NHSScotland Chief Executive's Annual Report 2011/12
The NHSScotland Chief Executive's Annual Report 2011/12 presents an assessment of the performance of NHSScotland in 2011/12 and describes key achievements and outcomes.
CHAPTER 3 KEY ACHIEVEMENTS IN HEALTHCARE QUALITY
In the Quality Strategy, we have established three Quality Ambitions that provide the focus for prioritising and integrating activity across NHSScotland, in partnership with the rest of the public sector, the third sector, and with the people of Scotland. In this chapter, we consider healthcare quality achievements and progress during 2011/12 in terms of their relevance to each of the three Quality Ambitions.
Of course, work undertaken will often simultaneously improve safe, effective and person-centred care, however, for the purposes of this report, we have separated out the work under the most relevant Quality Ambition.
QUALITY AMBITION
SAFE
There will be no avoidable injury or harm to people from healthcare they receive, and an appropriate, clean and safe environment will be provided for the delivery of healthcare services at all times.
NHSScotland has received international acclaim for its approach to implementing improvements in patient safety. We have established a shared Quality Ambition for no avoidable injury or harm across all aspects of healthcare services.
During 2011/12, there was further evidence of the success of the Scottish Patient Safety Programme with a reduction in Hospital Standardised Mortality Ratios (HSMR), and work began to bring additional areas into the acute programme, including interventions to reduce sepsis and venous thromboembolism. The Programme was extended to Paediatrics and Primary Care and work has been taken forward to extend its focus into mental health and maternity services. There were further improvements in tackling Healthcare Associated Infection (HAI) with reductions in the prevalence of infections including Clostridium difficile and cases of Methicillin-resistant Staphylococcus aureus (MRSA) are at the lowest level since recording began.
PATIENTS AND THE PUBLIC
THE SCOTTISH PATIENT SAFETY PROGRAMME
The Scottish Patient Safety Programme (SPSP) is playing a significant role in delivering the Quality Ambition of no avoidable injury or harm to people from the healthcare they receive. Its key objectives are to reduce Healthcare Associated Infection (HAI), reduce adverse surgical incidents, reduce adverse drug events, improve critical care outcomes and improve organisational and leadership culture on safety. Its primary aim is to reduce Hospital Standardised Mortality Ratios by 15 per cent and adverse events in Scotland's acute hospitals by the end of 2012. The most recent Hospital Standardised Mortality Ratio (HSMR) statistics, which include data to March 2012, shows a reduction of 10.6 per cent since December 2007 as set out in Chart 8 below.
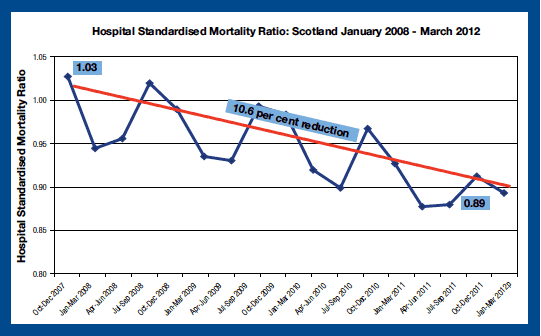
Source: NHS Information Services Division (ISD): Quarterly HMSR[9]
Broadly, over the same period, mortality in Intensive Care Units fell by 20 per cent as demonstrated in Chart 9.
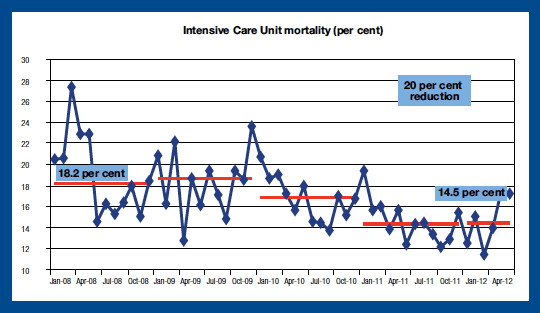
Source: NHS Information Services Division and Scottish Patient Safety Programme Extranet [10]
One of the interventions of the Scottish Patient Safety Programme has been the reliable introduction of the surgical checklist. This is an evidence-based intervention known to improve outcomes and mortality after surgery. Along with a range of other programmes and interventions, this has contributed to a significant reduction in surgical mortality. Following a period of relative stability in the percentage of postoperative mortality, there has been a drop of 19.5 per cent since 2008/09 as illustrated in Chart 10.

Source: NHS Information Services Division: SMRO1[11]
New elements have also been brought to the programme this year, including the three-year sepsis and venous thromboembolism (VTE) collaborative which was launched in January 2012. The sepsis intervention aims are a 5 per cent reduction in mortality from sepsis in pilot areas by 2012 and a 10 per cent reduction by December 2014. In relation to VTE management, the aim is to achieve 80 per cent reliability with thromboprophylaxis by December 2012 and to 95 per cent by December 2014.
We have also announced a three-year extension of the acute programme which will begin in January 2013. It looks to learn from our experience over the last five years, build on the successes demonstrated by the first phase of the project and continue to drive forward improvements in patient safety. It sets ambitious new goals by increasing our aim of reducing Hospital Standardised Mortality Ratios in acute hospitals from 15 per cent to 20 per cent, and achieving 95 per cent of care free from avoidable harm as listed in a Scottish Safety Index.
KEY RESULTS FOR PATIENT SAFETY
Considerable progress has been made at NHS Board level as we continue to work towards achieving the key aims of the Scottish Patient Safety Programme. Board-reported achievements of the Programme across NHSScotland (covering 1 April 2011 to 31 March 2012 compared to the baseline) include:
- NHS Ayrshire and Arran - An Emergency Response Team has been established at both Ayr and Crosshouse Hospitals to identify patients at risk to enable earlier intervention. Up to January 2012, NHS Ayrshire and Arran reports that it has had no central line blood stream infections in critical care for 776 days.
- NHS Dumfries and Galloway - The Board reports that, in Intensive Care Units, it has had no cases of Clostridium difficile since January 2009, and no cases of Staphylococcus aureus bacteremia since March 2010. It also reports that surgical site infections have reduced by 72 per cent within Dumfries and Galloway Royal Infirmary Orthopaedics Department between 2007-2011.
- NHS Fife - The Board reports that surgical briefing/pause is now being carried out in all specialties across NHS Fife. The endoscopy Units at Victoria Hospital and Queen Margaret Hospital have sustained 95-100 per cent compliance. Surgical pause is a standardised way for surgical teams to make a set of final checks before starting surgery to ensure safety.
- NHS Forth Valley - As of January 2012, NHS Forth Valley report that its pilot critical care ward has achieved 606 days since its last Ventilator Associated Pneumonia incident.
- NHS Grampian - The Board reports that all theatre teams at the Royal Aberdeen Children's Hospital are demonstrating 100 per cent compliance with the surgical briefing/pause for six months, with general surgery compliance at 100 per cent for 14 months.
- NHS Highland - In Intensive Care Units, the Board has achieved 697 days between Ventilator Associated Pneumonia incidents and 573 days since its last central line infection. This has led to improved patient care, better staff morale and a reduction in the average length of stay.
- National Waiting Times Centre Board - The Golden Jubilee National Hospital has achieved 95 per cent or above compliance in medicines reconciliation for all orthopaedic patients over the last seven months.
- NHS Lanarkshire - Crash calls (sudden and often unexpected deterioration in a patient's condition requiring a very fast response to save their life) have been reduced in Monklands District General Hospital in general surgery from 27 in November 2009 to 16 in November 2011. The Board also reports that there has been a significant improvement in reducing surgical site infections across all three acute hospitals. Safety briefings are being conducted in 59 general ward areas in the three acute hospitals.
- NHS Lothian - The Board has maintained a 42 per cent reduction in adverse events and continues to sustain a reduction in crash calls at Edinburgh Royal Infirmary.
- NHS Orkney - Will start to implement its Harm and Mortality Reduction Plan, which is a single document pulling together work from the Scottish Patient Safety Programme, case note reviews and samples identified from quarterly Hospital Standardised Mortality Ratio (HSMR) data. This will allow the Board to align all its safety and improvement work to the aims of the Scottish Patient Safety Programme.
- NHS Tayside - The Board reported that there have been no new central line infections since the opening of its Medical High Dependency Unit in Ninewells Hospital in 2007. Perth Royal Infirmary has reduced its crash call rates against the baseline median by 25 per cent.
HEALTHCARE ASSOCIATED INFECTION
The results of Health Protection Scotland's (HPS) second national Scottish Point Prevalence Survey of Healthcare Associated Infection (HAI) and Antimicrobial Prescribing* were published on 4 April 2012. The survey recorded a snapshot of all types of infections on the day of the survey. It found that prevalence of HAIs was 4.9 per cent in acute hospitals and 2.5 per cent in non-acute hospitals - lower by a third compared to that found in the first Scottish survey (carried out in 2005/06). A markedly lower prevalence of gastrointestinal prevalence and in particular Clostridium difficile infection was found. The report notes that the lower prevalence and changing epidemiology of HAI since the last survey are associated with implementation of the national programme of targeted interventions in the intervening period. The 4.9 per cent prevalence figure compares well with the corresponding figure of 6.4 per cent in England.
CLOSTRIDIUM DIFFICILE AMONG THE OVER 65s
One of the HEAT targets on Healthcare Associated Infection (HAI) is that by March 2013 NHSScotland's rate of Clostridium difficile infections in patients aged 65 and over is 0.39 cases or less per 1,000 total occupied bed days. Figures from Health Protection Scotland confirm that for the year ending June 2012, the rate across NHSScotland was 0.30. The rate of Clostridium difficile infections in over 65s has decreased by 78 per cent from 1.32 cases per 1,000 occupied bed days in 2007/08 to 0.30 cases in the year ending June 2012.
