National autism post-diagnostic support service - pilot programme: evaluation
An independent evaluation of national post diagnostic support pilot programme which began in December 2020.
Executive Summary
Introduction and summary of the aims of the pilot project.
Despite the wider awareness of autism among professionals and the public, the process of obtaining an autism diagnosis is reported as protracted, fragmented, and challenging. The immediate post-diagnostic period remains uncertain and difficult, even though individuals and families report that receiving an autism diagnosis is helpful.
Several voluntary agencies across Scotland, led by Scottish Autism, came together as part of a government-initiated pilot to respond to the post-diagnostic needs of families of autistic children, and the needs of adults. Some are led and managed by autistic people. Responses indicate the varied services and activities of these agencies are highly valued by those who use them, and they undoubtedly provide essential support to their communities and to government.
This executive report summarises an evaluation of a pilot programme between 1st December 2020 and 1st June 2021 of the post-diagnostic support services delivered via the following seven agencies.
1. AMASE (Autistic Mutual Aid Society Edinburgh) https://amase.org.uk
2. ARGH (Autism Rights Group Highland) www.arghighland.co.uk
3. AI (Autism Initiatives) https://www.autisminitiatives.org
4. The National Autistic Society https://www.autism.org.uk/what-we-do/scotland
5. Scottish Autism (Get Set 4 Autism) https://www.scottishautism.org
6. Scottish Women's Autism Network (SWAN) https://swanscotland.org
7. Triple A's One Stop Shop Aberdeen (TA-OSS) https://webspace.oss-aberdeen.co.uk
Short summary of the evaluation methodology and process
AT-Autism was commissioned by the Scottish Government to provide an independent evaluation of the effect of NPDS programmes delivered as part of a pilot programme.
The format and processes involved in the evaluation were developed and approved by the Scottish Government and all participant agencies. As part of this, agencies defined their operation and aims and outcomes (PICO). Registrations for all programmes were recorded. For those people who completed the NPDS pilot programme a confidential link would be sent to the evaluation.
Data were obtained via a confidential survey of participants, developed through a Delphi process, with all service organisations acting as the expert panel. The link was sent out by participant organisations to people who had used their services, with the predominant focus on those who had received an autism diagnosis within the past three years.
