Coronavirus (COVID-19) initial health and social care response: lessons identified
The report is intended as an illustrative, rather than comprehensive, examination of the response during March to September 2020. The report highlights examples of good practice and also cross cutting themes for further improvement.
Appendix: Case Studies
Case Study
1. Ontario Health – Lab Capacity and Testing in Candada
2. NHS Foundation Trust – Green/Blue Sites in England
3. Primary Care Referral Centre – England
4. Welsh Health Board – Review of Integrated Care in Wales
5. Partnering with Private Hospitals in Australia
6. Patient Activation and Engagement with the public in Israel
7a. NHS Orkney in Scotland
7b. Supporting the Nightingale in England Supply Chain and Global Learnings from Australia
8. Use of TeleHealth to Address Covid-19 Needs in the USA
9. Sustaining Virtual Care in Canada
10. In-House Communications during Covid-19 in England
11. NHS Foundation Trust – Working to a shared vision in England
12. NHS Nightingale – Workforce in England
13. 'Team Time' Initiatives in Ireland and England
14. Welsh Health Board – Findings on Governance in Wales
15. NHSE Elective Service Restoration in England
1. Case Study
Ontario Health – Lab Capacity and Testing in Canada
Challenge
In the midst of the pandemic response, Covid-19 testing in Ontario was lagging behind all other Canadian provinces and territories through a siloed approach involving a handful of disparate providers, creating a critical gap in the province's response to Covid-19. In the context of a growing backlog of samples waiting to be tested, increasing turnaround times (typically 4-6 days) and consistent critical media coverage, from late-March 2020, external support was engaged to diagnose the current state and establish a rapid solution to testing.
This has included supporting Ontario Health in establishing an integrated Covid-19 Provincial Diagnostic Network to coordinate testing provincially and evolved to include all aspects of testing: testing strategy, future capacity requirements, process automation, lab operations, assessment of new capacity ideas and transition planning.
Approach taken
a. Rapid diagnostic assessment
- Conducted a rapid review of the current Covid-19 testing landscape and approaches to immediately expand testing capacity across the province in partnership with Public Health Ontario.
b. Establishing integrated provincial testing network operations
- An integrated provincial testing network was quickly established, later named the Covid-19 Provincial Diagnostic Network, powered by the Covid-19 Provincial Diagnostic Network Operations Centre. The Network Operations Centre (NOC), primarily supported the integrated daily coordination of resources, procurement and test routing for Covid-19 testing in the province through Operational Huddles of all network laboratories.
c. Evolving and sustaining the testing response
- As testing volumes increased, the operations of the laboratory network became more complex. The Provincial Diagnostic Network evolved to refine daily operations but also prepare the network for future waves of Covid-19. The refined approach incorporated two important updates beyond the laboratory network operations: lab capacity strategy and transition planning.
Benefits/Lessons identified
Key learnings from what the local team felt 'worked well' have been captured below. These were deemed to be the 'critical success factors' for an effective testing approach and therefore may provide some insight for local, Scottish responses going forward.
- Leveraging the collective laboratory capacity across the province enabled rapid scaling of testing capacity for the province from 3,000 tests per day capacity to over 40,000 tests per day capacity (more than 13x increase).
- Regular engagement and coordination with all laboratory providers in the network helped share validation approaches to avoid repetitive tasks for each lab, resolve specimen overflow to maximize capacity, gather daily performance metrics and ultimately provide transparency into provincial operations
- Setting clear expectations regarding operational protocols through the Operating Manual and accountability agreements provided mutual understanding of requirements from each laboratory
- Diversification of testing platforms mitigated global supply chain issues to protect provincial testing capacity
- Separation of new ideas intake and assessment from daily operations allowed the laboratories to focus on scaling capacity without distraction from vendors
- Engaging testing experts helped to rapidly provide testing guidance recommendations to the Chief Medical Officer of Health to ensure any Ontarians requiring or wanting a Covid-19 test could get one.
2. Case Study
NHS Foundation Trust – Green/Blue Sites in England
Challenge
As part of the first wave response to the pandemic, a pause on elective procedures provided hospitals with the capacity to treat the increased number of Covid-19 patients without putting non-Covid-19 patients at risk of contracting Covid-19, as well as making staff and facilities resources available. This has led to concerns around a backlog of elective procedures, with an increased challenge as hospitals move into the winter months of dealing with rising Covid-19 cases in addition to trying to maintain elective services.
Approach taken
Having considered options to implement green or blue zones within hospitals to manage the flow of both Covid-19 positive and negative patients, this multi-site hospital made the decision in early May 2020 to designate one of its sites as a 'green site' for cancer, elective surgery and non-surgical procedures. Detailed oversight from Gold command resulted in plans being created for new clinical leadership, governance arrangements, workforce, and Infection Prevention and Control (IPC), with new procedures established to support these areas. Key elements of the approach included:
- Approximately 600 Trust staff and 50-75 third party staff being identified for potential relocation across sites
- Defined protocols for movement, particularly for surgeons, to prevent movement between green and blue sites in the same day
- A programme of asymptomatic staff swabbing on the green site to identify potential carriers;
- A clinical model for five-day-a week operating theatre scaling up to seven days a week; six day working for endoscopy; and transfers of existing chemotherapy patients onto the green site was developed and implemented; and
- The recommissioning of four theatres, an increase in elective care beds, the removal of medical admissions to designated blue sites, and the conversion of A&E into an Urgent Treatment Centre (UTC).
