Mental Health & Learning Disability Inpatient Bed Census, 2014
Overview of the results of the first Mental Health & Learning Disability Inpatient Bed Census, carried out by the Scottish Government and NHS Boards as at midnight, 29 October 2014. The report provides evidence for Commitment 26 of the Mental Health Strategy for 2012 to 2015, but also enhances the Scottish Government’s and NHS Scotland’s understanding of mental health, addiction and learning disability services, and about the patients who use these services.
1(b). Adult patients in NHS Scotland facilities, by age group

The types of service typically provided to mental health, addiction and learning disability inpatients in Scotland varies depending on the age of the patient. This section splits the adult patients into three age groups: young adults (ages 18-39), older working-age adults (ages 40-64) and older people (ages 65+) - and looks at the differences in provision between the three age groups.
Age breakdown
The following table shows the number of adult mental health, addiction, and learning disability inpatients treated by the NHS in Scotland at the time of the census.
| Category | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| Mental health, addiction & learning disability inpatients | 842 | 1369 | 1648 | 3,859 |
| % of all adults | 22% | 35% | 43% | 100% |
| Population (thousands)* | 1,507 | 1,838 | 947 | 4,292 |
| Patients per 10,000 population | 6 | 7 | 17 | 9 |
*NRS (National Records of Scotland) mid-year population estimates, 2013
- People aged 65+ are more than twice as likely to be a mental health, addiction or learning disability inpatient (17 patients per 10,000 population) than both those aged 18-39 (6 patients per 10,000 population) and 40-64 (7 patients per 10,000 population).
- The higher percentage of the 65+ population who are admitted to a mental health, addiction or learning disability bed can be partly attributed to Dementia. 59% of all patients aged 65+ in the census had a diagnosis of Dementia (more detail is available later in this section).
Ward Type
The number of mental health, addiction and learning disability patients in Scotland staying in different types of ward is shown in the table below. The data shows a clear relationship between the age of the patients and the type of ward they are in.
| Ward Type | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| Acute (General Psychiatry) | 353 | 622 | 635 | 1,610 |
| Continuing care / long stay | 25 | 171 | 825 | 1,021 |
| Forensic | 157 | 198 | 11 | 366 |
| Rehabilitation (non-addiction) | 93 | 163 | 65 | 321 |
| Learning Disability unit | 79 | 92 | 10 | 181 |
| Other | 135 | 123 | 102 | 360 |
| All | 842 | 1,369 | 1,648 | 3,859 |
Some notable findings include:
- 50% of patients aged 65+ are in a continuing care / long-stay setting, compared with 12% of 40-64 year olds and 3% of 18-39 year olds.
- 97% of adults in Forensic Units, 80% of adults in Rehabilitation and 94% of adults in Learning Disability units were aged 18-64.
- The proportion of patients in each age group who are in Acute wards does not vary greatly: 42% of 18-39 year olds, 45% of 40-64 year olds and 39% of those aged 65+ were in an Acute ward.
- The "Other"category includes 29 adults in an Addiction ward. The majority of these patients were aged 40-64, however we are unable to give exact figures due to small numbers in the other age categories.
Ward Security Level
To maintain patient confidentiality, we are unable to publish age group level analysis for Ward Security Level due to small numbers for the 65+ age group in some of the categories. A high-level summary can be found in Section 1 (a) of this report.
Specialty of Consultant
Data on the patients' consultants was also gathered in the October census. The information below shows how the patients in each age group were allocated to different specialties:
| Speciality of consultant | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| General Psychiatry | 502 | 876 | 102 | 1,480 |
| Psychiatry of Old Age | * | * | 1,394 | 1,474 |
| Forensic Psychiatry | 176 | 206 | 12 | 394 |
| Learning Disability | 106 | 110 | 10 | 226 |
| Other | * | * | 0 | 10 |
| Missing** | 53 | 92 | 130 | 275 |
| All | 842 | 1,369 | 1,648 | 3,859 |
*data suppressed due to small numbers
** The "Missing" cases comprise of 217 adult patients from Forth Valley and 58 from Borders with missing data for specialty of consultant.
- 92% of older people were seen by a consultant whose specialty was Psychiatry of Old Age.
- 60% of 18-39 year olds and 64% of 40-64 year olds were seen by a General Psychiatrist.
