Quality prescribing for respiratory illness 2024 to 2027 - draft guidance: consultation
We are consulting on this draft guide which aims to optimise treatment outcomes in the management of respiratory illness. Produced by Scottish Government, NHS Scotland and Experts by Experience, it builds on the 2018 to 2021 strategy. It promotes person-centred care, the 7-Steps process for medicine reviews and shared decision-making.
Patient Information Guide - Respiratory Conditions
Who is the guide for?
This guide is for people with asthma, Chronic Obstructive Pulmonary Disease (COPD), bronchiectasis and Idiopathic Pulmonary Fibrosis (IPF). Family members, friends and carers of individuals with respiratory conditions may also find this guide helpful.
What is this Respiratory Medicine Guide about?
This guide was developed to help you make informed decisions about your respiratory medicines. It provides information on medicines used in asthma, COPD, bronchiectasis and IPF. This guide is a shortened version of the Quality Respiratory Prescribing Guide produced by Scottish Government in conjunction with Experts by Experience and experts across NHS Scotland.
This guide provides evidence and reasons for treatment whilst trying to avoid unnecessary medicines and risk of harm from medicines. It also aims to help you prepare for a respiratory review, and where relevant, provides information on how to identify the right inhaler for your needs.
What are the key issues to be aware of in respiratory conditions?
It is important for all people with respiratory conditions to have a regular review with their health care provider. This ensures that you are receiving the right treatment to best manage and control your condition.
Environmental considerations
During a review, you will be offered the opportunity to consider the environmental impact of your treatment. For example, reviewing inhalers to consider a more environmentally friendly alternative where appropriate, discussion of safe disposal or recycling (where available), and stopping unnecessary medicine to reduce medicines waste.
How are the conditions treated?
Asthma
Asthma can be treated with medicines that people breathe in through an inhaler. The medicine can be delivered as a gas or a powder.
Some inhalers have medicines that are used to help prevent and control asthma. These are called ‘preventers’ and should be used regularly, as directed. The preventer medication reduces inflammation in the airways, which relieves the symptoms of breathlessness, cough and wheeze and prevents flare ups.
Other inhalers have medicine that helps to immediately relieve the effect of an asthma attack. These are called ‘relievers’. The reliever inhaler reduces breathlessness by relaxing the muscles around the airways.
Reliever inhalers should not be used regularly. They are for use during an asthma attack or period of breathlessness. If a reliever inhaler is being used more than three times a week, it may indicate that preventer therapy needs to be reviewed.
We recommend that people should have a medication review if they are:
- prescribed more than three reliever inhalers per year
- using high strength corticosteroid inhalers
- only using a reliever inhaler
- not ordering their preventer inhalers
We recommend that people should be seen for a priority review if they are prescribed six or more reliever inhalers a year.
People taking high dose inhaled corticosteroids should be given a steroid safety card. And if the dose of inhaled corticosteroids needs to be reduced, this should be decreased by approximately 25–50% every three months.
Chronic Obstructive Pulmonary Disease (COPD)
COPD can be treated with a range of therapies, including inhaler therapy, and mucolytics. Mucolytics are medicines that make the mucus less thick and sticky and easier to cough up.
These medicines help relieve the symptoms of breathlessness. They also help reduce the frequency and severity of flare ups (exacerbations) in COPD.
Oral corticosteroids are used to treat exacerbations (flare ups) in COPD. Sometimes antibiotics, which are medicines that treat bacterial infections, will be used to treat exacerbations. Most courses are for five days to help reduce antibiotic resistance. If the infection does not clear up after the antibiotic course, a sputum (phlegm) sample may be required, to help identify the right treatment.
We recommend that people should have a review if they:
- have started taking inhaled corticosteroids
- are on mucolytic therapy
- are using multiple inhalers that could be switched to a triple therapy inhaler
- have been recently switched to a triple therapy inhaler
We recommend that stopping treatment in the following cases:
- inhaled corticosteroids should be stopped if there is insufficient response or if there are adverse effects
- mucolytic therapy should be stopped if there is no productive cough or if symptoms have not improved with use
Bronchiectasis
Bronchiectasis can be treated with mucolytics and antibiotics. Mucolytics are medicines that make the mucus less thick and sticky and easier to cough up. Antibiotics are medicines that treat bacterial infections.
These medicines help relieve the symptoms of breathlessness. They also assist with sputum (phlegm) clearance and reducing frequency and severity of bacterial infections (exacerbations).
