Organ and tissue donation and transplantation: consultation
This consultation seeks views on increasing the number of deceased organ donation and tissue donors in Scotland.
Chapter 2 - Increasing Numbers of People considered as Potential Organ and Tissue Donors
Introduction
It is already accepted that, as part of good end-of-life care, everybody should have the option to be a donor, particularly if they have expressed a wish to do so. This is both for the wider public good by helping deliver much-needed transplants, but also as it can, in time, help grieving families to know that something positive has come from the tragic loss of their loved one.
The number of referrals to the Special Nurses for Organ Donation ( SNODs) has increased by 85% since 2011/12, despite a decline in numbers of people dying in circumstances where they could be organ donors. Therefore progress is already being made in identifying potential opportunities for donation. However, there are still some potential donors who are missed each year because the clinical teams caring for the patient do not consider donation and do not contact a SNOD or Tissue Donor Co-ordinator ( TDC), mainly for patients who die after circulatory death.
Figure 6 - proportion of total cases which met existing referral criteria that were referred to Specialist Nurses for Organ Donation - 2015-16
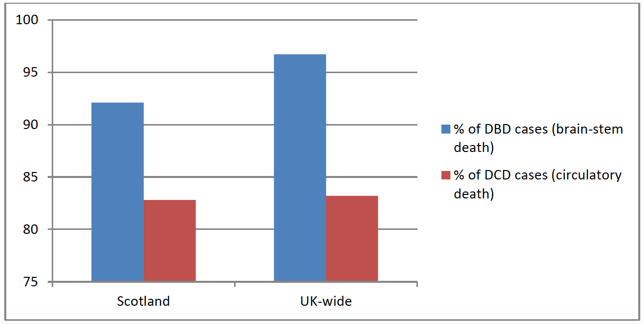
Figure 6 above shows that 17% of potential DCD patients in Scotland were not referred to the SNODs in 2015-16 - some of those patients were on the Organ Donor Register ( ODR). While Scotland's performance is not significantly lower than the UK average, there is still scope for improvement as around 20 referrals of potential donors are being missed each year. Meanwhile, for tissue donation, while there are fairly good referral rates from some hospital units, many patients who could be tissue donors are not referred by the relevant hospital departments.
In some cases, this lack of referral was due to an oversight by clinical staff who had not thought about donation - for tissue donation this seems to be common due to lack of awareness of the possibility of tissue donation, as well as, for example, staff in areas such as Emergency Departments feeling they are too busy to refer a patient. Further, in some cases, even though the patient met the current criteria for referral for donation, clinicians seem to have assumed the patient would not be a suitable donor. This is either because of health issues which may make the patient's organs/tissue unsuitable for transplantation or because the clinicians thought that the length of time between withdrawing treatment and the patient's death would be likely to mean the patient's organs would not be viable for transplantation. Organ or tissue donation should be considered in every case where the patient does not have any 'absolute' contraindication to donation i.e. where they definitely could not donate any of their organs [16] or tissue - for example if the patient was over a certain age (currently organs cannot be donated from those who are 85 years old or over, although it may be possible to donate corneas from patients who are older) or has certain 'live' cancers. For most patients, it may often be possible for at least some organs or tissue to be donated.
Hospital doctors may sometimes have concerns that the patient's health problems might be such as to make a particular patient unsuitable to be an organ/tissue donor. However, clinicians who are not dealing with organ/tissue transplantation on a daily basis are not necessarily experts in determining whether there are any contraindications to organ or tissue donation. It is the staff who deal with organ and tissue donation and transplantation on a daily basis who are the experts in this field and the ones who can best advise whether or not organs and/or tissue from a particular patient would be suitable for transplantation. Therefore, it is always best for the patient's case to be referred to the SNODs or TDCs early on to investigate if donation is possible, even if the doctor caring for the patient thinks it is unlikely. In some cases, the patient will indeed not be suitable for donation and he/she will be quickly ruled out after a telephone conversation with the SNOD or TDC; in other cases however, the patient may be able to successfully donate.
A limited system has been implemented in Scotland where the relevant Regional Clinical Lead for Organ Donation will require an NHS Board's donation committee (which is there to help support donation in their area) to investigate and provide an explanation, especially if a person who was pronounced brain-stem dead in an intensive care unit and was on the ODR was not referred to a SNOD.
