Inpatient census 2016: parts one and two
Results of the second Mental Health & Learning Disability Inpatient Bed Census and Out of Scotland NHS Placements Census, 2016.
2. Adult patients treated in NHS Scotland facilities (additional detail)

Specialty of Consultant
NHS Boards were asked to record the specialty of every Consultant who was responsible for overseeing the treatment of each patient in the Census:
Patients by consultant specialty, 2016 (Adults aged 18+)
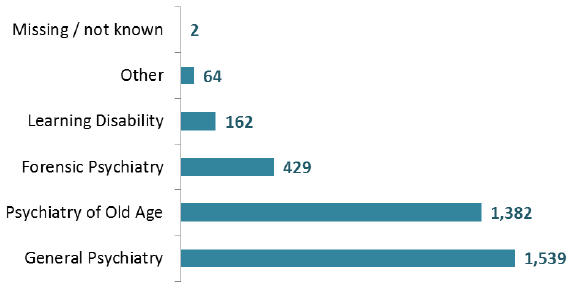
- 1,539 patients aged 18+ (43%) were seen by a consultant whose specialty was 'General Psychiatry'.
- 1,382 (39%) patients aged 18+ came under 'Psychiatry of Old Age'.
- 429 patients (12%) were seen by a consultant who specialised in Forensic Psychiatry.
Length of stay in hospital
There has been little change in the 'days since admission' between the 2014 census and the 2016 census. The average (median) number of days since admission for adults aged 18+ in March 2016 was 150 days, or around 5 months. In October 2014, the average time in hospital at the census date was 163 days.
The below chart shows the spread of patients by length-of-stay group. 478 adult patients (13%) were in hospital for 5 years or more at the census date, while 165 (5%) had been in for less than 72 hours.
Days since admission at census date, banded, 2016 (Adults aged 18+)
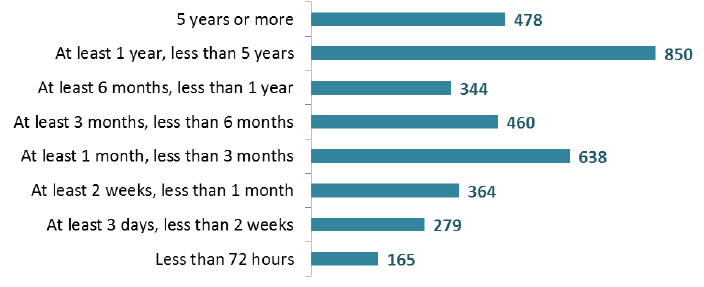
The average (median) number of days since admission for patients with a Learning Disability was 759 days (around 2 years and one month). The compares with 129 days (around 4 months) for non-Learning Disability patients.
Ethnicity
Of the 3,578 patients aged 18+ at the Census, White Scottish was the largest ethnic group. The full breakdown can be seen in the below table.
| Ethnicity | Adults aged 18+ (March 2016) |
|---|---|
| White Scottish | 2,777 |
| White Other British | 196 |
| White (unspecified)* | 108 |
| Other white ethnic group | 108 |
| Asian, Asian Scottish or Asian British | 43 |
| White Irish | 23 |
| African, African Scottish or African British | 17 |
| White Polish | 15 |
| Other/multiple ethnic groups | 22 |
| Not Known | 269 |
*May contain patients who fall under other White ethnic groups.
Living Circumstances
In 2016, NHS Boards were asked to record the 'Living Circumstances' from a range of
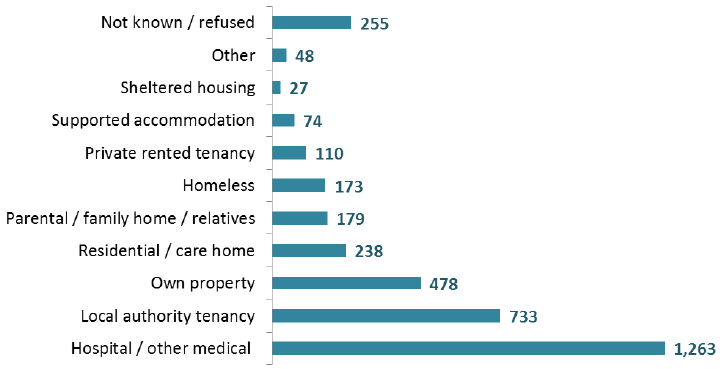
pre-defined options for each patient recorded in the census. 1,263 patients aged 18+ (35%) where in a Hospital or other medical establishment, while 733 (20%) where under Local Authority tenancy.
