Ministerial Task Force on Health Inequalities: report 2013
This is the second review by the Ministerial Task Force on Health Inequalities following publication of Equally Well in 2008.
3. Health inequalities in Scotland
This chapter briefly describes the evidence presented to the Task Force about Scotland's current position with regards to health inequalities, and what we can learn from how our health inequalities compare with similar parts of Europe and the UK. It draws from presentations to the Task Force which can be found on the government website [5] .
Key Points
- Scotland's health is improving.
- Scotland's health is improving more slowly than other European countries.
- Mortality rates have improved in deprived and affluent areas at broadly the same rate, leading to an increase in relative inequalities. In order to reduce health inequalities there needs to be a faster improvement in the most deprived areas.
- Scotland has not always been an unhealthy society compared to the rest of Europe.
- The origins of health inequalities are the inequalities in power, money and resources between deprived and affluent groups, which impacts through complex interactions between social economic, educational and environmental determinants of health.
- Conventional approaches to the problem that involve attempts to modify the health related behaviours of poorer people have failed.
- We must address wider inequalities in society, unless and until we do that health inequalities will persist.
3.1 The continuing problem of health inequalities
The Scottish Government published its health inequalities indicators in October 2012 (Annex B). The report showed that whilst there was evidence of improvement, this was only achieved amongst one or two of the indicators. For example, whilst there has been a narrowing of the gap in low birth weight babies, having a baby with a low birth weight was still twice as common in poorer homes in comparison with more affluent ones. There has also been a 40% reduction in first admission to hospital for heart attack between 1997 and 2009 in those under the age of 75. Not only had there been a significant fall in admission rate but there also had been a narrowing of the gap between rich and poor both in absolute and relative terms. However, these trends are small and fragile, and are minor exceptions when compared with other indicators. Since the Task Force last met (in June 2013) the latest position on these national health inequality indicators has been published [6] . Once again, no significant narrowing of the gap has been observed.
The Task Force noted that mortality among younger working age adults (aged 15-44 years) in Scotland is a particular cause for concern. Whilst mortality in this age group fell between the 1950s and the mid-1980s, there has been no net improvement for men or women in this age group since then. These trends are unusual in a European context and Scotland's relative ranking compared to other European countries has become progressively worse for both sexes across this age group over the last 55 years. This contrasts with trends amongst older working age or older age populations. There are also concerning trends amongst some specific causes of death, for example of lung cancer mortality of women and male suicides, which are contributing significantly to early death in the young working age population.
3.2 Comparing Scotland to Europe
In terms of life expectancy, until about 1950 Scotland ranked in the middle of the countries of Europe, neither exceptionally good nor bad. However, from the second half of the last century onwards, Scotland's position has worsened, so that as we approached the turn of the millennium, Scotland's health was at the bottom of the Western European league table.
This differential growth in life expectancy has puzzled many who believe that there is something inherently unhealthy about Scotland or the Scottish people. The evidence suggests that Scotland has not always been an unhealthy society.
Figure 1. Male life expectancy: Scotland (shown in blue) & other Western European Countries, 1851 - 2005
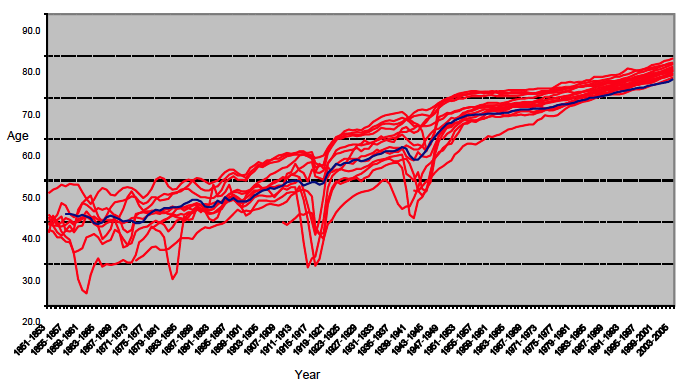
Source: Human Mortality Database
Figure 1 shows that a relative slowing in the rate of improvement in life expectancy, compared to the other countries of Western Europe, took place in Scotland's health around 40-50 years ago. This caused Scotland's life expectancy to fall behind our Western European neighbours after the 1950s.
Social Capital
Social capital describes the pattern of networks amongst people and the shared values which arise from those networks. Greater interaction between people generates a greater sense of community spirit. The definition used by the Office for National Statistics, taken from the Office for Economic Co-operation and Development ( OECD), is 'networks with shared norms, values and understandings that facilitate co-operation within or among groups'.