- 97% of adults who saw a Forensic Psychiatrist, and 96% who saw a Learning Disability specialist, were aged 18-64.
- Percentage figures exclude patients with "Missing" specialty data.
Length of Stay
The length of time a patient can expect to stay in hospital increases with age. At the time of the census, patients aged 65 or over had been in hospital for an average (median) of more than 6 months. This compares with over 4 months for 18-39 year olds and over 5 months for 40-64 year olds (see table below).
| Age Group | Average (median) number of days since admission | Average (median) months since admission (30 days per month) |
|---|---|---|
| 18-39 | 120 | 4 months |
| 40-64 | 160 | 5 months 10 days |
| 65+ | 189 | 6 months 9 days |
| All adults | 163 | 5 months 13 days |
While the above table shows that the average number of days since admission in Scotland was just over 5 months, the following chart provides more detailed analysis of the variation in lengths of stay by age group.
Number of days since admission
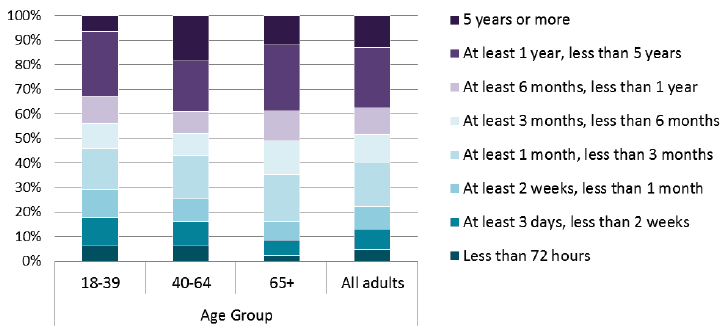
- 18% of patients aged 40-64 had been in hospital for five years or more at the time of the census. This compares with 12% for ages 65+, 6% for ages 18-39 and 13% for all adults.
- Only 2% of those aged 65+ had been in hospital less than 72 hours. This compares with 7% for 18-39 and 40-64 age groups, and 5% for all adults.
The following table shows that patients with a learning disability or autism are likely to have longer stays in hospital than other mental health patients:
| Category | Days / months | Average (median) time since admission, by age group | |||
|---|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | ||
| Patients with a learning disability or autism | Days | 574 | 1,731 | 728 | 986 |
| Months | 19 | 58 | 24 | 33 | |
| Other mental health patients | Days | 80 | 119 | 188 | 141 |
| Months | 3 | 4 | 6 | 5 | |
- The average time since admission for adult patients with a learning disability / autism was 33 months (2 years and 9 months).
- For other adult mental health and addiction patients, the average time since admission was around 5 months.
Self-harm
- 358 patients (12% of all adults in the census for which this information is known) had evidence of self-harm upon admission to hospital.
- 482 patients (17% of all adults in the census for which this information is known) had evidence of actual or threatened self-harm upon admission to hospital.
| Was self-harm a feature on admission? | All adults |
|---|---|
| All patients who have self-harmed | 358 |
| All patients who have self-harmed or threatened to self -harm | 482 |
The following table shows self-harm (actual and threatened) upon admission amongst mental health, addiction and learning disability inpatients by age (note that patients can be in multiple categories in this table):
| Was self-harm a feature on admission? | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| Yes - poisoning* | 26 | 55 | 19 | 100 |
| Yes - injury* | 117 | 130 | 19 | 266 |
| Threatened* | 41 | 57 | 31 | 129 |
| No | 541 | 958 | 1,408 | 2,907 |
| Missing | 127 | 171 | 172 | 470 |
*Note that patients can be in multiple categories - totals do not add up to sum of individual categories.
Please also note, not everyone who self harms will receive inpatient care and not everyone for whom it emerges as an important feature of their illness while they are receiving specialist treatment and care will have that recorded as their main symptom on admission.
Nurse observation level
All patients in mental health inpatient settings will receive some degree of observation. However, levels of observation will vary according to the patients' individual needs. Based on current guidelines[5] the level of observation of patients at the time of the census was also recorded. The three nurse observation levels are:
- "General Observation" - Staff should have a knowledge of the patients' general whereabouts.
- "Constant Observation" - Staff should be constantly aware of the precise whereabouts of the patient.
