Mental Health in Scotland: Closing the Gaps - Making a Difference: Commitment 13
Mental Health in Scotland: Closing the Gaps - Making a Difference: Commitment 13
Screening, identification and service planning
It is considered best practice for mental health and substance misuse agencies to have assessment procedures which identify co-occurring disorders. Service operational policies should not exclude those with substance misuse and mental health problems, although it may be appropriate to direct referrals to another service as part of an agreed pathway.
Recommendation
2. All services including all substance misuse and mental health agencies should have assessment processes which use an agreed assessment tool to identify co-morbidity systematically and which will help to match care appropriate to level and type of need.
This can be taken forward through the commitments and work streams that have been developed to implement the published 2006 commitments on mental health around integrated care pathways and the work in relation to access to a range of psychological therapies.
The Group identified a number of screening and identification tools for use in a range of situations by staff, at all levels and in all settings. There will be training needs on the application of the tools in each case:
- Identification of Alcohol Misuse. AUDIT;
- Identification of Drug Misuse. DAST-10;
- Mental Health Screening. GHQ-12 or HADS; and
- Alcohol Related Brain Damage. ARBIAS/ SAMH checklist and indicators.
These identification tools are reliable and have been validated in detecting the presence of substance misuse or mental health problems. Properly applied these instruments identify when further specialist assessment is required by appropriately qualified and trained staff. "Referral on" policies will vary between different types of agency. A core principle should be that the client should remain in contact with the original agency until clear transfer arrangements are in place.
While many agencies will have responsibilities, Primary Health Care teams will have a central role in identification, care co-ordination and treatment. The development of this role requires engagement with and support for Primary Care. Doing Well by People with Depression provides a good model of how to achieve this.
Mind the Gaps and A Fuller Life both make recommendations to planners and commissioners to ensure that services are co-ordinated between a wide range of potential agencies. The responsibilities of services must be made explicit and monitored. A whole person needs approach should be adopted including attention to any sensory issues - NHS - HDL (2005) 27 refers.
Primary Health Care has a central role in identification and provision of care. The anticipatory care approach is a promising one in the field of co-morbidity, with its focus on a proactive approach, targeting those most at risk. The role of the Nursing profession in designing, training and delivering brief interventions in Primary Care and other settings, such as Accident and Emergency (A&E) has been valuable and requires continued support and development. The evidence for the effectiveness of primary care interventions for alcohol misuse has been summarised by SIGN but the development of these services has been limited until now.
Where evidence has shown that the uptake of the Enhanced Services for Alcohol Misuse in Primary Care has been effective and delivered tangible change, other Boards and Community Health Partnerships ( CHPs) in discussion with GP practices should consider developing such a service. This would also fit with the principles of SIGN guideline 74 - Management of harmful drinking in and alcohol dependence in primary care.
This anticipatory care approach would be of benefit to those with co-occurring mental health problems and would also link to the work in Delivering for Mental Health around early identification of physical health needs through the work on severe and enduring mental health and the Quality and Outcomes Framework ( QOF) for offering an annual health check and also the links to the work around identifying those with diabetes and coronary heart disease ( CHD) who might be depressed, and in turn matching need with appropriate interventions.
The Group supports the conclusion of Mind the Gaps that a model of identifying lead agency responsibility depending on problem severity is the preferred approach.
The matrix below from the Department of Health Mental Health Policy Implementation Guide - Dual Diagnosis Good Practice Guide is a helpful representation.
Figure 1: The scope of co-existent psychiatric and substance misuse disorders
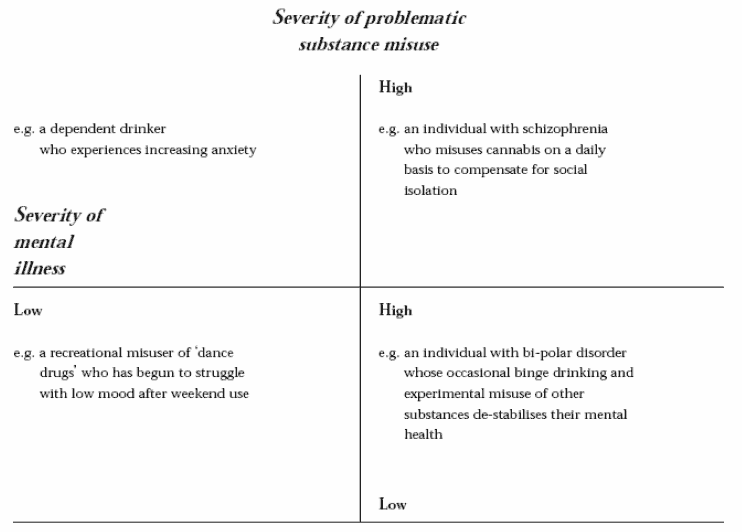
NB: The term "mental illness" includes cognitive impairment such as Alcohol Related Brain Damage ( ARBD).
