Health and Social Care: Winter in Scotland in 2014/15
This report provides an overview of Health and Social Care winter pressures and performance over the 2014/15 winter period.
Summary
1. In winter 2014/15, the NHS in Scotland increased capacity and carried out more activity. There were increased and prolonged pressures from influenza and respiratory illness. Pressures from delayed discharge continued to increase through to the end of 2014 and eased in to 2015. These pressures will have contributed to the reduced key whole-system 4 hour A&E waiting times performance in December, January and February. Scotland saw significant A&E waiting times performance improvements in the spring and summer months. Integrating health and social care and the £100m being invested to improve delayed discharge are priorities for the Scottish Government. The Scottish Government has also developed a fresh approach to improving unscheduled care across Scotland - in winter and all year round - which is based on six essential actions. This focus on integration, improving delayed discharge and the unscheduled care six essential actions, underpin the planning guidance for winter 2015/16 - with an additional focus on planning for the additional pressures and business continuity challenges that are faced in winter.
Purpose
2. The Scottish Government aims to create the conditions which support NHS Scotland to improve resilience by building capability to absorb, respond and recover from disruptive challenges. Winter disruptions can include increased demand and activity due to seasonal flu, respiratory and circulatory illness; increased numbers of falls and trips; and wards closed to admission due to higher levels of norovirus. There are also business continuity challenges associated with managing workforce rotas during the festive period, to ensure that patients continue to be safely and effectively admitted, diagnosed, treated and discharged.
3. This report draws together the key official statistics on system capacity, activity, pressures and performance. Unless otherwise stated, within the charts and tables, winter is defined as the two quarters ending December and March. This report should be considered alongside the preparing for winter guidance for 2015/16. The planning guidance for winter 2015/16 has been developed for NHS Boards and their partners. The guidance has been issued at the same time as this report on last winter. The guidance is based on integration, improving delayed discharge and the new unscheduled care six essentials with additional focus on planning for the additional pressures and business continuity challenges that are faced in winter.
Planning for Winter 2014/15
4. As in previous winters the Scottish Government and NHS Boards reviewed the 2013/14 winter as part of the planning for 2014/15. Winter 2013/14 saw increased pressures on the system due to delayed discharge of patients.
5. The Scottish Government developed winter guidance with NHS Boards and their partners over the summer of 2014. A National Unscheduled Care planning event was held on 11 September and winter guidance issued on 23 September 2014.
6. NHS Boards were required to formally sign-off their winter plans at their boards by the end of November at the latest.
7. In 2014/15, £10 million was allocated to health boards for winter resilience. This is in addition to £10 million made available for delayed discharge and £9.4 million for local unscheduled care plans to support NHS Boards over winter.
The NHS in Scotland strengthened capacity in Winter 2014/15
8. Between December 2013 and December 2014, the NHS Scotland workforce increased by 2,495.6 whole time equivalent (wte) or 1.8 per cent. This included an additional 298.9 wte Medical and Dental consultants and 1,126.1 wte nursing and midwifery staff (inc Interns). Over recent years there has been significant developments in the nursing and midwifery workload and workforce planning tools available to NHS Boards in Scotland. These evidence based tools provide information on the nursing and midwifery whole time equivalent requirement based on the measurement of workload generated by individual patients.
9. NHS Boards plan and manage the number of acute medial beds required throughout the year to take account of seasonal pressures. The number of acute medical beds increased throughout this winter. For quarter ending March 2015 they increased by almost 300 (excluding Highland for whom data is not available); from 10,899 in quarter ending December 2014 to 11,196 in quarter ending March 2015. This was on top of an increase of 147 between quarter ending September 2014 and December 2014.
10. There was also additional capacity in the community with health boards and local authorities creating a further 200 intermediate care beds by the end of March 2015 - an increase of over 40 per cent.
The NHS in Scotland delivered increased levels of activity in Winter 2014/15
11. Calls to NHS 24 core services increased by 115,574 or 17 per cent compared to last winter - the increase in calls was generally uniform over the whole winter. The increase to winter 2010/11 was around 8 per cent. This year's increase may be partly attributable to the introduction of the free to call 111 numbers.
