Public Bodies (Joint Working) Scotland Bill: Business and Regulatory Impact Assessment
An assessment of the business and regulatory impacts of the Public Bodies (Joint Working) (Scotland) Bill.
Options
(1) Do nothing
The integration of adult health and social care will be primary legislation and as such partners will not have the option to do nothing. The current model of commissioning services is not delivering the best possible care for those who need it, and against projected demographic trends, will be unsustainable in terms of finance and institutional capacity. The costs for health and social care in Scotland for all ages are expected to rise by £2.5 billion per annum over the next 20 years. If the delivery of services remain unchanged we will require yearly real increases of 1.25% and 2.7% to NHS and local authority budgets respectively.
- The options presented will provide a framework for the commissioning of care services that are more suited to individual needs and will better balance the demand on resources between institutional and community based care.
- Community Health Partnerships have been perceived in some areas by GPs and other professionals as having limited devolved decision-making power for limiting their opportunities to play an active role in local service planning and provision. There has also been frustration that some Community Health Partnerships pushed upwards to the parent Health Board and with little influence in particular over acute budgets. The Bill will address those concerns, by requiring locality planning arrangements to be developed and implemented in integration authorities.
- The Bill will place a duty on Health Boards and local authorities to fully involve local professionals, across extended multi-disciplinary health and social care teams and the third and independent sectors, on how best to put in place local arrangements for planning service provision, at the level between partnerships and individual GP practices. Having consulted, integration authorities will be required to put in place, and to subsequently support, review and maintain such arrangements.
(2) Adopt one of two models of integration
Background
The Bill establishes integration authorities and removes Community Health Partnership committees from the statute book. Health Boards and local authorities will jointly be required to set up an integration authority. Each integration authority will cover at least, a single local authority area.
Partnerships may choose not to integrate the budgets for other services along with adult health and social care, in which case the governance for other services might be provided by another Committee arrangement. Other options for the ongoing management of Community Health Partnership responsibilities are also possible. The Bill provides flexibility for the governance and delivery arrangements, and other areas which are currently Community Health Partnership functions, to be left to Health Boards and local authorities to determine. Secondary legislation will provide for the range of functions to be included and those not included in the integrated partnership arrangements.
The Bill requires integration authorities to put in place arrangements for locality planning that will inform the development and assist in the delivery of locally agreed strategic plans and that have the support of the professionals and other care providers who will deliver services.
Our aim is to create a system of health and social care where budgets can be used to best support the individual at the most appropriate point in the system, regardless of whether it is health or social care support that is required.
The Bill describes two options via which Health Boards and local authorities will integrate budgets to achieve this aim. Under these arrangements, integration authorities will be free to choose which approach they take to integrate budgets. Where partners fail to agree a model of integration, Ministers may direct the approach to be taken by the integration authority. Under each option, an integration plan will establish the nature and scope of the integration authority. Staff could move between employers to support a shift in functions, if there is local agreement to such a change.
The impact of these options on businesses is likely to be the same regardless of which option is implemented, as the partnership will be required to have an integrated budget and achieve the same outcomes within either option. It will be a decision made as a result of the implementation of the strategic plan which must be prepared under both models of integration, which may result in impacts on providers of health and social care services.
Option 1: Delegation between partners model
For the delegation between partners option, the local authority and the Health Board delegate functions either from 'one to the other' or 'to each other'. The delegator will be required to facilitate the allocation and delegation of financial budget for provision of delegated functions from their own organisation's budget to allow the other organisation to provide the services required under the function.
An integration plan between the Health Board and the local authority establishes the functions and resources to be delegated between the partners. The Health Board and local authority will jointly establish a committee to oversee the delivery of the integration plan and thus the provision of integrated services. This model requires the integration authority to formulate a strategic plan to describe which services are to be provided by which body and the money available to provide such services.
Where one organisation delegates its functions to the other, the other organisation provides the services necessary to deliver the function. The Chief Executive of the 'lead agency' would then be accountable through the integration joint monitoring committee to both partner organisations for the satisfactory delivery of the strategic plan.
Option 2: Delegation to a corporate body model
This model requires the Health Board and local authority to delegate agreed functions to the integration authority, which would be established as a body corporate of the Health Board and local authority. The Health Board and local authority agree the outcomes to be delivered and the amount of resources to be committed by each partner to the integrated budget for delivery of services, to support the functions delegated to the partnership.
The new corporate body becomes responsible for delivering the services, with the Board of the integration authority managing and directing the delivery of the services required to achieve the functions that have been delegated. A chief officer will be appointed to develop and implement the strategic plan. The integrated budget would be managed on behalf of the integration authority by the chief officer, whose authority and accountability in relation to delivery of the partnership's delegated functions will be determined by his or her statutory functions. The integrated budget would consist of the respective contributions from each partner organisation, each managed by the chief officer and subject to the respective financial governance arrangements of each partner.
