Mental health strategy 2017-2027: second progress report
Our second progress report on the Mental Health Strategy 2017-2027.
6. Public Mental Health and Suicide Prevention
Taking a public health approach to mental health recognises that there are a broad range of influences on individual experiences of mental wellbeing. Good mental health is not only the absence of mental illness. Poor mental health can be prevented and a range of support is needed to make sure people can enjoy good mental wellbeing.
Good mental wellbeing is one of Scotland’s six public health priorities. We recognise the inter-related nature of the public health priorities, and see a role for each in improving mental wellbeing. Good mental health can make a significant contribution to achieving a Scotland where:
- we live in vibrant, healthy and safe places and communities;
- we flourish in our early years;
- we reduce the use of and harm from alcohol, tobacco and other drugs;
- we have a sustainable, inclusive economy with equality of outcomes for all; and
- we eat well, have a healthy weight and are physically active.
We recognise that it is important to put mental health and wellbeing at the heart of all policies and to address inequality. Partnership working is needed to make the most of the contribution that a broad spectrum of policy areas, such as environment, economy, culture, education and work, can make to improve the mental wellbeing of the people of Scotland.
Suicide prevention
We continue to take action to prevent suicide in Scotland. The Scottish Suicide Prevention Action Plan: Every Life Matters was published in August 2018. This is the Action Plan through which the Scottish Government, working in partnership, aims to build on progress already made to prevent suicide. Every Life Matters sets out an ambitious aim to reduce the rate of suicide by a further 20% by 2022 (from a 2017 baseline).
We have established a National Suicide Prevention Leadership Group (NSPLG), chaired by former DCC Rose Fitzpatrick. The membership of the NSPLG is broad, including representation from Health and Social Care, Justice, Third Sector, Local Authorities and COSLA as well as clinical professionals, young people and people affected by suicide. Its plan for delivering on the ten actions of Every Life Matters was published in December 2018 and updated in June 2019. We recognise that working in partnership with organisations and those affected by suicide is needed to realise the vision of Every Life Matters. The NSPLG is a key part of this, and will be working in turn with a broad range of delivery partners and voices who are important to this work.
The NSPLG published its first Annual Report on 30 September 2019, describing its work to date and further planned activity, including approaches to local planning and reviews of suicides. The Group made observations on the evidence for a public health approach to suicide prevention, and made 11 recommendations to both the Scottish Government and COSLA. These recommendations were accepted.
Over the coming year, we will be working with partners to develop and promote best practice in local suicide prevention planning. This will include learning from multi-agency reviews of deaths by suicide; extending suicide prevention workforce development; and supporting the implementation of measures to support those in crisis and for those who have been bereaved by suicide.
Delivery Leads from a range of organisations have recently been put in place by the NSPLG to lead on each action within the Action Plan and drive forward work to progress each action. This work will develop over the coming months.
NHS Education for Scotland and NHS Health Scotland have recently produced the first in a range of new mental health and suicide prevention workforce development resources. They will be working over the next year to further develop these for use across different settings. We have asked all NHS Boards to include mental health and suicide prevention training as an essential element of local Workforce Development Plans.
Distress Brief Intervention (Action 11)
The Distress Brief Intervention (DBI) Pilot Programme provides the offer of next day contact with a distress worker from a third sector background to people presenting in distress to A&E departments, police, ambulance services and primary care. The DBI is a time-limited, problem solving approach in four pilot sites for all presentations of distress (including self-harm) that have an emotional component and associated risk, and that do not require alternative emergency service involvement. We are providing £3.4 million to test the DBI programme in four sites: Aberdeen, Inverness, Borders and Lanarkshire.
By mid-October 2019, there had been around 4,500 referrals from front-line services to the DBI Level 2 providers across the four pilot sites (Inverness: Support in Mind; Aberdeen: Penumbra; Borders: SAMH; Lanarkshire: Lanarkshire Association for Mental Health, Richmond Fellowship and Life Link).
