HEALTH FOR ALL CHILDREN 4: GUIDANCE ON IMPLEMENTATION IN SCOTLAND 2005
Guidance to support implementation in Scotland of Royal College of Paediatrics & Child Health recommendations on child health screening and surveillance activity.
Introduction
1.1 In 1988, the Royal College of Paediatrics and Child Health ( RCPCH) established a multi-disciplinary working group to review routine health checks for young children. Its report, first published in 1989, was entitled Health for All Children. In later years, the remit of the review was extended beyond routine checks to detect abnormalities or disease, to include activity designed to prevent illness and efforts by health professionals to promote good health. The report of the most recent RCPCH review of child health screening and surveillance programmes in the UK was published in February 2003 as the fourth edition of Health for All Children1, and is commonly referred to as Hall 4.
1.2 In February 2003, the Child Health Support Group, with the Scottish Executive Health Department, organised a national consensus conference to inform professionals and managers in NHSScotland and partner organisations about Hall 4 and to provide an opportunity to consider whether and how to implement its recommendations in Scotland. Stakeholders welcomed the proposals in Hall 4, and asked the Scottish Executive to provide national guidance on how best to apply the recommended core programme of child health surveillance, screening and health promotion in Scotland, and how to identify and target support for vulnerable children and families. The Child Health Support Group established a multi-disciplinary reference group, chaired by Dr Zoë Dunhill MBE, to assist preparation of this guidance 2.
1.3 Draft guidance was published in December 2003 for a three-month consultation. Children 1st were commissioned to undertake some focus group consultation with parents on behalf of the Scottish Executive, and submitted a report of their findings for consideration with other consultation responses. Reid Howie Associates undertook an analysis of the 153 consultation responses received, and have prepared an overview report, published concurrently with this guidance 3.
1.4 The majority of respondents welcomed implementation of Hall 4 in Scotland, and the draft guidance. Many respondents provided helpful comments and suggestions to strengthen the draft guidance, and wherever possible, these have been taken on board in finalising this guidance. In particular, an action template is now included as an appendix, to assist NHS Boards and their partners in developing implementation plans.
1.5 Many of the concerns raised in the consultation related to the original Hall 4 recommendations. The RCPCHHall 4 working group considered the best available evidence in arriving at their conclusions and recommendations, and this guidance does not, therefore, revisit these.
Aims of the guidance
1.6 This guidance has been prepared to support consistent implementation across Scotland of the recommendations made by the RCPCH in the fourth edition of Health for All Children ( Hall 4). In doing so, it sets Hall 4 in the context of other Scottish policies to promote effective and integrated provision of universal and targeted services for children and families, and describes the activity needed for implementation at national and local levels. It is not, and cannot be, a comprehensive guide to child health.
1.7 First and foremost, the rights and responsibilities to provide for their children's health and welfare rest with parents; this is enshrined in the Children (Scotland) Act 1995. But a range of services provided by the NHS, local authorities and voluntary and independent organisations, in health centres, nurseries, pre-schools and schools, family centres and community-based support services have a vital role in helping parents to ensure their child's healthy development and maximise their potential.
1.8 This guidance describes activities and initiatives already in place in Scotland; describes activities that are happening but not consistently around Scotland or to a sufficient level to meet the requirements of Hall 4; and makes recommendations, based on Hall 4, for changes to current practice. This guidance does not make an explicit distinction between these three aspects. Rather, it should be read as a holistic guide to child health surveillance and screening in Scotland, proposing that all aspects should be in place for effective child health promotion, screening and surveillance. This guidance also describes some initiatives that are currently in a developmental or pilot phase and will provide additional learning over the next few years to inform effective child health promotion and surveillance.
1.9 Throughout this guidance, the term "parent" includes all those with parental responsibility, including carers.
Who is the guidance for?
1.10 This guidance reflects the evidence-based framework set out in Hall 4, for intervention to assess, monitor and support children's health and development throughout childhood and adolescence, based on staged intervention and underpinned by strong health promotion activities. All those involved in planning, managing and delivering services for children and families have a role in ensuring its success.