Proposals to reduce numbers of missed referrals
If all patients in critical care areas were referred either at the point a doctor decides to carry out brain-stem death testing (for potential donation after brain-stem death ( DBD) cases) or at the point the doctor documents the decision to withdraw treatment (for potential donation after circulatory death ( DCD) cases) this would be likely to increase the number of organ donation referrals in Scotland by around 20-30 each year. We would consider whether the guidance should provide specific clinical triggers which should lead to an organ donation referral [17] . While not all of these patients would become actual donors, a proportion of them should do. For tissue donation, doctors should also refer patients who die outwith Critical Care Units as tissue donation can still take place up to 48 hours after the patient has died (or up to 24 hours in the case of eye donation) [18] .
Therefore, greater encouragement should be given to all hospital doctors to refer any patient for consideration as an organ and/or tissue donor if they are expected to die in a critical care area and are under the age of 85, with other parts of hospitals also encouraged to refer those who have recently died for consideration as a potential tissue donor. Greater awareness raising of organ and tissue donation and the role of SNODs and TDCs among staff working across hospitals could be helpful in making staff who have never or rarely been involved in donation more aware of the advice and support that SNODs or TDCs can provide. While some staff working in Intensive Care Units will be very familiar with organ donation, others in Emergency Departments may be much less familiar with it. Similarly, staff in other hospital departments are not always aware of the potential for tissue donation.
When a patient is referred to the donation service, the local SNOD or TDC will discuss the patient's key health issues with the clinician by telephone to decide if any absolute contraindications to donation apply and to check whether the patient had either opted in or opted out on the ODR. If there are any health concerns which might prevent a particular organ/tissue being donated, the SNOD or TDC would speak to transplantation medical staff to get their view on whether or not the organ(s) or tissue could be transplanted.
To help encourage further increases in referrals, the Chief Medical Officer ( CMO) could for example issue guidance to hospitals to encourage them to refer all patients who meet the criteria above - either as a potential organ or tissue donor. As SNODs and TDCs work closely together, staff would only need to refer a patient to one or other, not both. In cases where this did not happen and the patient was on the ODR, there may be a case in some circumstances for the Regional Clinical Lead for Organ Donation asking the relevant hospital to investigate the circumstances. That would help those hospitals to learn lessons for the future and address any issues identified locally, such as around lack of awareness of organ and tissue donation or misunderstandings about what constitutes a contraindication to donation.
The CMO's guidance could also re-emphasise the importance of all hospital staff doing what they can to facilitate donation, stress that SNODs and TDCs are there to support hospital staff, and encourage clinicians to always involve SNODs or TDCs in approaches made to families about donation. On average in 2015-16, SNODs were involved by doctors in only 69% of approaches to families in Scotland, although involvement rates improved during the second half of the year (across the UK they were involved in 83% of cases). Authorisation rates are significantly higher where a SNOD is involved in the approach discussions with the family.
The proposed CMO guidance has advantages in that it can be implemented relatively quickly and encourages all potential donors to be fully considered, even if it is later agreed that the person would not be a suitable donor for medical or other reasons. Some clinicians may have concerns that it could put additional work pressure on them and other NHS staff and lead to difficult discussions with families. However, given that these proposals would only be expected to lead to around 20 to 30 extra cases each year across Scotland where families would be approached about organ donation, it is unlikely to place individual departments under significant extra pressure. There would also be a likelihood of some extra approaches to families about donating tissue only (where the patient has been ruled out as a potential organ donor), but these would all be carried out by the TDCs. It is worth noting that, for example, the North West region of England already has a 'required referral' policy for hospitals - evidence from the operation of this policy could be considered in developing any new CMO guidance.
Strengthened guidance on referrals should help generate greater awareness and lead to more referrals to the donation service. It would reduce the risk of referrals being missed due to an oversight and some of these patients could reasonably be expected to become donors. It would also promote consistency in practice across NHS Boards and promote equity in the approach taken across Scotland. For those patients who are on the ODR, referral helps to ensure that attempts are made to see if their wish to be a donor can be taken forward. Where the person cannot be an organ donor for medical reasons, the referral may still help enable them to be a tissue donor instead.
Question 16 - what do you think about providing CMO guidance to encourage clinicians to refer almost all dying or recently deceased patients - particularly those who are under 85 years old - for consideration as a potential organ or tissue donor?
Question 17 - what do you think about making it a procedural requirement for clinicians to involve a specialist nurse for organ donation, tissue donor co-ordinator or another individual with appropriate training in approaches to families about donation, wherever that is feasible?