An interim evaluation report, undertaken by a research consortium led by the University of Stirling based Nursing Midwifery and Allied Health Professions Research Unit, is to be published in late 2019. It indicates that the DBI programme is:
- developing highly effective cross-sectoral working and extended professional networks both within and across the pilot sites;
- being delivered as intended and is broadly welcomed by all those involved; and
- helping and motivating the majority of individuals who access it to take the first steps in manage their distress more effectively.
Critically, the interim evaluation has evidenced that the DBI service is helping to prevent some suicidal behaviour and as a consequence is saving lives.
Building on Success: The Distress Brief Intervention (DBI) Programme
The 2018 Programme for Government committed to extending the programme to under-18s from 2019 and to establish a DBI Associate Programme for other regions wishing to implement the principles of DBI in existing programmes. Additional funding (£4.5 million in 2018-21) was made available for this extension process. Referrals to DBI became available for 16- and 17- year olds in all four pilots by Summer 2019. The first associate site (Moray) went live in June 2019; discussions are progressing with other regions interested in the associate programme.
Substance use, comorbidity, alcohol minimum unit pricing (Actions 27 and 28)
The delivery of minimum unit pricing for alcohol by Scottish Government was a major international achievement which is projected to significantly save lives and reduce the burden of alcoholic liver disease.
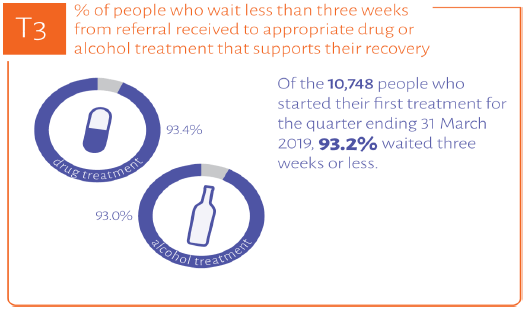
Waiting times for drug and alcohol treatments are included in the Quality Indicator Profile as a measure of whether alcohol and drug services are timely.
NHS Education Scotland produced the Lead Psychologists in Addiction Services Scotland report which describes an evidence-based approach to therapy. Its use has being promoted through seminars to commissioners, managers, trainers and practitioners across all sectors of alcohol and drug services.
As part of a £20 million, two-year funding package to tackle the drug deaths emergency in Scotland, we have committed to establishing joint working protocols between alcohol and drug services and mental health services to improve access, assessment and outcomes from January 2020. We will work with a range of stakeholders from mental health and substance use fields including professional bodies, service providers and commissioners and people with lived experience to develop this work.
In 2020, we will publish a written report on findings, which includes best practice in terms of a joint working protocol, and engage proactively with Integration Authorities to amend or create their own effective protocol. This will include a coordinated offer of peer support to local areas to support local protocol development. We will also make funding available to local areas to support the development of unified and integrated services for people who experience mental health and alcohol and drug problems.
Physical health improvement in those with mental ill-health (including work on activity, screening and smoking cessation)(Actions 29, 30 and 31)
The premature mortality of between 15-20 years in people with severe and enduring mental ill-health is a well-recognised major health inequality, and one of the core areas of focus for the Mental Health Strategy.
The Active Living Becomes Achievable (ALBA) pilot programme run by SAMH received £1 million funding across 2016-19 from the Scottish Government. ALBA aims to increase the physical activity levels for people living with mental and/or physical health conditions, leading to improved mental and physical health and wellbeing (Action 31). The programme was available in Fife, North Ayrshire, and West Lothian. Results from the evaluation of the ALBA intervention are expected to be available in early 2020. We are in discussions with SAMH and, depending on the detail of the evaluation, will consider options for extending or rolling out the programme beyond the three pilot areas.
With respect to Action 29, NHS Boards’ stop-smoking services are now utilising IMPACT guidance on appropriate and effective engagement with people in mental health settings and with people with mental health issues to ensure treatment and support is being prioritised.
To tackle inequality in screening services across Scotland, NHS Boards and third sector organisations, including those supporting people with mental health problems, have been invited to bid for the Health Screening Inequalities Fund. This is a fund set up under the Cancer Strategy to help improve access to screening services. Two projects are currently being undertaken specifically working with people with mental health problems and Stage 2 applications for 2019/20 funding are currently being considered and decisions will be announced shortly (Action 30).