Heart Disease Improvement Plan
The Heart Disease Improvement Plan sets out the priorities and actions to deliver improved prevention, treatment and care for all people in Scotland affected by heart disease.
3. Priorities
30. The Heart Disease Quality Improvement Plan 2014 identifies six priority areas for improvement linked by an overarching aim and underpinned by two common themes that are fundamental to success. Together, these contribute towards the prevention, detection, treatment and after care of heart disease and patients with heart disease. These priorities are summarised in Figure 1.
31. The Plan mainly focuses on those actions to be taken forward directly by local MCNs. However, there are also several significant national initiatives and programmes which require on-going support, energy and engagement of the heart disease community. Four of these national issues are highlighted below.
Congenital Heart Disease Services
Congenital heart anomalies remain the most common birth abnormality with an estimated incidence of approximately 1 in 145 live births. The range and complexity of cardiac problems are enormous. Fortunately, advances in paediatric cardiac surgery and catheter intervention has increased expected survival to greater than 80%, with the result that there is a new and growing group of adults living with congenital heart disease in addition to the paediatric population. Estimates in 2010 suggested there were more than 15,600 adults in Scotland living with congenital heart disease; in fact recent ISD data suggests that this figure may be an underestimate of the true disease burden with over 20,000 first admissions with congenital heart disease at all ages recorded between the years 1986 and 2009.
The Scottish Congenital Cardiac Network was nationally designated as a National Managed Clinical Network under the aegis of National Services Division (NSD) from April 2013. This Network was established to promote the improvement of services for children and adults with congenital heart disease; co-ordinate pan-Scotland planning with NHS Boards, Regional Planning Groups, clinicians and patient representatives; and support the continued provision of safe and sustainable paediatric and adult congenital cardiac services across Scotland. The Network works closely with the Paediatric Cardiac Service (which is due to move from Yorkhill to the new South Glasgow Hospitals Campus in summer 2015) and the Scottish Adult Congenital Cardiac Service (the specialist tertiary service based at the Golden Jubilee).
For the majority of adult congenital cardiac patients, emergency treatment of acute cardiac and non-cardiac illness and obstetric care will take place in their local hospital. The challenge is to ensure local services and people with congenital cardiac conditions are able to access high-quality specialist congenital cardiac care when needed, but have effective shared care arrangements for the treatment and management of non-complex conditions. The aim therefore is a networked approach which facilitates local flexibility and the delivery of safe care close to the patient's home.
Out of Hospital Cardiac Arrest (OHCA)
Surviving an out of hospital cardiac arrest depends on a series of events occurring seamlessly - the 'chain of survival'. This includes prompt recognition of the cardiac arrest and calling for help; early, effective cardiopulmonary resuscitation (CPR), early defibrillation to restart the heart; rapid access to advanced resuscitation skills (e.g. cooling therapy) for those requiring further resuscitation and the best possible post resuscitation care in hospital to allow the heart and brain to recover from the damage.
By building on current best practice - such as the joint project between the Scottish Ambulance Service and the Resuscitation Research Group to increase survivability rates for out of hospital cardiac arrests in Edinburgh; and the work of the British Heart Foundation, Chest Heart & Stroke Scotland and other third sector organisations, particularly in relation to cardiopulmonary resuscitation (CPR) - there is a real opportunity to improve Scotland's approach to out of hospital cardiac arrest. The Scottish Government is currently considering how best to take forward this goal.
Familial Arrhythmia Network of Scotland (FANS)
Familial arrhythmias are inherited conditions which cause instability of the heart's rhythm. These conditions can show themselves as life threatening heart rhythm disturbances, the medical term for which is 'arrhythmia'. People with these conditions usually have no symptoms until they are young adults. The first symptom of the condition may be sudden death from a life-threatening arrhythmia, an event called Sudden Arrhythmic Death Syndrome (SADS). During life, these conditions can be difficult to diagnose as they do not cause any obvious structural changes to the heart. It is important for a diagnosis to be made quickly so that family members can be screened for the condition. There are effective therapies available that can prevent SADS and allow affected individuals to lead a normal life.
