Heart disease: action plan
The heart disease action plan (2021) sets out our priorities and the actions we will take to minimise preventable heart disease and ensure equitable and timely access to diagnosis, treatment and care for people with suspected heart disease in Scotland.
3. Background and context
The Heart Disease Improvement Plan (2014) affirmed heart disease and stroke as a continued clinical priority for Scottish Government. The 2014 Plan set out a number of priorities and actions to deliver improved prevention, treatment and care for all people in Scotland affected by heart disease. An outline of progress achieved by that plan is included in Appendix A.
Whilst excellent progress has been made we will always strive to do more to deliver the best possible health and social care and to ensure that we continue to address the current needs of people living with heart disease in Scotland.
Heart disease continues to have a significant impact on people in Scotland. In addition, the Covid-19 pandemic has highlighted challenges and changed models of care across the entire health care system and this is an appropriate point to take stock and refresh our actions in this area.
We have received feedback on this plan from the National Advisory Committee for Heart Disease (NACHD), members of the wider cardiac community, people with lived experience of heart disease and policy colleagues across Scottish Government. This has been vital to our ability to produce this refreshed Heart Disease Improvement Plan, which is now retitled: Heart Disease Action Plan.
The vision and priorities of this plan are closely aligned with the vision and principles of the National Clinical Strategy for Scotland, which are; a focus on quality, change guided by evidence, allowing people and communities to manage their own health, new models of community-based provision, equitable access, encouraging collaboration and the implementation of Realistic Medicine.
This plan sets out a whole system approach, which encompasses primary, secondary and specialist care, community care and third sector services. Through the implementation of this plan, we endeavour to encourage collaboration and integration, where it will be of benefit to people with heart disease.
3.1 Scope of this plan
This plan addresses the needs of people with, and those at risk of developing, heart disease. It does not directly address diabetes or other cardiovascular conditions such as stroke. These are addressed separately in The Diabetes Improvement PlanandThe Stroke Improvement Plan, overseen by the National Diabetes Group, and the National Advisory Committee on Stroke, correspondingly.
Similarly, specific actions to address Out of Hospital Cardiac Arrest is covered by the Out of Hospital Cardiac Arrest strategy, delivered through Safe a Life for Scotland.
Despite this, there are many common themes in providing timely and equitable care for people with all cardiovascular conditions and many people live with more than one condition so many actions detailed in this plan may be applicable across boundaries. We will therefore work closely to align the implementation of relevant actions across condition specific plans.
Similarly, this plan focuses on the provision of diagnosis, treatment and care for people with heart disease and does not specifically address wider societal public health measures. Several policy commitments exist in Scotland in relation to this, including Raising Scotland's Tobacco-Free Generation: Tobacco Control Action Plan 2018; A Healthier Future: Scotland's Diet & Healthy Weight Delivery Plan 2018; A More Active Scotland: Scotland's Physical Activity Delivery Plan 2018; Alcohol Framework 2018: Preventing Harm and Cleaner Air for Scotland: The Road to a Healthier Future. The commitments set out in these plans in will have an important impact on heart disease in Scotland and should be seen as complementary to this action plan.
We seek coherence across a range of other policy areas and will continue to work collaboratively across the Scottish Government to ensure that appropriate links are made and maintained.
3.2 Scale of heart disease in Scotland
Heart disease remains a major cause of death and disability in Scotland, accounting for over 9,000 deaths each year[1]. There has been a steady rise in life expectancy over decades, but this has recently stalled, partly due to a slowdown in the progress in reducing mortality from heart disease, especially in people between the ages of 55 and 74[2].
Ischaemic heart disease, which can lead to a heart attack, is still Scotland's single biggest killer, responsible for 11.2% of all deaths in 2019[3]. It accounts for 25,000 hospital admissions each year[4].
Other forms of heart disease also have a significant and growing impact on people in Scotland. The incidence of conditions like heart failure[5], heart valve disease[6] and atrial fibrillation[7] have been increasing, partly as a result of an ageing population, improved detection and increased survival from acute coronary events. Many people are living longer with heart disease and may require lifelong care and support.
- More than 47,000 people have been diagnosed with heart failure in primary care[8]. This is likely to be an underestimation of the number of people living with heart failure in Scotland. In the past ten years, the incidence (new diagnosed cases) of heart failure has increased year on year in Scotland. In 2018/19 there were over 5200 incident cases of heart failure[9]. This increasing trend is projected to continue as the population ages.
- Based on global burden of disease estimates, more than 73,000 people in Scotland have heart valve disease[10].
- More than 106,000 people have been diagnosed with atrial fibrillation[11].
- Around 28,000[12] people in Scotland have an inherited heart condition, the most common of which is hypertrophic cardiomyopathy.
- Congenital heart disease is one of the most common birth defects in Scotland, affecting around one in every 150 births. Improved survival rates mean that a growing number of people are living into adulthood with congenital heart disease[13].
3.3 The impact of the Covid-19 Pandemic
The Covid-19 pandemic has brought the need for action to address heart disease in Scotland into even sharper focus, having had a significant impact on people with heart disease and on the services that support them.