- "Special Observation" - Patient should be in sight and within arm's reach of a member of staff.
The following table shows that most patients fall under the General Observation category. Please note, NHS Forth Valley were unable to provide data as part of their census return on observation levels for 196 patients.
| Level of observation | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| General Observation | 731 | 1,226 | 1,469 | 3,426 |
| Constant Observation | 54 | 53 | 38 | 145 |
| Special Observation | 13 | 11 | 15 | 39 |
| Not applicable** | * | * | * | 53 |
| Unknown code** | * | * | * | 196 |
| All adults | 798 | 1,290 | 1,522 | 3,859 |
*suppressed due to small numbers.
**196 patients with unknown level of observation codes from NHS Forth Valley.
**'Not applicable' relates either to patients who are being treated in care homes where a nurse observation level may not apply, or patients on pass.
- More than 9 in 10 adult patients (94%, excluding unknown codes) were under General Observation, meaning that staff should have knowledge of the patients general whereabouts at all times. This proportion is similar across all age groups.
- 4% of patients were under Constant Observation. There is also a pattern with age for this category: 7% of adults aged 18-39 were under constant observation, compared with 4% for those aged 40-64 and 3% of over 65s.
- 39 patients were under Special Observation (1% excluding unknown codes).
Selected Conditions
The table and chart below shows adults included in the census with a diagnosis for selected conditions. Patients are included in the analysis as having Dementia or a Learning Disability if they either had a Dementia or Learning Disability diagnosis on admission, or if this was their last known diagnosis (this could be within their current stay in hospital or during a previous stay in hospital). Patients with Schizophrenia, Depression and Personality Disorders are defined as those with a diagnosis within their current stay. For all the selected conditions, primary and secondary diagnosis information was analysed. Note that patients can have more than one condition and diagnosis information was missing entirely for 272 patients.
| Condition | Age Group | ||
|---|---|---|---|
| 18-39 | 40-64 | 65+ | |
| Dementia | * | 77 | 972 |
| Schizophrenia | 318 | 483 | 136 |
| Depression | 55 | 110 | 141 |
| Learning Disabilities | 103 | 116 | 11 |
| Personality Disorders | 74 | 81 | 17 |
*suppressed due to small numbers
Adult patients with diagnoses of specific conditions
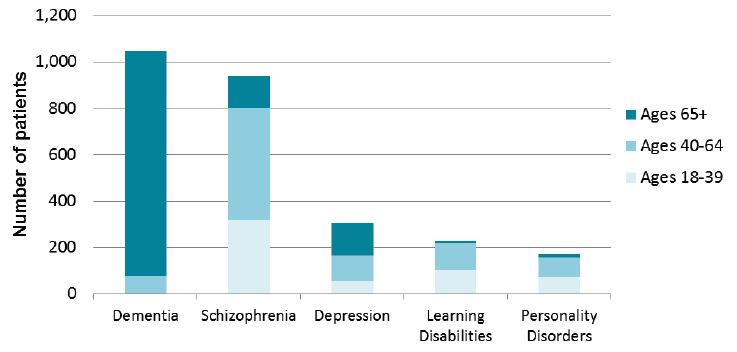
- 93% of Dementia patients were aged 65+. Dementia patients accounted for more than half (972, 59%) of all patients aged 65 or over.
- More than a third (318, 34%) of adult patients with Schizophrenia were aged 18-39. More than half (483, 52%) were aged 40-64 while 136 (15%) were aged 65+.
Drugs and alcohol
There were also some patients in the census who had a (primary or secondary) diagnosis for either Alcohol misuse or Drug misuse within their current stay. The figures are presented in the following tables, although it should be noted that this is likely to be an undercount as a secondary diagnosis information was only returned for around 12% of adults with a primary diagnosis recorded in the census:
| Selected conditions | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| Alcohol misuse | 39 | 101 | 60 | 200 |
| Age Group | |||
|---|---|---|---|
| Selected conditions | 18-39 | 40+ | All adults |
| Drug misuse* | 77 | 53 | 130 |
*Only a small number of adults are in the 65+ age group
- There were 200 patients with a diagnosis of alcohol misuse, around 1 in 20 (5%) of all patients in the census.
- 50% of alcohol misuse patients were aged 40-64.
- There were 130 patients with a diagnosis of drug misuse, around 1 in 30 (3%) of all patients in the census.