STAPHYLOCOCCUS AUREUS BACTERAEMIA (INCLUDING MRSA)
Cases of Methicillin-resistant Staphylococcus aureus (MRSA) are at the lowest level since recording began. One of the Healthcare Associated Infection HEAT targets is that by March 2013 NHSScotland's cases of Staphylococcus aureus bacteraemia (including MRSA) cases are 0.26 or less per 1,000 acute occupied bed days. Figures from Health Protection Scotland (HPS) confirm that for the year ending June 2012, the rate across NHSScotland was 0.30 cases per 1,000 acute occupied bed days. This represents a decrease of 35 per cent from 2007/08, when there were 0.47 cases per 1,000 acute occupied bed days.
HEAT TARGET
Further reduce Healthcare Associated Infections so that by March 2013 NHS Boards' Staphylococcus aureus bacteraemia (including MRSA) cases are 0.26 or less per 1,000 acute occupied bed days; and the rate of Clostridium difficile infections in patients aged 65 and over is 0.39 cases or less per 1,000 total occupied bed days.
During 2011/12, NHSScotland made further progress towards the 2012/13 HEAT target to reduce the level of Healthcare Associated Infection.
In terms of Staphylococcus aureus bacteraemia (including MRSA), the target is to achieve a reduction in the infection rate to 0.26 cases or less per 1,000 acute occupied bed days by March 2013. For the year ending June 2012, the rate of MRSA/MSSA cases across NHSScotland was 0.30 per 1,000 acute occupied bed days. This represents a fall of 11 per cent since 2010/11.
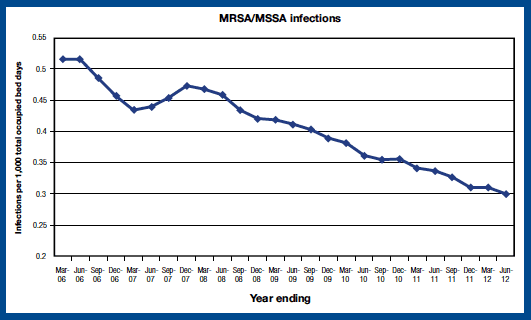
Source: Health Protection Scotland Quarterly Report on SAB (including MRSA)
In terms of Clostridium difficile infections (CDI) amongst the over 65s, the target is to achieve a reduction in the infection rate to 0.39 cases or less per 1,000 acute occupied bed days by March 2013. For the year ending June 2012, the rate of CDI cases across NHSScotland was 0.30 per 1,000 acute occupied bed days. This represents a fall of 24 per cent since 2010/11.
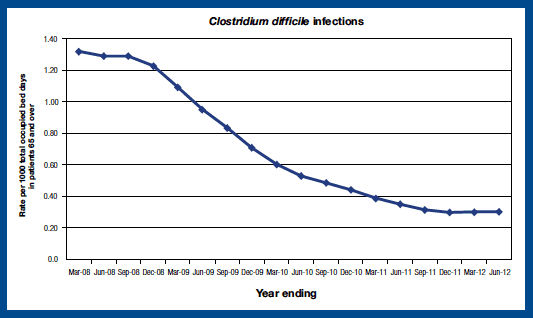
Source: Health Protection Scotland Quarterly Report on CDI
HEALTHCARE ENVIRONMENT INSPECTORATE
The Healthcare Environment Inspectorate (HEI) was established in 2009 to provide independent and rigorous scrutiny and assurance of hospitals in Scotland. The aim of this was to achieve improved performance in tackling Healthcare Associated Infections (HAI) and to ensure that patients and the public can have complete confidence in the cleanliness of hospitals and the quality and safety of services. Its initial three-year cycle of inspection meant that that all acute hospitals will have received at least one announced and one unannounced visit by September 2012. During 2011/12 the HEI conducted 32 inspections of 29 acute hospitals across 12 NHS Boards and for the first time inspected both the Scottish Ambulance Service and the State Hospitals Board for Scotland. In total, the HEI made 156 requirements and 88 recommendations[12].
ELECTRONIC TRANSFER OF PRESCRIPTIONS
The ePharmacy Programme has played a significant role in transforming how NHS pharmaceutical care is delivered in Scotland. The programme has introduced the Electronic Transfer of Prescriptions (ETP) between GP practices, Community Pharmacies and Practitioner Services Division. This has improved patient safety by reducing transcribing errors, modernised service delivery and increased the efficiency of the processing of prescriptions by removing the reliance on paper. The first live national system to fully support ETP in the UK, ePharmacy has also supported the development of a web-based pharmaceutical care planning tool - the Pharmacy Care Record (PCR). This assists pharmacists to provide pharmaceutical care for patients with long term conditions, helping to ensure they get the best outcomes from their medicines. At the end of March 2012, some 119,000 PCRs had been opened for patients, with 107,300 assessments completed and 12,640 care issues recorded.
REDUCING FALLS
A good practice self-assessment resource, Managing Falls and Fractures in Care Homes for Older People* was launched in June 2011. The resource supports care sector staff to comprehensively assess falls prevention and management, and the prevention of fractures within their care home settings. It provides: practical help and advice; gives guidance and access to resources which can be easily downloaded for use; and assists staff working in the care sector to improve falls prevention on an ongoing basis. Twenty-two per cent of homes report a reduction in falls due to the use of the resource pack. In addition, the Scottish Ambulance Service worked with its partners to develop a national care pathway framework for frail and elderly people in the community at risk of falling and suffering injury. This recognised that frail elderly fallers represent a significant proportion of unscheduled care activity. A national multi-disciplinary and multi-agency group developed a consistent framework and criteria-based screening tool to ensure direct patient access to the most appropriate care and services.
* All publications referred to within this document can be found in the publications section of the appendices.
NHS Board Story:
NHS Lothian
REDUCING HARM BY RECONCILING MEDICINES ACCURATELY ON ADMISSION TO, AND DISCHARGE FROM, AN ACUTE MEDICAL WARD IN NHS LOTHIAN†
Medication errors, within transitions of care, are potentially high risk for patients, with incorrect dosage and point of admission being associated with the most common errors.
In NHS Lothian, a team of early adopters and innovators were selected to join a multi-disciplinary group which undertook a review to reduce harm to patients by reconciling medicines accurately on admission to, and discharge from, one of their acute medical wards.
They used a model for improvement to gather data and information and to define measures and analysis. Failure Modes and Effects Analysis (FMEA) were conducted to identify the reasons for the errors and to prioritise factors with the highest risk. Process mapping was also conducted with Foundation Year Doctors to establish practices actually undertaken which resulted in a 'Gold Standard'.
As a result, the project has been successful in reconciling medications accurately with a significant reduction in errors on admission to the ward and on discharge.
A work plan has now been devised to spread changes to other areas throughout NHS Lothian.
There's evidence to show that reconciling medications accurately at points of transition can reduce the risk of harm to patients.
† This work was presented as a poster at the 2012 NHSScotland Event and won first prize in the 'Safe' poster category. To view the poster visit: www.nhsscotlandevent.com/posters/Posters-2012/
QUALITY AMBITION
EFFECTIVE
The most appropriate treatments, interventions, support and services will be provided at the right time to everyone who will benefit, and wasteful or harmful variation will be eradicated.
Many of the areas for improvement which have been prioritised over 2011/12 make a direct contribution to our Quality Ambition for more effective healthcare services. A clear focus of this activity has been to identify those improvements where there is clear and agreed evidence of clinical and cost effectiveness, and to support the spread of these practices where appropriate to ensure that unexplained and potentially wasteful or harmful variation is reduced.
Key areas of progress are set out in this section for both patients and public and for staff. They include further reductions in waiting times with NHS Boards successfully delivering the 18-weeks Referral to Treatment (RTT) target at December 2011, with more than 90 per cent of patients in Scotland now being treated in 18 weeks or less. In addition, NHSScotland achieved and sustained performance above 95 per cent against the new 62-day and 31-day cancer access targets throughout 2011 - well in advance of the delivery date of December 2011.
We are making good progress in reducing the need for emergency hospital care with reductions in emergency inpatient bed days rates for people aged 75 and over. Significant progress has been made in taking forward a world-leading programme to improve the response to, and care of, people with dementia and their families in acute general hospital settings. Following the launch of the Refreshed Framework for Maternity Care* we are taking forward the quality improvements necessary to strengthen the role of maternity services in reducing health inequalities and improving maternal and infant health.
* All publications referred to within this document can be found in the publications section of the appendices.
PATIENTS AND THE PUBLIC
WAITING TIMES
Patients tell us they want prompt access to treatment, delivered as locally as possible. Cutting waiting times improves outcomes for patients and ensures effective and efficient use of resources. There has been a complete transformation of waiting times with NHS Boards successfully delivering the 18-weeks Referral to Treatment (RTT) target at December 2011, with more than 90 per cent of patients in Scotland now being treated in 18 weeks or less. The 18 week RTT target has required NHSScotland to completely change internal systems so links are in place for each patient to be seen in the right care setting at the right time.
From October 2012, patients requiring inpatient or day case treatment will be covered by a 12-week Treatment Time Guarantee enshrined in law which will apply every day of the year. In Scotland, we have also retained the maximum waiting times for outpatient and diagnostic stage of treatment standards which completes the comprehensive package for patients. Within these maximum waiting times, patients are diagnosed and treated according to their clinical need.
During the period from April to December 2011, NHS Lothian applied periods of unavailability to some patients inappropriately, which artificially reduced the number of patients who would otherwise have been reported as breaching waiting time guarantees. That was done, in the main, by retrospectively adjusting the patient's waiting time record. The practices that were identified in NHS Lothian are completely unacceptable and we have been assured that they no longer take place.
There is no evidence that these practices are widespread. However, it is important to show that recording of waiting times data is accurate and transparent. NHS Boards have been asked to undertake a specific and detailed audit of local waiting times management and processes as part of each internal audit programme in 2012/13. Audit Scotland has agreed the remit of this audit and has also agreed to undertake a separate audit itself.