Quality and Equality Impact Assessments were carried out, and the Trust engaged with Trade Unions weekly on proposed changes to the services.
Benefits/Lessons identified
At the time of reviewing current performance for the green site, a series of objectives had been set out and Trust performance against these was as follows:
- Planned surgery was able to resume at a level which maintained the existing waiting list prior to the pandemic. At the time of review, the Trust was able to deliver 90% of the required activity to meet this target, leading to a small increase in waiting lists;
- Cancer targets were significantly met, with referrals to the Trust returning to pre-Covid-19 levels. Patients previously receiving chemotherapy at this site continued to receive treatment, with almost all existing patients from other sites being able to receive treatment at the green site (almost 2,000 patients). Note where patients were not able to transfer this was due to them requiring multiple services (e.g. radiotherapy and LINAC); and
- Urgent endoscopy lists being established meant the Trust had the largest recovery for diagnostic procedures of any hospital in the region.
The Trust also held a patient and staff survey to receive feedback on the approach. 95% of patients who responded felt the Infection Prevention Control procedures in place made them feel either 'fairly safe' or 'very safe', with some practical suggestions for improvement around available facilities for visitors. Staff fed back with additional practical suggestions, including ensuring that sufficient rehabilitation facilities are available within the green site.
3. Case Study
Primary Care Referral Centre – England
Challenge
Patients were being found to be reluctant to attend primary care facilities due to concerns around Covid-19, while those with suspected symptoms were looking for appropriate sites for testing and diagnoses which presented risks to staff and other patients within primary care. This creates a significant risk for both increased transmission of Covid-19 between patients and staff, as well as an increasing back log of unmet need for primary care provision in the community as the public are unable to access care in the same ways they previously had.
Approach taken
As part of the commissioners' response to the shortfalls in primary care capacity, a dedicated Covid-19 Referral Centre (a 'red site' for suspected Covid-19 patients) was stood up at short notice to reduce the potential back log for cases and provide continuity of provision of primary care services to the region. This involved the creation of specific pathways for referral for Covid-19-presenting patients to be referred directly to the centre. Care was provided by a flexible staffing model that could be increased at short notice to manage anticipated demand. Input into the creation of the centre was sought from a multidisciplinary team covering workforce management, logistics, urgent and non-urgent patient transport, IT infrastructure and clinical pathway redesign.
Benefits/Lessons identified
- Construction of a fully functioning triage facility for Covid-19 patients to assess and test patients within three weeks;
- Capacity to treat up to 1,500 patients a day through a newly created pathway (where patients had been referred for Covid-19 symptoms);
- Fully socially distanced, 'drive-through' facility which supported the safety of staff and other patients, while releasing capacity for 'green sites' across the region to continue receiving non-Covid-19 presenting patients;
- Evidence of the effectiveness of 'locality hub' models whereby patients would be willing to travel to centralised hubs for care.
- Recognition of the importance of data infrastructure for temporary/field settings when increasing data sharing across partners and use of digital tools becomes more commonplace in the provision of care.
4. Case Study
Welsh Health Board – Review of Integrated Care in Wales
Challenge
A Health Board in Wales has reflected on how the pandemic has highlighted that population health, care and support is 'everybody's business' and that the response goes beyond in-hospital provision of care. There is therefore a recognition that health and care services are only one part of a complex system that needs to work better together to improve health and wellbeing outcomes across the population.
Approach taken
Following the height of the first wave, the Board led a detailed review of activities undertaken during the response and constituted a new transformation group with representation from health (including primary care) and social and community care to capture and embed best practice from the first wave from June 2020. A key focus was placed on long-term care through a 'social model to health', and through this a number of key outputs were developed including:
- A regional 'Care Home Risk and Escalation Management Policy' approved and implemented by health, Social Care and care providers;
- Region-wide guidance on hospital discharge principles, intermediate care principles, and palliative care principles;
- An integrated end of life pathway, with partnership working between palliative care, nursing home providers, Primary and Secondary Care;
- A District Nursing Hub to coordinate new referrals for district services and to align community nurses where need is heightened; and
- The establishment of a PPE Cell with representation from local authorities, Social Care, domiciliary care, primary care, community services, mental health and learning disabilities and Acute care ensured an integrated approach through mutual aid.