Patients by living arrangements, 2016 (Adults aged 18+)
Dependents
For the purposes of the Census, a 'Dependent' is defined as someone who relies on the patient in the census in their day to day life. For example a child, a partner with care needs of an elderly relative. 370 patients aged 18+ had a Dependent at the Census date. This is 11% of patents in the Census for whom this data is known (data was missing for 325 patients).
162 patients aged 18+ at the census had a dependent child aged 0-18, 5% of patients for whom this information is known. From Scotland's Census 2011, there were an estimated 2,100,000 people in Scotland with dependent children aged 0-18, around 50% of the adult population.
Status
Patient who have been detained under the provisions of the Mental Health (Care and Treatment) (Scotland) Act of 2003 are defined as having 'Formal' status. 'Informal' refers to voluntary Mental Health admissions.
At the March 2016 Census, 1,580 adult patients (44%) had 'Formal' status, while 1,998 (56%) had 'Informal' status.
Other Legislation
In 2016 NHS Boards were asked to record all the pieces of legislation for which patients were subject to at the Census date. 1,063 patients (32% of known cases) were subject to the Adults with incapacity (Scotland) Act. 865 patients (26%) were subject to the Mental Health Act (Compulsory Treatment Order). Data was missing for 258 patients.
Patients subject to legislation*, 2016 (Adults aged 18+)

*Patients can be subject to multiple pieces of legislation.
** MHA Mental Health Act. CPA Criminal Procedure Act.
Employment Status
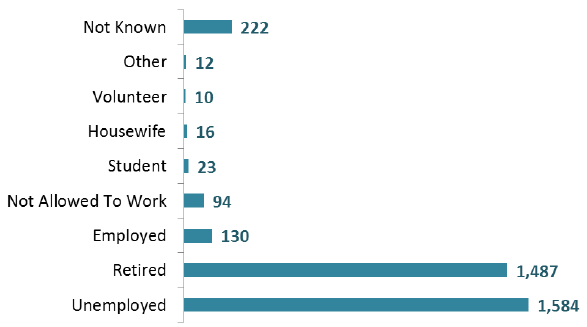
Of the patients aged 18+ for whom employment status was known at the March 2016 census, 1,584 (47%) were unemployed, 1,487 (44%) were retired and 130 (4%) were in employment.
Patients by employment status, 2016 (Adults aged 18+)
Health and Wellbeing
The following sections consider the mental and physical health of all patients aged 18+ at the Census. The 2016 Census additionally collected some information around lifestyle factors which can impact on a person's health and wellbeing.
Mental health morbidities
NHS Boards were asked to return diagnosis codes ( ICD10) for any mental health condition for which patients in the Census had a diagnosis. 2,784 patients aged 18+ (78%) had a diagnosis recorded for only one mental health condition, while 793 (22%) had a diagnosis for 2 or more conditions (see below chart).
Patients by number of mental health diagnoses* (Adults aged 18+)
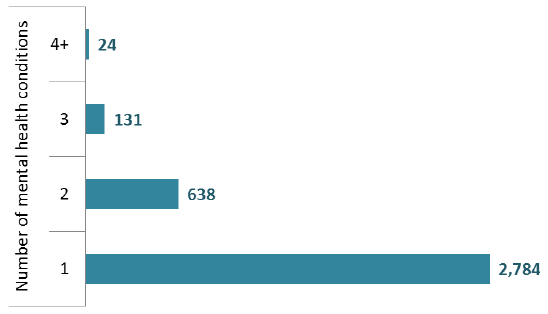
*based on recording of ICD10 codes.
*diagnosis data was not returned for one patient.
The following chart presents the most common diagnosed mental health morbidities, as at the census date for adults aged 18 or over in the March 2016 census. The two most common diagnoses are Schizophrenia (998 patients) and Dementia (995 patients), which each account for around 28% of all adult patients in the census. Note that a patient may have more than one diagnosis.
