Recommendations on The Future of Residential Care for Older People in Scotland
A strategic examination of the purpose and desired structure of residential care services fit for the aspirations and needs of future generation.
Part 3: Supporting Sustainable, Quality Care Services
Commissioning
Since the development of the National Care Home Contract in 2006, standardised contracts and more transparent and consistent approaches to funding care have been established. However, the current mix of services within the care home market is not producing optimum outcomes. There has been limited innovation in the sector. For example, the development of intermediate care facilities at scale has not happened (which would build up the confidence and abilities of older people who are ready to be discharged from hospital but not yet fit enough to live independently in their own home). In addition, generic long-term care provision has been variable, with a significant minority of operators continuing to provide care at undesirable quality levels.
There are a number of reasons that explain why we have been unable to move beyond the purchaser-provider paradigm. In part, this has been due to perception among commissioners that the private sector (which is the predominant sector), based on an appropriate return on capital investment, would make sound business decisions in localities with serviceable demand. In turn, consumer choice was held to drive market behaviour (in the sense that any market functions by responding to customers' preferences). As such, there was deemed to be less need for the purchaser (the local authority) to define what services were required since the end-user would be in a position to identify service requirements by exercising choice within the market place. In other words, the accepted paradigm was that care home operators would do the 'commissioning thinking' based on consumer preference, and local authorities and individuals would simply buy the product.
However, as the business models of providers became more elaborate, coupled with a downturn in the economy and a shift in policy direction, we have witnessed a gradual erosion of occupancy rates and a previously unknown financial fragility within the sector. What is more, the power of consumer choice has not delivered the innovation and market responsiveness that we would have expected. In a rational world, service users would avoid poorer quality homes, which would then be forced to exit the market; but in practice, the variability of information, fluctuating standards, the wish of service users to be placed close to their family or community, and the financial power of large national providers who can protect poorly performing homes, all distort the freedom of choice. And even in those circumstances where business failure does happen, there are significant political and professional reasons to prevent this form of market correction (there is significant evidence that sudden and unplanned closures impacts on the health and life expectancy of care home residents). For all of these reasons, a commissioning model has never developed. But precisely because of the deficits outlined above, now is the time to develop this thinking.
The commissioning process involves assessing and forecasting population need; planning the range, type and quality of services and support mechanisms that need to be put in place to meet to those population needs; putting in place arrangements to deliver or procure these services and support mechanisms; and reviewing the process by establishing whether objectives have been met. Health and Social Care Partnerships will be required to develop commissioning plans by law.
The Task Force has reviewed the effectiveness of commissioning levers. We believe that three central options are available to us to better support commissioning practice into the future:
- Develop and strengthen partnership working, to ensure that there is a common understanding of what type of services will be required into the future and at what volumes. This is implicit in the commissioning process, but can also be advanced through the use of Market Facilitation Plans;
- Explore new procurement methodologies, which would offer greater control over quality and capacity of provision in the market. For example, the commissioning partnership could enact preferences around quality, capacity and type of service by selecting 'preferred providers' through a tender process. While the non-successful providers will remain registered and hence a viable care destination, social workers would advise prospective service users of those care homes which meet the Partnership's commissioning requirements;
- Regulatory or legal controls over capacity. This could involve the introduction of a licensing regime, whereby the integration authority has a power to define local capacity. This is the model used in France, Canada and some parts of the US. It might also involve the use of physical planning regulations and policies to define the conditions under which a new care home development would be supported. Or finally, the Choice of Accommodation Directions could be revised once the Public Bodies (Joint Working) Bill is enacted, to ensure that care homes have been approved by the integration authority as meeting the requirements of its strategic plan.
In the end, the Task Force has come to the view that it is premature to take a more aggressive regulatory or legislative approach to controlling capacity - mainly because of possible unintended consequences / undesirable outcomes - and therefore recommends that Partnerships explore different procurement options within the context of their Joint Strategic Commissioning Plan. However, legal and regulatory reform should not be ruled out and the issue should be revisited within five years to ensure that local markets are responding to commissioning plans.
The Joint Strategic Commissioning Plan will specify the nature, scale and locality of provision a partnership intends to establish locally based on a strategic needs assessment. This will include plans for intermediate care and specialist long-term care provision for older people. Independent sector providers and their investors will be expected to take account of the JSC Plans. Where there is an expressed need for provision in areas of under-capacity it should attract new investment and new builds because of a clearly articulated need. The use of a Market Facilitation Plans will be crucial in working with private and voluntary sector providers. It is important that such statements are developed with a wide range of partner organisations, including financial institutions like the banks.
Commissioners will also need to develop clear information on the dependency levels of the current care home population. Tools, such as the Indicator of Relative Need (IoRN), should be promoted in order to obtain a better understanding of the needs of current care home residents to inform service development. Further work should be undertaken around care pathways, especially if we are to realise current policy goals such as the presumption against discharging direct from an acute bed direct to a care home.