Benefits/Lessons identified
Outcomes from the work done by the Board have been predominantly measured through clinician feedback rather than direct engagement with patients. Clinicians within the system reported benefits including:
- Virtual platforms to communicate with new colleagues to develop relationships and fast-track working together;
- Improved pace and scale of integrated commissioning across three local authorities and the health board; and
- Treatment of 20-30 patients a week through the district nursing hub with a reviewed caseload and workforce planning approach to inform future district nursing models.
- An appreciation of the work of care home staff - clinicians referenced an increased awareness of the shift patterns and conditions that care home staff worked in through closer working. This has led to an increased focus on the sector as part of the wider sustainability of the health system going forward.
5. Case Study
Partnering with Private Hospitals in Australia
Challenge
Facing rising demand for public hospital space in the response to Covid-19, the Australian federal government sought additional capacity from private sector hospitals are part of a national deal.
Approach taken
At the end of March 2020, the Australian Government requested that all private hospitals provide assistance with the Covid-19 response by temporarily integrating with the public hospital network. The Australian Govenrment guaranteed the viability of private sector hospitals temporarily in return for these hospitals making both staff and beds available for the nationwide response. The scope of private hospital involvement in the response included:
- Hospital services for public and private patients;
- Urgent elective surgery;
- Utilisation of wards and theatres for additional ICU capacity; and
- Accommodation for quarantine and isolation cases (where necessary).
As part of this transfer of services, additional support was requested to ensure that all private hospital funding claims were appropriately audited and reviewed for appropriateness; a review of revenue mapping within organisations to ensure improved alignment of claims and transfer of payments; and there were appropriate, new governance structures in place to manage the increased administrative requirement of joint working.
Benefits/Lessons identified
There were two key outcomes to this approach. The first of these was the on-going solvency of the private hospital sector, which had been impacted by Australian Government mandates on reduced elective care. One private hospital group notes that none of its staff were stood down during the pandemic, and instead were made available for the national response.
The second of these was the support provided by the private sector to the public hospitals; the same private group found that it treated over 87,000 public patients between February and September 2020 with over 28,000 procedures performed. Staff from this hospital group also covered 1,500 shifts within aged care facilities to provide additional workforce where needed.
The fact that the national arrangement had been first mandated also allowed a local response, where state governments were able to flex local requirements with private hospital groups based on the national template.
6. Case Study
Patient Activation and Engagement with the public in Israel
Challenge
Even before the additional impact of Covid-19, there is a recognition that healthcare systems globally are under increasing pressure. This is clearly seen within the NHS through a multi-morbid and growing population and a stretched NHS workforce to treat them. As part of this challenge, the largest healthcare provider in Israel has led the way on population health management by focusing on patient activation - the degree of patients' engagement with their own health. A specific focus on this work was on long-term care, with patients with comorbidities, and studies show that in the NHS while these patients spend 1% of their time with healthcare professionals, they account for approximately 70% of NHS spend.
Approach taken
This organisation has placed significant emphasis on social prescribing over the years leading up to the pandemic and how this leads to increased patient activation. These foundations and principles included:
- Ensuring it as simple as possible for patients to engage with healthcare (evidenced by an 81% increase in diabetic patients who attended eye tests when encouraged through an online account created for them compared to those without the online account);
- Ensuring treatment is personalised using algorithms. Patient preferences (informed by previous family medical histories or experiences) are used to target treatment towards their preferred aims and outcomes; and
- The use of apps to allow patients to engage with their own treatment. In Israel this provider launched an app which displayed current patient health information and identified risk factors. The app allowed patients to input lifestyle changes they hope to make, which links back into the health record for clinicians to approve appropriate prescriptions, tests or referrals remotely.
Benefits/Lessons identified
This organisation has reflected on the high emphasis for patient activation in Israel and how this may be applied across the UK to encourage self-management and determine how patients engagement with primary and secondary care in the current climate. These recommendations include:
- Investment in the assets but also skills to encourage patient-centered care. Patient activation starts with patient empowerment to manage their own care and to interact with health systems in a new way;
- Involvement of patients in the process of developing new tools. Co-production will help to support a shift away from organisation-led healthcare and will show patients how they can add value to their own healthcare; and
- Healthcare professionals should be supported to encourage patient activation through all communications. The principle that a patient should leave every encounter with the system more informed and more empowered to take control of their care moves focus away from a reliance on existing hospital or Social Care provision.
7a. Case Study
NHS Orkney in Scotland
The supply chain for all PPE has been under significant strain locally, nationally and internationally however there is now an element of stability in the supply chain with more PPE being manufactured in the UK. This has allowed the supply chain to return to more of a 'business as usual' 'pull model' to support re-mobilisation. As the rurality of NHS Orkney naturally creates delays in the delivery of PPE and essential supplies compared to more urban regions, the Board has made the decision to create a buffer stock of PPE to support any local outbreak of Covid-19 until centralised stocks can be delivered by National Procurement. To further mitigate risk against any local shortages of PPE NHS Orkney is working collaboratively with Orkney Islands Council to mutually support any shortfalls from stockpiles to ensure services can continue to be delivered at point of need. This virtual hub arrangement is shown below and outlines the services that each partner will primarily be responsible for in terms of the supply of PPE.