HEAT TARGET
Deliver 18-weeks RTT from 31 December 2011
The target for delivery in December 2011 was for 90 per cent of patients to wait no longer than 18 weeks from referral to treatment. In December 2011, 92.0 per cent of patients were reported as being seen within 18 weeks. Since then, NHSScotland has consistently maintained this level of performance, with 92.4 per cent of patients reported as being seen within 18 weeks during June 2012.
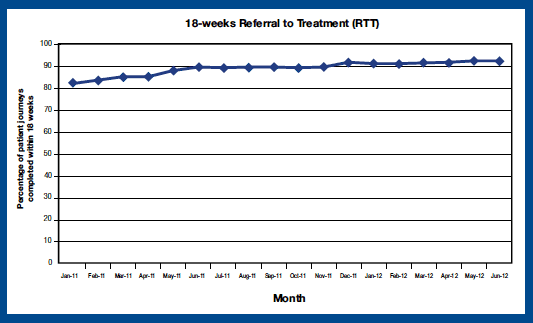
Source: NHS Information Services Division: Waiting Times Referral to Treatment
SCOTTISH AMBULANCE SERVICE
Events in 2010/11 highlighted that the rest break arrangements which were in place at that time within the Scottish Ambulance Service needed to be modernised. The Scottish Government, Scottish Ambulance Service management and staff side worked together to agree a new approach to see frontline ambulance staff work a 37.5 hour week, inclusive of rest breaks. The new approach involves additional investment in the Scottish Ambulance Service, allowing them to employ approximately 150 additional front-line staff. This will increase the resilience of the Service and help to ensure that there is no avoidable delay in ambulance response times.
REDUCTION IN DELAYED DISCHARGES
Over the past few years, NHSScotland has made significant progress in reducing the number of people inappropriately delayed in hospital for more than six weeks, with only 50 people delayed over six weeks on census night in July 2012, compared to over 2,000 people in July 2002. Following the report of the Delayed Discharge Expert Group, new ambitious delayed discharge targets were announced by the Cabinet Secretary for Health, Wellbeing and Cities Strategy in October 2011 setting out that no-one should be inappropriately delayed in hospital for more than 28 days by April 2013, and no-one should be inappropriately delayed in hospital for more than 14 days by April 2015.
The April 2012 census saw NHS Boards, along with their local authority partners, making good progress towards the new targets. At that time there were 108 patients delayed for more than four weeks, the lowest number since recording began in September 2000.
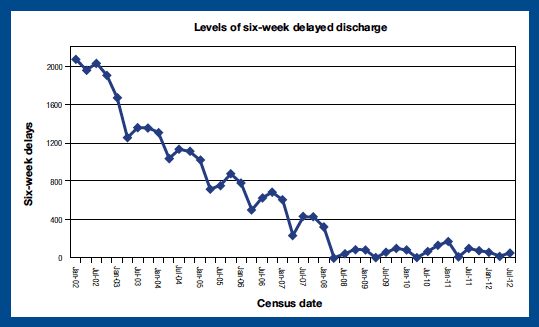
Source: NHS Information Services Division: Delayed Discharge
DEVELOPMENTS OF CANCER STRATEGIES AND INITIATIVES FOR 2011/12
The Cabinet Secretary for Health, Wellbeing and Cities Strategy launched the Detect Cancer Early Programme in February 2012, with an implementation plan that sets out the key areas for action to improve Scotland's five-year cancer survival rates. This is backed by £30 million of investment with the aim of encouraging earlier stage presentation, in the first instance for colorectal, breast and lung cancer. The National Cancer Quality Steering Group has continued to undertake an ambitious programme of work developing Quality Performance Indicators (QPIs) for all cancer types. The overarching aim of the cancer quality work programme is to ensure that activity at NHS Board level is focused on those areas that are most important in terms of improving survival and patient experience whilst reducing variance and ensuring safe, effective and person-centred cancer care. This was supported through the publication of a Chief Executive Letter (CEL): National Cancer Quality Programme (CEL 06 2012)* which set out the associated local, regional and national governance and reporting arrangements.
* All publications referred to within this document can be found in the publications section of the appendices.
CANCER WAITING TIMES
NHSScotland achieved and sustained performance above 95 per cent against the new 62-day and 31-day cancer access targets throughout 2011 - and well in advance of the delivery date of December 2011. During the last quarter, October to December 2011, 96.9 per cent of patients started treatment within 62 days of urgent referral with suspicion of cancer. Within the same period, 98.2 per cent of patients started treatment within 31 days of decision to treat, irrespective of the route of referral. When compared to the previous cancer waiting times targets in place before 2008, the changes made to waiting times standard definitions and the introduction of new cancer waiting standards has meant that the cancer treatment pathways for over 1000 additional patients are now subject to the standards to which NHS Boards must adhere.
HEAT TARGET
From the quarter ending December 2011, 95 per cent of all patients diagnosed with cancer to begin treatment within 31 days of decision to treat, and 95 per cent of those referred urgently with a suspicion of cancer to begin treatment within 62 days of receipt of referral.
The target was to achieve 95 per cent of patients diagnosed with cancer starting treatment within 62 days of urgent referral with suspicion of cancer from the quarter ending December 2011 and for 95 per cent of patients diagnosed with cancer starting treatment within 31 days of their decision to treat, also from December 2011.
In January to March 2012, 94.8 per cent of patients urgently referred with a suspicion of cancer began treatment within 62 days of their referral. This figure increased to 95.3 per cent in April to June 2012. In January to March 2012, 97.9 per cent of patients diagnosed with cancer started treatment within 31 days of the decision to treat. This figure increased to 98.0 per cent in April to June 2012.
EXPERIMENTAL CANCER MEDICINE CENTRES
The Scottish Government, with Cancer Research UK, has co-funded the two Scottish Experimental Cancer Medicine Centres (ECMCs) since 2006. In 2011, both Scottish ECMCs were successful in bidding to be part of the Cancer Research UK programme in Stratified Medicine. Of the 21 ECMCs across the UK, only six were selected to participate in this programme. The aim of the Stratified Medicine programme is to develop novel, targeted treatments that take account of the genetic profile of an individual's cancer. This will lead to more efficient treatments and avoid cancer patients being given drugs that are ineffective against their particular tumour sub-type.
CORONARY HEART DISEASE
Heart disease and stroke continue to be a clinical priority. There has been substantial investment and redesign in cardiology services across Scotland, which has helped achieve a 60.7 per cent reduction, against a 60 per cent target, in early mortality from Coronary Heart Disease (CHD) between 1995 and 2010[13]. This reduction in early mortality from CHD increased to 64 per cent in 2011. Importantly, early deaths from CHD have been cut nearly twice as fast in the most deprived areas as in the least deprived areas[14]. Since 2007, the percentage of people who have had a heart attack and accessed cardiac rehabilitation has increased from 52 per cent to 75 per cent. These improvements demonstrate that our strategies for improving the outcomes of people living with, or at risk of developing, heart disease are delivering real results.
STROKE
The Scottish Stroke Care Audit: 2010 National Report Stroke Services in Scottish Hospitals* demonstrates major improvements in stroke care across the full spectrum of stroke services over the past 10 years. People with stroke have better access to thrombolysis, specialist stroke units, brain imaging services, medication and neurovascular clinics than ever before. Service improvements have helped deliver improved outcomes for people with stroke and made a major contribution to a 59 per cent reduction in premature stroke deaths from 1995-2010[15], exceeding NHSScotland's target of a 50 per cent reduction in premature stroke mortality. A new HEAT target introduced in April 2011 will drive further improvements with better access to stroke units. Significant progress has been made already with the percentage of stroke patients admitted to a stroke unit on the day of admission, or the day following admission, increasing from 68 per cent in 2010 to 78 per cent in 2011[16].
* All publications referred to within this document can be found in the publications section of the appendices
EMERGENCY CARE FOR PATIENTS WITH CARDIOVASCULAR DISEASE
During 2011/12, the Scottish Ambulance Service took forward an integrated and co-ordinated programme of improvement in emergency care for patients with Cardiovascular Disease (CVD). Significant improvement has been achieved against a range of clinical quality indicators including: an improvement from 77.4 to 78.3 per cent in the emergency response within eight minutes for patients in cardiac arrest; an increase from 14.5 to 16.9 per cent across Scotland in Return of Spontaneous Circulation (ROSC) for patients in cardiac arrest; an improvement in the percentage of hyper-acute stroke patients taken to hospital within 60 minutes from 75.5 per cent to 78.4 per cent; and an increase of 14.9 per cent in the number of ST-Elevation Myocardial Infarction (STEMI) patients receiving Primary Percutaneous Coronary Intervention (PCI) treatment[17]. In addition, the Scottish Ambulance Service, through implementation of the Community Resilience Strategy, has continued to contribute to improved clinical effectiveness through Community First Responder Schemes, the development of emergency responder models within remote and rural communities, and continued increase in the numbers of public access defibrillators.
TELEHEALTH AND TELECARE
As Scotland's national Telehealth and Telecare organisation, the NHS 24 Scottish Centre for Telehealth and Telecare has played a key role in the development of a national network to support Telestroke services. Eleven NHS Boards are now part of the Telestroke network which provides urgent support to stroke patients and enables rapid thrombolysis to be offered to appropriate patients, both in and out of hours. During 2011, there was an increase of 145 per cent in patients receiving thrombolysis across Scotland (from 145 cases to 358), in those areas making use of the Telestroke technology[18]. The process has now become part of the routine management of stroke patients and the findings and evaluation of the success of this service have been shared across the UK and Europe.
The National Waiting Times Centre Board provides a national resource for Scotland with patients travelling from other parts of Scotland to be treated at the Golden Jubilee National Hospital. In order to make life easier for rural patients, it has introduced telehealth video conferencing sessions between the Golden Jubilee and the local hospital. This means that patients receive the continuity of care they need in a more convenient setting and without the need for unnecessary travel.