12. Overall Scottish Ambulance Service emergency demand (Cat A, Cat B, Cat C) increased by 17,499 or 3.8 per cent compared to last winter. The Scottish Ambulance Service utilised its Resource Escalation Activation Plan (REAP) to ensure that the highest acuity patients are prioritised and the safety of patients was maintained. A large proportion of the demand increase in January and February 2015 came from 999 calls, GPs, community alarm services and nursing homes, with continued demand for patient discharges.
13. Hospital activity was also at an increased level. The numbers of A&E attendances, emergency inpatients, and elective inpatients and day cases all increased this winter. A&E attendances were up 3,924 or 0.5 per cent; provisional emergency and transfer inpatient discharges up over 11,000 or 2.4 per cent this winter; and provisional elective inpatient and day case discharges up almost 3,900 or 1.2 per cent.
The NHS in Scotland faced significant respiratory and influenza pressures in Winter 2014/15
14. The pressures from respiratory illness were the highest seen in the last ten years. Hospital admissions can have a primary diagnosis and provisional data for the weeks in December 2014 and January 2015 is available on respiratory admissions where a respiratory illness was recorded as the primary diagnosis. Compared to the same period last year, there was a 22.5 per cent significant increase, with this year seeing high levels sustained for many weeks.
Chart 1: Weekly emergency inpatient admissions with respiratory illness as a primary diagnosis, by week 2004/05 to 2014/15
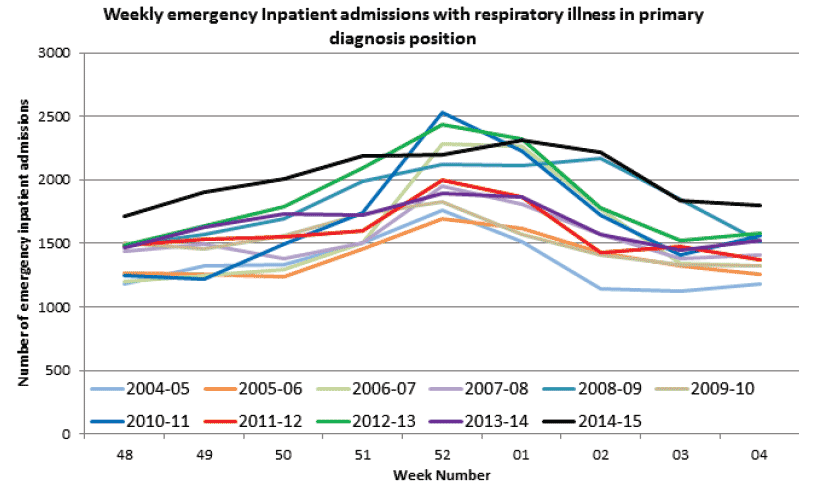
Source: ISD Scotland, provisional SMR01 data
15. Furthermore, it is clear that the provisional data for 2014/15 show an increase, compared with previous seasons, in number of hospital admissions with any diagnosis of influenza. The levels were at a sustained level over many weeks in the January and February of the 2014/15 season and this is in contrast to the more pronounced peak, but less sustained activity, seen in 2010/11. The number of hospital admissions with any diagnosis of influenza in 2014/15 are higher than the previous three years combined.
Table 1: Number of hospital stays with any diagnosis of influenza (regardless of specialty of admission) for weeks 40 to week 20 in seasons 2010/11 to 2014/15*
| Flu season | 2010/11 | 2011/12 | 2012/13 | 2013/14 | 2014/15* |
|---|---|---|---|---|---|
| wks 40-20 | 1460 | 235 | 935 | 762 | 2118 |
* Figures for 2014/15 are provisional (based on data on the SMR01 linked database as at mid-July 2015)
Chart 2: The Number of hospital stays with 'any diagnosis' of flu, by week and flu season, 2010/11 to 2014/15
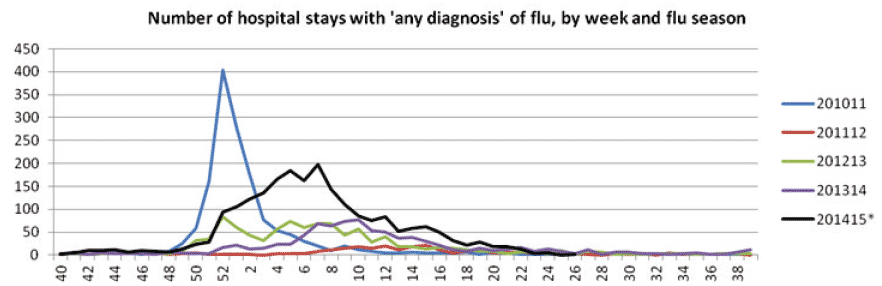
Source: Health Protection Scotland
In Winter 2014/15 pressures from delayed discharge continued through to December 2014 and eased significantly from January 2015
16. Bed days occupied by delayed discharge patients continued to increase through to December 2014 to over 55,000 bed days. Bed days occupied by delayed discharge patients began to reduce at the turn of the year to just under 47,000 in May 2015.