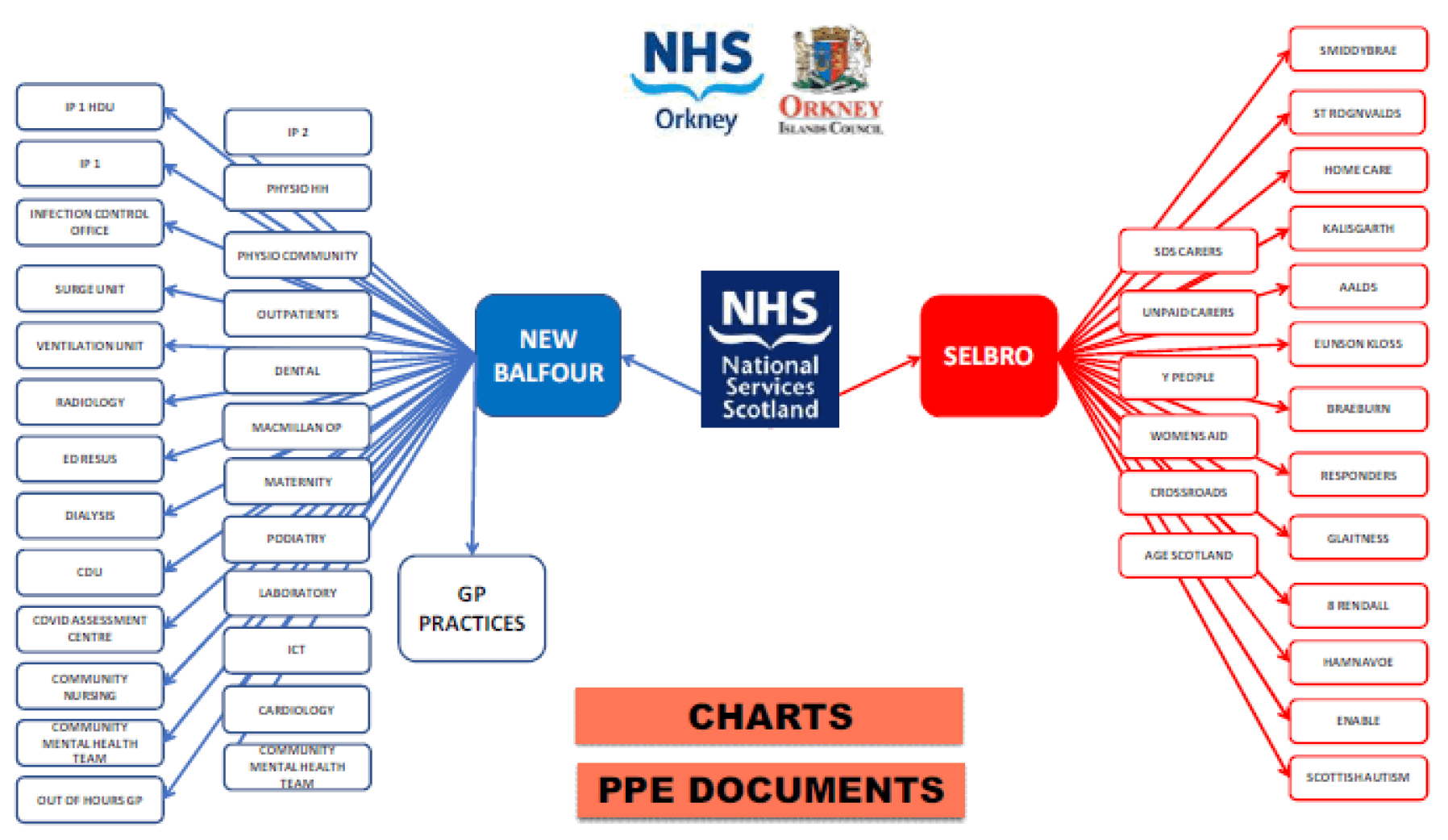
Moving forward the re-mobilisation of services and maintenance of a parallel Covid-19 response means there will be significant demands on PPE for both business as usual and the maintenance of a local pandemic stockpile. As national pandemic stockpiles of FFP3 masks have been used and new and existing manufacturers come on stream NHS Orkney will continue with a rolling programme of face fit testing for staff to ensure that they are matched to a sustainable supply of FFP3 masks. This will ensure that services can be supported to remobilise safely and for the longer term. As part of the winter planning process further sustainable stocks of PPE will be required in order to deliver the broader flu vaccination programme. With the risk of concurrent events (including the potential impact of Brexit on the supply chain) NHS Orkney will continue to work collaboratively with local partners and national procurement to ensure that PPE and essential supplies are available locally and stockpiled to mitigate against the current pandemic and emerging concurrent risks.