ASSISTED LIVING
NHSScotland secured £5 million from the UK Technology Strategy Board matched by £5 million from the Scottish Government and enterprise partners through a successful bid to the Delivering Assisted Living Lifestyles At Scale (DALLAS) competition. The 'Living It Up' programme will be led by the Scottish Centre for Telehealth and Telecare in collaboration with the Joint Improvement Team, the Scottish Government, Scottish Enterprise, Highlands and Islands Enterprise and the Health and Social Care Alliance. The programme will integrate new healthcare and wellbeing technology and services across public services, enterprise and the third sector. By 2015, it aims to provide innovative products and systems and to deliver integrated services to enhance health, wellbeing, independence and lifestyles for over 55,000 people (including 10,000 living with long term conditions) in Forth Valley, Moray, Highland and Argyll and Bute, Lothian and Western Isles partnerships.
DIABETES-RELATED LIMB LOSS
Diabetes is the leading cause of lower-limb amputation. The vast majority of cases, however, can be avoided. The Scottish Diabetes Group has been working to ensure everyone with diabetes gets their feet checked, in a person-centred, safe and effective way. A co-ordinated approach to foot risk began in 2008 with education programmes, local initiatives, inclusion of Quality Outcomes Framework indicators, as well as joint awareness campaigns with Diabetes UK Scotland. This has ensured that since 2008, the number of people with diabetes receiving appropriate foot-risk assessment, care and support has more than doubled. In 2011, 69 per cent of people with diabetes had their foot risk recorded within the previous 15 months compared to 31 per cent in 2008[19]. We know that this will have a major impact in reducing foot ulcers and lower-limb loss. Research will be published later in 2012 which will illustrate the effectiveness of our approach.
DEMENTIA CARE IN HOSPITALS
In 2011/12, significant progress was made in taking forward a world-leading programme to improve the response to, and care of, people with dementia and their families in acute general hospital settings. NHS Education for Scotland (NES), in collaboration with the Scottish Social Services Council, developed and are delivering a range of national education programmes and training resources on dementia and delirium. The first 100 Dementia Champions from hospital settings graduated in March 2012 and are already leading improvement work in hospitals. A further 200 Dementia Champions drawn from both health and social care settings will come on stream by April 2013.
Funding has also been provided to Alzheimer Scotland to support the appointment of a specialist Dementia Nurse to each NHS Board, with the majority of these posts filled by March 2012. The Healthcare Improvement Scotland programme of inspections into older people's care in hospitals include a particular focus on dementia and delirium. An Implementation and Monitoring Group, established in January 2012 and chaired by the Chief Nursing Officer, is overseeing and co-ordinating all streams of work on improving the person-centred care of people with dementia and the implementation of the Standards of Care for Dementia in Scotland* in hospitals.
* All publications referred to within this document can be found in the publications section of the appendices.
RELEASING TIME TO CARE
Releasing Time to Care (RTC) has resulted in staff spending more time providing face-to-face care for patients. In turn, this has resulted in increased direct patient care and measurable improvements to the working environment and to patient care. A stock take undertaken for the Scottish Government by Healthcare Improvement Scotland (HIS) illustrated uptake across different care environments including increasing use by community teams and more recently Productive General Practice (PGP). More than 300 practices have registered to use PGP including practices using it to improve medicines management and patient safety and over 300 practitioners and staff have attended learning sessions.
MUSCULOSKELETAL SERVICES
NHS 24 and the Scottish Government undertook a major re-design of musculoskeletal (MSK) care pathways in order to improve timely access for patients to the most appropriate advice and support from clinical specialists. The major change was the introduction of a new referral system with NHS 24 the single point of access. In future, the majority of the 240,000 adults with an MSK disorder who are referred currently by their GP to local physiotherapy services will be able to self-refer to NHS 24. NHS 24 staff will: provide telephone advice on the most appropriate treatment option; encourage patients to self-manage; or refer some to community physiotherapy or other Allied Health Professions services, or medical settings as required. The system has been introduced in NHS Lanarkshire and pilot work is being undertaken in NHS Lothian and NHS Ayrshire and Arran with a view to rolling it out across the rest of NHSScotland in the next 18 months. The system will improve outcomes for patients, given the evidence that early management reduces the chronicity of cases and the intensity of treatment required, and will mean much shorter waits for appointments.
CARE OF OLDER PEOPLE IN HOSPITALS
A programme of hospital inspections by Healthcare Improvement Scotland (HIS) commenced in February 2012 and has found many areas of strength in older people's care in hospital settings, as well as areas for improvement. NHS Board action plans are being implemented following each inspection, ensuring that the inspection programme drives improvement locally. HIS has also established an Improvement Board, which is taking forward national improvement activities in light of the findings from the reports. HIS will publish twice-yearly summary reports providing a national overview based on the findings from the inspections carried out in each six-month period.
RESHAPING CARE PROGRAMME
The Joint Improvement Team (JIT) is supporting Scotland's 32 health, housing and social care partnerships to deliver more care and support at home, with a greater focus on prevention to improve outcomes and manage future demand. These partnerships achieved a 7 per cent reduction in the days people aged over 65 spent in hospital as an emergency between 2006/07 and 2010/11[20]. Since 2006, the number of people delayed in hospital has reduced by 62 per cent and delays over six weeks are down 93 per cent[21]. This is delivering faster and better recovery, more effective continuity and collaboration and a stronger focus on personal outcomes. NHSScotland also made progress towards the 2011/12 HEAT target on reducing the level of emergency bed days for patients aged
75 and over.
HEAT TARGET
Reducing the need for emergency hospital care, NHS Boards will achieve agreed reductions in emergency inpatient bed days rates for people aged 75 and over between 2009/10 and 2011/12 through improved partnership working between the acute, primary and community care sectors.
The target was to achieve a reduction of occupied emergency bed days, in acute specialities, for patients aged 75+ per 1,000 population by 2011/12. Between 2009/10 and 2011/12 there was a 7.6 per cent decrease in the rate of occupied bed days for patients aged 75+ from 5,390 bed days per 1,000 population to 4,980. The graph below shows emergency bed days for patients aged 75+ (per 1,000 population) since 2004/05.
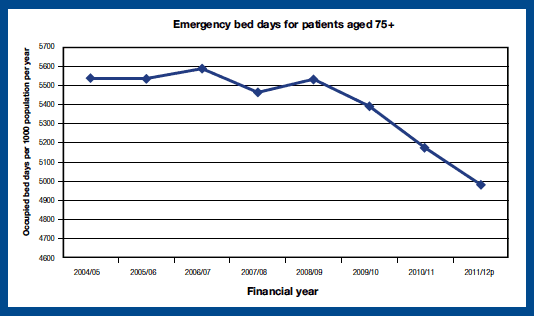
Source: NHS Information Services Division: Acute Hospital Activity (SMR01)
HOME OXYGEN SERVICE
NHS National Services Scotland (NSS) has helped nearly 5,700 patients at home by co-ordinating a home oxygen service, with cylinders and oxygen concentrators available from Community Pharmacies[22]. Plans are underway to improve the service by creating an integrated national service. This will involve direct delivery of updated equipment to patients' homes and improved prescribing guidelines to ensure that patients are getting care appropriate to their needs. The new service will also save NHS Boards money that can be reinvested into patient care.
MODERNISING NURSING IN THE COMMUNITY
The Modernising Nursing in the Community programme was established to provide support and direction for community nursing in order to realise its full potential. Resources developed by the programme in 2011 include an interactive website, career and development frameworks for eight professional disciplines and the development of three universal care pathways. Over the coming years, we will continue to support NHS Boards to improve community nursing care.
PRISONER HEALTHCARE
Prisoner healthcare formally transferred from the Scottish Prison Service to NHSScotland on 1 November 2011. This will ensure that services to prisoners have the same focus on quality through the pursuit of our Quality Ambitions and will ensure better continuity of care. Interventions such as the provision of support and services for vulnerable families of prisoners, particularly those with dependent children, will contribute to reducing inequalities. NHS organisations, such as the Community Health Partnerships (CHPs), will provide better links to other essential services such as job and employment training, housing and financial and social support. The transfer also ensures that healthcare staff working in the prison setting are supported and are not isolated.
REFRESHED FRAMEWORK FOR MATERNITY CARE
Following the launch of the Refreshed Framework for Maternity Care* by the Minister for Public Health and Sport, a national Implementation Support group has been leading three improvement themes to support NHS Boards realise the aims of the refreshed framework. This Implementation Support Group is a collaboration between the Scottish Government, Territorial NHS Boards, Special NHS Boards and Healthcare Improvement Scotland. A key focus of the implementation work is supporting NHS Boards to achieve the antenatal access HEAT target introduced in April 2012 and the quality improvements necessary to strengthen the role of maternity services in reducing health inequalities and improving maternal and infant health.
* All publications referred to within this document can be found in the publications section of the appendices.
UNSCHEDULED CARE
During 2011/12, the National Unscheduled Care Group (NUCG) developed plans to improve the quality of unscheduled care across the whole healthcare system. Proposals to be taken forward include: developing specific alternative services on hospital sites to people attending A&E; extending the range and availability of urgent care services in the community; and improving advice and 'signposting' for patients with urgent care needs. NHSScotland is committed to the standard that 98 per cent of patients attending emergency departments should be discharged, admitted or transferred within 4 hours. During the year, the Emergency Care Pathways Programme was launched to support achievement of the standard. The two-year programme, through a number of measures, aims to remove factors that can delay patients in A&E moving to an inpatient bed. This will not only improve care for emergency patients, but will generally help to ease pressures in A&E departments at peak times.