An integration plan will establish the terms of the arrangement between the Health Board and the local authority, and arrangements for partners to transfer resource between the two budgets at the discretion of the chief officer. Each delegating partner would retain their legislative responsibility for the functions that had been delegated to the integration authority.
Sectors and groups affected
The groups that we anticipate will be affected by the Bill are:
- Clinical/professional/support health and social care workforce;
- Carers;
- Service users;
- Health and social care providers (NHS, local authority and independent e.g. care homes);
- Statutory bodies; and
- Third and independent sectors.
We believe the biggest impact will be among care home providers and care at home providers, as a more 'joined up' approach to identifying care for individuals is likely to mean a shift away from institutional care being the preferred solution to a person's care needs.
Benefits to business
The main objectives behind both options are twofold: first, to achieve better outcomes for service users; and second, to address the pressures created by the projected demographic change in Scotland. In addressing these objectives, the Scottish Government is aiming to manage fiscal pressures (see figure 1), by delivering a more effective and cohesive service, and better meet the needs of individuals in the system. This will, in turn, benefit health and social care providers by providing increased opportunities to provide care in the home and community setting. This should also ease pressure on the resources of care homes for older people and hospitals, allowing them to devote more time to people who need the most care and attention.
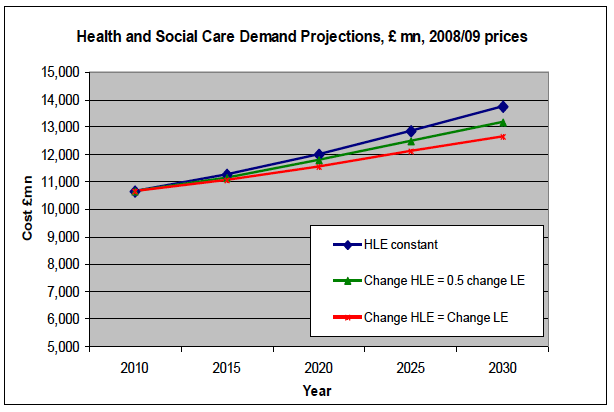
Figure 1: Graph showing the projected increase in costs for social care up to 2030 for three variables. The dark blue line shows the increase in cost assuming that the healthy life expectancy doesn't change i.e. people are healthy until, say, 68 and live until 70 now; and the line projects people who are healthy until 68 but live until, say, 75. The green and red lines show variations of the above idea, with the ideal situation being the red line: healthy life expectancy increases as does life expectancy to give the same time in the 'unhealthy' bracket. This still indicates that the projected increase in costs will be untenable. HLE= healthy life expectancy; LE= life expectancy.
Produced by Scottish Government, Analytical Services Division (Health)
Costs
The cost implications and the potential benefits arising from the models of integration permissible under the Bill are detailed in the Financial Memorandum published alongside the Bill.
Potential costs
We have identified the following areas which we expect will have potential costs or potential savings/benefits as a result of implementing the policy. It is important to note that businesses will be affected to differing degrees across Scotland dependent on the demographics of the area covered by the integration authority, but also in terms of the geography. An integration authority in the Highlands, for example, will face a different set of challenges to their counterparts in Glasgow and Edinburgh. Furthermore, no two individuals' care requirements are exactly the same, and will have different sets of care needs. It is therefore difficult to give meaningful estimates of potential costs and benefits, and any financial estimates should be received with the above caveats in mind. However, the areas in which we anticipate there to be cost implications are:
- Provision of more health and social care in communities, specifically care at home and care home services, pharmacy and community services;
- Costs associated with enabling GPs to participate in locality planning, for example the time spent away from the surgery to attend planning meetings will result in less patients being seen or could require a locum GP to back-fill;
- Costs associated with information technology and data sharing;
- Training and workforce development costs, including up-skilling staff to understand the commissioning process. This may not require attendance at a course, for example, but will require staff having time away from their jobs; and
- Operational environment for providers of health and social care services with respect to the commissioning of services, funding through the integrated budget arrangements and potential impact on demand, price and contractual arrangements.
Potential benefits
Dependent on the geographical area, strength of the partnership and demographics, there could be potential benefits and savings in the following areas:
- Reduction in rates of acute bed use, and length of stay, as care moves into communities and anticipatory services are improved, particularly for the frail elderly population;
- Efficiency savings arise from better understanding of activity, unit costs and reduced variation;
- Savings from reduced cost shunting e.g. reduced delayed discharges;
- Cost savings from potential reduction in number of committees and the requirement to have fewer integration authority than current numbers of Community Health Partnerships;
- Opportunity for businesses to work collaboratively across sectors, form strong relationships, reshape and redefine workforce roles and reduce duplication; and
- Efficiencies achieved through joint working and commissioning.
In addition, with the shift in the balance of care from institutional to community based care, it is likely that the amount of commissioned social care will increase and therefore the spend will shift from institutional to anticipatory and preventative measures. This will have an impact for the third and independent sectors, social work and local community health services, in particular GP practices.
Contact
Email: Gill Scott
There is a problem
Thanks for your feedback