Higher levels of social capital are associated with better health, higher educational achievement, better employment outcomes, and lower crime rates. There are a number of different aspects to social capital:
- levels of trust - for example, whether individuals trust their neighbours.
- membership - for example, to how many clubs, societies or social groups individuals belong.
- networks and social contacts - for example, how often individuals see family and friends.
Formal and informal networks are central to the concept of social capital.
- Bonding social capital - describes closer connections between people and is characterised by strong bonds. For example, among family members or among members of the same ethnic group: it is good for 'getting by' in life.
- Bridging social capital - describes more distant connections between people and is characterised by weaker, but more cross-cutting, ties. For example, friends from different ethnic groups, friends of friends: it is good for 'getting ahead' in life.
- Linking social capital - describes connections with people in positions of power and is characterised by relations between those within a hierarchy where there are differing levels of power: it is good for accessing support from formal institutions.
Shared norms, values and understandings relate to shared attitudes towards behaviour that are accepted by most individuals and groups as a 'good thing'. These norms of behaviour are understood by most members of society. Groups in this context are very broadly defined and can refer to:
- geographical groups - such as people living in a specific neighbourhood.
- professional groups - such as members of a local association or voluntary organisation.
- social groups - such as families, church-based groups, groups of friends.
- virtual groups - such as the networks generated through common interest groups.
Social capital is just one of the psycho-social explanations for inequality of outcome in life. There are many other theories that could be classified as supporting the concept of "salutogenesis", or the creation of health. These include ideas such as emotional intelligence, learned optimism, and social connectedness. All are theories which help to explain why some people are more successful at creating good lives regardless of their circumstances. However, all point to the importance of inner psychological capacity as critical to sustaining wellbeing.
3.3 Understanding health inequalities in post-industrial Scotland
Some council areas and communities across Scotland have health outcomes that are comparable with the best in Europe. However, when Scotland is divided into its constituent local authorities, it is those people in post-industrial West Central Scotland, together with Dundee and the Western Isles, that have the greatest burden of poor health and early death. Higher levels of poverty and disadvantage are the root causes; and continued efforts to reduce poverty and income inequality within Scotland [7] form an essential foundation for action to reduce health inequality.
In addition, more detailed analysis of the West of Scotland's position relative to comparable regions in Europe, and of Glasgow relative to other UK cities, have highlighted the presence of a significant 'excess mortality' - which cannot be explained by the levels of income deprivation, income inequality or deindustrialisation in these areas of Scotland. Explanations for this excess are currently being explored, and it is clear that there will be no single factor that accounts for the difference. That said, plausible causes include lower levels of some aspects of social capital ( e.g. trust, reciprocity and social participation) [8] . There are significant associations between higher social capital and lower mortality: a recent review [9] concluded that 'both individual social capital and area/workplace social capital had positive effects on health outcomes, regardless of study design, setting, follow-up period, or type of health outcome.'
That social capital is one important factor in meeting the Scottish Government's key strategic objectives is clear. For example, the strategic objective to 'Help local communities to flourish, becoming stronger, safer places to live, offering improved opportunities and a better quality of life' (Safer and Stronger), reflects assumptions from social capital theory that if individuals and communities are supported to build their own capacities and networks, this will lead to improvements in wellbeing.
3.4 Summary
In summary, whilst Scotland's health is improving, it is improving more slowly than comparable European countries, and from the middle of the last century our health has dropped below that of our neighbours. As a general pattern, the rate of improvement in health in the poorer areas of Scotland is significantly slower that in the more affluent areas. The age group of 15 - 44 year olds appears to be the group amongst whom Scotland compares most poorly with our European peers in terms of excess deaths. There are also concerning trends amongst older working age women.
The origins of health inequalities are complex and they are to be found in the many interactions between social, economic, educational and environmental determinants. During its most recent discussions, the Ministerial Task Force on Health Inequalities recognised the continued need for concerted action across this range of determinants. It noted that the government's performance framework provides a structure for monitoring progress and identifying priorities for enhanced attention within this wide range of factors. The specific focus of the Task Force on this occasion was to consider how better health might be supported within Scotland's communities through considering the role of Community Planning Partnerships, the recommendations of the Christie Commission on the Future Delivery of Public Services, and how aspects of 'place' impact on health. The Task Force noted that in trying to understand the similarities and differences between communities, the level of 'social capital' was a potential contributing factor in determining positive outcomes. This had also been identified by the Christie Commission and was a feature of the Equally Well test sites.