The Familial Arrhythmia Network of Scotland (FANS) is a Scotland-wide managed clinical network set up to improve the diagnosis and care for individuals and their families affected by familial arrhythmia. The Network was officially launched in February 2010.
The proper care of arrhythmias requires the involvement of many healthcare care professionals including cardiologists, geneticists, counsellors, GPs, specialist nurses, paediatricians and pathologists. FANS was formed to bring together the expertise of this wide range of clinicians from all over the country, to work together with patient representatives to streamline standards of care in Scotland, ensuring best clinical practice is achieved for all familial arrhythmia patients and their families. The Network aims to improve services offered to those affected, allowing them to access appropriate treatments in a timely manner.
Transcatheter Aortic Valve Implantation (TAVI)
Aortic stenosis affects around 3% of the population aged over 75. The most effective treatment is to replace the valve through open heart surgery. Approximately 900 such operations are preformed every year. Since 2012 people too ill to undergo open heart surgery, have been able to have a specialist operation at the Royal Infirmary of Edinburgh. Transcatheter aortic valve implantation (TAVI) is a relatively new non-invasive treatment for aortic stenosis If a person is either too unwell for open heart surgery, or their heart and vessels are not suitable for aortic valve replacement, TAVI can be offered as an alternative treatment option. The procedure is less invasive, as a replacement valve is passed through a hole in the groin and advanced up to the ascending aorta of the patient. Between October 2012 and January 2014, 75 patients were treated by the Edinburgh team.
Figure 1 Heart Disease in Scotland: Priorities for Improvement
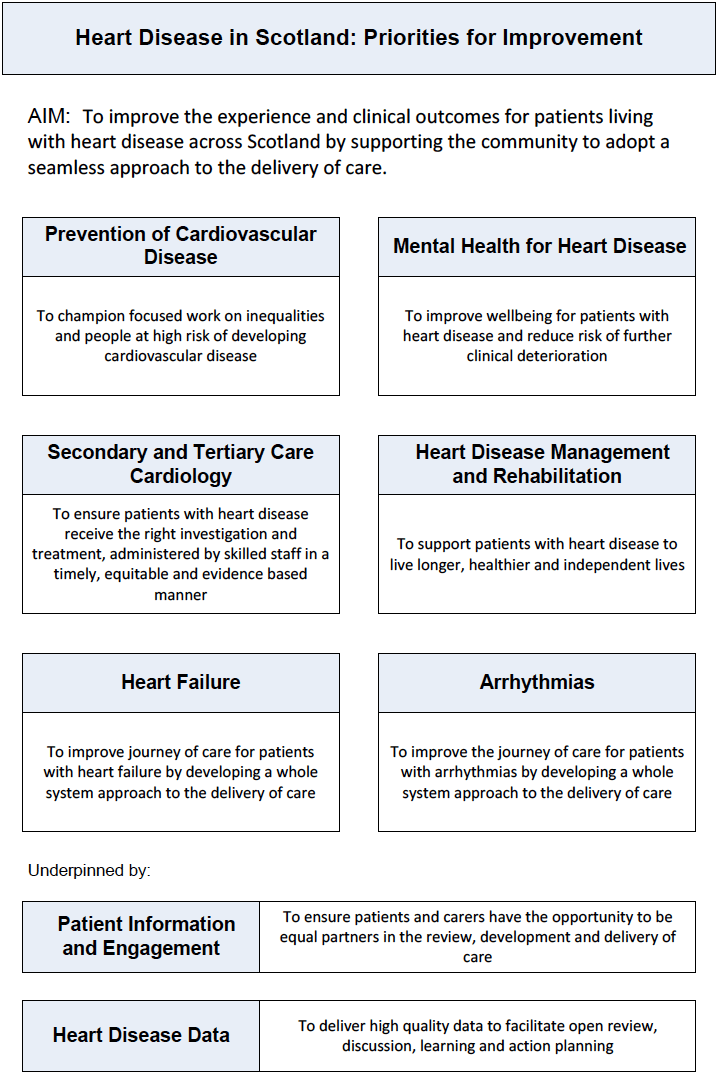
Priority 1: Prevention of Cardiovascular Disease
| Aim: | To champion focused work on inequalities and people at high risk of developing cardiovascular disease. |
|---|---|
| Background: | Primary prevention of cardiovascular disease is now widely established and mainstreamed within the work programmes of NHS Boards Health Promotion and Improvement Departments. NHS Boards are developing health promotion programmes that are sensitive to inequalities based on social deprivation. The Health Promoting Health Service (HPHS) is one such example. Prevention lies at the heart of HPHS policy as it is about promoting healthier behaviours and discouraging detrimental ones, by ensuring that healthier choices are the easier ones and that appropriate support systems are in place to encourage and re-enforce these choices. HPHS is transformative in its mission to bring preventative action to the fore and actively change the culture of the hospitals to help support this. A Ministerial and non-executive director champion groups have been established to help take forward the actions as described in the HPHS 01(2012) letter to NHS Boards Chief executives. HPHS in collaboration with MCNs can integrate preventative action within the scope of secondary care, ensuring pathways for health improvement are built into clinical care to encourage and support positive behaviours and increase access to support and health improvement services. Consideration is being given to socially deprived populations not accessing treatment with programmes targeting communities to encourage families to be 'healthy together' i.e. physical activity/diet/smoking/alcohol. However, there remain issues in relation to very specific groups at high risk of developing cardiovascular disease and it is, therefore, considered appropriate for Heart Disease Networks to provide a more focused approach within this area. |
