National dementia strategy: 2017-2020
Our new strategy builds on progress over the last decade in transforming services and improving outcomes for people affected by dementia.
3. What we will do now: our commitments
Diagnosis and post-diagnostic support
There are obvious benefits to obtaining a dementia diagnosis earlier rather than later, and it remains our ambition that more people are diagnosed earlier and get timely access to good quality post-diagnostic support. However, we also accept that there are still challenges around earlier diagnoses, especially in those cases where a definitive diagnosis is harder for a clinician to make in the earlier stages of the illness.
Scotland's Health Improvement, Efficiency, Access and Treatment ( HEAT) Standard from April 2013 is that everyone newly diagnosed with dementia is entitled to be offered, at minimum, a year's worth of post-diagnostic support, coordinated by an appropriately trained Link Worker. [8] Alzheimer Scotland's 5 Pillars Model of Post Diagnostic Support has been suggested as a useful model for post-diagnostic support (see Figure 1 below). [9] This model provides a framework for people living with dementia, their families and carers. It offers strategies, connections and resources on how to plan living as well as possible with dementia and to prepare for the future.
We will offer everyone newly diagnosed the guaranteed minimum of one year of appropriate post-diagnostic support. Those individuals diagnosed early, and assigned a named Link Worker, will continue to receive support using the 5 Pillars approach for the duration of their time living with dementia, or until such times as their needs change, and they require greater care coordination.
Figure 1: Alzheimer Scotland's 5 Pillars Model of Post-Diagnostic Support
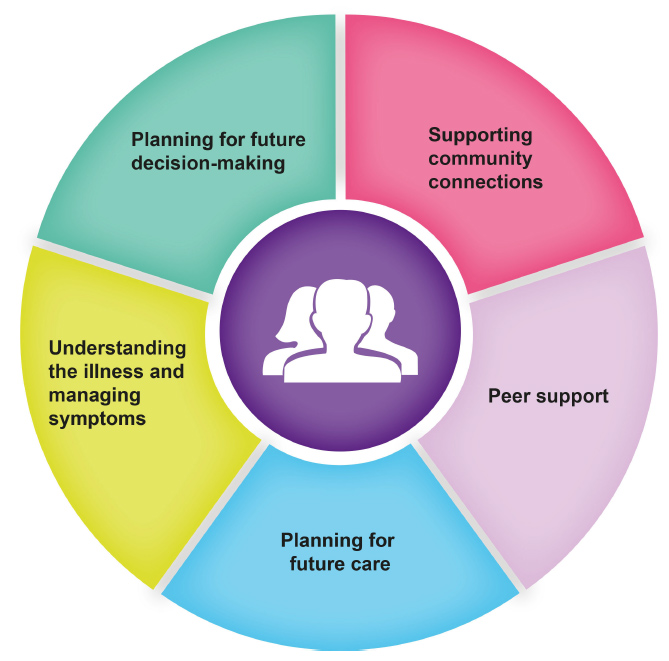
The development of the 5 Pillars Model and the post-diagnostic service offer was originally framed with a focus on people receiving an early diagnosis and living at home or in the community, with little formal health or care service support.
Feedback from people receiving this post-diagnostic service is that it works well. Our recent research on dementia incidence has shown, however, that increasing numbers of people are being diagnosed later in life and that many also already have significant care needs. [10] Such people are eligible for post-diagnostic support but may already be receiving substantial support for other long-term or chronic conditions, or for palliative care; some may also be in residential care settings. We believe that people in this category should continue to benefit from post-diagnostic support, but the consensus is that they should move directly into the care coordination phase, with appropriate support forming part of that process rather than standing as a separate process.
Alzheimer Scotland's 8 Pillars Model of Integrated Community Support provides a useful platform for coordinated care to support people with dementia living at home during the moderate to severe stages of the illness (see Figure 2 below). [11] The approach centres around a Dementia Practice Coordinator who provides tailored post-diagnostic support while at the same time increasing the level and focus of integrated care coordination.