7b. Case Study
Supporting the Nightingale in England and Supply Chain and Global Learnings in Australia
Challenge
Historically, the supply chain needs of the NHS have been met locally, via a patchwork of local process and systems which have not been seen as core to the clinically-focused structure of the NHS. The challenge to these systems of the Covid response revealed that the structural issues in those supply chains threatens the NHS' ability to fulfil their mission. These causes include:
- Inconsistent data - the wide range of complex products and services are described in different ways and with different codes.
- The absence of common descriptors and Stock Keeping Units (SKUs) makes it difficult to share information on constrained items (including inventory levels) during a crisis and leverage procurement during 'business as usual';
- Inefficient processes - Processes are highly manual and do not link supply and demand - slowing down the crisis response and significantly reducing agility in the move to a recovery phase;
- Processes and systems vary widely across Trusts, hampering the ability to share information and operate collaboratively at pace;
- Hidden supply chain risk - data and systems issues prevent the easy identification of points of failure (such as over-reliance on a single supplier or country). Systems used to assess risk are backward looking rather than predictive and can't keep pace with rapidly changing situations.
Through engagement with global teams, we are aware that similar work has been compared and contrasted across England and the Australian health service as part of both countries' response to the pandemic.
Approach taken
In London Nightingale, the host trust (Barts Health NHS Trust) developed an emergency escalation hub across the North East London health and care system. Work was undertaken to develop a medium term (12 month) solution, as the initial workforce, logistics and premises solutions were short term. A working group was established to rapidly engage with stakeholders across the system, manage the process, and play an active role in sourcing workforce and logistics solution. Learning from three Nightingale Hospitals (London, Birmingham and Leeds) in sourcing and supplying critical equipment, PPE and consumables indicates that taking the approach below is crucial to success:
- Step 1 - Cleanse Master Data - use of data and analytics to develop clean master data at local / regional level and enable this to be rolled up at a national level (e.g. to provide a clear view of inventory);
- Step 2 - Review and improve Supply Chain resilience - Deploy technology tools to map supply chain for critical items (e.g. PPE, consumables) to build single risk profile;
- Step 3 - Develop & implement Supply Chain technology - Implement cloud-based technologies (best of breed + health specific) to begin to automate key elements of the supply chain process (e.g. replenishment) and allow organisations to collaborate; and
- Step 4 - Implement common processes - implement a suite of standardised processes across organisations to enable better coordination on a regional / national basis
In Australia, teams also highlighted the importance of master data. A significant exercise was undertaken with an Australian state to take the 'historic' PPE list from the health service, review and expand this through engagement with stakeholders to confirm completeness and accuracy of the new list. This exercise provided a significant increase in the granularity of categories available, which supported more informed management decision-making and oversight of existing supplies.
Benefits/Lessons identified
A clear and consistent supply chain strategy is needed to enable healthcare to deliver BAU services as efficiently as possible and enable it to respond to crises like Covid-19 in an agile way. Current supply chain operating model, processes, systems, and data prevent this. There has also been a historical focus on cost rather than supply chain resilience. Benefits achieved and lessons identified from the Nightingale Hospitals in England and through global learnings from Australia include:
- Materials management system is vital
- Making 'a decision' quickly can be better than waiting for a perfect decision when working at pace;
- Clean master data is essential to provide one version of the truth for an organisation's inventory picture.
- Creating a single risk map showing key supply risks (both future and current risks) provides easy oversight;
- Develop common processes, underpinned by technology across organisations to support collaboration;
- Regional or organisational command centres specifically for PPE have worked well in England and Australia;
- Sophisticated data and analytics and visualisation outputs to model demand and supply supports operational decision-making.
8. Case Study
Use of TeleHealth to Address Covid-19 Needs in the USA
Challenge
There are a number of challenges involved with the rapid expansion of telehealth tools in response to the pandemic. Considerations made by this Medical Centre were around how best to expand existing services, identifying sufficient resources to support both the initial demand and on-going consultations using telehealth, how best to integrate telehealth tools with existing health records and what the relevent clinical protocols and patient inclusion/exclusion criteria are to continue treating the right patients safetly.
Approach taken
As part of the response to Covid-19, relevant factors considered included:
- Establishing a governance task force with clinical, IT, administration, marketing and Access representation, with nominated champions for each area across the hospital;
- Reviewing existing cold, flu, and fever clinical and medication prescribing protocols as a basis for Covid-19 protocols;
- Worked closely with marketing teams to develop targeted and general awareness messaging to ensure patients interacted with the system in the right way;
- Rollout of training materials across identified stakeholders (beyond clinicians into access and pathway coordinators) in relevant telehealth tools; and
- Developing logistical plans for primary care, specialty care, ED and urgent care to offer dedicated 'telehealth rooms' within the organisation to promote telehealth to inbound patients.