1.11 The framework set out in Hall 4 is firmly rooted in the need for an integrated approach to the delivery of services and support for children and families. This guidance is therefore for the range of professionals who work with children and families, including social workers, family support workers, community learning development workers, and practitioners in state and independent sector schools and early years settings, as well as staff in NHSScotland who plan, commission and provide care and treatment for children.
1.12 The Scottish Executive proposes to work with NHS Health Scotland to develop a leaflet for parents, setting out the core programme of screening, surveillance and health promotion and explaining the service that they will receive. NHS Boards will be responsible for disseminating this to parents, and advising how the programme is being rolled out in their area.
What does Hall 4 say?
1.13 The fourth RCPCH review examined the evidence for existing child health surveillance and screening activity, including the purpose, content and timing of interventions. It takes account of the impact of social, economic and environmental factors on children's health. The recommendations in Hall 4 also reflect the advice of the National Screening Committee ( NSC), which considers all screening programmes on a national level.
Child health surveillance - used to describe routine child health checks and monitoring.
Child health screening - the use of formal tests or examination procedures on a population basis to identify those who are apparently well, but who may have a disease or defect, so that they can be referred for a definitive diagnostic test.
Health promotion - used to describe planned and informed interventions that are designed to improve physical or mental health or prevent disease, disability and premature death. Health in this sense is a positive holistic state.
1.14 The recommendations in Hall 4 reflect a move away from a wholly medical model of screening for disorders, towards greater emphasis on health promotion, primary prevention and targeting effort on active intervention for children and families at risk. The philosophy and recommendations set out in Hall 4 aim to:
- Establish an evidence-based core universal child health programme of screening, surveillance and health promotion, that effectively supports children's health and development.
- Ensure that parents are supported and empowered to keep their children healthy and safe.
- Ensure that the needs of vulnerable children and families are identified and met.
- Promote the development of seamless support through integrated models of service delivery to make best use of available skills and resources across agency boundaries.
- Promote a holistic model of family care, in which adult services recognise the impact of adult physical or mental ill health on children in the family.
- Promote the need to monitor population health through systematic and effective data recording.
- Highlight the need for efficient information sharing.
1.15 The guidance recognises that it is also important to empower and support children and adolescents themselves to take responsibility for their own health needs.
1.16 The RCPCH review found little or no evidence for the effectiveness of some of the health checks currently carried out by health professionals on children's health or wellbeing. Consequently, Hall 4 recommends that certain checks be discontinued and that a reduced core programme of child health surveillance, with some enhanced screening activity, be offered to all children based on interventions proven to be effective in supporting children's health and development. Hall 4 also recommends that this should incorporate enhanced health promotion work to inform and educate parents about their children's development and needs, so that they can seek the right advice and help when they need it. These proposals recognise the regular contact that children and families have with other professionals in, for example, pre-school or family centres, and highlight a need to draw more effectively on these, by providing increased support and ensuring that there are clear routes for liaison, consultation and referral to health professionals when there are concerns about a child.
1.17 Hall 4 recommends more effective targeting of support for those children and families who are most in need, whether by virtue of disability, disadvantage or other stresses. For the first time, the report includes recommendations for children's care from birth to adolescence.
1.18 Hall 4 also stresses that screening and surveillance activity is of no value unless supported by high quality and accessible diagnostic, treatment and care services, planned and developed with service user involvement.
1.19 The Executive Summary from the fourth edition of Health for All Children is included in this guidance as Annex 2.
Key principles
1.20 The NHS provides a universal service to all families with young children. Current policy recognises the need to target that service more effectively in order to ensure that those families with greatest need receive the greatest level of support. This is reflected in the recommendations made in Hall 4.
1.21 Scottish data 4 show that take up of health promotion advice and child health screening and surveillance contacts is much higher amongst parents from more affluent areas and circumstances, with children in need more likely to remain disadvantaged in health status and access to health care. When formal child health checks are made at 6-8 weeks, almost one in 10 children in deprivation 5 categories 6 and 7 do not attend clinic appointments. By the time checks are made at 22-24 months, almost one in four children in deprivation categories 6 and 7 do not attend for clinic appointments, and this rises further to almost two in five children by the routine checks that currently take place at 39-42 months.