Figure 2: Alzheimer Scotland 8 Pillars Model of Integrated Community Support
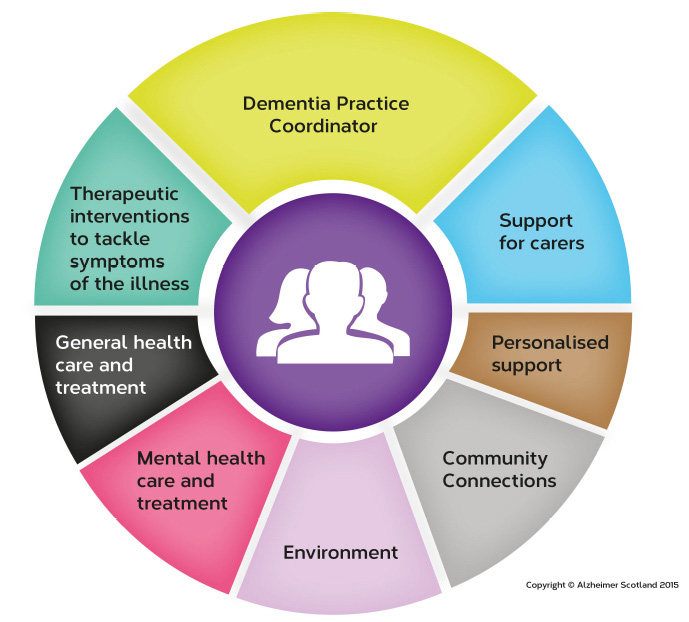
This approach offers a foundation for good quality integrated care and does not need to be driven by time constraints - because the dementia support will be integrated within the existing support being delivered by the established health and social care team. Individuals' and their carers' needs will determine how long the support will be needed to ensure it provides added value to the individual's care. In these cases care and support will already be intensive and ongoing. This approach will also be essential to support people with dementia and their families as they progress towards the more advanced and palliative stages of the illness.
On the basis of our research, we are therefore proposing that:
- All people newly diagnosed with dementia will receive appropriate support following diagnosis, with that support being either (a) the current model of post-diagnostic support, or (b) care coordination, based on the 8 Pillars Model of Integrated Community Support. The decision as to the most appropriate option will be based on clinical assessment
- The period of support in each case will be open ended and flexible. For those who receive post-diagnostic support in an integrated community-based way, this will continue without a time limit. Following the conclusion of the initial programme of work, and if the individual does not move on to the care coordination phase, they will be able to access their named Link Worker again, whether within the year previously stipulated or not. This will allow flexibility for those who might require additional contact or reengagement with the service.
Examples of how a Dementia Link Worker establishes a relationship and develops person-centred support can be viewed in the media clips available http://www.alzscot.org/link-worker-video. These short clips capture and convey the lived experience of good dementia support and care.
Alternative method to measure quality of post-diagnostic support
Adopting a more flexible approach, rather than specifying a particular time frame in which to deliver post-diagnostic support, requires the adoption of a new quality measurement framework. Adapting the arrangements for measurement of delivery will enable us, over time, to give assurances that the commitment is being delivered appropriately. We will work with stakeholders to develop this framework and to agree a new set of standards and monitoring requirements.
COMMITMENT 1: We will revise the national post-diagnostic dementia service offer to enhance its focus on personalisation and personal outcomes in the delivery of post-diagnostic services.
Role of primary care services
The 'optimum' model of post-diagnostic support continues to be one where the person with dementia is diagnosed early enough that they can take as active a part as possible, and have as much control and choice as they want, in the process. We want to make more progress in achieving this, and we believe there are benefits in offering post-diagnostic services within primary care.
One key benefit is that these services will become more accessible, which may encourage more people to come forward earlier for diagnosis or a memory assessment. While this service would not remove the need for referral into specialist diagnostic services, the management of an individual's care and support would sit in primary care, led by the Dementia Link Worker, thus ensuring that people receive support at the right time. This sits well with our vision for the future of primary care services in Scotland, where multi-disciplinary teams work together to deliver support to people in the community that anticipates and prevents illness, allowing GPs to spend more time with patients.