Benefits/Lessons identified
Through engagement with this medical centre, reported benefits and impacts from engaging with telehealth were referenced as being:
- The launch of a standardised internal process across specialties using one technology platform and data management approaches that integrated with the existing platforms used;
- Alignment between wider access initiatives beyond Covid-19 response into telehealth. A team of triage nurses were embedded within a transfer centre with a focus on referrals across community providers and were able to draw on standardised clinical protocols develop for telehealth to direct patients into new pathways; and
- A well-established governance structure for telehealth to continue operating beyond the first wave response to Covid-19. As a for-profit provider, this included financial analysis and modelling to provide evidence of return on investment for patients engaging through this service.
9. Case Study
Sustaining Virtual Care in Canada
Challenge
As with many other health organisations across the globe, this Canadian health system recognised the increased need for digital healthcare as the pandemic impacted the ability of clinicians to treat patients face to face. In addition, this organisation had not yet implemented Microsoft Teams and therefore had a significant journey to undertake, much like across the UK, to embed digital ways of working both internally and as part of new clinical pathways.
Approach taken
In order to rapidly develop new virtual care pathways, this hospital implemented a 'virtual care pilot' targeted at its respiratory clinic to ensure it would be able to meet the needs of potentially Covid-19-positive patients during the pandemic. A key emphasis was placed on the 'planning' phase of this rollout, with the hospital emphasising virtual care should be treated as if it were a new clinical service, not just a change to an existing service. During this planning phase, the hospital ensured to capture feedback from a wide group of stakeholders, ensuring that patient concerns and queries were at the centre of the design process. As part of this stakeholder engagement, involvement from data privacy teams, clinical records, and patient scheduling were all involved to provide an end-to-end assessment of the new pathway.
Benefits/Lessons identified
Working in conjunction with external advisors, this virtual care pathway has resulted in an updated digital strategy for the hospital, as well as a nine point 'action plan' for considerations on the further introduction of digital into existing services. Key elements of this action plan that could be relevant for NHS Boards include:
- Providing clear channels for patients and service users to give feedback on the process, ensuring this aligns with existing patient experience processes;
- Design virtual care into the patient's end-to-end journey. Patient expectations and cultural sensitivities must be considered when hospitals move towards virtual care.
- Build the use of digital pathways into the performance management process to help embed the change and limit the risk of reverting to previous ways of working for staff;
- Determine the impacts of where any technology or data may be held and how data will be managed. Privacy and cybersecurity processes will become more and more important as pathways become more digitised;
- Develop an awareness and marketing programme for patients and service users which aligns to organisational targets. Service redesign requires patient involvement and specific segments of patient groups should be targeted using different awareness strategies.
10. Case Study
In-House Communications during Covid-19 in England
Challenge
Similar to all organisations during the pandemic, this Trust had to consider how best to communicate with staff to provide them with enough, regular information without overwhelming teams. This involved responding to national guidance as well as providing a source for any staff and family queries or concerns. These challenges covered:
- The postponement and eventual restart of elective activity;
- Patient and family anxiety around delays to accessing services; and
- Staff working remotely
Approach taken
The organisation had previously created a Communications Strategy for 2020, but with the unpredictable environment facing the communications team, this was rapidly reviewed and updated. To react to this changing environment, the team moved to providing a 24/7 press office, with a shift pattern introduced to ensure appropriate coverage of any incoming requests seven days a week. The team also created a series of new resources and materials for staff and the public, while holding different forms of engagement sessions to provide additional information. These included:
- A daily communication issued to staff via 'all staff' mailing lists;
- The launch of an internal Covid-19 Information Hub with over 550 documents available;
- Regular 'Live' broadcasts on MS Teams with over 700 questions answered and a maximum attendance of over 1,000 staff members at once;
- A 'Stay Safe' campaign using large-scale, social distancing floor vinyls, posters, leaflets and banners. This has subsequently been shared with other Trusts in the region with elements being adopted nationally;
- A Covid-19 Public Information Hub, being a single platform for all resources for the public which included visiting details, family support, helplines, education, FAQs and a 'fun' section for children. This has had over 30,000 views; and
- A dedicated 'Coronavirus for Kids' campaign to help reduce anxiety in young people; explaining what the virus is, how it is transmitted and reassuring young people that it isn't their fault if someone they know catches the virus.
Benefits/Lessons identified
The communications team involved were nominated for national awards for communications during the pandemic, and won a Special Award from the Corporate Communications Magazine for their innovations and efforts during the pandemic.
The communications were also well received by staff and patients, with feedback including:
- "Communications truly bring everyone together, and [this approach] has provided rapid and accurate information in a time of constant change" - Staff member (consultant)
- "If it wasn't for the communications team and the support they've given us at an overwhelming time, we'd have been completely lost" - Patient family member
- "They [the team] have supported the delivery and cascade of ever-changing information, provided supportive resources, delivered care packages to the most vulnerable staff and so much more' - Staff Member
11. Case Study
NHS Foundation Trust – Working to a shared vision in England
Challenge
Facing significant competing priorities across regulatory and operational requirements, this NHS Foundation Trust sought to streamline its priorities and make targeted efforts to improve performance in a more meaningful way in a smaller number of areas, rather than trying to improve slightly across a wider range of objectives.