ORGAN DONATION
A high-impact media campaign was run to raise awareness of organ donation and to 'make it usual' by encouraging people to join the NHS Organ Donor Register. Thirty-nine per cent of the Scottish population is now registered - the highest percentage of any part of the UK[23]. This increased awareness, coupled with the improved organ donation infrastructure in Scotland - including additional specialist nurses, clinical leads and NHS Board donation committees - resulted in the highest ever number of deceased organ donors and, in turn, a record number of solid organ transplant operations.
CHILD ORAL HEALTH
The Childsmile Nursery and School Programme continues to improve oral health. The most recent survey of Primary 7 schoolchildren in 2011 found that 69.4 per cent of children had no obvious signs of dental decay[24]. This is significantly higher than the 2010 Scottish target of 60 per cent. The targeted approach of the Childsmile programme will help to further improve the oral health of children in the most deprived communities, who continue to carry an additional burden of dental disease.
INDEX OF ORTHODONTIC TREATMENT NEED
The use of Index of Orthodontic Treatment Need (IOTN) was proposed in An Action Plan for Improving Oral Health and Modernising NHS Dental Services in Scotland (2005)*. It came into effect in NHS dentistry in October 2011. IOTN gives an evidence-based framework to decision-making around treatment, and will ensure that orthodontics is provided for those children who have a clinical need for treatment and who will have an oral health benefit at its completion.
* All publications referred to within this document can be found in the publications section of the appendices.
PATIENT REMINDER SERVICE
NHS 24 launched a pilot Patient Reminder Service that supports NHS Boards to deliver more efficient and effective outpatient services. During the pilot project, delivered in partnership with NHS Forth Valley, significant improvements were made in attendances to outpatient clinics. The pilot scheme, in which NHS 24 staff called patients in advance to remind them of appointments, was conducted in gynaecology, paediatrics, gastroenterology and oral maxillofacial clinics. Average rate reduction for the pilot in DNAs (Did Not Attends) was 27 per cent. NHS Forth Valley has now formally commissioned the service. NHS 24 is also delivering a Patient Reminder Service across all outpatient appointments for NHS Western Isles.
INVESTMENT IN RESEARCH
The Scottish Government Chief Scientist Office completed a strategic investment of £10 million per annum in 188 new (whole time equivalent) NHS Research Scotland (NRS) clinical infrastructure posts. This was complemented by the launch of a £3 million NRS Career Researcher Fellowship scheme enabling NHS clinical staff to develop a research career by funding protected time. These investments address current and future needs of NHSScotland in its pursuit of clinical research for patient benefit. This has attracted interest from industry, resulting in NRS entering into strategic collaborations with PPD and Quintiles, two of the world's largest contract research organisations.
STAFF
RESHAPING SCOTLAND'S MEDICAL WORKFORCE
Since 2009, Scotland has been taking steps to reshape its medical workforce, moving away from a service delivered by trainee doctors to one which is delivered predominantly by trained doctors. During 2011/12, further progress has been made towards this, with a continuing reduction in trainee numbers accompanied by some changes in consultant working patterns, with job planning being used more effectively than before to produce more hands-on consultant-delivered care in the evenings and at weekends. Following a recent review of the project, a refined and improved approach to determining future specialty training numbers has been developed, with a specialty by specialty risk analysis used to inform decisions on the training establishment on an annual basis.
MEDICAL REVALIDATION IN SCOTLAND
Good progress was made throughout 2011/12 towards ensuring that NHSScotland will be ready to meet its obligations when revalidation for all doctors is introduced from December 2012 (introduction of revalidation is subject to the approval of the Secretary of State for Health). Feedback from patients and colleagues together with critical incident data form part of a new and more robust appraisal process. Medical Revalidation will help to identify areas of practice where there are concerns about performance, and will assist in improving effectiveness, providing information on where development and support are required.
SUPPLEMENTARY MEDICAL STAFFING
Boards are continuing to make good progress on the implementation of actions to address the issues raised by Audit Scotland in its report Using Locum Doctors in Hospitals* and in implementing the guidance setting out the best practice framework to address supplementary medical staffing issues.
* All publications referred to within this document can be found in the publications section of the appendices.
NEW CONTRACT FOR SPECIALTY DOCTORS AND ASSOCIATE SPECIALISTS
During 2011/12, NHSScotland employers and the Scottish Government worked with BMA Scotland to ensure the implementation of a new pay and terms and conditions of service package for Specialty Doctors and Associate Specialists in NHSScotland. The benefits of this new contract include: better access and experience for patients as a result of increased overall capacity; more appropriate recognition and reward for doctors; and an improved ability of NHS employers to manage doctors' time in ways that best meet local needs and priorities.
REDUCTION IN SENIOR MANAGEMENT POSTS
A national target was introduced to reduce the number of senior managers by 25 per cent between 31 March 2010 and 1 April 2015. In the first two years significant progress has been made. The overall reduction in senior management between March 2010 and March 2012 was 202 WTE, a reduction of 16 per cent, representing good progress towards meeting the 2015 target[25]. This target will continue to support the move towards a leaner senior management structure.
ESTATES AND FACILITIES
REDUCING CARBON EMISSIONS AND ENERGY CONSUMPTION
Through reducing energy-based carbon emissions and energy consumption, NHSScotland will make a significant contribution towards the Scottish Government's aim to reduce greenhouse gas emissions by 50 per cent by 2050 and the interim target of a 42 per cent reduction by 2020. A reduction in energy consumption is also important in the context of increasing global fuel costs and the impact of their resulting cost increases on the delivery of core NHS services. The specific targets for NHSScotland are to reduce CO2 emissions for oil, gas, butane and propane usage annually by 3 per cent to 2014/15; and NHSScotland to continue to reduce energy consumption annually by 1 per cent to 2014/15. During 2011/12, NHSScotland delivered a 1.4 per cent reduction in energy consumption compared to the previous year, thus exceeding the target. CO2 emissions reduced by 1.7 per cent on the previous year, which was below target[26]. However, first quarter energy and CO2 performance figures for 2012/13 indicate that NHSScotland is on course to meet the 2012/13 targets.
NHS Board Story:
NHS Greater Glasgow and Clyde
REVIEWING LONG-TERM ANTIDEPRESSANTS CAN REDUCE DRUG BURDEN†
Antidepressant prescribing continues to rise across NHScotland, Europe and the US. Contributing factors are increased long-term prescribing and possibly the use of higher Selective Serotonin Re-uptake Inhibitor (SSRI) doses. In 2007, the Scottish Government set targets to reduce antidepressant prescribing. In Scotland, the majority of antidepressants are prescribed by GPs for the treatment of depression. Currently there are no formal process to support GPs to review patients with common mental health problems and the effect of such reviews is unknown.
Four Community Health and Care Partnerships committed to reviewing a proportion of patients prescribed with the same antidepressant for two years or more and to evaluate prescribing and management changes pre and post-review.
Seventy-eight of 96 practices agreed to participate, representing a population of 388,656 over 18 year olds, of whom 33,313 (8.6 per cent) were prescribed an antidepressant, excluding amitriptyline due to non-mental health use, and 15,689 (47.1 per cent) were defined as long-term users.
2,849 (18.2 per cent) of long-term users were reviewed with one in four (28.5 per cent) having a change in antidepressant therapy: 7.0 per cent stopped, 12.8 per cent reduced dose, 5.3 per cent increased dose and 3.4 per cent changed antidepressant, resulting in a statistically significant 9.5 per cent reduction in prescribed daily doses and observed 8.1 per cent reduction in prescribing costs. 6.3 per cent were referred onwards, half to NHSScotland mental health services.
This initiative is currently running as a prescribing indicator in NHS Greater Glasgow and Clyde.
As a result of this exercise, more than 140 of the 270 practices in NHS Greater Glasgow & Clyde are now reviewing and are continuing to review a proportion of their patients who have been prescribed long-term antidepressants since 2010.
† This work was presented as a poster at the 2012 NHSScotland Event and won first prize in the 'Effective' poster category. To view the poster visit: www.nhsscotlandevent.com/posters/Posters-2012/
QUALITY AMBITION
PERSON-CENTRED
Mutually beneficial partnerships between patients, their families and those delivering healthcare services which respect individual needs and values and which demonstrate compassion, continuity, clear communication and shared decision-making.
During 2011/12, we have made some important progress towards our Quality Ambition for person-centred healthcare. In this section we set out details of progress on the range of initiatives that are being pursued across NHSScotland for the benefit of patients, carers, the public and for staff.
Key areas of progress include improvement in people's experiences of hospital and wards, with evidence that patients were positive about their involvement in their care and treatment. Patients were also positive about their experiences of out-of-hours healthcare. Work continued to implement the Patients Rights (Scotland) Act 2011 with regulations and directions laid before Parliament to support the provisions in the Act which include: a treatment time guarantee; patient feedback, comments, concerns and complaints; and healthcare principles. There was a continued focus on improving palliative and end of life care with the achievement of many of the actions contained in Living and Dying Well* and its subsequent Building on Progress* report, and a range of initiatives were taken forward to support carers and young carers.
* All publications referred to within this document can be found in the publications section of the appendices.
PATIENTS AND THE PUBLIC
BETTER TOGETHER - SCOTLAND'S PATIENT EXPERIENCE PROGRAMME
The Better Together programme is a fundamental component in improving healthcare quality through the person-centred focus of the Quality Strategy. It provides national information on patient experience, along with tools and practical advice to support improvements prioritised through analysis of the data as well as local information.
In August 2012, robust, comparable data on the quality of healthcare experience from the third Inpatient Survey were published. Data were provided by hospital as well as by NHS Board. NHS Boards have developed action plans to address the areas people have identified as being important to them and where improvements can be made. The emphasis is firmly on improving at a local level.
KEY FINDINGS
2012 INPATIENT PATIENT EXPERIENCE SURVEY
There was a slight improvement in the experiences of patients nationally compared to the previous survey in 2011. Scottish inpatients were again generally positive about their hospital stay.