We recommend that:
- people taking mucolytics should have a review every six months to determine how well the medicine is working
- antibiotics should be selected based on positive sputum (phlegm) cultures - if there is no positive sputum (phlegm) culture, a, broad spectrum oral antibiotic should be used to cover common respiratory pathogens
- where someone has four or more exacerbations in any 12-month period, we recommend that a specialist considers treatment with azithromycin 250mg, three times a week
Idiopathic pulmonary fibrosis
Idiopathic pulmonary fibrosis (IPF) can be treated with antifibrotics. Antifibrotics can help to slow down the build-up of scar tissue in the lungs. These medicines relieve symptoms of breathlessness and cough. They also preserve lung function whilst minimising side effects.
We recommend that antifibrotics should only be prescribed:
- by a clinician with experience of treating IPF
- when there is confirmed fibrotic lung disease with evidence of physiological progression
How will your treatment be monitored?
Healthcare professionals will determine how well treatment is working by monitoring:
- symptoms, such as how often a person gets breathless, has a wheeze or has a cough
- how often a person uses their reliever inhaler
- ability to take part in physical activity with minimal symptoms (asthma)
- lung function, through peak flow monitoring and spirometry
- levels of blood oxygen at rest and when mobile, using an oxygen saturation monitor
If you are being treated with long term azithromycin (an antibiotic), side effects are monitored using echocardiogram (ECG), hearing tests and liver function tests.
Are there any unwanted effects of treatment?
Sometimes medicines that treat illness or manage symptoms also have unwanted side effects.
Using a reliever inhaler often can cause a fine tremor (shaking), that you might notice in your hands. This may be a sign that preventer treatment needs to be changed or restarted.
Using inhaled corticosteroids too often or incorrectly can lead to increased risk of:
- oral thrush - this can be reduced by improving inhaler technique and using a spacer with an inhaler
- pneumonia – the risk versus the benefit of treatment can be discussed with a healthcare provider
- adrenal insufficiency (not producing enough cortisol) - this is associated with high doses of corticosteroids
- osteoporosis – this can be reduced by using minimum corticosteroid doses and there are actions that can improve bone health
Using anti-muscarinic antagonist inhalers (for example, ipratropium, tiotropium, glycopyrronium, aclidinium and umeclidinium) can cause people to experience dry mouth.
When using long term antibiotics, there is a risk of drug-drug interactions. Medication should be reviewed to reduce the likelihood of these side effects.
The anti-fibrotics used to treat IPF can cause lots of different side effects. These include: liver damage, diarrhoea, nausea, abdominal pain, weight loss and decreased appetite indigestion, photosensitivity and rashes. People on these medicines should have their blood tested and monitored regularly.
If you are taking high dose corticosteroids, you should be given a steroid treatment card. The card records the dose of steroids and should be shown to anyone providing treatment, for example a doctor or dentist (see figure 1).

In addition, there is a steroid emergency card which highlights the risks of adrenal insufficiency and how to treat them (see figure 2).

If you feel you might need a steroid treatment card or emergency card, please contact your health care provider for advice.
How will your treatment be reviewed?
All people with respiratory conditions should have a medicine review every year to make sure treatment is still appropriate. A healthcare provider might recommend reviewing medicines more often if medication has been changed, if symptoms are getting worse, or if symptoms are happening more often.
People with asthma and COPD may benefit from a personalised self-management plan. The plan should be discussed and agreed with your healthcare professional who reviews your asthma. This could be your nurse, GP or pharmacist. A plan provides guidance for how often reviews should take place and when to seek help beyond regular reviews.
What guidance is available for specific groups?
Rescue packs of oral corticosteroids and antibiotics may be issued to some people at risk of frequent or severe flare ups, for example, in COPD or bronchiectasis.
Pulmonary rehabilitation may be suitable to help achieve the maximum benefit from lung function.
Sputum clearance advice is an important management tool for people with bronchiectasis. This is usually taught by a physiotherapist.
Lifestyle information
Healthcare providers will be able to offer healthy lifestyle information and advice which can help individuals manage and improve respiratory conditions. Respiratory conditions can be helped by considering the following:
- stopping smoking - there are many options available to help, such as free services at the community pharmacy or smoking cessation services
- keeping active and engaging with exercises offered at pulmonary rehabilitation classes.
- keeping vaccinations up to date (including influenza, pneumococcal, COVID-19, diphtheria, tetanus, and pertussis)
- maintaining a healthy weight, diet and alcohol intake
- attending local support groups, to help maintain lifestyle changes
The seven-steps review process
The seven-steps review process is used across Scotland when reviewing people’s medicines. The steps below will take you through the journey and the treatment of your respiratory condition.