It is for these reasons that we wish to test the relocation of post-diagnostic services in primary care settings. The test sites will be located in Nithsdale, North-East Edinburgh and Shetland. Their overall purpose will be to assess the value of delivering post-diagnostic support in primary care settings.
COMMITMENT 2: We will test and independently evaluate the relocation of post-diagnostic dementia services in primary care hubs as part of the modernisation of primary care
Integrated care and support
One of the most important outcomes for this new strategy is that more people with dementia are able to live safely and with as good a quality of life as possible at home or in a homely setting for as long as they and their family wish.
To this end, we will support and encourage Integration Authorities to further develop and embed home-based, enabling and preventative supports for people with dementia - supports which keep people safe and sustain quality of life at home or a homely setting for as long as possible. Such supports might include helping the individual with dementia to attend to their other health needs such as hearing, eyesight and dental care.
Actions will include:
- dementia-specific and associated national improvement support through Healthcare Improvement Scotland to encourage and support ongoing local whole-system re-design
- ongoing national and local approaches to educating, training and developing staff on dementia
- ongoing development, sharing and exploration of dementia data
- ongoing engagement with local dementia service commissioners, planners, service managers and data specialists around the national post-diagnostic commitment.
We will work with Integration Authorities to inform and support planning, commissioning and redesign of local dementia services, across the whole care pathway. This will include improvement support for dementia palliative and end of life care and testing Alzheimer Scotland's Advanced Care Dementia Palliative and End of Life Care Model through Healthcare Improvement Scotland. [12]
COMMITMENT 3: We will support the Integration Authorities to improve services and support for people with dementia as part of our implementation of key actions on delayed discharge, reducing unscheduled bed days, improving palliative and end-of-life care and strengthening community care.
Alzheimer Scotland's 8 Pillars Model of Integrated Community Support has been tested in five areas: Greater Glasgow and Clyde, Highland, Midlothian, Moray, and North Lanarkshire. These sites have received national improvement support from Health Improvement Scotland's Focus on Dementia team.
Considerable learning has been generated from the tests, which will be useful in the ongoing development of dementia services. A subsequent evaluation found that, overall, the 8 Pillars Model was seen as a useful framework for delivering integrated, home-based services for people with dementia and their families, particularly by encouraging and reinforcing a 'whole person' approach to supporting individuals. [13] Individuals and families also valued having a named Dementia Practice Coordinator.
The evaluation also highlighted a number of challenges, including the need to ensure continuity of care and the adoption of preventative approaches within current resource constraints. In addition, while there were clear benefits to interdisciplinary approaches and co-location of services, there were challenges in embedding such approaches. Finally, the evaluation highlighted the need to develop staff skills and competencies around therapeutic interventions.
COMMITMENT 4: We will consider the learning from the independent evaluation of the 8 Pillars project on the benefits and challenges of providing home-based care coordination and proactive, therapeutic integrated home care for people with dementia.
Palliative and end of life care
We are committed to ensuring that more people get timely access to good quality palliative and end of life care.
Alzheimer Scotland's Advanced Dementia Practice Model combines the skill and understanding of the existing 8 Pillars team, particularly the Dementia Practice Coordinator, as described in the 8 Pillars Model of Community Support, and introduces an Advanced Dementia Specialist team to provide optimum care. In such circumstances, the Dementia Practice Coordinator would retain primary responsibility for the direction and management of the care, but would also coordinate any input from the advanced team. The coordinator would have a critical role in supporting the person with dementia to die in their place of choice and to support those closest to the person through the bereavement process.
COMMITMENT 5: We will test and evaluate Alzheimer Scotland's Advanced Care Dementia Palliative and End of Life Care Model.