Most common diagnosed mental health morbidities, 2016 (Adults aged 18+)
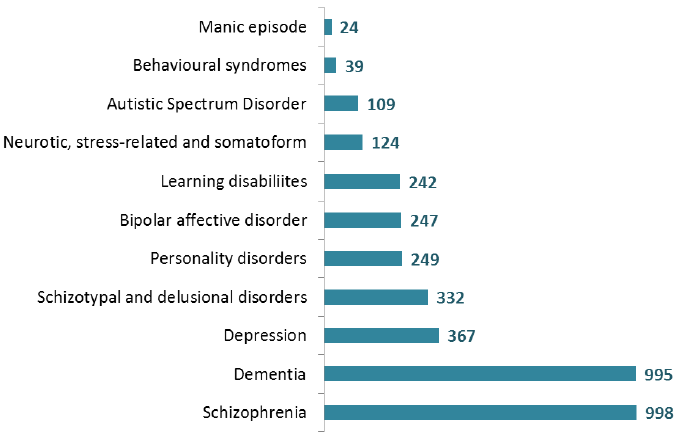
Note: All mental health diagnoses are based on ICD10 codes. Primary and secondary diagnoses included.
Note: Patients may have more than one diagnosis.
Learning Disabilities and Autism
Of the 3,578 patients aged 18+ at the Census, 291 patients (8%) had a diagnosis for either a Learning Disability or Autism. 242 patients had a diagnosis for a Learning Disability, 109 patients had a diagnosis for Autism (60 patients had a diagnosis for both).
Physical health co-morbidities
One of the key outcomes from the 2014 Census was the need to improve the recording of both mental health and physical health morbidities. Mental Health and Learning Disability services in NHS Boards are working towards routinely recording physical health conditions under the International Classification of Diseases. As an interim, the 2016 Census included a suite of Yes/No physical health questions. A small number of patients (less than 10) did not have physical diagnosis information recorded for certain conditions.
List of yes/no physical health morbidities questions in the census:
● Hypertension,
● Dyslipidaemia,
● Coronary heart Disease,
● Epilepsy,
● Chronic Kidney Disease,
● Thyroid Disease,
● Cancer,
● Alcohol Acquired Brain Injury,
● Diabetes,
● Chronic Obstructive Pulmonary Disease,
● Chronic Pain,
● Sensory Impairment,
● Liver Disease,
● Acquired Brain Injury,
● Stroke / Transient Ischaemic Attack,
● Parkinson
- 1,881 patients aged 18+ (53%) had at least one physical health co-morbidity based on the suite of Yes/No physical health questions as at the census.
Patients by number of physical health co-morbidities* (Adults aged 18+)
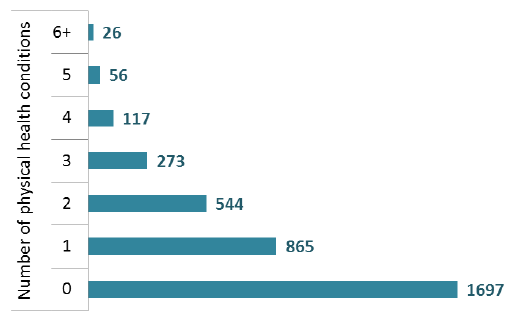
*Physical health co-morbidities are based on responses to a suite of Yes/No physical health questions in the census. Morbidities included: Hypertension, Diabetes, Dyslipidaemia, Chronic Obstructive Pulmonary Disease, Coronary heart Disease, Chronic Pain, Epilepsy, Sensory Impairment, Chronic Kidney Disease, Liver Disease, Thyroid Disease, Acquired Brain Injury, Cancer, Stroke / Transient Ischaemic Attack, Alcohol Acquired Brain Injury, Parkinson.
The following chart illustrates the prevalence of selected physical health morbidities for patients aged 18+ at the Census. Note that a patient can have more than one physical health morbidity.