1.22 Hall 4 is based on the principle of universal access to NHS services, but recommends that the way in which those services are delivered must be tied much more closely to identified need. In other words, universal access to NHS services does not necessarily have to mean uniform provision of those services.
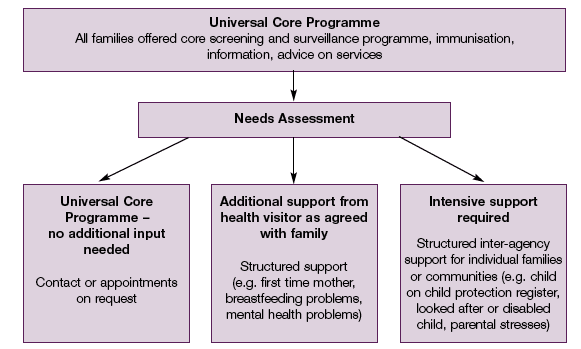
1.23 There will always be a need to ensure universal provision of a health promotion and surveillance programme for all children and young people to enable families to take well informed decisions about their child's physical and mental health and development; to identify children with particular health or developmental problems; and to recognise and respond when a child may be in need. This guidance sets out a core programme of contacts that every parent can expect, wherever they live in Scotland. However, beyond this, contacts must be determined on the basis of each family's circumstances and needs, which will be different. Some parents need only information and ready access to professional advice when their child is injured or unwell or when they are worried about their child's development or welfare. Other parents may need considerable support, guidance and help at specific times, or over a continuous period, perhaps because of their child's serious ill health or disability, or because of their own personal circumstances. This approach is represented in the diagram below.
1.24 Nursing for Health6 advocated the development of Family Health Plans as an instrument to help families to think, with their health visitor, about their health and wellbeing.
For families where a particular need had been identified, the plan would provide a means to record those needs, to set clear goals to address them, and actions that both professionals and the family would take in order to do so. NHS Health Scotland commissioned research on the potential development of Family Health Plans, followed by a consensus conference in September 2003. The Family Health Plan concept will be given further consideration within the context of the Integrated Assessment Framework ( see Policy Context section).
1.25 In line with the recommendations made in Hall 4, this guidance promotes:
- A shift away from child health surveillance activity that concentrates on prevention and detection of specific developmental problems and disorders, to a more holistic approach which supports parents to ensure that they have the information, skills and resources they need to maximise their child's potential.
- A refocused universal core programme of routine child health contacts that all families can expect, wherever they live in Scotland, with additional support and contacts for some families or communities on the basis of assessed need.
- Enhanced neonatal and pre-school screening within the universal core programme to achieve optimum detection and treatment for specific conditions.
- Improved team working so that parent support, health promotion and child assessment activities already being undertaken by a range of children's services - in, for example, family centres, nurseries and schools - support the early identification and referral of children with additional needs for support.
- Development of community involvement and development approaches to public health promotion for child health, with priority for action in areas of disadvantage, in conjunction with Community Health Partnerships.
1.26 Allocation of NHS resources, such as input from health visitors and school nurses, should reflect the greater concentration of need.
1.27 Hall 4 indicates that population-based child health screening and surveillance is only one way in which children's health problems are detected. Evidence has shown that parents notice and seek help for most significant health problems in the first instance, especially if they receive timely, appropriate and accessible information. Other family members, playgroup staff, childcare workers, nursery nurses, teachers and GPs may also detect problems in the course of their general contact with a child.
1.28 Individual children and families will require routine and targeted support from a range of professionals and agencies. Effective health promotion can also be universal and targeted and health promotion measures will require both a population focus, with information in a range of media provided to the public or sections of the public at large, and more focused and tailored information, targeted at vulnerable individuals and communities.
1.29 Central to the delivery of any new child health programme are integrated processes for assessment and planning services to meet the needs of families with identified needs. In order to ensure that a reduced universal core programme of contacts is augmented by targeted approaches to meeting the needs of families, the following will be needed:
- Reliable, effective and consistent assessment tools and approaches.
- Universal and tailored packages of information to underpin the programme.
- An effective needs assessment and planning process.
- An efficient information system that supports professional activity.
- Appropriate and efficient sharing of information between professionals about children with particular needs.
