National health and social care workforce plan: part one
Framework for improving workforce planning across NHSScotland, including the establishment of a National Workforce Planning Group.
Chapter 4 - The changing shape of our workforce
1. Getting the right people in the right place at the right time involves estimating patterns of the demand and supply of health and social care workers. This Plan considers what the future shape our medical and nursing and midwifery workforces will look like going forward.
2. This Plan offers an initial set of projections of future supply and demand. Much evidence already exists, but data is held in different places and does not always use the same metrics. There is scope to improve its co-ordination to give a more sophisticated picture of future supply and demand requirements across all the professions working in NHS Scotland.
3. This will require continued and close working between NHS Scotland workforce planners, service planners and clinical staff in developing scenarios, agreeing planning assumptions and parameters, refining methodologies and sense checking data used for modelling. In doing so, we will be able to take forward work that will assess:
- How known and anticipated pressures affecting demand and supply should be reflected in workforce projections;
- How planning the NHS workforce should reflect medium - and long-term trends in demand for healthcare;
- The potential impact of an ageing workforce and retirement patterns;
- Changing patterns of employment and workforce profile, how these influence supply, and what measures should be used to address them;
- How training, education and supply factors interact, and how they need to continue to evolve in future to address anticipated demand;
- The shift in the balance of care from acute to community settings;
- Inter-sectoral and cross-border flows, taking particular account of the potential effects of Brexit.
4. The answer cannot always be to grow a workforce which accounts for 15% of the total workforce in Scotland. A multidisciplinary and flexible approach should be at the heart of future workforce planning and system sustainability.
5. Scotland currently has good quality data to support workforce planning but as healthcare changes, the methods used to project the future workforce need to be developed further. NHS Boards need to project their future workforce against estimated changes in population demography and health factors, alongside changes in the way healthcare is delivered. The workforce plans they produce must be able to set out the actual expected workforce required, supported by analysis of workforce supply and demand trends, and taking account of available financial resource, including staff costs as part of the overall picture.
6. In Scotland, there is a need to enhance capacity to project future supply and demand, using scenario planning. This is relevant for all employers across health and social care, involving input from economists, service and workforce planners, statisticians and policymakers. There is also considerable scope to learn from the approaches to workforce planning being taken by the OECD [19] and by other health systems in EU countries, such as in the Netherlands [20] and from reviews of those approaches. [21]
7. Along with the other recommendations in this Plan, the National Workforce Planning Group will need to support NHS Scotland workforce planners to develop and refine local and regional workforce forecasts based on future demand and supply. These will inform workforce decisions by:
- providing a national picture to manage and address risks;
- enabling more accurate scenario planning which factors in future population, demand, and workforce supply changes (eg retirals) - informing the care provided to people; and
- informing decisions taken about future skills mix and how multi-disciplinary teams can best work to meet service demands.
Projecting the future workforce
8. Examples of projections for the Medical Workforce and for Qualified Nursing and Midwifery have been included in this plan to highlight the on-going work to model demand and supply. These build on well-established processes and project over a longer timeframe with varying demand and supply scenarios.
9. It should be noted that this modelling work requires further development, reflecting the phased approach involved in achieving improved workforce planning.
10. Although the examples illustrated here are relevant only to the medical and nursing workforces within NHS Scotland, the underlying principles and workforce demand and supply planning technical approaches can also apply to other key groups such as Allied Health Professionals, Nursing and Midwifery Support Staff and GPs.
Projecting the Consultant Medical Workforce 2017-2022
11. Much work has been undertaken in recent years to address challenges in the medical workforce, with workforce numbers expanding. [22] For example, recognising the need for increased speciality numbers, training post numbers have increased by 115 since 2014; for General Practice, training places have increased by 100; and to help meet different working patterns, there has also been an increase so far in part-time training of around 35 extra places to compensate for less than full time. This increase will be adjusted annually.