Patients by most common physical health conditions (Adults aged 18+)
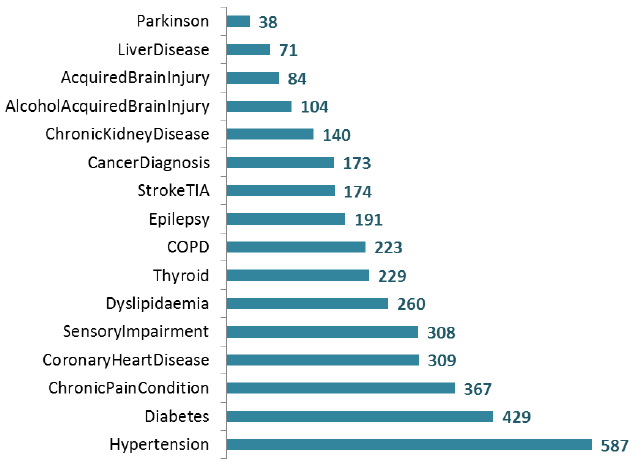
- 16% of all adult inpatients had Hypertension as at the census date. This was the most common physical health co morbidity from the suite of physical health conditions which were asked specifically about in the census.
- Diabetes was the next most prevalent physical health co-morbidities (12% of all adult patients).
Lifestyle factors
BMI (Body Mass Index)
- The following chart shows the BMI (Body Mass Index) distribution for adult patients. Note the chart excludes 163 patients where height and weight information was not provided in order to calculate BMI scores, as well as a small number of patients in Eating Disorder wards.
Patients by BMI Index (Adults aged 18+)
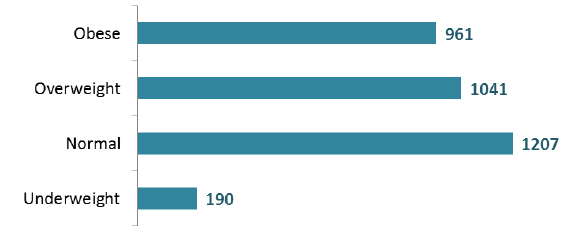
- 2002 adult patients (59%) for whom BMI was known were either Overweight or Obese at the March 2016 census date (excluding Eating Disorder wards).
- Around a third of adult patients (1207, 36%) had a Normal BMI score as at the census (excluding Eating Disorder wards).
Smoking, alcohol and drug misuse
The 2016 census included a number of questions around alcohol and other substance misuse. It is known that not all patients with alcohol dependence or substance abuse will have a formal ( ICD10) diagnosis. This section contains analysis of patients with alcohol dependence and / or substance misuse based on responses for a combination of questions (see Section 6 for further detail).
- Around one third of adult patients (1,248, 35%) smoked tobacco in the 12 weeks prior to the census date.
- 688 patients aged 18 and over (19%) had a dependence on alcohol / harmfully used alcohol. Of these, 193 (28%) had an alcohol-related diagnosis based on ICD10 codes.
- 616 patients aged 18 and over (17%) had abused substances (excluding alcohol). Of these, 193 (31%) had a diagnosis of drug misuse based on ICD10 codes.
Smoking, drugs and alcohol (Adults aged 18+)
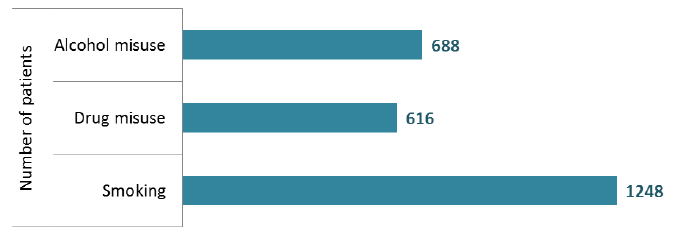
Substances used prior to admission
In the March 2016 Census, NHS Boards were asked to record the substances which patients used prior to admission.
For those patients who did have a record of substance abuse (excluding alcohol) in the four weeks prior to admission (522 known patients), Cannabis was the most prevalent with 289 patients (55%) recorded as having used it.
Substances used in four weeks prior to admission* (Adults aged 18+)
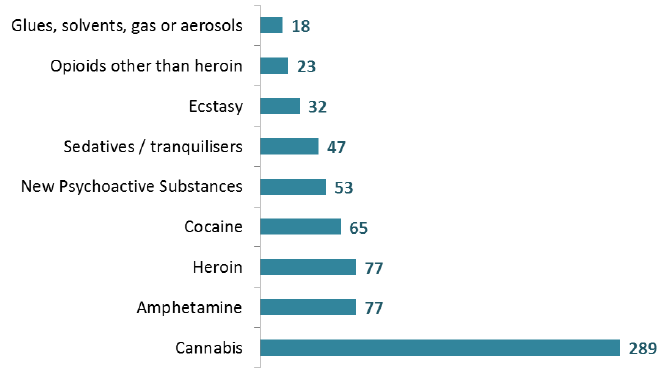
*Patients can be in more than one category.