Chart 3: Bed days occupied by delayed discharge patients, April 2012 - May 2015
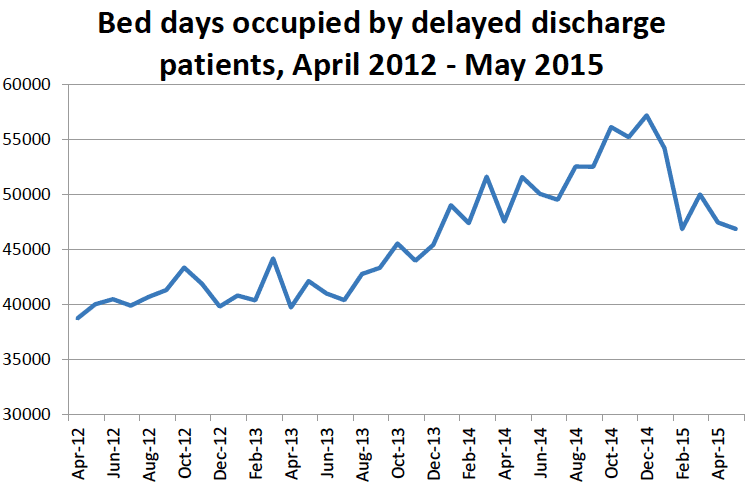
Source: ISD Scotland
The norovirus season was relatively mild, and the weather was not particularly cold
17. The norovirus season 2014-15 was relatively low compared to the 2008-2014 season average. Significant effort has gone into improving norovirus outbreak prevention, preparedness, detection and management, the circulating virus strain is also key to determining how much impact norovirus will have on hospitals.
18. The average temperatures this winter were broadly comparable with the 30 year averages.
In Winter 2014/15 pressures impacted on A&E waiting times performance with A&E waiting times performance improving significantly in to the spring and summer
19. The length of time A&E patients wait to be seen, treated and discharged can be a proxy measure of how the NHS is managing the pressures it is facing. The increased flu and respiratory emergency activity will have contributed to the reduced A&E waiting times performance in December, January and February 2015. Particular challenges were faced in NHS Ayrshire & Arran, NHS Greater Glasgow & Clyde, and NHS Lanarkshire. These boards historically have relatively high levels of emergency activity. The Scottish Government worked closely with these boards over the winter.
20. A&E waiting times performance improved significantly through the end of the winter in to spring. Official statistics published for May 2015 on core and Minor Injury Units show 4 hour A&E performance was 93.5 per cent and up on the May 2014 figure of 92.7 per cent. Weekly official statistics for core sites showed performance increased to over 95 per cent during the weeks ending 12 and 19 July 2015.