- The majority of drug misuse patients (59%) were aged 18-39.
Physical Co-morbidities
Only 6 NHS Boards recorded patients' diagnoses of other physical health conditions in the census, and for some of these boards the numbers are very small which suggests that physical health diagnosis were under recorded. In this report, therefore, we are unable to present accurate results on other health problems experienced by mental health, addiction and learning disability patients. The Scottish Government will work towards improving this data with the NHS Boards in the coming year due to the importance of being able to understand the mental health and physical health of our patients and the implications for service planning.
Source of referral
Information on the source from which the patients were referred to hospital was also gathered in the census:
| Source of referral | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| Community Mental Health Service / Out-Patients | 249 | 448 | 530 | 1,227 |
| Direct Transfer from other Psychiatric Inpatient Care | 194 | 390 | 485 | 1,069 |
| GP | 55 | 82 | 214 | 351 |
| Referral from Non-Psychiatric Inpatient Care | 37 | 68 | 151 | 256 |
| Crisis Service | 61 | 86 | 23 | 170 |
| A&E Department (not admitted to an A&E Ward) | 39 | 74 | 31 | 144 |
| Other | 201 | 207 | 188 | 596 |
| Not Known | 6 | 14 | 26 | 46 |
| All | 842 | 1,369 | 1,648 | 3,859 |
- More than a third of patients (38%) were referred to hospital from a community mental health service.
- 28% (1,069) of adult patients were recorded as being referred to hospital from a direct transfer from other psychiatric impatient care. Note that this may be an over count due to some NHS boards including some patients being transferred from another ward in the hospital in this category. Further work on the guidance for this question in the census will be carried out in 2015.
- There were 351 adult referrals from a GP (around 1 in ten patients). Of these, 214 patients (61%) were for older people.
- 'Other' referral sources include Prison/Penal Establishment, Domiciliary Visit, Judicial (Court), Transfer within the same NHS Board - Specialty Not Known, Local Authority/Voluntary Agency, Police Station/Custody Suite and NHS 24.
Crisis Contacts prior to admission
A "Crisis Contact" is a contact a patient has had with a dedicated Crisis Team / Service. These teams / services provide a period of treatment of an acute psychiatric episode by staff with a specific remit to deal with such situations, in and beyond 'office hours'. This can include alternatives to admission through intensive interventions to support patients in their own environment.
Adult patients in hospital for less than one year, crisis contacts prior to admission
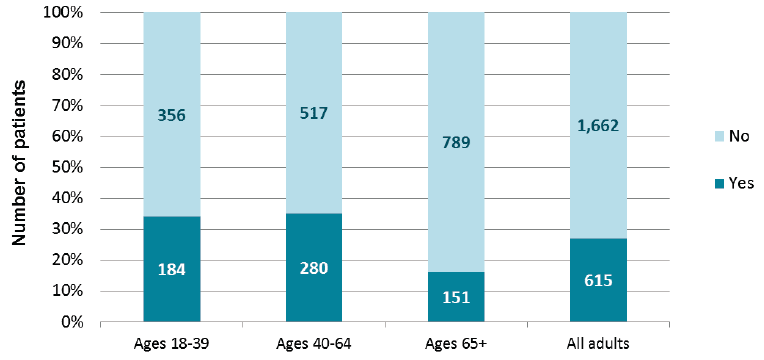
Note: Excludes 132 patients for whom crisis contact information was unknown.
- Around 1 in 4 (27%) adult patients in the census who had been in hospital for less than a year had had at least one crisis contact prior to admission.
- This figure was highest for the 18-39 (34%) and 40-64 (35%) age groups.
Who makes the decision to admit patients?
| Service Decision to admit | Age Group | |||
|---|---|---|---|---|
| 18-39 | 40-64 | 65+ | All adults | |
| Community Mental Health Service | 290 | 531 | 782 | 1,603 |
| Liaison Psychiatry | 115 | 173 | 127 | 415 |
| Primary Care Mental Health Service | 74 | 118 | 159 | 351 |
| Consultant | 30 | 59 | 135 | 224 |
| Crisis Service | 73 | 94 | 27 | 194 |
| Missing / not known | 200 | 324 | 292 | 816 |
| Other | 60 | 70 | 126 | 256 |
| All | 842 | 1,369 | 1,648 | 3,859 |
For those patients for whom it was known which service made the decision to admit them to hospital, over half (1,603, 53%) were admitted on the basis of a decision of a Community Mental Health Service. Around 14% (415) of known cases were admitted as a result of a decision from Liaison Psychiatry.
