A realist evaluation of the enhanced health visiting service in NHS Ayrshire and Arran
An evaluation of the NHS Ayrshire and Arran enhanced health visiting service. The evaluation aimed to understand how the service works for both parents and health visitors with a view to informing the implementation and evaluation of an increased health visiting service in Scotland.
Appendices
Appendix 1. Sample and recruitment
Phase 1. Identifying the programme theory/logic model (linking activities and outcomes)
All eight key stakeholders were given information about the study. A member of the research team contacted them to arrange date and time for focus group. Signed consent form was obtained from each participant before the start of focus group.
Phase 2. Testing the programme theory (does the programme works as anticipated?)
Potential participants (health visitors and parents) were recruited via an administrator at Ayrshire central hospital who has no direct job responsibilities to either health visitors or parents. Participants were sent information pack containing an invitation letter, participant information sheet, expression of interest form and a stamped self-addressed envelope. Interested participants were asked to complete and return an expression of interest form to a member of the research team. All individuals who expressed interest to take part in the evaluation met the inclusion criteria and were contacted directly to arrange a convenient date, time and venue for interview, where a consent form was obtained before interview. Parents were also given an option to participate in a telephone interview. Verbal consent were obtained from those who took part in telephone interviews. Interviews were audio recorded. All parents received £15 high street store vouchers.
Appendix 2. Data collection for phases 1 and 2
Phase 1
The focus group explored key stakeholders accounts of the purpose and key aspects of the structured, increased home visiting programme, its implementation, how it was expected to work and its anticipated outcomes on families and health visiting practice (see appendix 3 for topic guide). Eight key stakeholders agreed to take part in focus group to discuss the activities involved in the enhanced programme and how they could be expected to link with outcomes for children, parents and health visitors. One member of the research team facilitated the focus group, whilst another member recorded the discussions according to key activities implemented and their outcomes expected on a whiteboard. This was done in addition to audio recording. After the focus group, participants reviewed and revised what was recorded on the whiteboard.
Phase 2
Interviews with health visitors focused on perceived changes in practice and their account of perceived outcomes of the programme for children and families (see appendix 4 for topic guide). Parents were asked about their perceptions and experiences of the service and how the changes have influenced them (see appendix 5 for topic guide).
Appendix 3. Topic guide - Stakeholders
- 1. What are the key changes that have been introduced to Health Visiting since April 2013?
- 2. What are the key contents that the service will provide over and above what was previously offered?
- 3. What do you think was the rationale for implementing these new changes?
- 4. What additional resources were needed to implement these changes?
- 5. How was it envisaged that the changes would make things better for:
Health visiting practice?
Children and families?
- 6. How do you think delivery of the revised universal pathway home visits by Health Visitors could improve outcomes for children and families?
- 7. How are the changes going to contribute in terms of keeping children safe and also promote their wellbeing?
- 8. What specific plans/structures have been put in place to ensure that Health Visitors improve their knowledge and awareness of community assets, care and referral pathways?
- 9. What strategies or activities were put in place before the changes were introduced?
(prompt to find out more about whether Health Visitors were trained and details about the training programme)
- 10. Could you tell me how these changes were implemented?
- 11. Were there any partners involved in planning or implementing these changes? If so, could you tell me how they were involved?
- 12. What do you think are the challenges to implementing and delivering this enhanced service?
- 13. What organisational structures do you think might act as barrier to these enhanced health visiting service?
- 14. How are you addressing them?
- 15. What do you think have been the key benefits of implementing these changes to the health visiting service in NHS Ayrshire and Arran?
- 16. What were you expecting to achieve in the short, medium and long term?
- 17. In your opinion, what would success looks like?
- 18. What other ways do you think the service can further be improved?
Appendix 4. Topic guide - health visitor
Introduction: A brief description of health visiting changes and explanation of information leaflet/consent process.
1. How is your service responding to the national drive for early intervention and prevention, to ensure that all children have the best start in life?
2. I understand that you are now delivering a structured, increased home visiting service for all families, apart from workload issues what difference has this made for:
a. Children
b. The families
c. Professional partnership working
d. You as the Health Visitor
3. What opportunities does a home visiting programme provide you with? Are there specific interventions that you are able to deliver? (prompt: in terms of assessing the child's needs and risks?)
4. Neuro-development, child development and attachment are of key importance to give children the best start in life.
a. How has your individual practice changed in response?
b. How has service delivery changed in response?
c. Do you have any other suggestions to enhance professional learning around Neuro-development, child development and attachment?
5. Has the service you provide enabled you to link to wider services such as nurseries and social work in ways that you had not previously done?
6. Can you give me some examples of interventions or supports that you have been able to access earlier for children and families due to the more frequent contacts?
7. Does the home visiting service and universal contacts allow you to:
a. Strengthen relationships with families?
b. Improve outcomes for children and families?
c. If so how?
8. Has the increased visit schedule affected other parts of your work? If so, in what ways?
9. We know that the introduction of an enhanced home visiting programme in Ayrshire has been challenging due to workload and high caseloads. However when Ayrshire has the additional 50 Health Visitors what will you be able to provide that you are currently unable to do, due to workload constraints?
10. What are the differences between assessing children in their home to a clinic setting?
11. I understand that Ayrshire Health Visitors promote a less advisory approach when working with families and moved to an individual asset and strength based way of working.
a. How do you understand the term strengths based working?
b. How has this influenced your practice?
c. What is your experience of working with families in this way?
Appendix 5. Topic guide - Parents
1. What age is your child/children?
2. How do you feel about the number of visits you have received from your HV so far?
3. Have these visits been carried out by the same Health Visitor? If not do you know why?
4. If you have other children, has your experience of having a Health Visitor changed?
5. How do you feel about the quality of visits you have received? Do you feel supported by your HV?
6. Can you tell me what support you received from your Health Visitor? (prompt: in terms of supporting you with knowledge and skills of being a parent?) Did the HV help you with issues/concerns that were important to you?
7. What support did you receive from your Health Visitor regarding feeding your child?
a. Was this enough?
b. If not, what else would have helped?
8. Do you feel that your views are always considered as part of your child's assessment?
9. Are you able to contact your Health Visitor with any concerns?
10. Has your Health Visitor helped in terms of engaging your family with other services or professionals? If so how?
11. What is the most important part of having a Health Visitor to you?
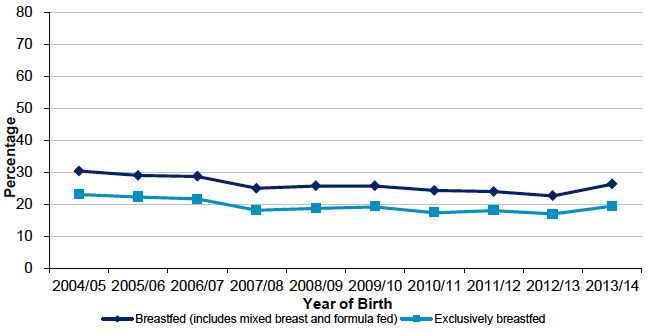
Appendix 6. Breastfeeding at the 6-8 Week in NHS Ayrshire and Arran
Appendix 7. Annual Primary Immunisation Uptake Rates in NHS Ayrshire and Arran
| 2008 | 2009 | 2010 | 2011 | 2012 | 2013 | 2014 | |
|---|---|---|---|---|---|---|---|
| Diphtheria | 97.0 | 98.4 | 97.6 | .. | .. | .. | .. |
| Tetanus | 97.0 | 98.4 | 97.6 | .. | .. | .. | .. |
| Pertussis | 96.9 | 98.4 | 97.6 | .. | .. | .. | .. |
| Polio | 97.0 | 98.3 | 97.6 | .. | .. | .. | .. |
| Hib | 96.9 | 98.3 | 97.6 | .. | .. | .. | .. |
| DTP/Pol/Hib | .. | .. | .. | 98.0 | 98.3 | 98.6 | 98.3 |
| MenC | 97.2 | 98.2 | 97.6 | 97.8 | 98.2 | 97.6 | 99.0 |
| PCV | 97.2 | 98.4 | 97.9 | 98.1 | 98.4 | 98.6 | 98.5 |
Contact
Email: Julia Egan