National Demand Optimisation Group (Ndog) – Phase 3 Report
The National Demand Optimisation Group (NDOG) is a Scottish Government commissioned group. Its main objective is to reduce unwarranted variation in laboratory diagnostic testing, contributing to improved patient outcomes The group has recently completed its third phase of work.
3 Introduction
3.1 Background
It has been widely accepted and demonstrated that there is considerable variation in the use of diagnostic tests across the NHS[2]. While some of this variation may be attributed to clinical and demographic differences, the degree of variation suggests an element of over/under-requesting, or unnecessary repeat testing. In addition, the lack of availability or awareness of certain tests within some NHS Boards will also limit their optimal use and thus further amplify any variation in use.
Demand Optimisation is defined as the process by which diagnostic test use is optimised to maximise clinical utility, which in turn optimises clinical care and drives more efficient use of associated scarce NHS resources.
The key areas to consider in targeting Demand Optimisation are:
- Minimising over-requesting and under-requesting, both of which can be damaging to patient care.
- Reducing unnecessary repeat requesting.
- Ensuring appropriate and useful test repertoires are universally available across all healthcare outlets.
- Standardisation of nomenclature/test coding to reduce unnecessary variation and allow automated data monitoring systems to extract laboratory test usage information in an efficient, consistent and timely manner.
- Internal standardisation of laboratory practice – to ensure the optimal processes, procedures and testing protocols are adhered to.
Optimisation of rational diagnostic testing may bring about more efficient use of resources within diagnostics, however it is the associated effect on patient care pathways that will ultimately be more valuable. Appropriate diagnostic test use drives appropriate and timely patient diagnoses which impact on subsequent patient flow and treatment and ultimately patient outcomes.
It is also vital to acknowledge that diagnostics and patient pathways interact in complex ways which may not be immediately evident. There may be occasions where sub-optimal tests are used to triage patients to different treatment pathways. It is vital therefore that Demand Optimisation takes a whole systems approach, with open communication and collaboration between laboratories and referring clinicians; to ensure the end to end management of patients using diagnostics is appropriate and optimises NHS resource and patient outcomes.
Demand Optimisation has become a focus programme within the Scottish Government's Healthcare Science National Delivery Plan (NDP). In 2015, the Scottish Government requested that a National Demand Optimisation Group (NDOG) be established to review the third deliverable of the NDP.
The first Phase of Demand Optimisation began in 2016 in order to review existing demand optimisation work, to deliver an improvement plan to optimise diagnostic testing for patients and to support the implementation of the National Clinical Strategy and Scottish Government's Healthcare Science NDP. The extensive report, providing a comprehensive overview of existing demand optimisation and demand management activity within structures across NHS Scotland, was published in 2017[3].
Following publication, diagnostic networks reformed their demand optimisation subgroups or directed their Steering Groups to progress implementation of the report and local arrangements were put in place in some NHS Board areas. However, there was no over-arching, cohesive national plan to progress the recommendations of the report.
The second Phase of Demand Optimisation began in February 2018 and focused on supporting the implementation of the key recommendations identified from the report. This included the regular collection of data that captures diagnostic test requesting activity, presenting it in an easy accessible format, and coordinating with laboratory network clinical leads to initiate and progress quality improvement initiatives. The second report detailing the prototype Atlas of Variation and the many existing quality improvement activities was published in 2019[4].
The development of the Atlas prototype and its potential in identifying unwarranted variation that could facilitate interventions to drive more optimal testing across NHS Scotland was welcomed universally. It was clear that there was a demand to maintain the momentum and implement improvement strategies locally and nationally.
3.2 Group Membership
The multidisciplinary National Demand Optimisation Group (NDOG) was formed to progress Phase I in 2015. During the subsequent life cycles there have been named stakeholder changes, yet there has always been representation from Scottish Government, National Services Scotland and the National Managed Diagnostic Networks. In addition, there has been representation from specific discipline laboratory groups (Biochemistry, Microbiology / Virology, Pathology, Haematology and Clinical Immunology) and from the Genetics / Molecular Pathology consortia. In Phase III, to coincide with the refinement of the Atlas for referring clinicians, there has been consistent representation from primary care. Full details of the group membership can be found in Appendix A.
The group representatives ensured that the work was cascaded through established formal and informal networks to lab users. Engagement with service users was sought throughout the development of the Atlas of Variation and accompanying education materials.
3.3 Governance of the NDOG
The Scottish Government Healthcare Science Officer commissioned the work, Scottish labs teams provided the expertise and NSS provided the resource and methodology to ensure improvements could be replicated and sustained.
The group function as a subgroup of the Diagnostic Steering Group (now Diagnostics in Scotland Strategic Group), reporting into Scottish Government via the Healthcare Science Officer (now via the Chief Healthcare Science Officer). As a new governance structure was developed in early 2020 (see Figure 1 below), the NDOG were represented in discussions.
The governance structure employed in the work was: -
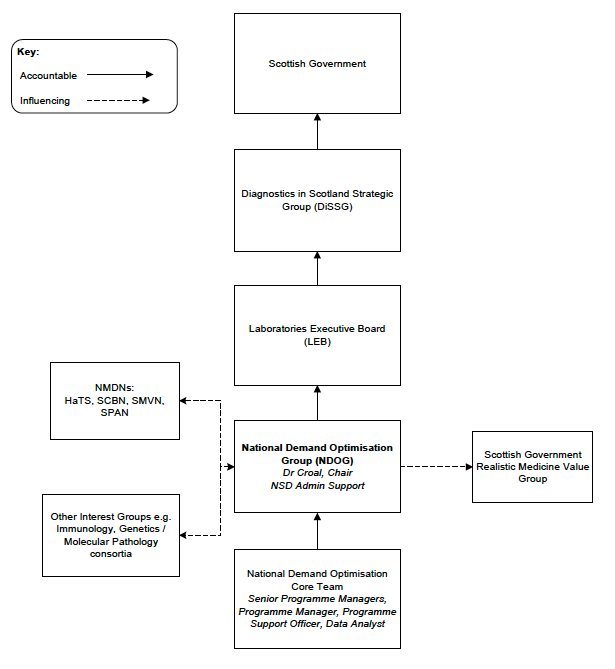
A dedicated website provided additional information and regular bulletins were issued to stakeholders to highlight the work of the NDOG.
Contact
Email: Julie.Townsend@gov.scot