| Actions: | 1. HD MCNs should champion health improvement work, with a focus on inequalities, specifically targeting case finding strategies for people at high risk of developing cardiovascular disease. 2. The HPHS 01 (2012) explicitly states the crucial role of MCNs in championing preventative action and engaging the workforce to deliver on this with a focus on inequalities. Access and use of health services is socially patterned with people living in socio-economic deprived circumstances and at risk of poor health, are more likely to use services than those living in affluent areas. Competing priorities and a focus on clinical aspects has meant that there has been limited engagement with MCNs on this agenda but serious action now needs to be taken to integrate anticipatory care into routine practice. |
Priority 2: Mental Health for Heart Disease
| Aim: | To improve wellbeing for patients with heart disease and reduce risk of further clinical deterioration. |
|---|---|
| Background: | Although there has been significant progress over the past few years in relation to identification and intervention for people with established CHD affected by anxiety and depression, services are still patchy across Scotland with some areas struggling to access services for patients within reasonable timescales. There is also a general lack of awareness and understanding of the impact mental health has on both the individual with heart disease and the healthcare system. However, evidence to support this approach has increased in recent years, identifying that prevalence of mental health within this patient group is becoming significant with associated impact on patient morbidity and mortality leading to increased usage of the healthcare system. It is also highly relevant to note that mental health is now acknowledged as an independent risk factor for cardiovascular disease. In addition, it has been identified that having a diagnosis of heart disease make the individual more at risk of experiencing mental health problems which in turn increases the risk of further cardiac events. |
| Actions: | 1. Develop a mental health pathway for patients with heart disease. 2. Deliver level 1 and 2 psychological support training to generic and specialist staff respectively. |
Priority 3: Secondary and Tertiary Care Cardiology
| Aim: | To ensure patients with heart disease (including congenital heart disease) receive the right investigation and treatment, administered by skilled staff in a timely, equitable and evidence based manner. |
|---|---|
| Background: | Significant progress has been made by NHS Boards, Regional Planning Groups and Scottish Ambulance Service over the past 12 years in relation to immediate treatment and intervention for patients with ST Elevated myocardial infarction. As such, it is considered time to expand the parameters of the priority to encompass wider aspects of the management of all patients with heart disease, whether this is congenital or acquired, within the hospitals in-patient and out-patient setting. The new actions outlined below provide continuity by ensuring ongoing quality improvement in relation to management of acute coronary syndromes but also expands into other areas of acute cardiac care and the ongoing monitoring and management of life-long conditions, whilst moving focus towards continuity across regions. |
| Actions: | 1. Improved patient-centred flow into, through, between and out of hospital for patients with chest pain. 2. Develop local and regional pathways including strategy for cardiac investigation and intervention. 3. Develop clear diagnostic and treatment pathways for patients with valvular heart disease. |
Priority 4: Heart Disease Management and Rehabilitation
| Aim: | To support patients with heart disease to live longer, healthier and independent lives. |
|---|---|
| Background: | Cardiac Rehabilitation services are very well established across Scotland with all areas providing full menu based programme incorporating educational sessions to meet the individual needs of patients. However, several NHS Board areas are experiencing capacity issues due to finite resources. In many areas this has led to limited capacity to accommodate the needs of patients with congenital disease and acquired heart failure, angina and ICDs. Consequently, it is considered time that CR services were modernised around the patient with the aims of the priority expanded to include long-term management of patients via anticipatory care planning and good self management strategies. |