Our Strategic Framework for Action on Palliative and End of Life Care outlines the key actions to be taken to allow everyone in Scotland to receive services that respond to their individual palliative and end of life care needs. We will seek to ensure that people receive health and social care that supports their wellbeing, irrespective of their diagnosis, age, socio-economic background, care setting or proximity to death. Moreover, we will seek to ensure people have opportunities to discuss and plan for any future decline in health, preferably before a crisis occurs. Many people at this stage in life are frail and elderly and have a range of conditions. Attempting to provide support often results in a number of parallel approaches, which are not always well connected. One element these approaches have in common is a focus on having conversations about what matters to people and the development of collaborative, relational decision making and planning, which lies at the heart of person-centred care.
One model which many are finding helpful in supporting such approaches is the House of Care. [14] This model details the components necessary to ensure collaborative care and support planning. This approach supports and enables people to articulate their own needs and decide their own priorities, through a process of joint decision making, goal setting and action planning.
The House of Care represents a tangible approach that allows health and care services to embrace collaborative care and support planning and to fulfil their responsibility to support people to live and die well, on their own terms, with whatever long-term conditions they have.
Figure 3: The House of Care Model
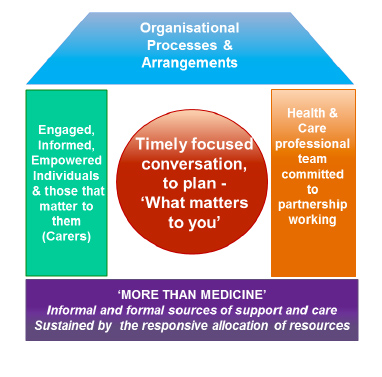
COMMITMENT 6: We will work with stakeholders to identify ways to make improvements in palliative and end of life care for people with dementia.
Improving dementia care in acute and specialists settings
Improving the care of people with dementia in acute general hospitals and specialist NHS dementia hospital settings has been a key priority in recent years, and this will continue through this new strategy. We will strengthen the links between this work and our action on delayed discharge and reducing avoidable admissions and inappropriately long stays in hospitals.
Much of our focus remains on ensuring people with dementia are not unnecessarily admitted to acute care. This means, for example, making adjustments at home to minimise the risks of burns and falls. When someone with dementia does require acute care, the challenge is to ensure that, as well as receiving safe and effective care, their dementia is recognised and responded to appropriately.
In partnership with stakeholders, we published the 10-Point National Action Plan. This plan supports the implementation of the Standards of Care for Dementia in acute care to ensure the current system of hospital care is improving the capability and capacity of staff working in such settings. [15] As well as supporting service transformation and strategic ownership of this agenda at an NHS board level, it has helped to focus and coordinate a range of existing initiatives.
As part of this national action, Healthcare Improvement Scotland's ( HIS) Focus on Dementia team is working with local teams to improve the quality of care experience and outcomes for people with dementia and staff within acute settings. HIS also uses the Standards of Care for Dementia in its ongoing programme of inspections of older people's care in acute general hospital settings.
Within specialist dementia NHS settings, we are committed to improving the quality of care. The Mental Welfare Commission report, Dignity and Respect, found that too many people did not have an adequate care plan and that medication reviews were often lacking for those receiving psychoactive medicines. [16] Our 10-Point National Action Plan sets out a range of actions around educational and improvement work and self-assessments and reporting.
COMMITMENT 7: We will continue to implement national action plans to improve services for people with dementia in acute care and specialist NHS care, strengthening links with activity on delayed discharge, avoidable admissions and inappropriately long stays in hospital.
Care homes
Challenges remain around the provision of care for people with dementia in care homes. Going forward, care homes will increasingly need to provide specialist care, including palliative and end of life care, for people with dementia.
Much of our ongoing national dementia workforce activity involves supporting improvements in the quality of dementia care and support in these settings, including increasing the provision of dementia training the range of therapeutic interventions available. This complements our other commitments such as paying the Living Wage to adult social care staff to improve recruitment and retention rates, and the reform of the National Care Home Contract.