1.30 These issues are explored in more detail in this guidance.
Achieving change
1.31 Implementation of this guidance, along with the NHS modernisation programme already underway, provides an opportunity for coherent planning to shape the future of child health services. Effective implementation of the recommendations made in Hall 4 and in this supporting guidance will require:
- Genuine joint working between services and agencies.
- Effective information exchange and transfer protocols and systems.
- Effective cross-referral mechanisms.
- Multi-agency staff training and development.
- Clear referral protocols and pathways which are familiar and accessible to non-health professionals.
1.32 Planning for implementation, including decisions about prioritisation, should therefore be considered on an inter-agency basis, and within the integrated children's services planning context. NHS Boards should agree with local authority planning partners an organisational development plan for implementation of this guidance over a three year period, aiming for full implementation by 2008.
1.33 Workforce planning and development will obviously be a key element in planning for implementation of Hall 4. This will require local planning partners to identify the contribution of staff across agencies and services to health improvement and support for children and families, and action to ensure that mechanisms are in place to support these contributions. The opportunity to develop the individual roles of primary care, health promotion, nursery, childcare and school staff will be key to implementing Hall 4. To support this, NHS Boards should consider:
- Allocation of a named health visitor or school nurse for every pre-school establishment.
- More and regular health visitor or school nurse time in pre-school setting and family centres, to ensure effective liaison, support and training for non-health professionals.
1.34 Pre-qualifying training may also need to take this into account and the Scottish Executive will consider this issue with training providers. NHS Education for Scotland is currently reviewing the child health workforce in the context of a range of national policy developments, with a view to developing an associated educational framework.
1.35 Scottish Ministers have established a Cabinet Delivery Group on Children and Young People to drive forward work across the Scottish Executive to secure an integrated approach to the delivery of services focussed on children. The Delivery Group, which includes the First Minister and Ministers with responsibilities for health, education, justice, communities and finance, has identified workforce development issues as one of its five priorities for action. A National Review of the Early Years and Childcare Workforce is currently underway, examining roles and responsibilities, qualifications and training, recruitment and retention, career pathways and workforce planning. The Review is expected to be complete by the Summer of 2005, and will provide the longer-term direction for qualifications and training for early years and childcare staff.
1.36 To support local planning, an action template is attached at Annex 1, summarising the key areas of activity that NHS Boards are expected to take forward with their local partners.
Resources
1.37 The reduction in the number of universal routine contacts and developmental checks by health visitors and school nurses is expected to release some capacity to provide additional or intensive support for those children and families most in need.
1.38 The best way of delivering against a common set of outcomes, shared across all agencies, may be to pool or align resources with partners to deliver key inputs. For example, local authorities and NHS Boards might consider pooling resources to expand child and family support services.
Accountability and monitoring
1.39 This guidance is intended to be used to support local planning through integrated children's services planning arrangements. The Scottish Executive will be monitoring integrated children's services plans for each area, and these, together with annual updates, will inform the accountability process for NHS Boards. The Scottish Executive is working to rationalise existing quality improvement and accountability arrangements across services for children and young people. This will include new arrangements for an integrated system of inspection of services for children.
1.40 The Integrated Children's Services Planning Guidance lists the current performance indicators that the Scottish Executive and NHSScotland use to monitor progress in improving the health of children and young people. Revised and more focused national indicators will be published in 2005, as part of a quality improvement framework for services for children, young people and their families.
1.41 Responsibility for ensuring delivery of the universal core child health programme and of targeted support will continue to rest with the Chief Executive of the NHS Board, and for those aspects of the programme commissioned or delivered by local authority staff, with the Chief Executive of the local authority. In most cases, responsibility for delivery is likely to lie with Community Health Partnerships.
1.42 In terms of monitoring trends more generally, the Scottish Executive has commissioned Growing Up in Scotland, a longitudinal social survey to monitor the impact of Scottish Executive early years policies on longer term outcomes for children and young people. The survey will track a number of representative cohorts of children from birth until the age of 5. The first cross-sectional times series data are expected to be available for 2-3 year olds in 2007, 3-4 year olds in 2008 and 4-5 year olds in 2009. This will be published by the Scottish Executive.