*Excludes other substances which were recorded for small numbers of patients.
Of the patients with a record of substance abuse (excluding alcohol) in the four weeks prior to admission,
291 patients used only one substance, while 152 used two or more (see below table). Detailed information on substances used was not returned for 72 patients.
| Number of substances used per patient in 4 weeks prior to admission | 2016 |
|---|---|
| One | 291 |
| Two | 79 |
| Three | 41 |
| Four | 19 |
| Five or more | 13 |
| Not known | 72 |
Of the patients with recorded substance abuse in 4 weeks prior to admission, 294 used smoke or nasal as the main route of substance abuse, 204 oral and 46 injecting (patients can use more than one route).
Substances used during stay
NHS Boards were also asked whether patients had used non-prescribed drugs during their stay in hospital / care home. 145 adult patients used non-prescribed drugs during their stay, 6% of patients for whom this information was known (information was not returned for 239 patients). Patients in Continuing Care and Dementia Care wards are excluded.
For those patients who used non-prescribed drugs during their stay, Cannabis was again the most prevalent with 93 patients using it (64%), while 26 patients (18%) used New Psychoactive Substances ( NPS) during their stay.
Substances used during stay* (Adults aged 18+)
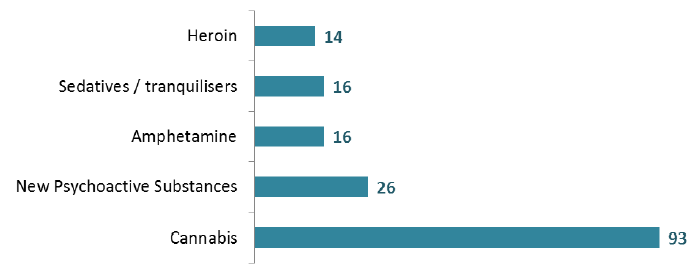
*Patients can be in more than one category.
*Excludes other substances which were recorded for small numbers of patients.
*Excludes Continuing Care and Dementia Care ward types.
Of the 145 patients who used non-prescribed drugs during their stay. 27 patients used two or more substances prior to admission (see below table).
| Number of substances used per patient during stay | 2016 |
|---|---|
| One | 118 |
| Two or more | 27 |
Of the patients with recorded substance abuse during their stay in hospital / care home, 82 used smoke or nasal as the main route of substance abuse while 75 patients used oral route. A small number (less than 10) used injecting (patients can use more than one route).
Self harm
This information was provided for 3,334 out of 3,578 patients.
- 445 adult patients self harmed in the week prior to admission to hospital. This is 13% of patients where this information was known.
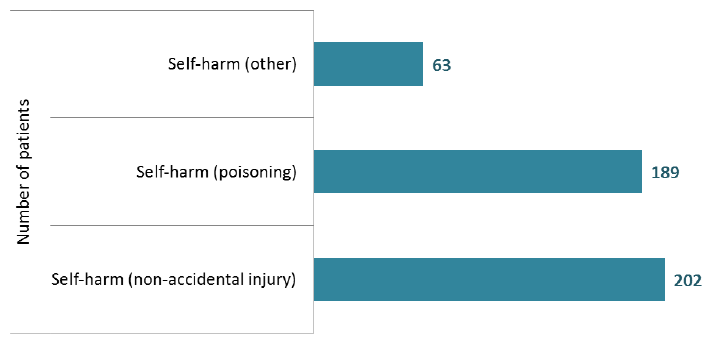
- 202 patients self harmed by non accidental injury (45% of all self-harm).
Note that patients can be in multiple categories in the following chart.
Self harm (Adults aged 18+)
Suicidal ideation
This information was provided for 3,290 out of 3,578 patients.
- 412 adult patients expressed suicidal ideation on admission to hospital. This is 13% of those for which information was known.
Contact
Email: Steven Gillespie, swstat@gov.scot