Delayed Discharges
A 'delayed discharge' is a hospital inpatient who has been judged clinically ready for discharge by the responsible clinician in consultation with all agencies involved in planning the patient's discharge and who continues to occupy a bed beyond the ready for discharge date.
In total there were 251 adult patients in the census who had a delayed discharge, and 29,388 bed days lost as a result. The following charts show that, while the majority of patients with a delayed discharge are elderly, the actual bed days lost as a result of delayed discharges is mostly from younger adults:
Delayed discharges (number of patients and median number of days per patient)
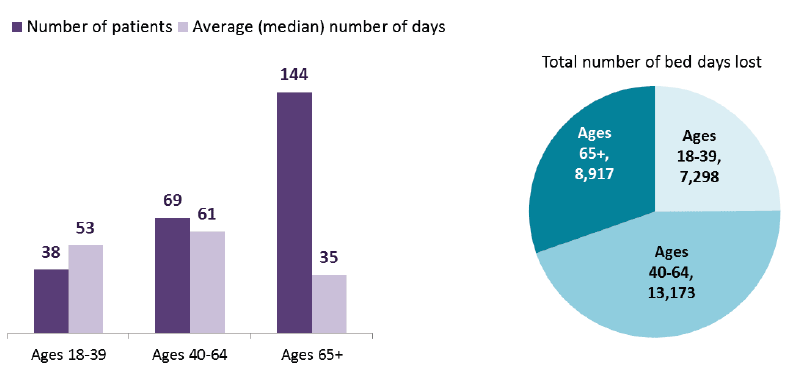
- 144 mental health, addiction and learning disability patients aged 65+ had a delayed discharge. This is 57% of all delayed discharge patients in the census.
- However the 65+ age group only accounted for 30% of all bed days lost as a result of delayed discharge: patients aged 40-64 made up 45% of bed days lost while those aged 18-39 accounted for 25%.
- This is because the delays for patients aged between 18 and 64 tend to be longer than the delays for older people. The average (median) delay for patients aged 65+ was 35 days. This compares with 61 days for patients aged 40-64 and 53 days for those aged 18-39.
Status of patient
A patient had a "formal" status if they were being detained under the Mental Health Act 2003. The following chart and table shows the status of adult patients, at both admission and as at the census date.
| Status of patient: | On admission | Census date | ||||
|---|---|---|---|---|---|---|
| Formal | Informal | All | Formal | Informal | All | |
| 18-39 | 478 | 364 | 842 | 495 | 347 | 842 |
| 40-64 | 665 | 703 | 1,369 | 702 | 667 | 1,369 |
| 65+ | 356 | 1,292 | 1,648 | 298 | 1,350 | 1,648 |
| All adults | 1,499 | 2,359 | 3,859 | 1,495 | 2,364 | 3,859 |
*status on admission information is missing for one client
Status of patients (on admission v census date)
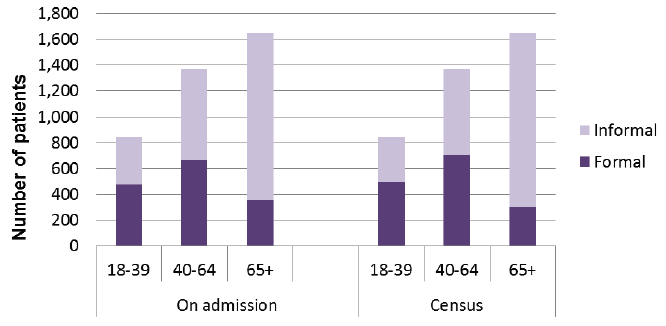
- Patients in the 65+ age group were least likely to have a "formal" status" (18% as at the census date.
- More than half of patients in the 18-39 age group (59%) and the 40-64 age group (51%) had a "formal" status at the census date.
- For the 18-39 and 40-64 age groups, there were more patients with a "formal" status at the census date than on admission. The reverse was true for the 65+ age group.
Contact
Email: David Scott / Ellen Lynch