Health and Social Care integration: progress review
Final report from the Ministerial Strategic Group for Health and Community Care reviews the progress and draws together the proposals for ensuring the success of integration.
Ministerial Strategic Group for Health and Community Care, Review of Progress with Integration of Health and Social Care - Final Report
Introduction
Since 2016, work has been underway across Scotland to integrate health and social care services in line with the requirements of the Public Bodies (Joint Working) (Scotland) Act 2014. By integrating the planning and provision of care, partners in the public, third and independent sectors are improving people’s experience of care along with its quality and sustainability. Evidence is emerging of good progress in local systems. Audit Scotland’s[1] report on integration that was published on 15 November 2018 highlights a series of challenges that nonetheless need to be addressed, in terms particularly of financial planning, governance and strategic planning arrangements and leadership capacity.
The pace and effectiveness of integration need to increase. At a health debate in the Scottish Parliament on 2 May 2018, the then Cabinet Secretary for Health and Sport undertook that a review of progress by Integration Authorities would be taken forward with the Ministerial Strategic Group for Health and Community Care, and that outputs arising from any further action stemming from such a review would be shared with the Health and Sport Committee of the Scottish Parliament.
Why has Scotland integrated health and social care?
We have integrated health and social care so that we can ensure people have access to the services and support they need, so that their care feels seamless to them, and so that they experience good outcomes and high standards of support. We are also looking to the future: integration requires services to be redesigned and improved, with a strong focus on prevention, quality and sustainability, so that we can continue to maintain our focus on reforming and improving people’s experience of care. In undertaking this review we have built upon Audit Scotland’s observation that integration can work within the current legislative framework, but that Integration Authorities are operating in an extremely challenging environment and there is much more to be done: our focus is on tackling the challenges rather than revisiting the statutory basis for integration.
As part of the review, it is important to acknowledge fully the key importance of staff working across the entirety of health and social care. People working in health and social care services are driving forward many improvements in the experience of care, every day and often in challenging and difficult circumstances. Without the insight, experience and dedication of the health and social care workforce we will simply not be able to deliver on out ambitions for integration. This review does not make recommendations about the health and social care workforce: that work is being undertaken through the National Workforce Plan for health and social care. We nonetheless felt it important to emphasise here the importance of our shared ambitions to develop and support the workforce for integration.
Reviewing progress with integration
As we have reviewed our progress to date, our approach has been to focus on the key questions that matter most to people who use services and the systems we have put in place in order to better support those priorities. We have asked ourselves where we are making progress and where the barriers are that may prevent professionals and staff across health and social care from using their considerable skills and resources to best effect. When the Scottish Government first consulted upon plans for integration[2], it focused on four key objectives, which remain central to our aims:
- Health and social care services should be firmly integrated around the needs of individuals, their carers and other family members
- Health and social care services should be characterised by strong and consistent clinical and care professional leadership
- The providers of services should be held to account jointly and effectively for improved delivery
- Services should be underpinned by flexible, sustainable financial mechanisms that give priority to the needs of the people they serve, rather than the organisations through which they are delivered
The legislation for integration, the Public Bodies (Joint Working) (Scotland) Act 2014, sets out principles and outcomes, which sit at the centre of our ambitions:
Principles of integration: services should[3]:
1. Be integrated from the point of view of service-users
2. Take account of the particular needs of different service-users
3. Take account of the particular needs of service-users in different parts of the area in which the service is being provided
4. Take account of the particular characteristics and circumstances of different service-users
5. Respect the rights of service-users
6. Take account of the dignity of service-users
7. Take account of the participation by service-users in the community in which service-users live
8. Protect and improve the safety of service-users
9. Improve the quality of the service
10. Be planned and led locally in a way which is engaged with the community (including in particular service-users, those who look after service-users and those who are involved in the provision of health or social care)
11. Best anticipate needs and prevents them arising, and
12. Makes the best use of the available facilities, people and other resources.
National health and wellbeing outcomes[4]
1. People are able to look after and improve their own health and wellbeing and live in good health for longer
2. People, including those with disabilities or long term conditions or who are frail are able to live, as far as reasonably practicable, independently and at home or in a homely setting in their community
3. People who use health and social care services have positive experiences of those services, and have their dignity respected
4. Health and social care services are centred on helping to maintain or improve the quality of life of people who use those services
5. Health and social care services contribute to reducing health inequalities
6. People who provide unpaid care are supported to look after their own health and wellbeing, including to reduce any negative impact of their caring role on their own health and wellbeing
7. People using health and social care services are safe from harm
8. People who work in health and social care services feel engaged with the work they do and are supported to continuously improve the information, support, care and treatment they provide
9. Resources are used effectively and efficiently in the provision of health and social care services
The purpose of this review is to help ensure we increase our pace in delivering all of these objectives.