| Actions: | 1. Modernise cardiac rehabilitation services. 2. Develop anticipatory care programmes for patients with heart disease. 3. Develop condition and wellbeing self-management programmes for patients with heart disease. |
Priority 5: Heart Failure
| Aim: | To improve the journey of care for patients with heart failure by developing a whole system approach to the delivery of care. |
|---|---|
| Background: | Heart Failure services are generally progressing well across Scotland despite some residual difficulties in relation to resources. However, as the incidence of heart failure rises in line with the aging population the impact on individuals and the healthcare system is becoming increasingly problematic. Improvement in the quality of care and implementation of readily accessible treatment throughout the patient journey would greatly increase patients' quality of life with associated efficiencies for healthcare system. In addition, there is an increasing body of evidence that patients with heart failure have similar or worse symptoms burden, morbidity and mortality compared to patients with cancer. Patients with cancer have well developed, formalised palliative care services provided by appropriately trained staff to address their needs. Despite the obvious equivalent need, patients with heart failure do not. There is clear national and international policy and guidelines all stating that palliative care should be provided for patients with advanced disease including heart failure. Although many areas around Scotland are now making significant progress in relation to developing palliative care and anticipatory care planning for patients with heart failure, we still have a long way to go. |
| Actions: | 1. Improve identification, diagnosis and long-term management of patients with heart failure. 2. Improve patient centred flow into, through, between and out of hospital. 3. Develop palliative care pathway for patients with heart failure. |
Priority 6: Arrhythmias
| Aim: | To improve the journey of care for patients with arrhythmias by developing a whole system approach to the delivery of care. |
|---|---|
| Background: | Heart Disease Networks are making progress in relation to improving management of patients with arrhythmias but in many areas this work remains at the early stages of development. Consequently, future actions seek to provide a continued focus on improving the management of atrial fibrillation as a long term condition, again, underlining the importance of developing seamless whole system services. In addition, the priority has been expanded to take cognisance of other arrhythmia conditions and the more advanced therapies including implantable devices. |
| Actions: | 1. Improve identification, diagnosis and long-term management of patients with atrial fibrillation. 2. Improve patient centred flow into, through, between and out of hospital for patients with arrhythmias. 3. Develop pathways for the identification and treatment of patients at risk of familial arrhythmia conditions. |
Underpinning Themes
In addition to the six priorities, NHS Board HD Networks should continue to address the core principles of MCNs. In particular, the following areas should underpin the Heart Disease Improvement Framework and the work on each individual priority:
Patient Information and Engagement
| Aim: | To ensure patients and carers have the opportunity to be equal partners in the review, development and delivery of care. |
|---|---|
| Actions: | NHS Boards HD MCNs should have a: 1. Patient information strategy 2. Patient and carer engagement strategy 3. Annual programme to capture patient feedback in relation to satisfaction and experience |
Heart Disease Data
| Aim: | To deliver high quality data to facilitate open review, discussion, learning and action planning. |
|---|---|
| Actions: | NHS Board HD MCNs should have: 1. A process to review HIS HD Indicators 1-3, (mortality for myocardial infraction and congestive cardiac failure, length of stay and readmission to hospital). 2. A process to collate and review local data in relation to HIS Indicator 4 which is the indictor for quality improvement. |
Contact
Email: Cheryl McNulty