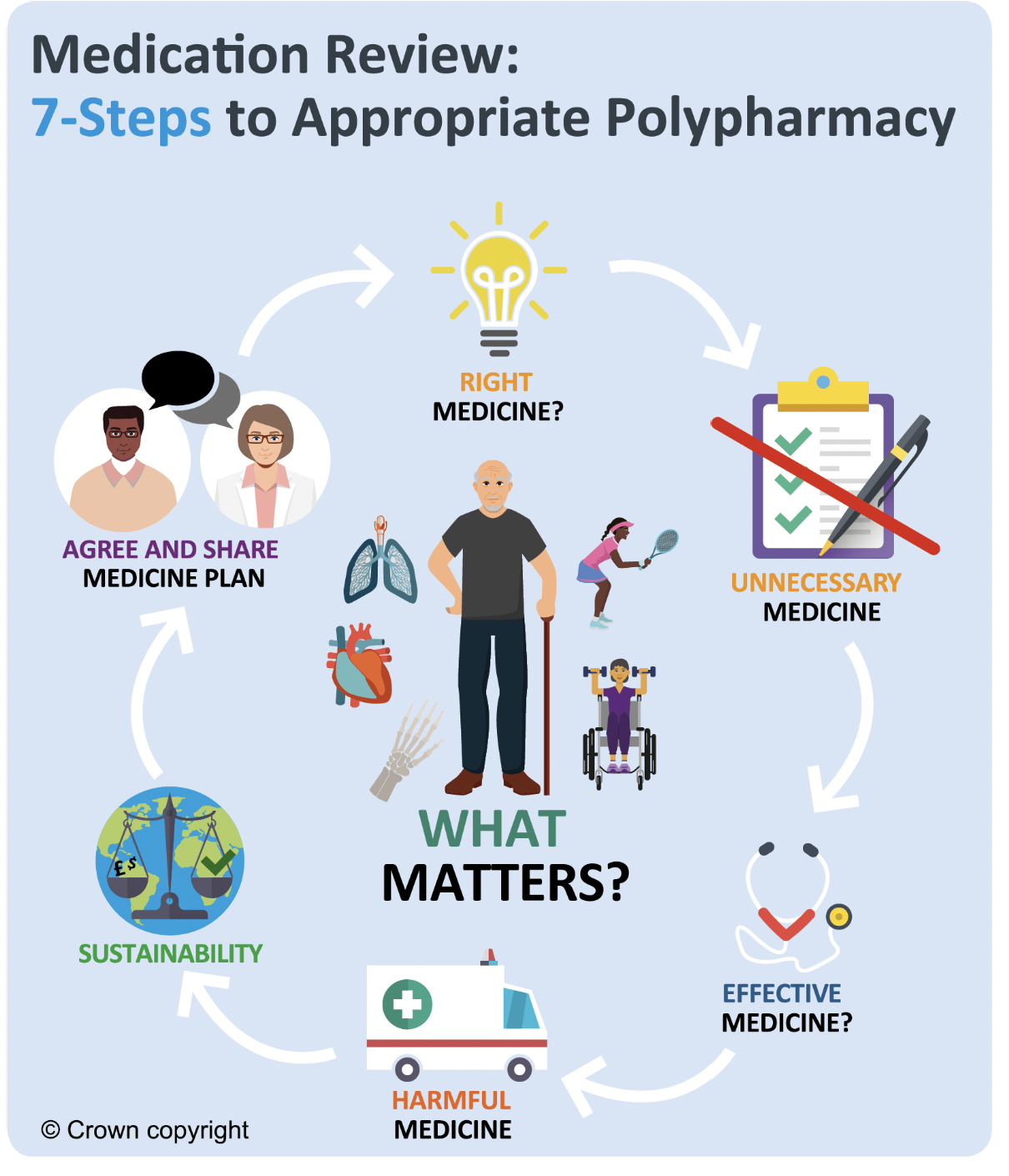
Where can people with respiratory illness find out more information?
Table 1 – Information Resources
Resource
NHS Inform NHS inform has information on the symptoms, causes and treatment for a range of respiratory illnesses.
My Lungs My Life
My Lungs My Life is a comprehensive, free website for anyone living with COPD, asthma or for parents/guardians of children with asthma. The resource is a collaboration between NHS, third sector and the University of Edinburgh.
Don’t Waste a Breath
The Don’t Waste a Breath website, developed by NHS Grampian, provides information for patients on inhaler technique and how to recycle inhalers. This website complements My Lungs My Life.
Charity Resources The Chest Heart and Stroke Scotland and Asthma + Lung UK | Asthma home have lots of information to support patients including patient leaflets, booklets and toolkits and both have a patient helpline providing advice
Personal Asthma Action Plans
There is substantial evidence to support the value of personalised actions plans for asthma in both adults and children. Access a generic template from Asthma + Lung UK.
Respondent Information Form
The Respondent Information Form can be found within the supporting documents section of this publications.
Contact
Email: EPandT@gov.scot