Contingency Planning
The stability of the care home sector is of vital importance to the effective delivery of care and support to many older people in Scotland. Sadly, over the last five years, contingency planning has had to play a more prominent role in the management of the sector than we would have wanted. There are a variety of reasons that a care home may close, including: in response to unforeseen environmental factors, such as flooding or fire; as a result of enforcement action taken by the Care Inspectorate; or as a result of an organisation or business ceasing to operate. Our recent experience in Scotland has been of the latter example: a number of care home providers and/or owners have fallen into administration and have announced closure plans, sometimes at very short notice.
Inasmuch as the avoidance of a care home closure is not always possible or desirable, it is important that satisfactory arrangements are in place for the closure of an individual care setting and to ensure continuity of care for the residents affected. In planning for the closure of a care home, the interests and the welfare of the residents affected are paramount.
A high-profile example of the importance of good contingency planning relates to the collapse of Southern Cross Healthcare in 2011. This episode illustrated the dependency that we have on non-statutory providers to deliver care and of the importance of all parties - providers, lenders, local authorities, Health Boards, government and the Care Inspectorate - collaborating in the management of contingencies. Southern Cross operated 96 care homes in Scotland, across 28 local authorities. While the subsequent transition from Southern Cross to HC1 and other providers was managed effectively, it underlined the importance of having good contingency planning arrangements in place nationally and locally.
It is appropriate that the Task Force should take a view about how to deliver stability for the care home sector into the future, especially as the make-up and funding of the sector is likely to change. In particular, it is important that accurate information is shared across commissioning partners in relation to a number of key factors which the evidence tells us makes the difference between success and failure. It is therefore recommended that in Scotland we work towards a comprehensive risk register, to provide an early warning system for care providers experiencing operational or financial challenges - and an associated ladder of intervention for public authorities to co-produce solutions for exit or redesign of struggling services. An example risk register is set out in Annex B.
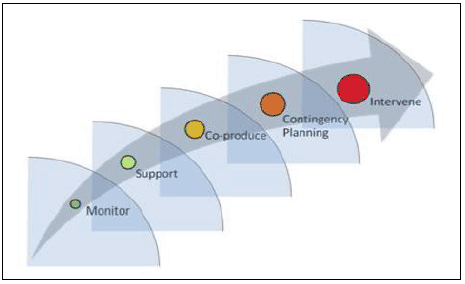
It is important to point out that this register should not function primarily to support punitive measures. Rather, it is intended to operate as a system of early intervention and prevention. It provides a ladder of support, to ensure that a standard monitoring of risk can be used to target support where care homes find themselves in difficulty, which in turn should lead the local authority or Health Board to work with the provider (and where appropriate the lender) to coproduce a solution that remedies the business failure. In the event that recovery is not possible, contingency planning and direct intervention may then be required.
It is also important that local partners give thought to the impact of risk assessment on the viability of a care home business, especially where the focus is on recovery. The use of tools to embargo admission can be helpful to ensure that prospective and existing residents are not placed at risk and to provide an incentive for care providers to improve performance. However, they can also expedite business failure because of lower occupancy levels and therefore it is important that their use is carefully considered. It is important that the local authority (or Health Board), the Care Inspectorate and provider communicate effectively where embargoes are used and that the same parties work constructively together when there are opportunities to lift these.
Regulation
The Care Inspectorate is Scotland's independent scrutiny and improvement body, and is responsible for providing assurance and protection for people who use social care services, their families and carers and the wider public. It also plays a key part in improving services for adults and children across Scotland.
As we move towards greater integration of health and social care, the Care Inspectorate is working more closely on developing a joint inspection regime covering health and social care services in partnership with Healthcare Improvement Scotland (HIS). This is a positive move for care homes and housing support providers whose clients often also require complex health care.
In terms of the scope of this report, the key service types under regulation, which we believe require either review or greater flexibility, include care home services; housing support services; support services; and adult placement services. The Task Force is clear that flexibility should be given to providers to innovate and provide different service design or delivery options - for example, more community outreach services. The Care Inspectorate's view is that variations (from the standard service template) that are reasonable, specific and justified, are possible. For example, conditions about numbers of service users, for specific service types, and conditions unique to the service at the point of registration are agreed with the service provider. The Care Inspectorate has signalled a willingness and strong support for the adaptation of approaches to registration and the process of agreeing conditions to registered services, to facilitate greater innovation in older people's care services. In terms of more specific reforms, the Task Force is recommending:
- a discussion on a new definition for housing support services within secondary legislation, to allow for more flexible service design and registration;
- further discussion on registered care home services adding to their functions (e.g. day care/respite; laundry; meals; activities) to provide an outreach service to non-residents in the local community. In addition, regulations may need to be reviewed to facilitate greater flexibility;
- the use, recruitment and training of volunteers. It is recognised that volunteers are an under-used resource. There is an incorrect assumption by some that volunteers and unpaid carers are prevented from 'working' in a service by the Care Inspectorate. As such, new protocols and toolkit materials should be developed to combat these misperceptions;
- further work should be undertaken to establish the regulatory implications of moving to a tenancy based model within some care homes - this might be explored through a pilot; and
- the implementation strategy being developed on the back of the Task Force report must be linked to the review of the National Care Standards to ensure that the reforms being recommended here are supported in the new standards.
Contact
Email: George Whitton