Review process
At its meeting on 20 June 2018, the Ministerial Strategic Group agreed that the review would be taken forward via a small “leadership” group of senior officers chaired by Paul Gray (Director General Health and Social Care and Chief Executive of NHS Scotland) and Sally Loudon (Chief Executive of COSLA). A larger group of senior stakeholders has acted as a “reference” group to the leadership group.
Membership of the review leadership group is as follows:
- Paul Gray (co-chair) (Director General for Health and Social Care and Chief Executive of NHSScotland)
- Sally Loudon (co-chair) (Chief Executive of COSLA)
- Paul Hawkins (Chief Executive of NHS Fife, representing NHS Chief Executives)
- Andrew Kerr (Chief Executive of Edinburgh City Council, representing SOLACE)
- David Williams (Chief Officer of Glasgow City IJB and Chair of the Chief Officers’ network, representing IJB Chief Officers)
- Annie Gunner Logan (Chief Executive of CCPS, representing the third sector)
- Donald MacAskill (Chief Executive of Scottish Care, representing the independent sector)
The work of the review leadership group followed this timetable:
| Meeting date | Topics for discussion |
|---|---|
| 24/09/18 |
Finance: agreeing, delegating and using integrated budgets |
| 23/10/18 |
Governance and commissioning arrangements, including clinical and care governance |
| 27/11/18 |
Delivery and improving outcomes including consideration of the Audit Scotland report on integration (published 15/11/18) |
| 19/12/18 |
Conclusions and agreement on recommendations, to be reported to the MSG on 23/01/19 |
This report draws together the group’s proposals for ensuring the success of integration. It builds upon the first output of our review, the joint statement issued on 26 September 2018, which is at Annex A of this report.
Integration Review Leadership Group
4 FEBRUARY 2019
Audit Scotland report
1. The group recognised that the Audit Scotland report on integration that was published in November 2018 provides important evidence for changes that are needed to deliver integration well. The group noted their agreement with Audit Scotland’s recommendations. The group recommends that these recommendations should be acted upon in full by the statutory health and social care partners in Scotland. In addition, the group noted that workforce issues were not considered in any detail in the audit, but recommends that those should be a key focus for statutory and non-statutory partners taking forward integration.
2. Within a broad context of focussing on improving outcomes for people who use services and delivering sustainable, high quality services, the group noted specifically that exhibit 7 from the Audit Scotland report, reproduced below, provides a helpful framework within which to make progress. The group agreed to set out its proposals, in this report, under the headings identified in the exhibit, each of which was considered fully in turn.
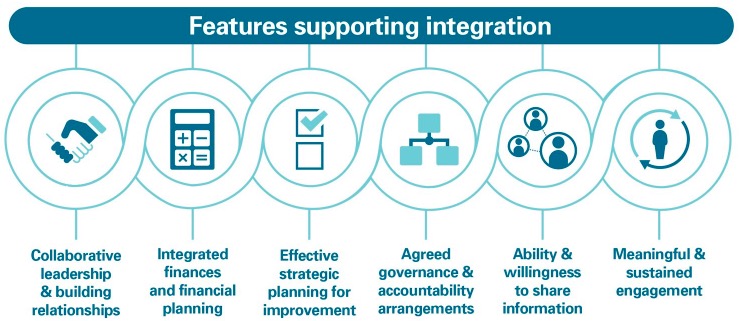
3. As a group, we decided to set out “proposals” in this report rather than “recommendations” to underline that the commitments our proposals make are a shared endeavour, which we are each signed up to on a personal level as senior leaders and on behalf of our respective organisations. We have used “we” throughout the proposals set out in this document to further emphasise this.
4. In our review work, we recognised, as the Audit Scotland report does, that there is good practice developing, both in terms of how Integration Joint Boards (IJBs) are operating, and in how services are being planned and delivered to ensure better outcomes. However, this is not yet the case in all areas. We know there are challenges we must address and want to make use of good practice to drive forward change and reform to truly deliver integration for the people of Scotland.