12. The process of establishing training numbers for medical and surgical specialities is supported by the Medical Specialty Profiles, which offer a single comprehensive source - combining data and triangulating intelligence across the complete range of medical specialties - to give us an understanding of supply and demand drivers across NHS Scotland.
13. The graph below outlines estimated numbers of consultants (headcount) required over the period 2017-2022.
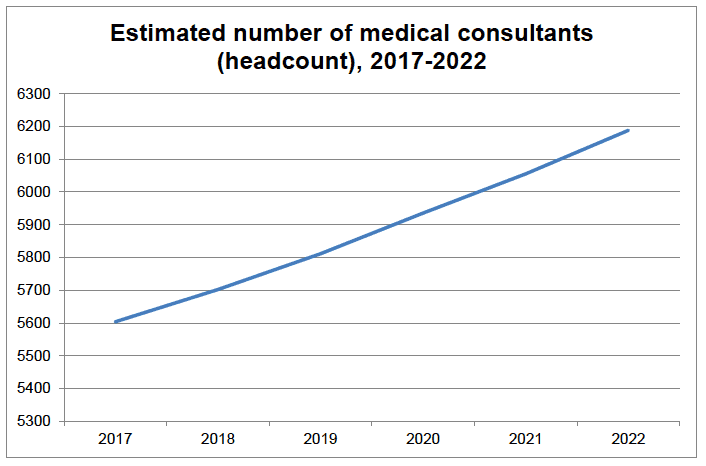
14. It is estimated that we will require around 600 more consultants by 2022. This projection takes account of anticipated annual retirement numbers over the period shown. These generate considerable additional annual demand on consultants which requires to be factored into supply adjustments, taking account of the long lead-time for training.
15. In terms of supply, the numbers of doctors exiting training at completion of clinical training ( CCT) - especially those beyond the immediate horizon of five years - need to be treated with caution as these are based on estimates of CCT (end of training) output. There is also a high degree of variation between the medical specialties.
16. The graph below demonstrates estimated demand, as outlined above, against expected supply from 2017-2022. This is based on consultant output from training across all specialities. It is known that at least 20% upon CCT completion do not take a post in the medical workforce of Scotland. Although these numbers need to be interpreted with caution, they show that the forecast increase in the supply of consultants will continue to meet estimated demand in the period up to and including 2022.
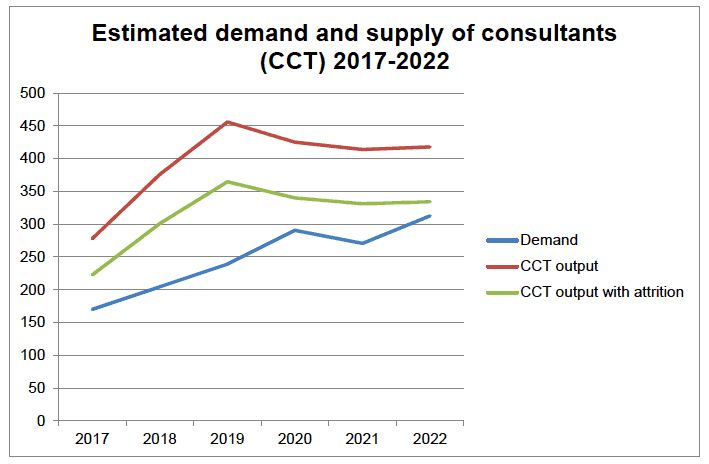
17. Further measures to reduce attrition and increase the overall medical training establishment will help ensure demand continues to be met over the period to 2022, combined with further work to profile the medical workforce being developed between Scottish Government and NHS Education for Scotland. These steps will give added confidence in projecting numbers ahead for the overall consultant workforce.
