Scottish Government: Suicide Prevention Strategy 2013 - 2016
The Scottish Government's suicide prevention strategy to 2016 sets out key areas of work that we believe will continue to reduce the number of suicides in Scotland.
Progress since 2002
The Scottish Government's target is to reduce the suicide rate in Scotland by 20% by 2013. Since 2002 - when the target was originally set as part of the Choose Life strategy and action plan - we have seen an 18% reduction in the suicide rate. In the years 2009 to 2012 we have seen the lowest number of suicides since the early 1990s[3] and a reduction in the number of suicides at a time when most other jurisdictions are seeing an increase.
Taking probable suicide figures for 2011 and 2012 together, almost three quarters (1,112 - or 72.5%) of those who died were male. This gender imbalance has been broadly consistent for much of the last 10 years - a major element of the 18% reduction in the suicide rate since 2000-2002 has been the reduction in male suicides, whereas those for females have been more stable. Indeed, female suicide rates have been fairly stable since the early 1990s.
The graph below shows the change in suicide rates over time using three-year rolling averages.[4]
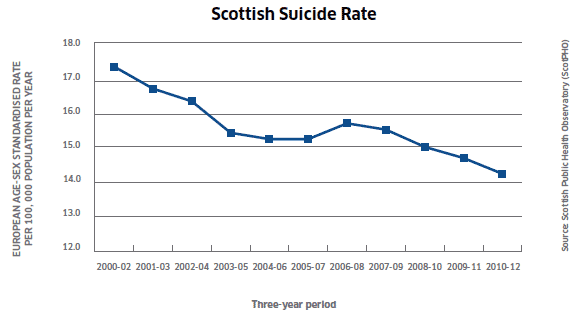
Though comparative figures are problematic given the different approaches to reporting suicide across the world, Scotland's rate of 14.0 deaths per 100,000 population in 2012 is below the "global" mortality rate of 16 per 100,000 and around the EU average.[5]
Suicide is a complex phenomenon and it is difficult to attribute increases or decreases in the overall national suicide rate to particular changes in circumstances, services or policy, but there are a number of factors which may explain why the experience in Scotland has been different from elsewhere:
- The emphasis on tackling problem drinking - this work has been in place since 2008 and in the most recent year to end March 2013, over 61,000 alcohol brief interventions were delivered in primary care, A&E and antenatal care settings with a further 33,000 interventions carried out in other locations, exceeding the target by 55%.[6]
- The increased focus on identifying and treating depression in primary care settings - since 2006 the GP contract has targeted this work with the consequence that more people who are ill receive treatment, with that treatment since 2008 being more likely to be through access to an evidence-based psychological therapy.[7]
- Local patient safety improvements introduced on the basis of evidence developed by the UK-wide National Confidential Inquiry into Suicide and Homicide by People with Mental Illness,[8] in particular work on discharge planning taken forward as part of the previous reducing readmissions target.
- Work to increase workforce knowledge and understanding of suicide - by September 2013 more than 50% of frontline NHS staff had received at least one specific course on suicide intervention (STORM, ASIST, safeTALK or SMHFA).
- Having a 10-year national strategy and action plan that has been regularly evaluated and refreshed, giving us a sustained focus on suicide prevention actions and outcomes.
Contact
Email: Janet Megoran