Leadership Group Proposals
Our proposals focus on our joint and mutual responsibility to improve outcomes for people using health and social care services in Scotland. They are a reflection of our shared commitment to making integration work, set out in our joint statement from September 2018.
1. Collaborative leadership and building relationships
Shared and collaborative leadership must underpin and drive forward integration.
We propose that:
1. (i) All leadership development will be focused on shared and collaborative practice. An audit of existing national leadership programmes will be undertaken by the Scottish Government and COSLA to identify gaps and areas of synergy to support integration of health and social care. Further work will be delivered on cross-sectoral leadership development and support.
Timescale: 6 months
1. (ii) Relationships and collaborative working between partners must improve. Statutory partners in particular must seek to ensure an improved understanding of pressures, cultures and drivers in different parts of the system in order to promote opportunities for more open, collaborative and partnership working, as required by integration.
Timescale: 12 months
1. (iii) Relationships and partnership working with the third and independent sectors must improve. Each partnership will critically evaluate the effectiveness of their working arrangements and relationships with colleagues in the third and independent sectors, and take action to address any issues.
Timescale: 12 months
2. Integrated finances and financial planning
Money must be used to maximum benefit across health and social care. Our aim for integration has been to create a system of health and social care in Scotland in which the public pound is always used to best support the individual at the most appropriate point in the system, regardless of whether the support that is required is what we would traditionally have described as a “health” or “social care” service. Our proposals for integrated finances and financial planning focus on the practicalities of ensuring the arrangements for which we have legislated are used fully to achieve that aim, and to support the Scottish Government’s Medium Term Framework for Health and Social Care[5].
We propose that:
2. (i) Health Boards, Local Authorities and IJBs should have a joint understanding of their respective financial positions as they relate to integration. In each partnership area the Chief Executive of the Health Board and the Local Authority, and the Chief Officer of the IJB, while considering the service impact of decisions, should together request consolidated advice on the financial position as it applies to their shared interests under integration from, respectively, the NHS Director of Finance, the Local Authority S95 Officer and the IJB S95 Officer.
Timescale: By 1st April 2019 and thereafter each year by end March.
2. (ii) Delegated budgets for IJBs must be agreed timeously. The recently published financial framework for health and social care sets out an expectation of moving away from annual budget planning processes towards more medium term arrangements. To support this requirement for planning ahead by Integration Authorities, a requirement should be placed upon statutory partners that all delegated budgets should be agreed by the Health Board, Local Authority and IJB by the end of March each year.
Timescale: By end of March 2019 and thereafter each year by end March
2. (iii) Delegated hospital budgets and set aside requirements must be fully implemented. Each Health Board, in partnership with the Local Authority and IJB, must fully implement the delegated hospital budget and set aside budget requirements of the legislation, in line with the statutory guidance published in June 2015. These arrangements must be in place in time for Integration Authorities to plan their use of their budgets in 2019/20. The Scottish Government Medium Term Financial Framework includes an assumption of efficiencies from reduced variation in hospital care coupled with 50% reinvestment in the community to sustain improvement. The set aside arrangements are key to delivering this commitment.
Timescale: 6 months
2. (iv) Each IJB must develop a transparent and prudent reserves policy. This policy will ensure that reserves are identified for a purpose and held against planned expenditure, with timescales identified for their use, or held as a general reserve as a contingency to cushion the impact of unexpected events or emergencies. Reserves must not be built up unnecessarily.
Timescale: 3 months
2. (v) Statutory partners must ensure appropriate support is provided to IJB S95 Officers. This will include Health Boards and Local Authorities providing staff and resources to provide such support. Measures must be in place to ensure conflicts of interest for IJB S95 Officers are avoided – their role is to provide high quality financial support to the IJB. To ensure a consistent approach across the country, the existing statutory guidance should be amended by removing the last line in paragraph 4.3 recommendation 2, leaving the requirement for such support as follows:
It is recommended that the Health Board and Local Authority Directors of Finance and the Integration Joint Board financial officer establish a process of regular in-year reporting and forecasting to provide the Chief Officer with management accounts for both arms of the operational budget and for the Integration Joint Board as a whole. It is also recommended that each partnership area moves to a model where both the strategic and operational finance functions are undertaken by the IJB S95 officer: and that these functions are sufficiently resourced to provide effective financial support to the Chief Officer and the IJB.