Approach taken
With external support, this Trust sought to:
- Identify a small number of strategic goals to focus on, and create a system to cascade these priorities throughout the organisation to ensure all efforts at all levels were aligned;
- Developed a specific room where performance data was displayed on the relevant metrics. Meetings were scheduled to take place in this room with a multi-disciplinary team to ensure any barriers to problem solving were mitigated;
- Coach frontline teams in a series of skills and tools, as well as a change of mindset, to empower staff who work closest with patients to solve problems they come up against and to embed continuous improvement into daily working;
- Deploy daily 'huddles' within wards and corporate teams for a short, focused meeting on identifying and solving problems. Escalation processes were aligned so these huddles would happen at all levels of the organisation; and
- Realign existing performance management processes to ensure more focus was placed on those areas that were deemed to be relevant for the Trust's strategic priorities.
Benefits/Lessons identified
We note this work is not based on an organisational response to Covid-19, but emphasises key messages raised in document reviews and consultations around the importance of aligning to a few, key tasks rather than tackling a larger number of tasks with less resource and effort. In deploying this approach, the organisation here:
- Had dramatically increased staff engagement scores in all departments;
- Had a 30% reduction in patient falls within three months (one of the strategic priorities);
- Had an 18% increase in theatre start times and 25% increase in breast surgery cases per list;
- Had planned to close 17 out of 34 weekly theatre sessions due to efficiencies, releasing a cost pressure of c.£800k; and
- Was rated 'Outstanding' in all domains by the Care Quality Commission in its latest inspection.
12. Case Study
NHS Nightingale – Workforce in England
Challenge
As part of the national response to the pandemic, the Department of Health and Social Care commissioned a series of 'Nightingale' field hospitals to provide additional surge capacity for either the treatment of high acuity Covid-19 patients, or for convalesence to release existing ICU capacity within local providers. In doing this, additional workforce was required to staff the field hospitals while providers locally were facing challenging workforce planning within their own hospitals.
Approach taken
A number of steps were taken as part of the response to ensure there was sufficient staff available within the field hospitals. These included:
- Aligned with national approaches to reduce staffing ratios for critical care nurses, moving away from 1:1 care towards a 'team-based' approach whereby additional support was provided by non-specialist nurses and healthcare assistants to make the best use of critical care nurse capacity;
- Early agreement of multi-disciplinary team requirements, with sign off from senior clinical leaders across nursing, medicine, pharmacy, allied health, and medical engineering to confirm appropriate staffing ratios for a set number of beds for anticipated pathways;
- Distillation of key skills within each of these roles, with requests for additional support aligned to the skills most needed rather than those roles.
- A daily update of roles to be filled mapped against existing supply of staff, with the number of beds to be opened capped at the maximum supply of safe staffing ratios available. Additional supply was sourced through 'returners' (recent retirees and medical professionals who had recently left the NHS), with a tailored programme of training and onboarding developed to ensure clinical teams were able to meet the agreed skill-mix as approved by senior regional leads; and
- A modelling approach whereby existing headcount across local hospitals was weighted to the total requirement, with hospitals providing staff to the central field hospitals in a proportionate manner. Where any shortfalls were identified, local commissioners and other sources of supply (e.g. volunteers) were engaged to provide additional staff.
Benefits/Lessons identified
At the time of the field hospital being required to open, sufficient staff had been identified to safely support the treatment of the first wave of beds. Training needs and skills mix analyses had been carried out, and a handover of the daily mapping model used to inform the demand modelling.
13. Case Study
'Team Time' Initiatives in Ireland and England
Challenge
Recognising the challenges faced by staff during Covid-19 and the barriers that social distancing might have on being able to obtain personal support within the workplace and outside of this as existing support networks become broken down.
Approach taken
Building on evidence-based 'Schwartz Rounds' as a tool for emotional support within health and Social Care, this organistion supported over 500 people across the NHS in England, HSE Ireland, children's care centres and hospices to become trained in how to implement and run 'Team Time' in their organisations. Team Time is a 45 minute reflective practice that is run and facilitated online to provide staff members with the space and opportunity to share experiences of their work. The audience is limited in size to ensure small groups are able to focus on their emotional and social response to existing work conditions, and this became particularly important during Covid-19 as staff found themselves under significant amounts of pressure. These sessions were facilitated online to allow easy access for teams who might work in community or non-ward settings, and are centred around volunteers telling stories about their experiences and welcoming other attendees to reflect on their experiences alongside this.
Benefits/Lessons identified
This organisation captured qualitatitive and quantitative data from feedbacks to understand the impact of holding these 'Team Time' sessions. Key findings from this quantitative data include:
- 85% of respondents felt the sessions either somewhat or completely made them feel they would work better with their teams;
- 89% of respondents felt they gained insights from the sessions to make them feel more calm and supported back in their day-to-day role;
- 94% of respondents felt they had a better insight into how members of their team felt about their work.