The survey ran from February 2021 and received 149 responses. All Health Regions are represented except for Orkney (see Fig 1.). The responses comprised quantitative and qualitative data and detailed commentary. The response rate varied between 86% and 20% with an average of 35% across agencies, a confidence level of 95% and a margin of error of 7%.
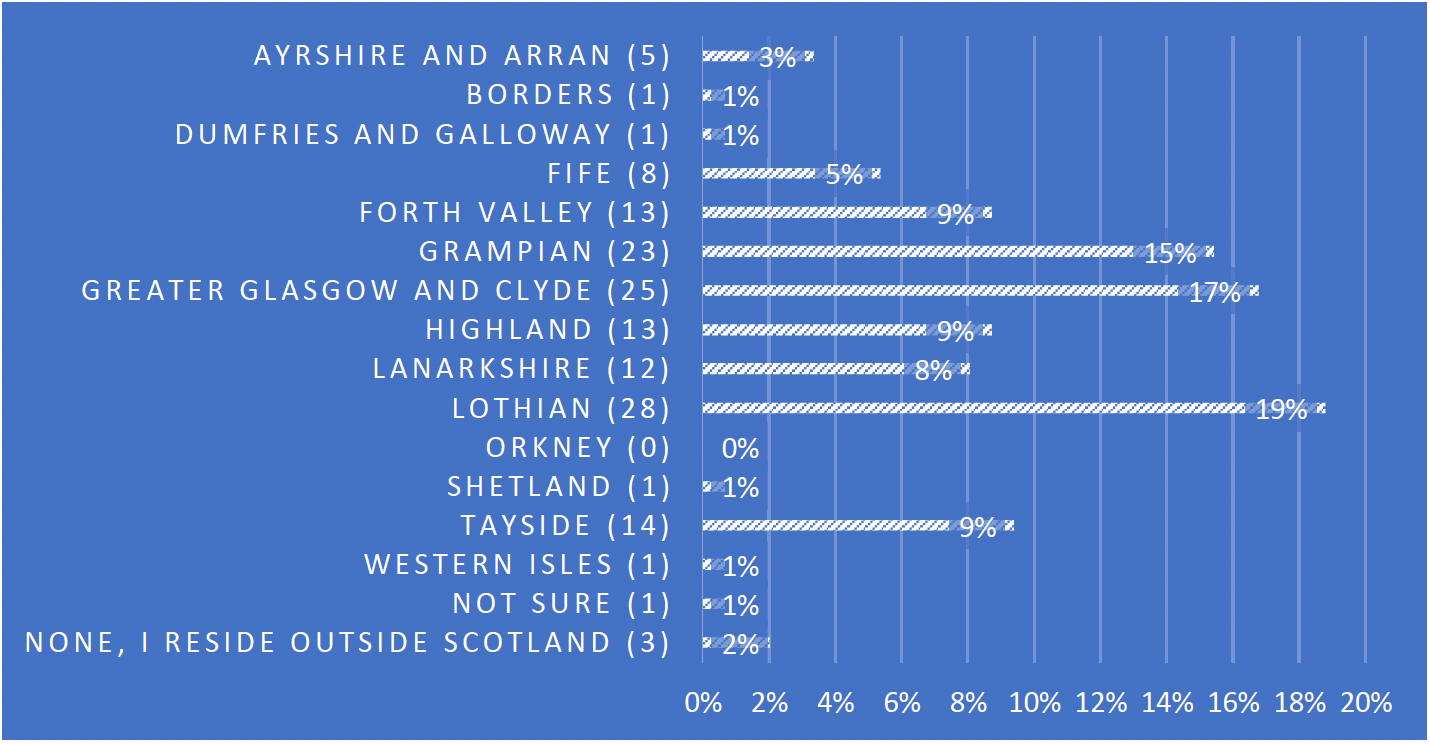
Profile of respondents
- 66% autistic people post 16
- 34% families in respect of a child
- 73% post 16 received diagnosis within past 3 years (M 31%: F 67%: Not declared 3%)
- 88% families received a diagnosis for their child within past 3 years
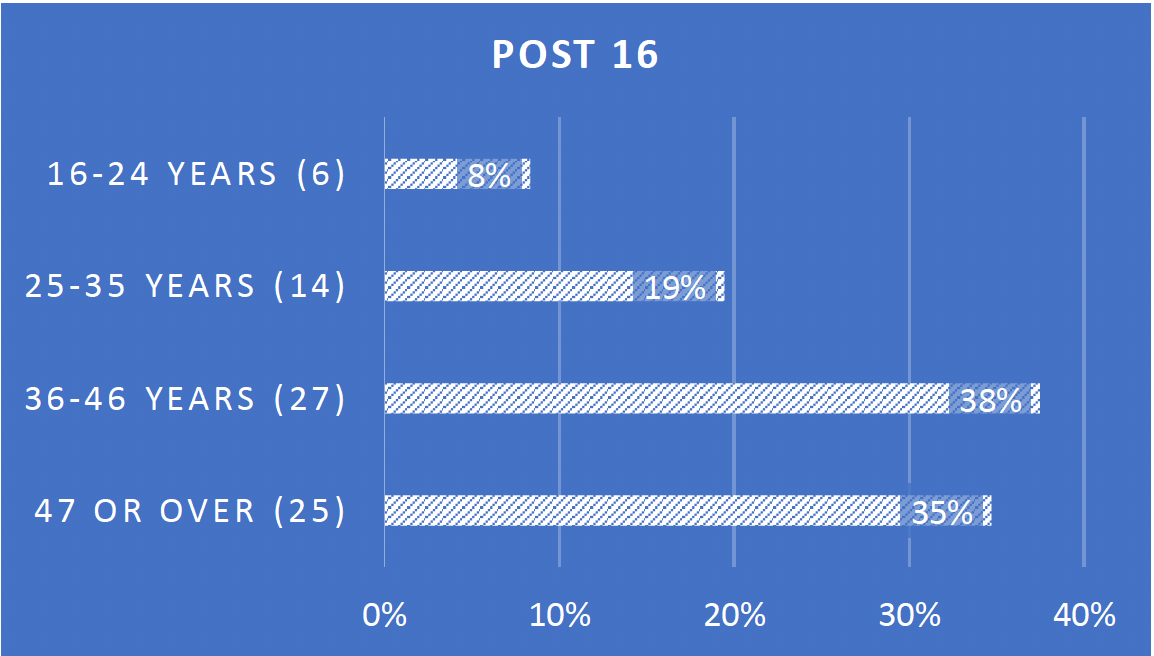
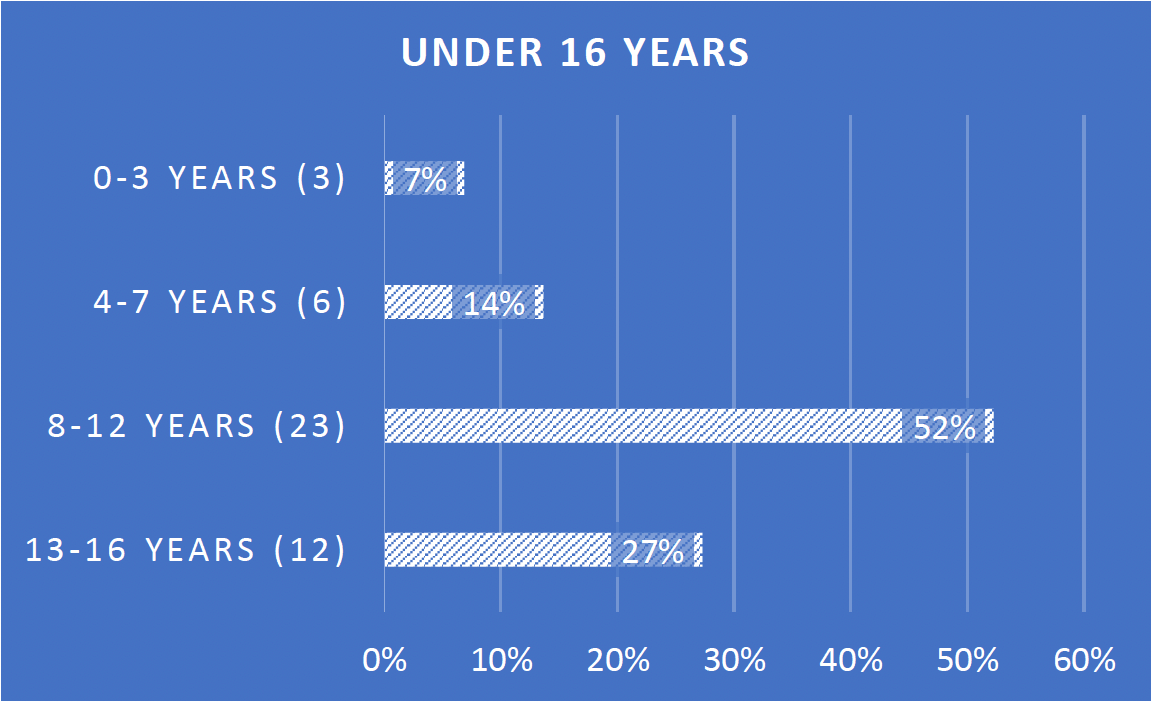
Figure 3: Age at diagnosis (under 16)
Summary of key findings
- Family and adult respondents consistently reported a protracted struggle to obtain recognition and responses. 'A battle' was the term commonly used by families and by autistic adults to describe the often lengthy and stressful process of getting a diagnosis. Many reported the that lengthy delay or concerns about the quality of the process forced them to seek a private diagnosis.
