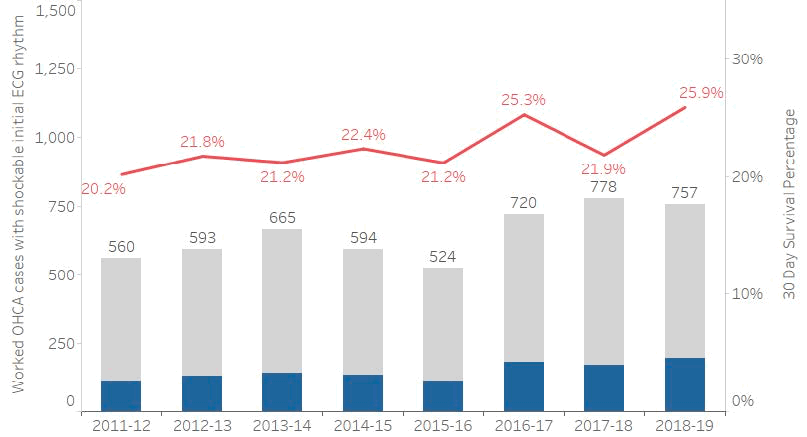
Figure 7: Shows the number of worked OHCA cases where the patient had a shockable initial ECG rhythm (blue shade in bar are 30 day survivors) and the percentage who survived to 30 days (red line), 2011/12 to 2018/19. Note: these data include linked incidents only.
Figure 8: Number of worked OHCA cases with a shockable initial ECG rhythm, and the percentage where bystander CPR was performed
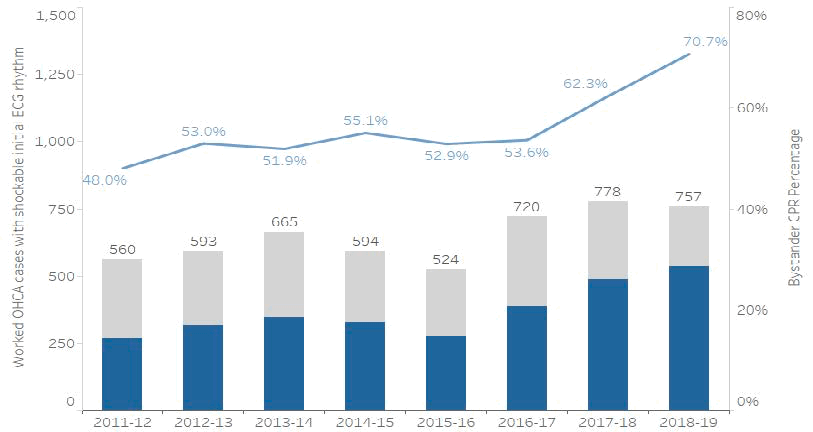
Figure 8: Shows the number of worked OHCA cases where the patient had a shockable initial ECG rhythm (blue shade in bar received bystander CPR) and the percentage where bystander CPR was performed (blue line), 2011/12 to 2018/19. Note: these data include linked incidents only.
Figure 9: Number of worked OHCA cases with a non-shockable initial ECG rhythm, and the percentage of which survived to 30 days
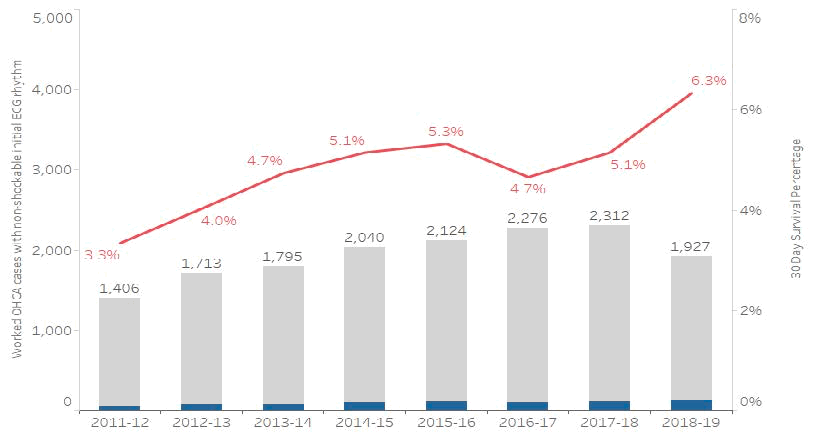
Figure 9: Shows the number of worked OHCA cases where the patient had a non-shockable initial ECG rhythm (blue shade in bar are 30 day survivors) and the percentage who survived to 30 days (red line), 2011/12 to 2018/19. Note: these data include linked incidents only.