The area with the most improvement was people's experiences of the hospital and ward environment. This year, slightly more patients indicated that the ward, bathrooms and toilets were clean; they were happy with the food and drink they received; and noise at night was less of a problem.
Despite the improvements elsewhere, the percentage of patients who were confident that they could look after themselves when they left hospital saw a further reduction by one percentage point to 85 per cent; it had dropped by two percentage points in 2011.
This year, questions about care and support services that needed to be arranged before patients could leave hospital were introduced. Of patients that required care or support services, 82 per cent rated that, overall, the services they got after leaving hospital were excellent or good.
In May 2012, the results of the 2011/12 Patient Experience Survey of GP and other local NHS services were published. Individual reports were published for all NHS Boards, Community Health Partnerships (CHPs) and GP practices. The questionnaire was sent to a random sample of people who were registered with a GP in Scotland in October 2011. Over 145,000 people provided feedback on their experiences.
KEY FINDINGS
2011/12 PATIENT EXPERIENCE SURVEY OF GP AND LOCAL NHS SERVICES
The experiences of Scottish GP patients in 2011/12 were similar to those reported for 2009/10:
- Patients were mainly positive about their experience of consultation with doctors or nurses. At least 90 per cent of patients responded positively to all of the questions about doctors and nurses.
- Patients remained very positive about their involvement in their care and treatment. Overall, 89 per cent of patients felt that the care provided by the GP practice was excellent or good.
Patients were slightly more positive about their experiences of doctors and nurses than they were in the 2009/10 survey.
Patients were less positive about their experiences of accessing GP practice services - there was a decrease in the percentage of patients rating the overall arrangements for seeing doctors and nurses as good or excellent. This decrease was seen across almost all NHS Boards. As in 2009/10, there was considerable variation in the results for individual GP practices on patients' experiences of the overall arrangements for seeing doctors.
Patients were generally positive about their experiences of out-of-hours healthcare with 72 per cent rating the overall care they received as good or excellent. However, 11 per cent of patients rated the overall care as poor or very poor.
PATIENT RIGHTS (SCOTLAND) ACT 2011
The Patient Rights (Scotland) Act makes provisions for: a treatment time guarantee; patient feedback, comments, concerns and complaints; and healthcare principles. Regulations and directions to support these were laid before Parliament in February 2012, and each will be introduced in stages during 2012/13, along with a Charter of Patient Rights and Responsibilities. Good practice guidance for NHSScotland in relation to feedback, comments, concerns and complaints was revised and issued in March 2012. The legislation and supplementary guidance is part of an ongoing development to support the Quality Strategy, ensuring that patients are at the heart of our NHSScotland.
ENABLING PEOPLE TO SELF-MANAGE THEIR HEALTH
Supporting people to self-manage and to look after their own health is key to achieving our 2020 Vision. In order to do this, people need to have access to and to understand the information they are provided with. They also need to be able to link up with the local resources that can help them. Two initiatives, managed by the Health and Social Care Alliance (previously the Long Term Conditions Alliance Scotland), are helping people across Scotland to self-manage their health: the innovative Accessing Local Information to Support Self Management (ALISS) project; and the Self Management Fund, established under the Self Management Strategy in 2008. During 2011/12, the ALISS project has gone from strength to strength, making local information resources visible and accessible, while an extension of the Self Management Fund, with an additional £1.6 million of funding support, has supported 30 projects across Scotland.
KEY ACHIEVENMENTS
ENABLING PEOPLE TO MANAGE THIER HEALTH
In the last year the Self Management Fund has enabled:
- Clydeside Action on Asbestos to produce a digital self management programme and to develop a system for providing those diagnosed with self management information at the point of diagnosis.
- No Strings Attached to deliver their music self management programme for young people living with Asthma to the Pririe Park area of Glasgow, to develop parent peer support roles and to create a digital music and Asthma resource to support participants between sessions.
- Pink Ladies First Scotland to extend their self management programmes for women living with anxiety and depression by providing pre-course support for first time participants and run advanced programmes for Pink Lady graduates.
- Post Natal Depression Support Network, which has provided support to women living with post natal depression in an isolated area in Aberdeenshire, has developed peer support arrangements, linked up with maternity unit staff and supported 29 women plus many more via their web presence.
- Angus Cardiac Group to extend their work - recruiting local exercise leaders in health behaviour change techniques to improve people's understanding of self management - and to build on the 402 participants and 17 volunteers already involved.
CO-PRODUCTION AND COMMUNITY CAPACITY BUILDING
As Scotland's people enjoy longer and healthier lives, they want to remain living independently in their own homes and communities. Achieving this in a challenging economic environment requires that, as a nation, we maximise all our collective assets. Co-production places the person at the centre of their healthcare. It recognises that individuals, their families and communities possess assets such as circles of support, personal skills and the knowledge of the 'expert patient' which, when used in partnership with professional public services, can maximise their health, wellbeing and independence. During 2011/12, work was undertaken to increase awareness of the benefits that a focus on co-production and community capacity building can bring in improving the health and wellbeing of service users and the effectiveness of providers. In collaboration with social enterprise Governance International, a training package was rolled out for care partnerships across Scotland, culminating in a high profile national learning event in January. Outcomes from this event included the further promotion of these approaches through the development of the Scottish Co-production Network.
PALLIATIVE AND END OF LIFE CARE
In the autumn of 2011, NHS Boards were asked to report progress against the actions in Living and Dying Well* and its subsequent Building on Progress* report. This demonstrated a continued focus on improving palliative and end of life care with many of the key actions in Living and Dying Well* being achieved consistently across NHSScotland. Many examples of innovation and good practice are in place across the country. The areas of work which continue as a priority are: early identification of patients who may need palliative care; advance/anticipatory care planning; palliative and end of life care in acute hospitals; improved use of the electronic palliative care summary (ePCS); and embedding of the Do Not Attempt Cardiopulmonary Resuscitation (DNACPR) policy.
* All publications referred to within this document can be found in the publications section of the appendices.
COMMUNITY PHARMACY - PUBLIC HEALTH SERVICE
Through the Public Health Service (PHS), access to smoking cessation support is increasing. The number of nicotine replacement items dispensed through the community PHS has almost doubled in the last year with items dispensed increasing from around 23,000 in March 2011 to around 41,700 in March 2012[27]. The support offered through the PHS has been instrumental in NHS Boards meeting HEAT targets. The PHS also provides convenient access to sexual health advice and support including free access to Emergency Hormonal Contraception (EHC).
COMMUNITY PHARMACY - MINOR AILMENT SERVICE
It is estimated that, on average, there are over 11,500 consultations a day in Scotland where a pharmacist advises on or treats minor ailments. The Minor Ailment Service (MAS) enables people who are eligible to register with the Community Pharmacy of their choice for the consultation and treatment of common conditions without the need to visit their GP. Under the service, the pharmacist advises, treats or refers the patient according to their needs. The service, which is now available across Scotland, is particularly valued by patients and NHS 24 in the out-of-hours period. At the end of March 2012, there were some 844,843 patients registered with MAS - an increase of 6.8 per cent compared to March 2011[28].
COMMUNITY PHARMACY - CHRONIC MEDICATION SERVICE
The Chronic Medication Service (CMS) improves patient care through a systematic approach to the pharmaceutical care of patients with long term conditions. It uses the skills and expertise of Community Pharmacists to support patients by helping to improve their understanding of their medicines, and helping to maximise the clinical outcomes from their therapy by providing an individualised, person-centred model of care. The partnership approach and systems in place through CMS are also helping to minimise adverse drug reactions, preventing potential problems with medicines and reducing wastage. Steady progress continues to be made in rolling out the CMS. By the end of March 2012, over 141,000 patients were registered for the service with Community Pharmacies across Scotland - more than double compared to the same period in the previous year.
DENTAL REGISTRATION
As of March 2012, 78 per cent of the Scottish population was registered with an NHS dentist[29]. This represents a continued improvement from previous years. Importantly, within the 6 to 12-year-old age group the registration level is 99.1 per cent which is a tremendous achievement. The majority of the Scottish population now have access to individualised care and advice to support them improve their oral health.
APPS TO SUPPORT PATIENT DECISION-MAKING
The first in a series of applications (apps) for patients (for iPhone, iPad, Android phones and tablets) has been developed to help patients better understand the latest medical evidence and to use this to make decisions about their healthcare. The app was developed by the Scottish Intercollegiate Guidelines Network (SIGN) as part of Healthcare Improvement Scotland (HIS), and will help ensure patients get the best care available, no matter where they live.
NEW BARRHEAD HEALTH AND SOCIAL CARE CENTRE
The new £17 million Barrhead Health and Social Care Centre, built by NHS Greater Glasgow and Clyde in partnership with East Renfrewshire Council, provides health and community services under one roof and has been developed in conjunction with the Community Health and Care Partnership (CHCP). The facilities include three GP practices, two dental practices, an elderly day care centre, physiotherapy and podiatry services and accommodation for up to 100 community-based staff including social workers. The CHCP has been a leader in managing local authority social care services and local NHS services within a single structure and is a model now being replicated across Scotland.
NEW CARDIAC AND INTERVENTIONAL RADIOLOGY SUITE, RAIGMORE HOSPITAL, INVERNESS
With the expansion of cardiology services provided at Raigmore, as many as 400 patients every year no longer have to travel to Aberdeen for percutaneous coronary intervention (widening a narrowed artery) and many hundreds of inpatients have angiograms locally. The new £5.1 million purpose-built Cardiac and Interventional Radiology Suite at Raigmore Hospital was one part of a three-phase project that also included the refurbishing of staff changing rooms, a new medical records department and interventional radiology services. Procedures that previously involved open operations can now be performed using keyhole techniques. It also allows emergency department staff to treat critically ill patients all of which enhances the quality of patient care.