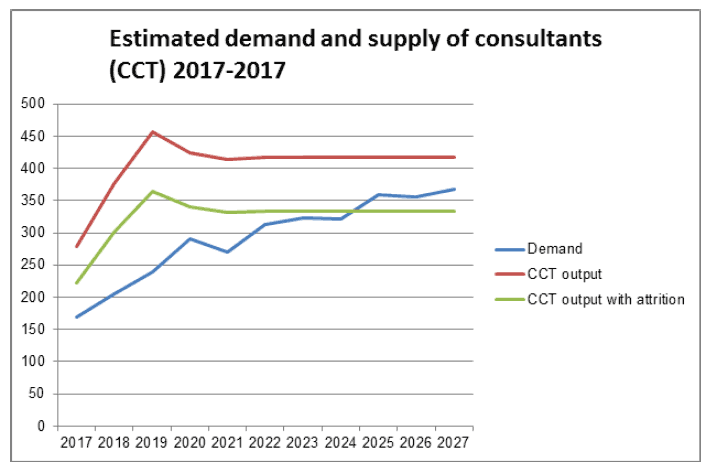
18. However, the long lead times involved in medical training require us to look further forward. Extending the projection for demand and supply of consultants to 2027, as in the graph above, shows that demand for consultants is likely to continue to grow post-2022. To address this trend, more concrete steps therefore need to be taken now. We are therefore increasing the number of overall medical training places available in future years. An additional 40 undergraduate places will derive from the ScotGem programme from September 2018; and between 50-100 additional undergraduate places will also be created across the wider system throughout the course of this Parliamentary term. Taken together, these increases of up to 140 in undergraduate numbers will help to widen access to medical careers; to ensure supply continues to be met, particularly at Foundation and Specialty stages, which are known pressure points; and to take account of the UK-wide approach to increasing numbers over the coming years. The increase is proportionate and logical in the wider UK context, and will be required to support the future consultant and GP workforce for the longer term beyond 2027.
Projecting the Registered Nursing and Midwifery Workforce to 2021/22
19. Nurses and midwives play a vital role in achieving the vision for health and social care, and maximising their role and contribution is the key aim of the Transforming Roles programme of work. There is constant change to the way nurses and midwives work, the work they do, where they work and the people they work with - particularly in taking on new or extended roles, or working as part of multi-disciplinary teams. All of these factors have an impact on the numbers of Nurses and Midwives that will be required in future.
20. The current model for setting annual student intake numbers is being developed to forecast future supply and demand for registered nurses. The model is informed by known demographics for the Nursing and Midwifery workforce, particularly the age profile set out below. A high proportion of nurses and midwives falls within the current retiral band of 55 to 60 years. The model uses recent retiral rates (over four years) to demonstrate the impact of retirals on both supply and demand.
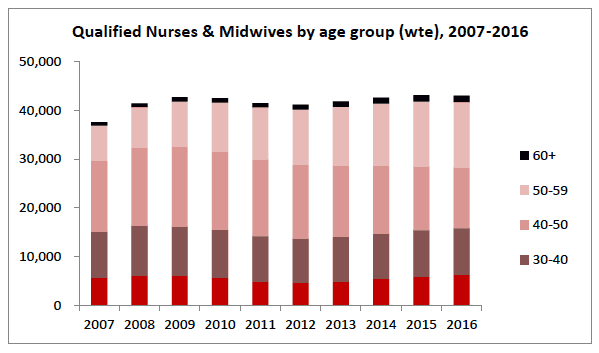
However the Nursing and Midwifery workforce continues to change: while nursing and midwifery is currently perceived as an 'older workforce', longer term demographic trends showing continued growth in the under 30 workforce indicate that supply will eventually need to be adjusted to match demand, should fewer staff retire and work later into life.
21. The model of demand for nurses and midwives is informed by NHS Board workforce projections, and available non- NHS demand data from social care, independent healthcare providers and GP independent contractors. ISD Scotland collects data on current staffing demographics, and NHS Education for Scotland collects data on enrolled student intake/completion rates.
22. The model produces a series of scenarios of required student supply which are shared and discussed with stakeholders in the Student Intake Planning Process ( SIPP) group. In projecting forward to 2020-21, stakeholders' discussion have, for example, focused on the effects on the nursing and midwifery workforce of remoteness and rurality, social care (in particular, care homes) and the potential effects of Brexit. Professional judgement plays a significant role in this process, and recommendations on numbers of commissioned places for pre-registration nursing and midwifery education and training are presented annually to Scottish Ministers.