Timescale: 6 months
2. (vi) IJBs must be empowered to use the totality of resources at their disposal to better meet the needs of their local populations. Local audits of the Health Board and Local Authority must take account of the expectation that money will be spent differently. We should be focused on outcomes, not which public body put in which pound to the pot. It is key that the resources held by IJBs lose their original identity and become a single budget on an ongoing basis. This does not take away from the need for the IJB to be accountable for these resources and their use.
Timescale: from 31st March 2019 onwards.
3. Effective strategic planning for improvement
Maximising the benefit of health and social care services, and improving people’s experience of care, depends on good planning across all the services that people access, in communities and hospitals, effective scrutiny, and appropriate support for both activities.
We propose that:
3. (i) Statutory partners must ensure that Chief Officers are effectively supported and empowered to act on behalf of the IJB. This will include Health Boards and Local Authorities providing staff and resources to provide such support. The dual role of the Chief Officer makes it both challenging and complex, with competing demands between statutory delivery partners and the business of the IJB. Chief Officers must be recognised as pivotal in providing the leadership needed to make a success of integration and should be recruited, valued and accorded due status by statutory partners in order that they are able to properly fulfil this “mission critical” role. Consideration must be made of the capacity and capability of Chief Officers and their senior teams to support the partnership’s range of responsibilities.
Timescale: 12 months
3. (ii) Improved strategic inspection of health and social care is developed to better reflect integration. As part of this work, the Care Inspectorate and Healthcare Improvement Scotland will ensure that:
- As well as scrutinising strategic planning and commissioning processes, strategic inspections are fundamentally focused on what integrated arrangements are achieving in terms of outcomes for people.
- Joint strategic inspections examine the performance of the whole partnership – the Health Board, Local Authority and IJB, and the contribution of non-statutory partners – to integrated arrangements, individually and as a partnership.
- There is a more balanced focus across health and social care ensured in strategic inspections.
Timescale: 6 months
3. (iii) National improvement bodies must work more collaboratively and deliver the improvement support partnerships require to make integration work. These bodies include Healthcare Improvement Scotland, the Care Inspectorate, the Improvement Service and NHS National Services Scotland. Improvement support will be more streamlined, better targeted and focused on assisting partnerships to implement our proposals. This will include consideration of the models for delivery of improvement support at a national and local level and a requirement to better meet the needs of integration partners.
Timescale: 3 - 6 months
3. (iv) Improved strategic planning and commissioning arrangements must be put in place. Partnerships should critically analyse and evaluate the effectiveness of their strategic planning and commissioning arrangements, including establishing capacity and capability for this. Local Authorities and Health Boards will ensure support is provided for strategic planning and commissioning, including staffing and resourcing for the partnership, recognising this as a key responsibility of Integration Authorities.
Timescale: 12 months
3. (v) Improved capacity for strategic commissioning of delegated hospital services must be in place. As implementation of proposal 2 (iii) takes place, a necessary step in achieving full delegation of the delegated hospital budget and set aside arrangements will be the development of strategic commissioning for this purpose. This will focus on planning delegated hospital capacity requirements and will require close working with the acute sector and other partnership areas using the same hospitals. This should evolve from existing capacity and plans for those services.
Timescale: 12 months
4. Governance and accountability arrangements
Governance and accountability must be clear and commonly understood for integrated services.
We propose that:
4. (i) The understanding of accountabilities and responsibilities between statutory partners must improve. The responsibility for decisions about the planning and strategic commissioning of all health and social care functions that have been delegated to the IJB sits wholly with the IJB as a statutory public body. Such decisions do not require ratification by the Health Board or the Local Authority, both of which are represented on the IJB. Statutory partners should ensure duplication is avoided and arrangements previously in place for making decisions are reviewed to ensure there is clarity about the decision making responsibilities of the IJB and that decisions are made where responsibility resides. Existing committees and groups should be refocused to share information and support the IJB.
Timescale: 6 months
4. (ii) Accountability processes across statutory partners will be streamlined. Current arrangements for each statutory partner should be scoped and opportunities identified for better alignment, with a focus on better supporting integration and transparent public reporting. This will also ensure that different rules are not being applied to different parts of the system particularly in circumstances of shared accountability.
Timescale: 12 months
4. (iii) IJB chairs must be better supported to facilitate well run Boards capable of making effective decisions on a collective basis. There are well-functioning IJBs that have adopted an open and inclusive approach to decision making and which have gone beyond statutory requirements in terms of memberships to include representatives of key partners in integration, including the independent and housing sectors. This will assist in improving the effectiveness and inclusivity of decision making and establish IJBs as discrete and distinctive statutory bodies acting decisively to improve outcomes for their populations.
