NHS Ayrshire and Arran - redesign of urgent care - pathway finder programme: rapid external review
The National roll out of the Redesign of Urgent Care was informed by a Rapid External Review of NHS Ayrshire & Arran Pathfinder site that went live on 3 November 2020. The review was chaired by Sir Lewis Ritchie and Commissioned by Interim Chief Executive NHS Scotland to monitor preliminary issues.
Annex 3: The Role and Management of Psychosocial Wellbeing in the Redesign of Urgent Care National Programme
Jacques Kerr, Senior Medical Officer, Scottish Government
Craig Whyte, Project Manager, PGMS, NSS
22 November 2020
1. Data from the period 2014-2019 (Information and Statistics Division/Public Health Scotland; ISD/PHS ) have shown an apparent 68.4% uplift in Mental Health (MH) attendances to emergency departments (ED) versus a 4.1% increase in all ED attendances. The table below shows the number of MH attendances and all ED attendances over this period:
| Financial Year | ED Attendances (All Sites) | ED Attendances (Episode Level Data1 ) | MH Attendances 1 | Proportion of Attendances with MH Diagnosis |
|---|---|---|---|---|
| 2014/15 | 1,639,991 | 1,535,934 | 37,944 | 2.5% |
| 2015/16 | 1,606,682 | 1,505,042 | 42,089 | 2.8% |
| 2016/17 | 1,622,272 | 1,522,477 | 45,878 | 3.0% |
| 2017/18 | 1,645,849 | 1,551,190 | 55,456 | 3.6% |
| 2018/19 | 1,691,952 | 1,598,651 | 63,891 | 4.0% |
(1) Patients attending EDs with a mental health diagnosis can only be identified from sites that submit episode level data, the proportion calculation in the table above relates to episode level data. A list of these sites can be found at Public Health Scotland.
2. Performance against the four-hour standard where MH presentations are concerned has gradually deteriorated over the last six months (April-October 2020; data source: ISD/PHS):
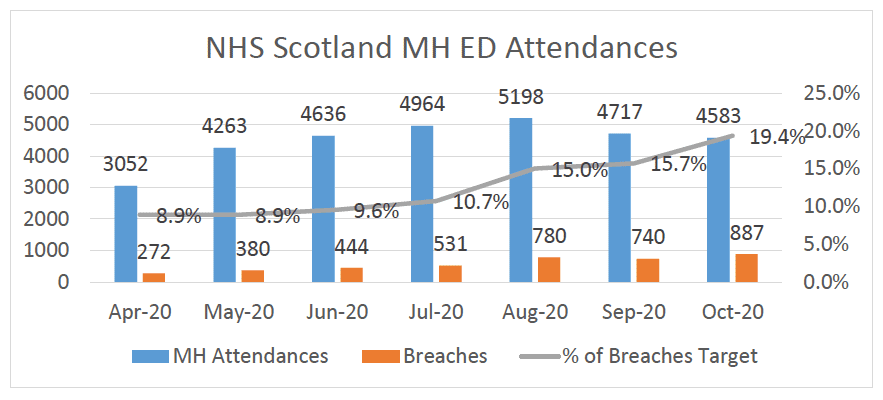
3. The COVID-19 pandemic has had a significant impact, not only on physical health presentations, but also on psychosocial wellbeing as a consequence of the necessary suppression measures resulting in increased social isolation and deprivation. Societal impacts on mental health presentations have been highlighted previously as reported in the Hard Edges Scotland publication from 2019. Affected individuals access services regularly, often through an unnecessarily linear process with multiple hand-offs between Police Scotland (PS), Scottish Ambulance Service (SAS) and Emergency Departments (EDs).
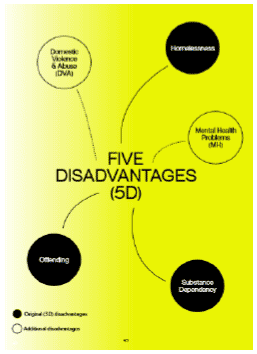
4. As one NHS board-level example, the 'Glasgow 80' are the most 'frequent attenders' who presented to Glasgow Royal Infirmary's (GRI) Emergency Department between October 2018 and September 2019. This cohort accounted for 1,940 attendances to GRI, which represents 1.98% of all GRI ED attendances (total 97,912). At an allocated baseline minimum cost of £206 per attendance, these targetable attendances may be conservatively estimated at a current cost burden of £2,768,846, and with an identified mortality rate within this group of 15% there is a strong moral as well as fiscal case for improving their care.