Chart 4: NHS Scotland, 4 hour A&E performance, winter 2012/13 to 2014/15
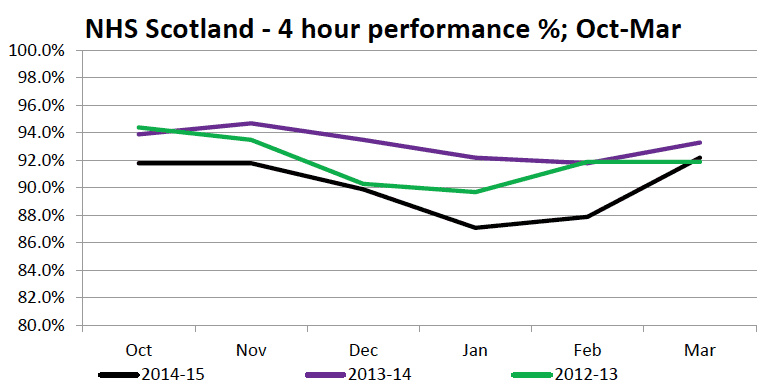
Source: ISD Scotland, A&E Datamart
Table 2: NHS Scotland Monthly A&E 4hr Performance, by month in winter 2012/13 to 2014/15
| Year | Oct | Nov | Dec | Jan | Feb | Mar | Range % points |
|---|---|---|---|---|---|---|---|
| 2014-15 | 91.8% | 91.8% | 89.9% | 87.1% | 87.9% | 92.2% | 5.03 |
| 2013-14 | 93.9% | 94.7% | 93.5% | 92.2% | 91.8% | 93.3% | 2.90 |
| 2012-13 | 94.4% | 93.5% | 90.3% | 89.7% | 91.9% | 91.9% | 4.73 |
Source: ISD Scotland, A&E Datamart
Table 3: Monthly A&E 4hr Performance, by board by month in winter 2014/15
| 2014 /15 | Oct-14 | Nov-14 | Dec-14 | Jan-15 | Feb-15 | Mar-15 | Winter |
|---|---|---|---|---|---|---|---|
| NHS AYRSHIRE & ARRAN | 91.9% | 91.3% | 89.5% | 82.1% | 82.7% | 87.8% | 87.6% |
| NHS BORDERS | 96.7% | 97.8% | 91.1% | 90.2% | 91.4% | 91.8% | 93.1% |
| NHS DUMFRIES & GALLOWAY | 95.9% | 97.5% | 97.2% | 96.1% | 94.3% | 96.8% | 96.3% |
| NHS FIFE | 91.6% | 95.2% | 90.9% | 92.6% | 90.8% | 92.5% | 92.3% |
| NHS FORTH VALLEY | 91.2% | 92.4% | 84.2% | 89.0% | 95.7% | 93.6% | 91.0% |
| NHS GRAMPIAN | 93.6% | 95.0% | 94.4% | 89.9% | 91.7% | 95.0% | 93.3% |
| NHS GREATER GLASGOW & CLYDE | 89.2% | 88.4% | 84.5% | 79.9% | 79.6% | 88.5% | 85.2% |
| NHS HIGHLAND | 96.8% | 97.7% | 96.9% | 96.8% | 96.7% | 97.4% | 97.1% |
| NHS LANARKSHIRE | 87.0% | 83.0% | 86.5% | 87.0% | 85.5% | 91.8% | 86.9% |
| NHS LOTHIAN | 92.7% | 94.2% | 92.4% | 87.2% | 91.6% | 92.6% | 91.8% |
| NHS ORKNEY | 99.5% | 99.5% | 98.8% | 99.0% | 96.9% | 99.7% | 98.9% |
| NHS SHETLAND | 94.6% | 97.0% | 98.1% | 97.8% | 97.7% | 97.2% | 97.1% |
| NHS TAYSIDE | 99.2% | 99.0% | 98.8% | 99.2% | 99.2% | 99.3% | 99.1% |
| NHS WESTERN ISLES | 97.3% | 98.6% | 97.0% | 97.5% | 97.3% | 99.0% | 97.8% |
| NHS SCOTLAND | 91.8% | 91.8% | 89.9% | 87.1% | 87.9% | 92.2% | 90.2% |
Source: ISD Scotland, A&E Datamart
21. Despite the increase in the number of calls, NHS 24 maintained high performance throughout the year exceeding its key performance target of answering 90 per cent of calls within 30 seconds during winter 2014/15. The winter presented a number of challenges for the Scottish Ambulance Service. The average Cat A performance from October 2014 to March 2015 is 70.2 per cent for the six month period. In that period, the performance ranged from 73.2 per cent in October 2014 to 68.4 per cent in February 2015. This reflects some regional challenges particularly in the West of Scotland where demand is traditionally high. The Scottish Ambulance Service worked closely with Boards in these areas developing action plans to improve patient discharge and hospital turnaround times.