NEW £27 MILLION ACUTE MENTAL HEALTH HOSPITAL IN DUMFRIES
The replacement of the cramped and decaying 1930's Crichton Hospital mental health units was necessary as they lacked an appropriate environment for safely treating acute adult, older adult and dementia mental health cases and therefore compromised the quality of care being provided, for both patients and staff. This has been remedied by putting privacy, dignity and security at the heart of design. The provision of 85 beds includes modern intensive and high care units in addition to therapeutic, occupational and recreational space, creating a healing environment that should impact positively on readmission rates.
CARERS
CARERS STRATEGY
Progress continues to be made in implementing Caring Together: The Carers Strategy for Scotland 2010-2015*. With support from the Scottish Government of £4.9 million in 2011/12, NHS Boards and the Scottish Ambulance Service have taken forward a wide range of initiatives to support carers and young carers[30]. This includes the provision of information and advice, carer awareness training and carer training. This is helping to ensure that carers are better supported to sustain them in their caring role. The Scottish Government has also funded the pilot in six NHS Boards of a Young Carers Authorisation Card to help support young carers in health settings.
* All publications referred to within this document can be found in the publications section of the appendices.
EXPANSION OF THE FAMILY NURSE PARTNERSHIP PROGRAMME IN SCOTLAND
The Family Nurse Partnership Programme works closely with teenage mothers from early pregnancy until the child reaches the age of two. A Scottish Government commitment of £2.73 million in 2011/12 has enabled implementation of the programme across NHS Tayside with the recruitment of 295 clients over a 12-month recruitment period (July 2011 to June 2012). The first evaluation report was published in July 2011, with a second report in June 2012. Lessons are being used to shape the wider implementation, to include five new NHS Boards by the end of 2013. Four NHS Boards have been nominated so far: NHS Fife, Greater Glasgow and Clyde, Ayrshire and Arran, and Lanarkshire, together with Highland Council which has an integrated health and social care model. A recent, further investment of £11 million will establish Family Nurse Partnership teams across the whole of Scotland by the end of 2015. The programme provides skills and resources to support the Family Nurses to deliver a pre-set programme, whilst being flexible enough to respond to the individual needs of the client.
STAFF
OCCUPATIONAL HEALTH AND SAFETY
Safe and Well at Work: Occupational Health and Safety Strategic Framework for NHSScotland* was launched in March 2011. Successful implementation of the model by NHS Boards will help reduce the numbers of staff who suffer from work-related injury or illness, promote positive health and wellbeing and ultimately deliver better patient care. During the past year, the Working Well programme has delivered two web-based packages for NHSScotland staff; Who Cares?[31], which provides advice for staff and managers on balancing work and care; and What Counts?[32]* providing advice for staff on managing their money.
* All publications referred to within this document can be found in the publications section of the appendices.
REVIEW OF PARTNERSHIP WORKING IN NHSSCOTLAND
Researchers from Nottingham University have undertaken research into the industrial relations model in NHSScotland that was introduced in 1999, commonly known as Partnership Working. The final report for this research was published on 1 February 2012. The two-year study reveals how a 'mature and positive' approach to industrial relations has helped underpin NHSScotland's commitment to high quality patient care: 'The Scottish Government and employers have fostered staff representatives' commitment to health policies and organisational restructuring in order to improve patient care.' The study also shows that NHSScotland's handling of partnership agreements represents a leading-edge example and offers important lessons for public services throughout Britain: 'In our view, partnership in NHSScotland has matured into probably the most ambitious and important contemporary innovation in British public sector industrial relations.'
STAFF EXPERIENCE
The Staff Experience project commenced in November 2011. It focuses on defining, improving and measuring staff experience, recognising the critical link between staff experience and organisational performance (and in particular patient experience). It is being undertaken jointly by NHS Dumfries & Galloway, NHS Forth Valley and NHS Tayside. During 2011/12, a literature review was undertaken, the results of which were used to inform the review of the Staff Governance Standard, as well as informing early discussions about potential measures of staff experience. The project has already received some positive high profile attention from outwith NHSScotland.
NHS Board Story:
NHS Lanarkshire
JUST-IN-CASE BOXES: IMPROVING ACCESS TO END OF LIFE MEDICATIONS†
Many patients nearing end of life wish to remain in their own home for as long as possible and ensuring timely access to medications can prevent unnecessary crises and distress for both patients and their carers; preventing hospital admissions and calls to out-of-hours.
NHS Lanarkshire has introduced 'Just-In-Case' boxes to facilitate anticipatory prescribing and improve access to medications. Each box contains medications that are commonly required to manage symptoms at the end of life.
In order to measure the outcomes, such as hospital admissions, out-of-hours calls and patients being able to stay in their preferred place of care, each box contains an audit form to be completed for all patients by the team which looked after them.
Using this data, NHS Lanarkshire has been able to identify that 180 of 219 boxes were used (at least one drug administered) as of February 2012. This resulted in 84 hospital admissions being avoided and 114 out-of-hours calls being avoided due to the box being in place. These results come after an approximate period of 18 months' data collection with regular reporting to the Palliative Care Managed Clinical Network.
The 'Just-In-Case' box provides patients with reassurance, allows symptoms to be managed promptly and prevents hospital admission.
† This work was presented as a poster at the 2012 NHSScotland Event and won first prize in the 'Person-centred' poster category. To view the poster visit: www.nhsscotlandevent.com/posters/Posters-2012/
INFRASTRUCTURE
SUPPORTING AND FACILITATING ACHIEVEMENT
The Quality Strategy recognised that there were a number of key national areas of development, which need to be co-ordinated, accelerated and aligned to support and facilitate NHSScotland and its partners to have the maximum impact on the three Quality Ambitions. These include:
- Measurement;
- Information Technology;
- Workforce, Education and Training;
- Quality Improvement;
- Communication; and
- Governance.
There has been a national focus on these issues and work has continued to challenge progress, accelerate pace, and to create linkages and a shared ownership of these vital developments.
MEASUREMENT
During 2011/12, work has taken place on developing a new Information Framework for Health and Social Care. This will provide the strategic context against which organisations working across health and social care in Scotland can make decisions about allocation and prioritisation of resources to support the development of information and intelligence. The Framework is built upon the clear understanding that having the right information and intelligence is essential to drive improved quality in health and social care.
Information Services Division (ISD) is key to ensuring we have the right data to support world-class health and social care services. Its reorganisation over the past year means that it is now better placed to do this, while streamlining existing data collection and achieving efficiencies.
Work continues on the development and improvement of the Quality Outcome Indicators[33] (level 1 of the Quality Measurement Framework). New information on several of the indicators has been published during the year, and a web portal to provide information on progress with all the indicators will be available in early 2013. This will provide one source to get an at-a-glance view of progress, as well as provide links to look underneath the data. Some of the indicators are still under development, and have created helpful debate on how we can best capture quality in a measurable way at different levels within the Quality Measurement Framework.
The indicators and outcomes will be reviewed in the coming months to ensure they are fit for purpose and in view of the integration of health and social care agenda. At the same time work will be underway to look at the specific integration outcome indicators for partnerships. The HEAT targets reflect the agreed areas for specific accelerated improvement each year, contributing to progress towards the Quality Ambitions and Quality Outcomes. We continue to provide ready access to NHSScotland and NHS Board performance through Scotland Performs[34] which is updated on a continuous basis.
INFORMATION TECHNOLOGY
Developing and supporting the appropriate IT infrastructure to deliver safe, effective and person-centred care is a key priority for NHSScotland. The areas of progress are described here and provide an overview of activity during 2011/12.
eHEALTH STRATEGY 2011-17
A new eHealth Strategy - The Second eHealth Strategy for NHSScotland 2011-2017* - was published in September 2011. The strategy focuses on benefits and customers rather than products and suppliers. It aligns IT activity with our Quality Ambitions and includes six key aims in the areas of: clinical communication; person-centred care; patient safety; support for patients in the community; improvements in efficiency; and access to key information. Following a significant capital investment programme in the previous period (2008-11), this strategy focuses on delivering these key aims by maximising the value of previous capital investment. Supporting strategies have also been agreed on information assurance, applications, infrastructure and finance.
* All publications referred to within this document can be found in the publications section of the appendices.
PATIENT MANAGEMENT SYSTEM
A consortium of NHS Boards led by NHS Lanarkshire has procured and implemented the new Patient Management System (PMS) in Scotland. An investment of £44 million has been made in the system which will cover over 70 per cent of the Scottish population and is now operational in NHS Borders, Grampian, Lanarkshire, Ayrshire & Arran, Greater Glasgow and Clyde and Lothian. The first phase of benefits are now being realised with additional capabilities including order communications - eliminating the need for paper-based diagnostic requests and results reporting - and clinical workflows planned over the next year.
NEW IT SYSTEMS FOR GPs
A consortium of NHS Boards led by NHS Greater Glasgow and Clyde worked together to purchase two new IT systems for GPs with an investment of £38 million. During 2011/12, all GP practices in Scotland (over 1,000) successfully migrated from the previous GPASS IT system to the new system co-ordinated by National Services Scotland (NSS). This migration was completed within the agreed timescale and budget. These systems provide enhanced capabilities and NHS Boards are working closely with GP practices to achieve the maximum benefit from these.
CLINICAL PORTAL
Clinical portals (electronic windows to information) are now firmly established in many NHS Boards and becoming a standard tool used in clinical encounters with patients across NHSScotland. They provide comprehensive access to clinical systems and information to support excellent and safe patient care. In secondary care they have become the clinician interface with the electronic patient record. Clinical portal implementation has continued to make steady progress across NHSScotland. The NHS Greater Glasgow and Clyde portal has over 17,300 users and around 390,000 documents (results, letters assessments etc.) are being accessed each week. Most users are in the acute sector with around 2,000 in the community. The Golden Jubilee National Hospital has rolled out its portal to around 80 per cent of its staff where feedback has been extremely positive. The members of the South and East portal consortium (NHS Lothian, Borders, Fife and Dumfries & Galloway) all have plans to roll out the clinical portal to their hospital sites during 2012. Within the North of Scotland portal consortium, NHS Tayside continues to make progress, with around 3,500 clinical users accessing the portal regularly and around 10,000 accesses per week.