During the first lockdown period of the pandemic, overall attendance at Accident and Emergency decreased[14] and this period coincided with a 30% decrease in emergency cardiology admissions in Scotland[15]. There was also a deferral and reduction of other services, including diagnostics, access to specialist support in the community and cardiac rehabilitation. There are concerns that all of this will have implications for mortality and morbidity for people with heart disease and result in an increase in the number of people who require continued support from the health system for many years to come.
Health inequalities, already significant in Scotland, have increased during the pandemic as Covid-19 has had a disproportionate impact on people living in areas of socioeconomic deprivation[16], and people of South Asian ethnicity appear to have been at proportionally greater risk[17].
Addressing inequality will be monitored and considered carefully throughout the implementation of this plan. That means listening to a wide range of voices in our efforts to create pathways and reshape models of care, embedding the actions on cardiac disease identified within the Women's Health Plan within the implementation of actions identified by this plan, and ensuring that we are appropriately measuring and acting upon inequalities within the data and improvement work outlined in Priority 4.
Despite the challenges, the pandemic has also provided opportunities for us to think about how we deliver health care services. Healthcare and support services have had to be creative, resilient and innovative about how they can provide the right support to patients. The use of technology and care closer to home has been vital to maintaining care throughout the crisis and has important lessons for delivering person-centred care in the future.
3.4 Vision and Priority Areas
Vision: We want to minimise preventable heart disease and ensure that everyone with suspected heart disease in Scotland has timely and equitable access to diagnosis, treatment and care that supports them in living well with their condition.
Priority 1: Prevention - tackling risk factors: We will minimise preventable heart disease by improving the detection, diagnosis and management of risk factor conditions.
Priority 2: Timely and equitable access to diagnosis, treatment and care: We will ensure that everyone with suspected heart disease in Scotland has equitable access to timely and evidence-based diagnosis, treatment and care.
Priority 3: Workforce We willensure appropriate staff resource and training to deliver timely and equitable services across Scotland for people with heart disease.
Priority 4: Effective use of data: We will ensure that high-quality, standardised data is available and used effectively to support clinical decision-making, understand patient outcomes and enable better service-planning, so that people experience better quality of care, and improved outcomes.
3.5 Governance
The implementation of this plan will be overseen by the National Heart Disease Task Force (previously known as the National Advisory Committee on Heart Disease), supported by the Scottish Government Clinical Priorities team.
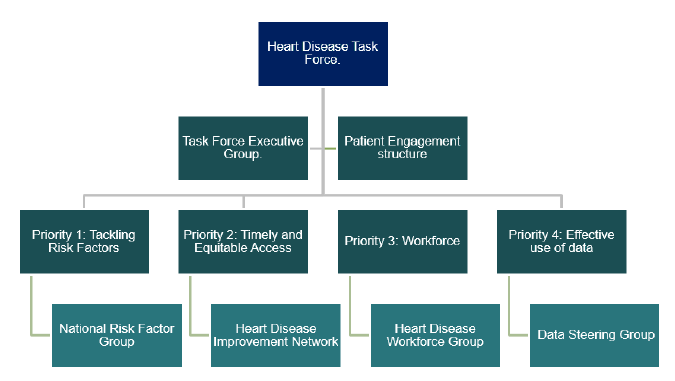
The ethos of Realistic Medicine is that the person receiving care should be at the centre of decision making through meaningful conversations around what matters most to people, with a shared understanding of what healthcare might realistically contribute to this. It is therefore vitally important that we place people with lived experience of heart disease at the very centre of implementing this plan. This will be supported by a robust lived experience structure which will feed directly into the Task Force.
There is often under-representation of women, people from black and minority ethnic backgrounds, people with disabilities, people who are LGBTI, and those living in areas of socio-economic deprivation in forums where engagement takes place. If we are to seriously address health inequalities and move towards the provision of equitable care then we must understand a wide range of lived experience. To do this we must make a strong and consistent effort to seek and amplify the voices of those typically underrepresented in decision making processes. In particular, our Equality and Impact Assessment for this plan has identified the need for us to make a concerted effort to amplify the voices of people from areas of deprivation (including a focus on people who experience homelessness), people from the gypsy traveler community, women, people with learning disabilities and older people.
Furthermore, groups of people who may be impacted by heart disease but are typically overlooked when it comes to engagement and addressing inequalities are people who are LGBTI and younger people. We will make a consistent effort to include their voices within the implementation of our lived experience structure.
A Task Force Executive Group will advance actions in between meetings and ensure continuous progress. This group will consist of, at least:
- Task Force Chair (CMO Advisor)
- Task Force Deputy Chair
- Heart Disease Improvement Network Lead
- Risk Factor Planning Group Lead.
- Heart Disease Workforce group Lead.
- Heart Disease Policy Lead (Scottish Government).
- Public Health Scotland (Audit lead)
- Patient Engagement Lead.
Each group identified in the infographic above will produce an annual implementation plan based on the strategic aims and actions outlined in this plan. The Task Force will agree these plans and oversee progress against them.
An annual report on progress towards the strategic priorities identified in this plan will be published, enabling continuous review of progress.
Contact
Email: Clinical_Priorities@gov.scot