Poor mental health / Low severity substance misuse
The issues highlighted under the section on Promotion, Prevention and Communications are designed to improve public awareness of the relationship between substance use, misuse and mental health. Frontline agencies in all sectors should provide advice and materials on this topic in order to reduce risk and harm.
Mild/moderate mental illness / High severity substance misuse, including dependence
The high rates of mental health problems in those treated for substance misuse are due to high rates of depression, anxiety and personality disorder (Department of Health 2004). There are strong associations between substance misuse and trauma, eating disorders and self-harm.
The mild to moderate forms of these problems, including ARBD, will be common among those with substance misuse and dependence, and substance misuse services should develop the knowledge, skills and capacity in psychological treatments to respond.
The disclosure of trauma and abuse, in particular sexual abuse, is common during assessment and treatment in substance misuse services. Staff should have skills in handling disclosure sensitively and competently. Some of these skills will be part of the core counselling skills necessary for effective substance misuse work and should be supported by a process of practice supervision.
The advocated stepped care model for psychological therapies will improve the range of expertise and services in Scotland. The established evidence for the effectiveness of specific psychological therapies in alcohol dependence has been reviewed by NHS Quality Improvement Scotland ( QIS) and there is emerging evidence in other areas of substance misuse (National Treatment Agency ( NTA). The stepped care approach, including guided self management, from the Doing Well by People with Depression programme provides valuable principles for the organisation of services by NHS Boards and partner organisations.
The development of evidence based psychological therapies (a further published commitment) will broaden the range of services available to those with mental health and substance misuse problems. Recent reviews have shown the effectiveness of some psychological therapies on substance use behaviour and on broader functioning. ( NTA review, Health Technology Board for Scotland, NICE guidelines). In advancing the principles set out for mental health in Scotland it is important to extend access to include those with co-occurring mental health and substance misuse problems where appropriate.
The personal planning process outlined in the National Quality Standards for Substance Misuse Services will help ensure co-ordination of care where a range of services are involved.
Where appropriate, care packages should take account of the Health and Homelessness Standards (Scottish Government, 2005).
Recommendations
3. Substance misuse services should develop knowledge, skills and capacity in psychological treatments to meet the mental health needs of their client group.
4. These training needs should form part of the plan for psychological therapies currently being developed by NHS Education for Scotland and NHS Boards under the 2006 published Commitment 4 to increase the availability of psychological therapies and in line with the 2007 standard for Integrated Care Pathway ( ICP) for Personality Disorder.
Severe Mental Illness
In the UK, the focus for specialist adult mental health services has been on severe and enduring mental illnesses, in particular schizophrenia and bipolar disorder, though policy statements have signalled an intention to respond to a wider range of disorders. This severe and enduring group have the focus of most attention in the study of co-morbidity in the UK. (Cantwell 2003, Weaver and Tyrer 2004.)
For England, the Department of Health Dual Diagnosis Good Practice Guideline recommends that for people with severe mental illness who misuse drugs, including alcohol, the lead responsibility for care should lie with mental health services. This is described as the mainstreaming model. The rationale for this is that Mental Health services may be better placed to offer services such as assertive outreach, crisis management and long term care. This is supported by the findings of the Scottish Co-morbidity Research Group (Cantwell 2003) which found that those with co-morbidity in contact with mental health services, had levels of health and social functioning similar to other mental health service patients.
Another reason is that the capacity of services for those misusing or dependent on alcohol, stimulants and cannabis, the drugs most often used by those with severe mental illness, is limited. ( CARES).
The needs for substance misuse interventions should be met through a consultative and co-working arrangement with substance misuse services. Advice and support from substance misuse services should be developed to meet the needs of mental health services, specifically to help deal with cannabis and stimulant use.
The priority is that that local responsibilities are clear and the service gap for these vulnerable people and their carers, previously identified in Scotland and elsewhere, is closed. There are a number of ways of organising services to achieve this and existing effective services should be supported. For other areas, the "mainstreaming" model is commended as a reliable approach for service development.
Recommendations
5. NHS mental health services should have the lead responsibility (including lead co-ordinating responsibility) for care of those whose mental health needs are severe and enduring and whose needs are best met within specialist mental health care.
While a recovery focus should be the predominant model, the Chronic Disease or problem model can be a useful approach for some people with co-morbid disorders. Given the terms of the Mental Health (Care and Treatment) (Scotland) Act 2003 access to Advocacy services should be ensured.
There are many examples of successful self and mutual help approaches to recovery, including for partners, children and others. Alcoholics Anonymous and its fellow organisations have been actively working in this way for over 70 years and groups are accessible throughout Scotland.
Individuals with mental health and substance misuse problems should have the same opportunities and needs assessment as other groups who have chronic disease management as individuals with other chronic disorders, for example to the development of an Integrated Care Plan and single point of contact.