Core A&E waiting times performance was higher in Scotland compared to the rest of UK in Winter 2014/15
22. Official statistics on waiting times in large Accident & Emergency departments are published by each of the four UK countries. While this report does not consider the nature of the pressures faced in other parts of the UK, the statistics suggest that all countries in the UK experienced increased pressures this winter. This winter, performance in Scotland was marginally above that in England, and significantly above the performance in Northern Ireland and Wales. Whereas in the previous winter England's performance was marginally above that of Scotland.
Table 4: UK A&E "Core" sites 4 Hr Performance, winter 2013/14 - 2014/15, percentage
| 'Winter' Oct-Mar 2013-14 |
'Winter' Oct-Mar 2014-15 |
Percentage point change | |
|---|---|---|---|
| Scotland | 92.4 | 88.9 | -3.6 |
| England | 93.1 | 88.2 | -4.9 |
| Wales | 86.6 | 79.3 | -7.3 |
| Northern Ireland | 73.3 | 72.4 | -0.9 |
Source: ISD Scotland, NHS England (derived from weekly statistics), NHS Wales Informatics and DHSSPSNI
Table 5: UK A&E "Core" sites 4 Hr Performance, by month in winter 2014/15, percentage
| Month | Scotland Core |
England Type 1 |
Wales Major |
N Ireland Type 1 |
|---|---|---|---|---|
| Oct 2014 | 90.8 | 90.7 | 81.3 | 75.4 |
| Nov 2014 | 90.6 | 90.2 | 80.3 | 77.4 |
| Dec 2014 | 88.6 | 85.3 | 77.2 | 73.5 |
| Jan 2015 | 85.4 | 86.0 | 78.6 | 71.4 |
| Feb 2015 | 86.2 | 87.7 | 80.0 | 67.3 |
| Mar 2015 | 91.1 | 89.0 | 78.4 | 69.7 |
Source: ISD Scotland, NHS England (derived from weekly statistics), NHS Wales Informatics and DHSSPSNI
NHS Boards reported increased levels of cancellation of elective inpatients
23. With the increased pressures in emergency activity, NHS Boards reported increased levels of cancellation of elective inpatients on the day or day before the planned procedures over the winter. Official statistics on cancellations were developed over the spring and were released for the first time in June 2015.
24. NHS Boards plan elective activity throughout the year and can carry out additional activity before winter - so as to build resilience in to their system. The reported increase in elective activity last winter was predominately seen in October through December. The reported increase in elective procedure cancellations had an impact on the inpatient and day case treatment time guarantee. The proportion of elective inpatient and day cases that were seen within 12 weeks reduced from 97.1 per cent in quarter ending December 2014 to 94.5 per cent in quarter ending March 2015.
Season Flu Vaccination
25. Early data on seasonal flu uptake by staff in 2014/15 was 36.3 per cent. This represents an increase on 2013/14 when uptake was 34.7 per cent, but overall recorded uptake still remains low and below the 50 per cent target. Some individual Boards consistently achieve higher levels of uptake, which may reflect local circumstances, but it may also reflect the initiatives and approaches adopted.
26. Last winter more than two million Scots were offered the free flu vaccine. People at greater risk from flu, including those with underlying health conditions, pregnant women and those aged 65 were encouraged to get the vaccine. Provisional uptake rates are shown in the table below.
Table 7: Provisional seasonal flu uptake rates, 2014/15
| Eligible Groups | Uptake | Target |
|---|---|---|
| 65 and over | 76.3% | 75% |
| Under 65 at risk | 54.0% | 75% |
| Pregnant Women (without risk factors) | 49.5% | 75% |
| Pregnant Women (with risk factor) | 65.0% | 75% |
| 2-5 year olds (not yet at school) - vaccinated at GP practice | 56.4% | 60%* |
| Schoolchildren aged 5-11 (P1-P7) - vaccinated at school | 71.8% | 75% |
* This target will rise to 65% for the 2-5 year olds in the 2015-16 programme
Source: HPS (National Influenza Report - week ending 17 May 2015)
27. Last winter (as part of the extended childhood programme), all children aged 2-5 (not yet at school) were offered immunisation through their GP practice, with all primary school-aged children (primary 1 to primary 7) - including those in at-risk groups who would formerly have been vaccinated in GP surgeries - being offered immunisation at school.