EMERGENCY CARE SUMMARY
The Emergency Care Summary (ECS) is widely used in A&E, out-of-hours, and NHS 24 to improve the care of patients in unscheduled care. Recently its use has been extended to the Scottish Ambulance Service and it is now widely used by ambulance and other emergency vehicle staff. There have been 10 million accesses since its introduction in 2006. Work is underway to extend its use into scheduled care as part of wider work to improve clinician access to up-to-date records of patient medications, particularly at hospital admission and discharge, in order to improve the care and safety of patients.
KEY INFORMATION SUMMARY
The Key Information Summary (KIS) is a focused extract of information from Primary Care systems designed to provide important patient details for clinicians in unscheduled care. This will replace paper processes and underpins improvements in care planning and patient centeredness. KIS includes patient wishes and details of care plans for patients with multiple conditions or special requirements. Widespread consultation with clinical groups and patients was completed in 2011 and development and pilots commenced in early 2012. Rollout continues in pilot practices and remains on track to meet the eHealth and quality milestones.
HEALTH AND SOCIAL CARE INTEGRATION
The Data Sharing Technologies Board was formed in November 2011. Its aim is to improve collaborative working across NHSScotland and local government, and to support health and social care integration. NHS Lothian and the City of Edinburgh Council are developing a portal which will enable the sharing of assessments and adult protection messaging. NHS Greater Glasgow and Clyde is working with two councils to develop a portal which will enable the sharing and viewing of single shared assessments. NHS Ayrshire and Arran is developing and hosting Ayrshare, which will enable health and social work practitioners to share information. NHS Lanarkshire, and North and South Lanarkshire Councils have an established framework, which enables the sharing of assessments, together with adult, child and pre-birth protection messaging.
USE OF VIDEO CONFERENCING TECHNOLOGIES
Room and desk based video conferencing services are benefiting both patients and staff. They are contributing to greater operational efficiency and improvements in the quality of patient care. There are over 660 video conferencing units, covering all NHS Boards, averaging around 100 conferences per day. These are saving on travel time and costs for patients and clinical staff, improving the efficiency, quality and safety of patient care, and freeing up clinical staff to focus on frontline service delivery. Following work commissioned by the North of Scotland Regional Planning Group and developed by NHS Grampian, NHS Highland and NHS National Services Scotland (NSS), improvements are being rolled out across Scotland. Video conferencing is boosting the quality of care particularly in rural areas and through telehealth developments, such as the National Telestroke Stroke Network, is providing potentially life-saving services to patients across Scotland and out-of-hours.
WORKFORCE, EDUCATION AND TRAINING
An appropriately trained and motivated workforce is essential to our aims for a modern, quality-driven and patient-centred service. Partnership working involving NHS Education for Scotland (NES), NHS Boards and education providers has, across the spectrum of NHS care, achieved significant gains for practitioners, for those in training, and tangible benefits for patients. This approach to agreeing and developing appropriate training, development and appraisal will provide the fundamental basis for NHSScotland to achieve our Quality Ambitions for safe, effective and person-centred healthcare - particularly focusing on the requirement to ensure that all staff feel supported and engaged in pursuing and achieving world-leading quality healthcare. The workforce contributions to our Quality Ambitions can be found throughout this report but a number of cross-cutting areas of progress and key achievements during 2011/12 are set out here.
2020 WORKFORCE VISION FOR NHSSCOTLAND
The NHSScotland workforce will be central to achievement of our 2020 Vision. In addition to the Strategic Narrative, which sets out the priority areas for action, it will be important to have a clear vision of what the workforce will look like. Work started in January 2012 to develop our 2020 Workforce Vision for NHSScotland. This will be informed by extensive staff engagement, with the intention that it will be published in June 2013.
SCOTTISH CLINICAL LEADERSHIP NETWORK
The Scottish Clinical Leadership Network, hosted by NHS Education for Scotland (NES) National Leadership Unit, was launched in August 2011 to engage and support clinical leaders to deliver sustainable quality. The Network established a Leading Quality Reference Group which now engages a wide range of clinical and non-clinical networks. This 'network of networks' across Scotland is building a critical mass of clinicians and managers who have capacity and capability to lead quality improvement. The Network offers a programme of masterclasses, and action learning and mentoring opportunities to extend clinical engagement, increase return on investment from development programmes and contribute to sustainable improvement in order to realise the 2020 vision and Quality Ambitions. Work is underway to help NHS Boards to identify their clinical and non-clinical staff who have leadership and quality improvement expertise. The aim is to establish local faculties/registers of improvement leaders and to connect these through the 'Network' section on the Quality Improvement Hub website in order to increase the pace of implementation and spread of local and national initiatives.
QUALITY IMPROVEMENT EDUCATION FRAMEWORK
NHS Education for Scotland (NES) launched the Quality Improvement Education Framework to support staff across NHSScotland to access learning in quality improvement thinking and techniques. The Framework reflects the priorities of the Quality Strategy and helps staff learn how to continually improve patient safety, person centred care, and the clinical effectiveness of care and treatment. The Framework enables staff with different roles in an organisation to identify the gaps between their current knowledge and skills and future requirements, and supports them to plan their own learning and development.
REVISED WORKFORCE PLANNING GUIDANCE
Revised Workforce Planning Guidance* was published in December 2011, ahead of the submission of NHS Boards' Local Delivery Plans (LDPs) and Workforce Projections for 2012/13. Contained in Chief Executive Letter (CEL) 32*, this provided clear guidance to assist NHS Boards in planning a workforce which will deliver quality healthcare for patients and a consistent framework to support evidence-based workforce planning. This framework required workforce planning to be integrated with service and financial planning. Analysis of the LDPs and Projections submitted for 2012/13 demonstrates that NHS Boards are following the guidance.
QUALITY IMPROVEMENT
The Quality Improvement Hub (QI Hub) is a national collaboration between Healthcare Improvement Scotland (HIS), Special NHS Boards and the Scottish Government, which aims to build national and local capacity and capability in quality improvement in support of the Quality Strategy, and to support NHS Boards with local implementation. The first Annual Report for the QI Hub* was published in March 2012. During its first full year of operating, the QI Hub received over 30 requests for implementation support and actively assisted NHS Boards and clinicians to design and develop improvement and measurement plans for a range of clinical projects.
* All publications referred to within this document can be found in the publications section of the appendices.
In 2012, the key focus for the QI Hub has been the development and launch of the Quality Improvement Hub website[35], a one-stop-shop for knowledge and implementation support for quality improvement. The QI Hub is currently working to develop a coherent work programme to support NHS Boards with the further implementation of the Quality Strategy.
COMMUNICATION
The need for clear and consistent communication of our vision for high-quality healthcare, and the respective roles of everyone who has a role to play has been identified as being key to the pursuit of our Quality Ambitions. Work has progressed during the year through the work of the Communications Action Group to ensure effective communication with staff, stakeholders and the public. Priority areas for action were identified including revised messaging and refreshed website content. Work has continued with NHS Boards to ensure that the 2020 Vision is communicated and understood, and that the accompanying strategic narrative provides the context for communicating all that we do.
Opportunities were identified to share messages and engage with people through a range of media including media releases, speeches, publications, conferences and meetings. The annual NHSScotland Event continued to provide a major platform to engage with staff across NHSScotland on the Quality Ambitions and the improvements required to deliver safe, effective and person-centred care. The Event has demonstrated the impact of work being undertaken across NHSScotland and has served to share best practice.
Work was begun to consider what is now needed to support a conversation with the public about its role in ensuring quality sustainable services for the future and to support the public engagement work already happening across NHS Boards.
GOVERNANCE
A key priority for supporting the implementation of the Quality Strategy is aligning the key strands of governance - clinical, staff and finance - to ensure that our approach provides NHS Boards, the Scottish Government, Parliament and the public with the assurance required to have confidence in the quality of healthcare in Scotland. Appropriate and focused governance will also ensure that early warning is given of any potential areas for improvement, before any issues arise.
In 2011/12, improvements were made to the way in which NHS Boards are required to submit assurances of their internal control systems. Through their Governance Statements, NHS Board Chief Executives fulfil their roles as accountable officers, responsible for maintaining sound systems of internal controls on quality and performance. The Governance Statement describes four strands of governance and includes clinical and staff governance.
NHS Board Story:
NHS Highland
GROWING QUALITY FROM THE ROOTS UP…†
In March 2011, NHS Highland established a new clinical advisory process with the aim of introducing a robust infrastructure which would provide recommendations on clinical and cost-effective best practice to NHS Highland's Senior Management Team.
A Steering Group and Core Group were set up to focus on areas such as health technologies, treatments and other healthcare developments. Each group is multi-professional and multi-disciplinary in composition. Both groups are collectively known as NHS Highland's Clinical Advisory Group (CAG).
The type of requests received by the groups have been extensive and to date a number of clear processes, protocols and reporting arrangements have been developed which has assured a systematic and transparent approach to clinical decision-making. In addition, positive engagement has taken place with many local and national healthcare colleagues and across organisations.
The work of the CAG continues to deliver a number of encouraging results and outcomes, and many of these have led to more clinical and cost effective practices across NHS Highland. For example, the implementation of a Highland-wide pilot of a Tier 3 Weight Management Service involving specialist dietetic input and the robust management of out-of-area referrals has resulted in the better use of local clinical services and service level agreements.
This robust infrastructure process has led to a number of encouraging results and outcomes which have led to more clinical and cost- effective practices across NHS Highland.
† This work was presented as a poster at the 2012 NHSScotland Event and won first prize in the 'Infrastructure' poster category. To view the poster visit: www.nhsscotlandevent.com/posters/Posters-2012
Contact
Email: Andrew Wilkie