23. In 2015, recognising some limitations in planning intakes on an annual cycle, Scottish Ministers approved a 3 year cycle for student planning purposes. This longer planning cycle helps to avoid 'boom and bust' scenarios, and helps employers and higher education institutions to consider and indicate their financial requirements over the longer term. The 3 year cycle sets out a 3.5% baseline increase rate, adjustable by +/-2% to take account of the SIPP group's professional judgement and recommendations.
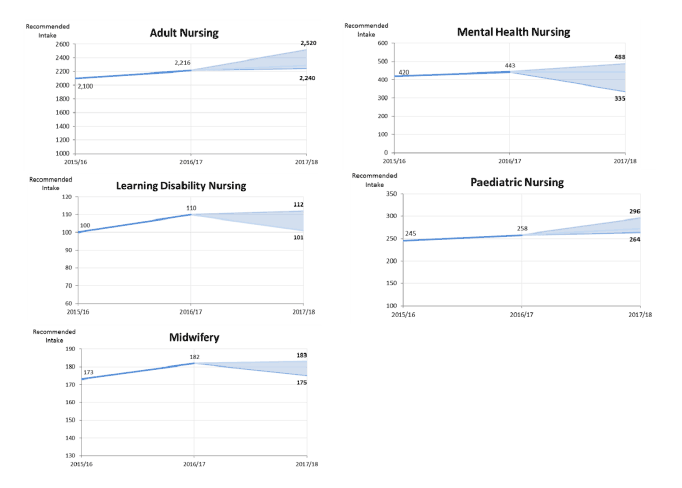
24. For 2017/18 intakes, an overall 4.7% increase was recommended, with effects on each of the main staff categories within Nursing and Midwifery, as follows:
- Adult 5% - increase to 2,326 training places
- Mental Health - 5% increase to 465 places
- Learning Disabilities - status quo at 110 places
- Children's Nursing - 3.9% increase to 268 places
- Midwifery - 4.9% increase to 191 places
25. The diagram below demonstrates the model projections for 2017 intakes for each of the categories, derived from projected workforce demand in 2020-21. The recommended 4.7% increase is towards the higher end of the model, and is the fifth consecutive increase in student intakes.
26. The following diagram sets out the total forecast supply (in 000s) of Nurses and Midwives in the workforce (including NHS, social care and care homes, and Primary Care), projected against three demand scenarios for each year to 2021/22.
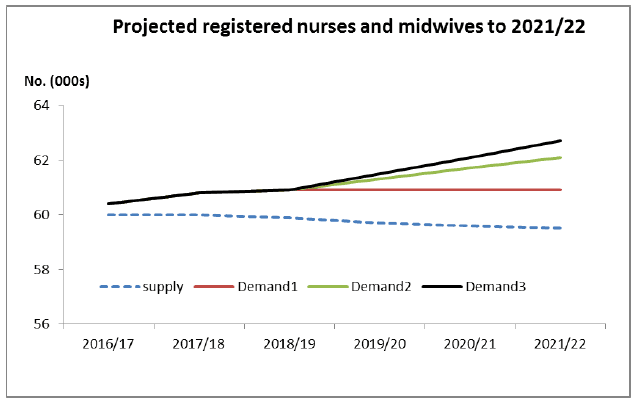
Data source: Scottish Government Health and Social Care Analytics
- Supply - assumed 5% annual increase in student intake
- Demand 1 - NHS Board projections to 2018, thereafter assumed to be constant
- Demand 2 - NHS Board projections to 2018, thereafter assumed to grow by 0.6%
- Demand 3 - NHS Board projections to 2018, thereafter assumed to grow by 1%
27. Current modelling projects that supply [23] , with a 5% annual increase in student intakes, will be sufficient to broadly sustain the current level of total staff establishment in a workforce of around 60,000. The critical years for projected shortfall are 2017-2020 where student intakes cannot be increased in time to balance supply and demand and other measures are required. From 2018-2021, the demand projected can be met by increasing student intakes alongside other actions. From 2021 onwards, we will continue to review the position; supply is expected to increase and demand to decrease.