5. Police Scotland established the Quality of Life Group in the north west of Glasgow in 2016 to help build stronger partnerships with Police Scotland, statutory services, primary care, third sector organisations and a range of private sector housing providers in Glasgow to offer better support to those with complex needs and vulnerabilities around problematic substance use, mental health and social isolation. The QoL Delivery Model has the following four steps:

6. The Redesign of Urgent Care National Programme (RUC) is taking forward the implementation of Flow Navigation Centres (FNCs) across Scotland to divert unnecessary attendances at EDs so that individuals get the right help at the right time from the right service. There is clearly the potential for partner agencies (PS, SAS and acute health) to work collaboratively in the acute management of individuals with complex needs through these new FNCs. This will align with the pledge made in this year's Programme for Government (page 72) to managing distress more effectively in the community across partner agencies:
'We will ensure that services from across our health, justice and social care systems are brought together to focus on the needs of any person experiencing distress, particularly those with multiple complex needs. Our direction of travel is that people in distress with complex needs who find our various systems difficult to access will be quickly identified and supported by a clearer referral pathway to the intervention that they need. We will explore the adoption of a model of support akin to the COVID-19 Hubs used during the pandemic - an immediate and multidisciplinary response, triaging and navigating pathways for appropriate and compassionate care'.
7. The conceptual model put forward by the National Distress Group back in January 2020 illustrates a potential approach which takes in the above initiatives around collaborative working between health, social care, third sector and justice:
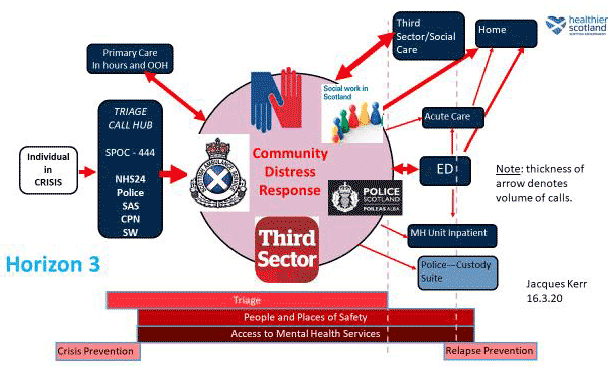
To achieve this operationally will require the following:
1. significant and sensitive change management
2. regular data updates on the activity of the FNCs
3. stakeholder engagement across health, social care and justice with close involvement of partner agencies
4. effective use of linkworkers and the Navigators service to ensure real-time connectivity with appropriate services, rather than defaulting to the current over-medicalised model of care
5. robust and GDPR-compliant data-sharing agreements, both real-time at the point of contact, but also in terms of data analytics
8. Project management began on this work in mid-October and to date the following have been achieved:
a) Stakeholder Engagement
- Regular meetings held with MH leads from the following boards: Ayrshire & Arran, Borders, Forth Valley, GGC, Lanarkshire, Lothian, Tayside and Western Isles. All leads have been positive when taken through the proposed approach and no concerns raised at this time
- Exploration of digital possibilities with Chris Wright (National Advisor for Digital Mental Health) and how technology might be used to enhance the hubs' reach through interconnectedness between boards thus addressing potential resource and workforce capacity issues
- Meetings with the MH and suicide prevention lead, and the Strategic Collaboration Manager, for Police Scotland and an invitation to present to the Assistant Chief Constable and Deputy Chief Constables in early December to develop further engagement across partner agencies as well as adopt an approach that involves co-production
- Engagement with the Criminal Law and Justice Group, chaired by the Chief Executive of Turning Point Scotland, to pioneer tests of change involving those with complex needs.
b) DPIA development
- Calls held with IG Leads to discuss previous attempts at data sharing between services in order to use these as lessons learned for the adoption of the required DPIAs
- Approach agreed to write a national DPIA with principles that must be met to allow Boards to develop local DPIAs in line with their current agreements
c) Navigators
- Multiple sessions held with the Navigator team to understand the reach of their work and the significant difference they can make to people currently stuck in a loop of recurrently attending ED with psychosocial distress
- Introducing the Navigators to MH leads from Boards they currently do not operate in. Ayrshire and Arran have been offered the opportunity to allow a Navigator do some nightshifts to provide them with evidence of what can be achieved
d) Process Mapping
- The development of draft driver diagrams as part of an improvement methodology approach supported by key improvement leads within SG and HIS
- Supporting MH leads in mapping their current pathways and offering advice and solutions on how to improve these by using the Flow Navigation Centres
9. Provisional timelines for the work are predicated on an approach that is person-centred, intelligence-led, assets-optimised and outcomes-focused as per the guiding principles used in the Primary Care Out of Hours Review - Pulling Together: Transforming Urgent Care for the People of Scotland. A draft Gantt chart for the work is given here and is built on a phased approach that places paramount emphasis on the safety and wellbeing of staff and individuals. Given the time taken to construct robust and effective data protection impact assessments it is likely that this will only begin to run operationally from March/April 2021, at the earliest:

10. Key deliverables
- Improved individual & staff experience
- Improved MH metrics such as a reduction in MH presentations at EDs and improved compliance with the four-hour standard
- Reduced police presence in secondary care systems
- Reduced unnecessary ambulance conveyance
- Enhanced compliance with MH Quality Indicators, as per the MH Strategy 2017-27
- Reduced variation - engagement with the Realistic Medicine team around the potential use of atlases of variation will be invaluable here.
Further information -
Any comments should be returned to RedesignUrgentCare@gov.scot and further information is available on the Scottish Government Website.
Contact
Email: RedesignUrgentCare@gov.scot