Participant feedback included:
- "[I] Just found it so supportive hearing and knowing that colleagues are facing similar challenges to me and that I am not alone with this struggle."
- "I think it is probably singularly the most important thing we have done for our staff mental and emotional wellbeing during this whole period."
- "Anything that is providing an opportunity for staff to reflect on and to share the emotional impact of work is just invaluable really, and is invaluable for the ripple effect for them to be able to deliver compassionate care".
14. Case Study
Welsh Health Board – Findings on Governance in Wales
Challenge
As with other health and Social Care organisations, this organisation recognised the imminent challenges of responding to the pandemic early in 2020, and devised new governance structures accordingly to provide for as much planning time as possible in advance of the full onset of the first wave.
Approach taken
As expected during the pandemic, the organisation rapidly mobilised. A Covid-19 'tactical group' was initiated as early as the 3rd of February with an informal bronze structure starting to be constituted on the same day. In the following month this tactical group focused on redesigning pathways across community care and paediatrics and working through the relevant workforce challenges this presented. Involvement from the finance team was formalised in late February. Bronze command was formalised on the 4th of March with focssued groups covering community care, primary care, Acute care and workforce to provide clear operational oversight of these areas.
Benefits/Lessons identified
Early planning has been cited as a key driver for a more efficient response. Having consulted with staff members involved in the first wave however, this organisation identified the following lessons. These cover both things that staff members reflected positively and negatively from the newly-constituted governance structure, and may serve for guidance for Scottish Government over the coming weeks and months:
- Staff felt having a clear structure worked well, everyone knew when the meetings were happening, who was involved in the meetings, and how decisions would be made;
- There was a specific focus on the Bronze groups as being 'problem solving' areas. The thematic nature of these groups meant problems were first escalated here and could be solved rapidly without further escalation; and
- Staff cited the fact that the framework of the command structure provided autonomy and 'freedom to act'. Decisions did not need detailed reports, and a multi-disciplinary membership on the command meetings meant that local decisions were made by local teams.
- There was however a feeling that Bronze teams were not necessarily connected with each other. Being organised by care group meant that while each group was able to act as a specialist in its own area, this created an element of 'silo working' and limited the ability to join up across pathways; and
- Some people noted a disconnect between Gold decisions and frontline delivery which impacted the ability for frontline teams to act.
15. Case Study
NHSE Elective Service Restoration in England
Challenge
The Adopt and Adapt programme is one of a number of key initiatives established to increase the pace at which the NHS in England recovers from the elective backlog. There are a number of challenges in recovering activity that are consistent across systems globally, and in this context the programme specifically considered:
- Delivering activity with revised Infection Protection Control measures;
- A backlog of demand from the pause of routine work during Phase 1, which resulted from changes in Public Health-seeking behaviours, access to primary care and referral services, and access to secondary care; and
- The available workforce capacity to continue to respond to the pandemic and increased planned activity while taking enough rest and recovery in order to maintain a sustainable response.
Approach taken
Adopt and Adapt focussed on five key service areas/pathways within planned care: Endoscopy, CT & MRI, Outpatients, Theatres and Cancer. The programme then worked with one region for each of these pathways to:
- Quantify a specific objective (defined broadly as the gap between pre-Covid and current activity levels);
- Run rapid problem-solving workshops with Subject Matter Experts, regional and national stakeholders, and clinicians to brainstorm 'big ticket' solutions that could be implemented rapidly;
- Complete further regional engagement with systems and frontline teams to refine ideas, develop system-level plans and establish a standardised programme approach;
- Share 'blueprints' from each of the five regions across the remaining regions to share best practice and solutions.
To take the example of the Endoscopy programme (focused on NHS London), specific interventions identified to support the immediate recovery of capacity included:
- Splitting upper and lower GI lists to boost productivity of lower GI (as upper GI 'aerosol-generating' procedures required additional IPC requirements;
- Expanded use of trans-nasal endoscopy and CT Colonoscopy;
- Region-wide sessional rates agreed for Waiting List Initiatives to encourage evening and weekend work;
- Role redesign to explore clinical support workers being redeployed to allow clinical teams to operate at the top of their licenses;
- Immersive training programme for ST5-7s and a targeted CT Colonoscopy training course agreed with Health Education England to increase the number of endoscopists able to practice independently.;
- Passporting arrangements across the system to allow endoscopists to work in multiple settings; and
- Maximised use of the independent sector for additional capacity (up to 32 rooms).
Benefits/Lessons identified
Based on the above approach, specifically looking at the actions within Endoscopy, the following benefits were achieved:
- Data shows activity in London at 90% of historic levels (believed to be underreported and actually closer to 100%);
- 5,000 procedures being completed a week; and
- Daily reporting showing the waiting list having declined by 16% from the peak (start of September 2020).
Wider benefits include the creation and agreement of new, region-wide governance structures for diagnostics, supported by pan-regional Clinical Reference Groups. Systems within London are also forming further networks with clinical leadership to further integrate across organisations.
Contact
Email: carole.finnigan@gov.scot