During the second dementia strategy, we set up the National Group on Dementia in Care Homes to consider ways to support delivery of the Standards of Care for Dementia in care home settings and to ensure that the wider ongoing work to transform the care home sector reflects the needs of the dementia care client group.
We will work with stakeholders in responding to the findings from the forthcoming Care Inspectorate report into dementia care in care homes due to be published in 2017.
COMMITMENT 8: We will continue the National Group on Dementia in Care Homes to help ensure that the ongoing modernisation of the care home sector takes account of the needs of people with dementia, and will consider the findings of the Care Inspectorate's themed inspections.
Workforce skills and competencies
We will continue to support the implementation of Promoting Excellence - our national knowledge and skills framework for staff working with people with dementia - through this new strategy. As well as extending the reach of workforce learning and training opportunities, we will support improvements across this strategy's priority areas: post-diagnostic support, integrated care and support for people at more advanced stages of dementia, and palliative and end of life care.
COMMITMENT 9: We will continue to support the ongoing implementation of the Promoting Excellence dementia health and social care workforce framework.
Allied health professional led interventions
We commissioned Alzheimer Scotland to develop an evidence-based policy document outlining the contribution of the allied health professionals ( AHP) to integrated home care and across the care pathway. Connecting people, connecting support: The allied health professional offer to people living with dementia in Scotland will be published in 2017. It will set out how the rehabilitation skills and expertise of the AHP workforce can have an even greater positive impact on the lives, experiences and outcomes of people living with dementia, for example in the provision of adaptations for the home and falls prevention. The programme will be underpinned by a national measurement framework based on improvement methodology to support local implementation. The programme will be implemented by a partnership including Alzheimer Scotland, senior AHPs from all professions across Scotland and other key stakeholders.
COMMITMENT 10: We will support the implementation of the new national AHP Framework Connecting People, Connecting Support.
Technology
We want to do more to make technology accessible for people with dementia. Whether it is simple adaptation of household gadgets, such as see-through toasters, large button remote controls, memory aids and prompts or the use of more cutting edge GPS technology, the opportunities for technology to successfully enable someone to live safely and longer in their own home are significant.
We are working with Alzheimer Scotland to develop a programme of transformational change around the use of technology for people living with dementia to ensure mainstreamed approaches to technology. The first stage of this was the creation and dissemination of the Technology Charter for People Living with Dementia in Scotland. [17] The charter's vision is that people living with dementia in Scotland will benefit from technology to help them live a healthy life - safely, securely and confidently as full citizens in society. This is a fundamental right, and we are working to embed technology-based solutions in every post-diagnostic conversation taking place across Scotland.
We have appointed three Senior Technology Coordinators who will support Integration Authorities. We are designing a blended training programme that will be similar to the Dementia Champions programme. The coordinators will lead on the grassroots changes needed to apply tech-based solutions and will support the workforce to implement a solution-based approaches.
COMMITMENT 11: We will implement the Technology Charter for People in Scotland with Dementia, ensuring that everyone with a diagnosis of dementia and those who care for them are aware of, and have access to, a range of proven technologies to enable people living with dementia to live safely and independently. We will continue to explore innovative ways in which technology can be used and adapted for people living with dementia.
Housing support and interventions
As people age, their housing needs change and some people, such as those with dementia, also need specialised housing-related support services. For people with dementia, a familiar home environment is particularly important, especially as their symptoms develop. Early consideration of the role of aids and adaptations is an essential part of enabling people to live safely at home.
Scotland's housing strategy for older people, Age, Home and Community, has an overarching aim that more older people are enabled to enjoy full and positive lives in their own home or in a homely setting. Over the next three years we will work with national and local stakeholders including Integration Authorities to develop and implement the next phase of national action in this area. This will include consideration of the potential to test models on specialist dementia housing.
We will also consider and respond to the Chartered Institute of Housing ( CIH) Scotland on their Housing and Dementia Programme Phase 2 Findings. [18] The CIH previously worked with partners on Phase 1 work on measuring the baseline on housing sector engagement on dementia and producing a dementia-friendly housing design guide with the Dementia Services Development Centre. We will also build on work already undertaken to spread elements of Promoting Excellence to the housing sector.