28. The most likely projection for Scotland's nursing requirement is that demand will increase according to the "Demand 3" line in the diagram above and that 62,400 nurses and midwives (around 2,600 additional nurses and midwives) will be required in the workforce by 2021/22, unless enhanced measures are taken to address demand and increase supply.
29. While some uncertainties remain about ongoing changes to NHS Scotland services and their consequential impact on the Nursing and Midwifery workforce, there is flexibility to increase numbers, and we will therefore take steps to ensure that our supply of nurses and midwives meets anticipated future demand in two ways:
i. To reflect the likely increased demand, further measures will be taken, informed by on-going evidence of demand and supply. The current estimate is that an additional 2,600 nurse and midwifery training places will be created over the next four years. These will include a further expansion of training places during the lifetime of this Parliament to provide an additional 1,600 places, in addition to the 1,000 extra places already anticipated as part of our workforce planning and committed to as part of our Programme for Government 2016-17. This will bring the total number of training places to over 12,000, a historical high.
ii. A further package of measures will extend and increase funding for Return to Practice programmes, enhance access programmes for support workers; improve recruitment, retention and completion rates particularly targeted at remote and rural areas; and support measures to retain and attract nurses and midwives to work in Scotland. These enhanced initiatives are expected to result in a further 1,300 nurses and midwives working in Scotland.
30. The package of measures will be targeted towards those practice and geographical areas where particular needs are identified, including primary care, mental health, midwifery, maternal and child health and more remote and rural areas, particularly the North of Scotland. It will be closely aligned to the Chief Nursing Officer's commission into widening access to nursing and midwifery education and careers and will help deliver its recommendations. The report - which will be produced later in 2017 - will identify best practice and current barriers to nursing and midwifery careers, both in terms of ambition and access, and make recommendations to support and enhance access across the education and employment sectors.
31. This additional supply will give sufficient flexibility for the nursing and midwifery workforce - who will be working longer - to reduce hours of work as they near retirement. It will also enable the workforce to be boosted by younger staff, allowing the additional maternity or parental leave and flexible working they will need to support work/life balance.
32. We are committed to reviewing the model that is designed to estimate the required nursing intake, and further analytical work will be carried out into Autumn 2017. This will help to further refine these projections, and will be an important part of future annual editions of the Plan.
Next steps in understanding the workforce required in future
33. It is important that the right processes are in place to manage workforce supply and demand on an ongoing basis. We will continue to develop our understanding of these projections, reviewing how identified needs are being met through the National Workforce Planning Group.
34. The recent publication of the Mental Health Strategy: 2017-2027 highlighted improved access to CAMHS and other mental health services across Scotland. The publication of this Plan will provide opportunities to develop services further, increasing the mental health workforce by 800 additional mental health workers in our hospitals, GP surgeries, prisons and police stations.
35. The recommendations in this plan will provide a new framework for workforce planning which will help to predict the numbers of staff we will need for the future. This will require further work at local, regional and national levels, via NES and other NHS Scotland bodies, to get a better understanding of future workforce demands, and to introduce a more sophisticated methodological approach to modelling all of this.
36. As well as continuing to refine the student intake modelling process for Nursing and Midwifery, the Scottish Government is developing a more integrated model to scenario plan and carry out workforce projections across the GP workforce, qualified Nursing and Midwifery and the medical workforce, with potential to extend this approach to Allied Health Professionals, who are a key part of the vision for health and social care in the future and are critical to multi-disciplinary team working.
Contact
Email: Grant Hughes
Phone: 0300 244 4000 – Central Enquiry Unit
The Scottish Government
St Andrew's House
Regent Road
Edinburgh
EH1 3DG