28. Children of primary school age received a letter and consent form in their school bag. If they had no contra-indications they were given Fluenz Tetra, a live attenuated vaccine administered by nasal spray. Otherwise they were given an intra-muscular injection. Children of parents with particular faith issues with the porcine element of the Fluenz nasal spray were offered the injection instead. Health Boards in Scotland offered a range of mop-up facilities for children unable to attend school on the day of the vaccination, in order to ensure maximum protection for the school population.
29. The flu vaccine offered each season offers the best chance of protecting against flu. Vaccination is highly recommended for those in 'at risk' categories, including people aged over 65. Each year, a supply of flu vaccines is produced in the UK before our flu season starts to ensure sufficient supplies are in place to vaccinate relevant groups in the population in advance of the flu virus circulating. The different vaccines created each year are based on an analysis of the strains of the flu virus most likely to be circulating. These strains can change due to the fluid nature of the flu virus so the vaccine created may not cover all strains. Each year, it is therefore possible for someone to get flu even though they had the vaccine.
30. During the last 10 years, the flu vaccine has generally been a good match for the circulating strains of flu. However this season's vaccine was less well matched to one of the chosen A flu strains. This was because a slightly different A/H3N2 subtype was circulating early in the season. This is referred to as 'drift'. However messaging has remained clear. Being immunised is still the best protection available against an unpredictable virus that can cause severe illness and is the best way to protect yourself from flu.
Integration of health and social care, improving delayed discharge and fresh 'six essentials' approach to improving unscheduled care across Scotland underpin the winter guidance for 2015/16 with additional emphasis on planning for the additional pressures and business continuity challenges that are faced in winter
31. Scottish Government officials, along with the Joint Improvement Team, have been working with new integration partnerships to develop innovative solutions to delayed discharges, many of which also have potential to reduce avoidable admissions. Partnerships are being supported to develop strategic commissioning plans. Strategic Commissioning will be the vehicle under integration to deliver the shift in the balance of care from institutional settings into the community.
32. An additional £100m is being made available to integration authorities over the next three years to help local partnerships deliver the integration indicators, including a move to discharging mare patients within 72 hours of being ready for discharge. Funding will be issued in three instalments of £30m in 2015/16; £35m in 2016/17 and £35m in 2017/18.
33. The Scottish Government has also developed a fresh approach to improving unscheduled care across Scotland - in winter and all year round - which is based on six essential actions. The approach builds on the actions taken over the previous two years through the £50 million national unscheduled care action plan to strengthen unscheduled care.
Essential Action 1 - Clinically Focussed and Empowered Hospital Management
This Essential Action is about the Clinical Leadership and operational management of basic hospital and facilities, determining appropriate staffing levels linked to activity, creation of clear escalation policies and appointment of an appropriate site director alongside medical and nursing chiefs of staff and duty managers across all services and targets. This is central to what we do around performance and management on a day to day basis within our acute sector hospitals and working across a whole system approach.
Essential Action 2 - Hospital Capacity and Patient Flow (Emergency and Elective) Realignment
This will establish and then utilise appropriate performance management and trend data to ensure that the correct resources are applied at the right time, right place and in the right format. The initial work will establish a current footprint of flow into, through and out of the hospital to identify where capacity meets or does not meet demand. It will examine where solutions such as streaming and high volume specialty pathways will improve flow and the hidden consequences of altering current systems. Wider work in this area will centre around producing a combined elective and emergency capacity plan for each of the major sites as well as promoting increases in day-case surgery, for example.
Essential Action 3 - Patient Rather Than Bed Management - Operational Performance Management of Patient Flow.