COMMITMENT 12: We will work with national and local stakeholders to implement actions in the refreshed Age, Home and Community: A Strategy For Housing For Scotland's Older People: 2012 - 21 to support people to live safely and independently at home for as long as possible.
Transport
People living with dementia have the right to full inclusion and participation in the community. This includes the use of private and public transport. However there are difficulties for people living with dementia such as journey planning, challenging travelling environments and lack of service integration. It is vital that we work with relevant service providers to create integrated, enabling journeys; this requires education and training for service providers. We need to move towards new approaches in service design, delivery and support which help providers to understand their role in enabling people living with dementia to travel well. This can only be meaningfully developed and delivered with and by people affected by dementia.
COMMITMENT 13: We will consider what national action is required to support further improvements in transport for people with dementia.
Dementia-friendly communities
There have been considerable advances in local areas in developing and embedding dementia-friendly community initiatives, including in Motherwell, the Highlands, Stirling, Edinburgh and Prestwick. There are helpful national initiatives such as Alzheimer Scotland's Dementia Friends initiative, and its Football Memories project, which it delivers in partnership with the Scottish Football Museum as part of its pioneering Football Reminiscence work. This has now expanded to include other sports. There is a range of other dementia friendly initiatives such as Playlist for Life, dementia friendly checkouts in supermarkets, as well as a wide range of mainly locality-based investment by The Life Changes Trust. An evaluation of the Life Changes Trust projects can found in Dementia Friendly Communities in Scotland Report 2. [19]
We are keen to work with partners, including Alzheimer Scotland and Integration Authorities, to explore the possibility of further supporting and nurturing dementia befriending.
COMMITMENT 14: As part of supporting local activity on dementia-friendly communities, we will work with partners to explore the potential to promote and support increased participation in dementia befriending.
Dementia and equalities
Addressing equalities issues around accessing a dementia diagnosis and services remains a key part of our work. The main themes in the NHS Health Scotland report Dementia and equality - meeting the challenge in Scotland 2016 were:
- raising awareness and increasing understanding of signs and symptoms of dementia among all of Scotland's different population groups is fundamental to promoting early diagnosis
- there is a need to continue to ensure clearly signposted, robust, culturally competent, locally informed services and post-diagnostic support pathways for people from the protected characteristic groups with a diagnosis of dementia
- appropriate workforce knowledge and skills are essential to encouraging people to seek help early especially those with protected characteristics, and to providing a supportive post-diagnostic pathway
- further research is needed to determine the most effective ways to raise understanding and awareness of dementia among different population groups. [20]
COMMITMENT 15: We will support implementation of NHS Health Scotland's report recommendations on dementia and equalities.
Adults who go missing
People, including those with dementia, can and do go missing from communities across Scotland. Work in local authority areas to respond to this issue vary depending on the local circumstances, but all agencies engaged focus on locating those who have gone missing. The response to a missing person is determined by the available information - or in some cases the lack of information. There are particular groups who may be at higher risk of going missing, including children and young people in care and adults with dementia.
Police Scotland have developed and piloted protocols, with partners, for three high-risk groups, including adults who go missing from care homes in Scotland. The pilots began in 2015 in three Police Scotland divisions with the aims of safeguarding and preventing people at risk of going missing, and of activating the appropriate response when they do go missing to ensure they are found safe and well.
COMMITMENT 16: We will consider the upcoming recommendations of Police Scotland Missing Persons report for the dementia client group.
Dementia research
Dementia research in Scotland covers a range of disciplines from basic science through to clinical, social and policy research, and involves people with dementia through an increasing body of co-produced research. Activity focuses around key research themes: drug discovery, diagnosis, improving lives and prevention.