Timescale: 12 months
4. (iv) Clear directions must be provided by IJBs to Health Boards and Local Authorities. Revised statutory guidance will be developed on the use of directions in relation to strategic commissioning, emphasising that directions are issued at the end of a process of decision making that has involved partners. Directions must be recognised as a key means of clarifying responsibilities and accountabilities between statutory partners, and for ensuring delivery in line with decisions.
Timescale: 6 months
4. (v) Effective, coherent and joined up clinical and care governance arrangements must be in place. Revised statutory guidance will be developed based on wide ranging consultations with local partnerships, identifying good practice and involving all sectors. The key role of clinical and professional leadership in supporting the IJB to make decisions that are safe and in accordance with required standards and law must be understood, co-ordinated and utilised fully.
Timescale: 6 months
5. Ability and willingness to share information
Understanding where progress and problems are arising is key to implementing learning and delivering better care in different settings.
We propose that:
5. (i) IJB annual performance reports will be benchmarked by Chief Officers to allow them to better understand their local performance data. Chief Officers will work together to consider, individually and as a group, whether their IJBs’ annual reports can be further developed to improve consistency in reporting, better reflect progress and challenges in local systems, and ensure that, as a minimum, all statutorily required information is reported upon.
Timescale: By publication of next round of annual reports in July 2019
5. (ii) Identifying and implementing good practice will be systematically undertaken by all partnerships. Chief Officers will develop IJBs’ annual reports to enable partnerships to identify, share and use examples of good practice, and lessons learned from things that have not worked. Inspection findings and reports from strategic inspections and service inspections should also provide a clear means of identifying and sharing good practice, based on implementation of the framework outlined below at 5 (iii) and the national health and social care standards.
Timescale: 6 - 12 months
5. (iii) A framework for community based health and social care integrated services will be developed. The framework will be key in identifying and promoting best practice in local systems to clearly illustrate what good looks like in community settings, which is firmly focused on improving outcomes for people. This work will be led by Scottish Government and COSLA, involving Chief Officers and other key partnership staff to inform the framework.
Timescale: 6 months
6. Meaningful and sustained engagement
Integration is all about people: improving the experience of care for people using services, and the experience of people who provide care. Meaningful and sustained engagement has a central role to play in ensuring that the planning and delivery of services is centred on people.
We propose that:
6. (i) Effective approaches for community engagement and participation must be put in place for integration. This is critically important to our shared responsibility for ensuring services are fit for purpose, fit for the future, and support better outcomes for people using services, carers and local communities. Revised statutory guidance will be developed by the Scottish Government and COSLA on local community engagement and participation based on existing good practice, to apply across health and social care bodies. Meaningful engagement is central to achieving the scale of change and reform required, and is an ongoing process that is not undertaken only when service change is proposed.
Timescale: 6 months
6. (ii) Improved understanding of effective working relationships with carers, people using services and local communities is required. Each partnership should critically evaluate the effectiveness of their working arrangements and relationships with people using services, carers and local communities. A focus on continuously improving and learning from best practice will be adopted in order to maximise meaningful and sustained engagement.
Timescale: 12 months
6. (iii) We will support carers and representatives of people using services better to enable their full involvement in integration. Carers and representatives of people using health and social care services will be supported by partnerships to enable meaningful engagement with their constituencies. This will support their input to Integration Joint Boards, strategic planning groups and locality arrangements for integration. This would include, for example, receipt of IJB papers with enough time to engage other carers and people using services in responding to issues raised. It would also include paying reasonable expenses for attending meetings.
Timescale: 6 -12 months
In support of these proposals we will:
- Provide support with implementation;
- Prepare guidance and involve partners in the preparation of these;
- Assist with the identification and implementation of good practice;
- Monitor and evaluate progress in achieving proposals;
- Make the necessary links to other parts of the system, such as workforce planning;
- Continue to provide leadership to making progress with integration;
- Report regularly on progress with implementation to the Ministerial Group for Health and Community care.
In support of these proposals we expect:
- Every Health Board, Local Authority and IJB will evaluate their current position in relation to this report and the Audit Scotland report, and take action to make progress using the support on offer.
- Partnerships to initiate or continue the necessary “tough conversations” to make integration work and to be clear about the risks being taken, and ensure mitigation of these is in place.
- Partnerships to be innovative in progressing integration.
Contact
Email: Christina Naismith