This Essential Action will examine processes that follow and facilitate the patient journey (flow) rather than about bed management. A key outcome will be focussed on coordinated planning and implementation of appropriate discharge without delay. This includes focus on early morning and weekend discharge. This will require engagement with all departments such as laboratory, pharmacy and allied health professionals as well as discharge lounges and transport services. This workstream is basically all about effective patient tracking through the pathway and is about operational management grip and control. From an unscheduled and scheduled care point of view, and from a patient centred point of view. These aspects should be coordinated to ensure optimum focus on effective discharge.
Essential Action 4 - Medical and Surgical Processes Arranged to Improve Patient Flow through the Unscheduled Care Pathway
This Essential Action will ensure that internal hospital departments are geared with appropriate links to pull patients from the Emergency Department (for example, assessment units and acute receiving wards) with appropriate workforce and job planning to ensure that this becomes a reality. This action should ensure that there is prompt access to appropriate assessment and clinical intervention from specialists in the appropriate environment to enhance patient experience and establish care management plans promptly, minimising unnecessary waits and delays wherever possible.
Essential Action 5 - Seven Day Services Appropriately Targeted to Reduce Variation in Weekend and Out of Hours Working
We already have a national programme for Seven Day Services led by a Task Force of clinical and operational experts and the Unscheduled Care programme will align itself closely to this, supporting priorities that improve unscheduled care. The priority will be to reduce evening, weekday and weekend variation in access to assessment, diagnostics and support services focused on where and when this is required to: avoid admission where possible, shift emergency to urgent care, reduce length of stay, and improve weekend and early in the day discharges safely. The activities of the seven day task force will also support aspects of Essential Actions 3 and 4.
Essential Action 6 - Ensuring Patients are Optimally Cared for in their Own Homes or Homely Setting
This essential action will consider how someone who has an unscheduled care episode can be optimally cared for, or discharged to their own home, as soon as possible. This work will align to other portfolios of work ongoing to enhance self-management and longer term focus on preventative care and improvements in access to self- directed care and enablement services for complex conditions and comorbidity will be supported by the introduction of Integrated Joint Boards and community care developments. Managing the patient journey to promote living well and dying well at home includes a focus on patient led self-care and improved communication between the whole system health care team.
34. The Cabinet Secretary announced this new unscheduled care 'six essentials' approach in January and launched it in May. It is aimed at improving outcomes for people who are using the services while recognising this is a multi-disciplinary issue that requires commitment across every part of the health and social care system to ensure better care on a sustainable basis. It joins up several work strands to ensure a much more strategic approach and will provide a clear focus on early joint winter preparation between health boards and new integration partnerships to develop plans and put in place adequate services to ensure optimum care is in place for winter.
35. These key actions have underpinned improvements in NHS Boards last winter, for example the Royal Alexandria hospital in NHS Greater Glasgow and Clyde, to ensure best practice is installed throughout the hospital system. Each Health Board will appoint dedicated teams to work with the National team to ensure these actions are implemented timeously to support winter.
36. Planning guidance for winter 2015/16 has been developed for NHS Boards and their partners. The guidance has been issued at the same time as this report on last winter. The guidance is based on the work to improve delayed discharge and the unscheduled care six essentials with additional focus on planning for the additional pressures and business continuity challenges that are faced in winter. It focusses on the outcomes to be achieved and local indicators to support delivery. The winter guidance covers the following:
i) Safe & effective admission/discharge continues in the lead-up and over festive period and also in to January
ii) Workforce capacity plans & rotas for winter / festive period agreed by October
iii) Whole system activity plans for winter: post-festive surge / respiratory pathway
iv) Strategies for additional winter beds and surge capacity (community/hospital)
v) The risk of patients being delayed on their pathway is minimised
vi) Discharges at weekend & bank holiday
vii) Escalation plans tested with partners
viii) Business continuity plans tested with partners
ix) Preparing effectively for norovirus
x) Delivering seasonal flu vaccination to public and staff
xi) Communication plans
xii) Winter analysis
Improved access to official statistics
37. This year saw the introduction of weekly A&E activity and performance statistics for the 30 core sites in Scotland (formerly quarterly); monthly A&E activity and performance statistics for all sites in Scotland including minor injury units (formerly quarterly); and monthly statistics on delayed discharge. A new website called NHS Performs was also developed to make it easy to access statistics about hospitals and NHS Boards in Scotland.