This third dementia strategy will continue to support the collaborative efforts of the Scottish Dementia Research Consortium in pooling the resources and skills of the wide ranging research community in Scotland and using this platform as a means of encouraging greater investment and research into Scotland.
The Scottish Government Chief Scientist Office will continue to welcome applications to its funding committees from those working in dementia research. The Scottish Dementia and Neuroprogressive Disease Research Network will continue to promote a culture of clinical research in dementia across Scotland and maximise access to clinical trials for patients living in both rural and urban areas.
We will continue to build linkages with the UK Dementia Research Institute, in particular the hub based at the University of Edinburgh, and look to build links from research evidence into the public health review and Scotland-wide health and social care policy.
COMMITMENT 17: We will support the clinical and non-clinical research community in Scotland, including supporting linkages to the UK-wide research institute, linking policy and research in Scotland, and showcasing examples of dementia research in Scotland.
Reducing inappropriate prescribing of antipsychotic medication
A key driver to ensure care and treatment is always safe, effective and appropriate is working with partners to reduce the inappropriate prescribing of psychoactive medication for people with dementia.
People with dementia are entitled to care that is appropriate to their needs which recognises, promotes and protects their rights and dignity, including safeguarding rights to safe and appropriate care and treatment. We should seek to maximise their involvement and say in how care and treatment is delivered, as well as help people retain existing capabilities, as far as possible. These principles underpin the dementia standards and the Promoting Excellence framework.
In 2012 we commissioned research into time trends in the prescribing of antipsychotic and other psychotropic medications to older people with dementia between 2001 and 2011. [21] The research shows that, since 2009, there has been a decline in the initiation of new antipsychotics and a moderately decreasing trend in antipsychotic use. The report also show that in the first quarter of 2011 the rate of older people with dementia being prescribed an antipsychotic was at the lowest level over the period 2001 to 2011.
COMMITMENT 18: We will commission and publish a renewed study on trends in the prescribing of psychoactive medications for people with dementia.
Estimating dementia prevalence
When Scotland's first national dementia strategy was published in 2010, the Scottish Government adopted a dementia prevalence model used by Alzheimer Scotland called Eurodem. As dementia policy developed, Alzheimer Scotland, the Scottish Government and others adopted the Eurocode (plus Harvey) model, the result of which estimated dementia prevalence In Scotland - that is, the estimated number of people living with dementia at a particular point in time - to have risen from 70,000 to up to 90,000. NHS England has used the Dementia UK model which, if applied to Scotland, would give an estimated prevalence of around 65,000.
Following the successful completion and publication of Scotland's first estimated annual diagnosed dementia incidence report in December 2016, we think it would be useful to investigate dementia prevalence further, in collaboration with our partners.
COMMITMENT 19: We will commission fresh work to assess dementia prevalence, and consider which current prevalence model applies best.
Practice guidelines
The Scottish Intercollegiate Guidelines Network ( SIGN) develops evidence-based clinical practice guidelines for the NHS in Scotland. SIGN guidelines are derived from a systematic review of the scientific literature and are designed as a vehicle for accelerating the translation of new knowledge into action to meet our aims of reducing variations in practice and improving patient-important outcomes.
SIGN 86 on dementia was published by SIGN in 2006 and includes clinical advice on best practice in areas such as medications to slow progression of the illness and prescribing sedative medication in response to stress and distress. [22] The Standards of Care for Dementia provide overall standards on dementia care, including the options which should be considered before considering prescribing sedative, or psychoactive, medication.
COMMITMENT 20: We will assess if there is any need for updated dementia clinical guidelines or guidelines on specific elements of clinical dementia treatment.
Governance
As in our previous strategies, a national governance group will be established to oversee monitoring and implementation of this new strategy. The group will be a broad-based and include service users and carers as well as Integration Authorities. The group will also invite additional contributors, from Scotland and beyond, and will sit alongside the national implementation and monitoring group on post-diagnostic support.
COMMITMENT 21: We will establish a national policy governance structure for monitoring and implementing the third national dementia strategy.
Contact
Email: Darren Tierney
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG