Realising Potential our own and others
Report from the National Allied Health Professional Mental Health LeadsGroup on Implementation of the Action Plan 2010-2011
Designing and delivering psychological interventions
Psychological therapies[11] have been defined as:
"... a range of interventions, based on psychological concepts and theory, which are designed to help people understand and make changes to their thinking, behaviour and relationships in order to relieve distress and to improve functioning. The skills and competencies required to deliver these interventions effectively are acquired through training, and maintained through clinical supervision and practice."[12]
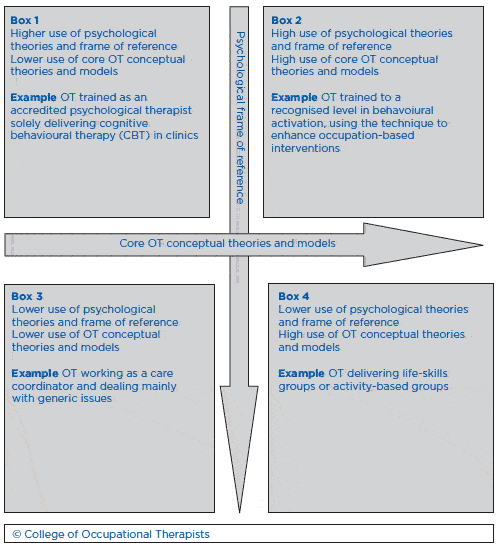
Realising Potential states that the challenge for services is to utilise the AHP staffing resources at their disposal to deliver a range of evidence-based psychological interventions and to maximise AHPs' potential to promote better outcomes for service users and carers. The challenge for AHPs, the action plan continues, is to clearly articulate their contribution to delivering psychological interventions and actively engage in local psychological forums and strategy groups, working in partnership with NHS Education for Scotland (NES) psychological therapies coordinators. An example of how occupational therapists are approaching incorporating psychological therapies and interventions into practice is shown in Fig. 1.
AHPs' core psychosocial skills are unique to each profession and vary according to undergraduate education and postgraduate development activity. AHPs nevertheless contribute significantly to the national psychological therapies agenda by enabling service users and carers to have a choice of evidence-based, non-pharmacological therapies. AHPs can work at all levels of the psychological therapies "matrix" developed by NES and the Scottish Government[13] while continuing to provide specialist AHP rehabilitation interventions to promote health and well-being, integrating recognised psychological interventions[14] into their core practice and/or directly providing a psychological therapy.[15]
Realising Potential recommended that NHS boards should ensure the delivery of evidence-based psychological interventions by appropriately trained AHPs to support rehabilitation, self-management and recovery approaches as part of local delivery strategies.
Fig. 1 The role of occupational therapists (OTs) in incorporating psychological therapies and interventions into practice
The HEAT[16] access target, "Deliver faster access to mental health services by delivering 18 weeks referral to treatment for psychological therapies from December 2014", was approved by the Scottish Government in November 2010 for inclusion in HEAT from April 2011. AHPs are playing, and will continue to play, a significant role in achieving this target by delivering skilled psychological therapies. Nationally, an AHP mental health clinical lead sits on the monitoring and implementation group for the target, and the full potential that the target and the recommendation from Realising Potential present are being explored. Locally, AHPs are building new levels of expertise and developing new service delivery approaches to providing psychological therapies.
AHPs' specific contribution to the HEAT access target is highlighted in the November 2011 issue of ISD's online Psychological Therapies HEAT Target newsletter.[17]
NHS boards are carrying out audits of personnel who are trained in psychological therapies. These are showing that NES-supported training in therapies such as cognitive behavioural therapy (CBT) and behavioural activation is being taken by AHPs across the country with a view to practitioners embedding psychological therapies in their practice as part of their everyday service delivery. Figures from NES show that 70 AHPs took training during 2010/2011.
Promoting psychological therapies with the CORE tool in NHS Grampian
A national consultation on the standardisation of outcome measures for adult psychological therapy services in Scotland revealed a majority opinion that the psychological measuring tool CORE (which stands for Clinical Outcomes in Routine Evaluation) could be the main measure across adult psychological therapy services, with other measures being used with it as clinically appropriate.
The NHS Grampian Art Psychotherapy Service began using CORE, which is recommended by the British Association of Art Therapy as the best of its type for meeting patients' needs, in May 2008.
The 34 items of CORE provide the means to conduct an immediate patient assessment, including recent history, clinical severity of problems, risk, and functioning and well-being issues. From this assessment, the service can triage for short- or long-term focused art psychotherapy interventions on an individual or group basis.
The tool captures information that allows the service to compare the effectiveness of interventions with different International Classification of Diseases (ICD−10) diagnostic categories and control for age, gender and ethnic variations. It provides feedback on which interventions work with whom, which individual art psychotherapist, interventions and techniques perform best on which clinical population, and how the service can generally improve and hone practice to achieve effective clinical outcomes.
CORE also allows a comparison of efficacy with other forms of psychotherapy and departments in Scotland and abroad. It provides NHS managers and service providers with "before and after" statistical information and contributes towards the development of an art psychotherapy research and clinical effectiveness database.
Promoting behavioural activation in NHS Lanarkshire
Psychological therapies teams in NHS Lanarkshire, working with senior management, have agreed that occupational therapists in mental health will be trained in behavioural activation (BA) therapy. The occupational therapy workforce in mental health are now working to complete the BA training package. A supervision structure will be developed to support the introduction of the BA model for community mental health teams and roll-out will be monitored by the mental health AHP clinical lead, who will track the numbers of referrals over an initial six-month period.
Promoting psychological therapies within a specialist team in NHS Greater Glasgow and Clyde
A specialist trauma service in Glasgow recognised that it needed to respond to the complex psychological needs of traumatised and socially isolated female asylum seekers and refugees. An innovative stage 1 trauma intervention was devised, led and delivered by the art psychotherapist.
The art psychotherapist's core skills in addressing the complex psychological needs of service users with traumatic experiences were developed through training in Narrative Exposure Therapy, an evidence-based intervention specifically for complex trauma cases, and a women's group based on this creative and psychodynamic approach has been established to build safety and lessen symptoms of depression and anxiety. All interventions are currently being measured using the pre- and post-intervention CORE tool.
Evaluations of service users' experiences have shown significant improvements in perceived well-being and trust. The intervention has won a national AHP innovation and health improvement award.
Contact
Email: Elaine Hunter