Figure 10: Number of worked OHCA cases with a non-shockable initial ECG rhythm, and the percentage where bystander CPR was performed
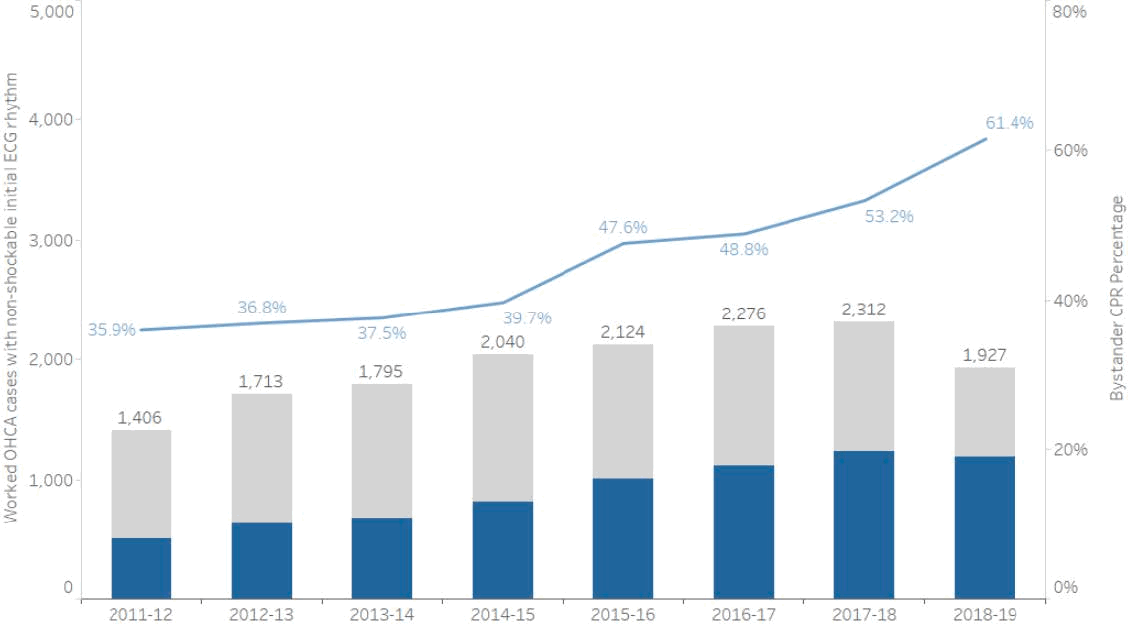
Figure 10: Shows the number of worked OHCA cases where the patient had a non-shockable initial ECG rhythm (blue shade in bar received bystander CPR) and the percentage where bystander CPR was performed (blue line), 2011/12 to 2018/19. Note: these data include linked incidents only.
ROSC and 30 day survival have increased fairly steadily year on year for both types of cardiac arrest with shockable rhythms having a much higher rate of survival. This difference is in keeping with the international literature and reflects differences in the reversibility of the underlying cause of cardiac arrest in the two groups8 9. It is notable that those presenting in a non-shockable rhythm appear less likely to have received bystander CPR. This raises the possibility that lack of bystander action in this group of patients means that shockable VF rhythms may deteriorate to non-shockable asystole by the time the ambulance service arrives.
Contact
Email: SWStat@gov.scot