- Significantly, most of those diagnosed as adults were female (67%)
- Frequently, respondents reported they received little practical or emotional help during the process. This confirms the need for pre- as well as post-diagnostic support. But we also had reports where the process was well handled, and these examples can be built upon.
- Several respondents expressed concern about outdated knowledge of many professionals on the nature of autism, particularly in women and girls, and what they experienced as inconsistent, stigmatising, inaccessible, and fragmented diagnostic pathways. They often felt such 'othering' added to their difficulties.
- Respondents reported a lack of support, information or contacts and follow-up immediately after their diagnosis. Many felt 'abandoned' or left in limbo.
- Respondents reported that despite the difficulties, a diagnosis had been helpful to them, on several levels, including navigating future directions, connections, health and wellbeing, identity, education, and work, and in dealing with professionals.
- For many, a diagnosis was self-affirming as they had felt they had self-identified as autistic before seeking a diagnosis. For families, three quarters felt their child was autistic prior to embarking on the diagnostic journey.
- Respondents reported a much more positive experience on the post-diagnostic phase, with most having their expectations fully met, or exceeded, and that the information provided to them was clear and accessible. Most reported that they were listened to. Importantly, a majority reported their goals for what the programme would achieve were fully met or exceeded.
- A significant number felt that their self-confidence and self-esteem had improved since participation in the programme and that they now knew where and how to get further help if they needed it.
- Respondents reported that their connections with other autistic people had increased, and that they had a better understanding of autism and how it impacted them. Others reported a reduction in social isolation and anxiety and developed an improved ability to cope with uncertainty.
- A smaller number of respondents reported reduced stress and improved quality of life and an improvement in general health. A larger number reported improved mental health.
- Almost all said they would recommend the programme that they attended to others.
- It was clear from the comments that the support from other autistic people was a significant plus for autistic respondents, in reducing their feelings of being an 'outsider'. They reported that they finally felt comfortable, understood, and 'a part of something' – in many instances for the first time.
- For families, support in the form of listening and active follow- up was highly valued.
- Gaps in local provision and information were highlighted by many respondents and distance and geographical location was cited as problematic, even though the programmes were delivered remotely.
Sample of quotes from respondents
'It would have been beneficial had there been an NHS autism pathway available for me to access as this would have hopefully offered continued support or referrals after diagnosis and reduced financial burden to myself. I am aware there is one now however this has left me concerned my private diagnosis will no longer be validated based on reports heard from others or private vs NHS which has been a huge source of worry to myself'
'Although I have received a diagnosis, I have felt somewhat abandoned since, with not much support, certainly not from the Health Board'
'Would have loved to have had this service at the time of diagnosis. Instead, we were given a page of links to useful websites'
'We received a same day assessment and diagnosis feedback. This was a fantastic process and we found not having to go away and come back another day. The team at the Vale of Leven Hospital were fantastic and very reassuring'
'We had no idea our daughter was autistic as she was always so sociable. We had been blamed for poor parenting'
'The diagnostic process has added to the damage inflicted. We were handed a piece of A4 with outdated information on it and shown the door – no explanation of what autism was'
' I have found the post-diagnostic service to be a lifeline. I feel much more confident, and brave and can live life on my own terms in this world'
'The (post-diagnostic) support has been life changing. Don't feel alone anymore and really benefitted'
'Some of the professionals I met before the final diagnostic meetings had very outdated information about autism. Particularly about women and girls. There were a lot of stereotypes. I was asked repeatedly why I wanted to be diagnosed and as I am able to mask well in public, I found this really upsetting'
'The service was brilliant throughout. Has improved my understanding of myself and others and my mental health has improved since attending'
'They were so biased against women, and in the diagnosis, there were so many barriers and unpleasant people to navigate as well as a long waiting list so in the end I had to go for a private assessment'
'The programme was well run, in small groups. It was great meeting other adults diagnosed late in life such as myself. I had not met other autistic adults prior to this.'
'We ended up getting a private diagnosis due to struggles getting NHS support'
Contact
Email: suzanne.kinross@gov.scot