The Future of Residential Care for Older People in Scotland - Full Report
A strategic examination of the purpose and desired structure of residential care services fit for the aspirations and needs of future generation.
Current Landscape
Demographic projections of recent years have presented a picture of a growing older population and a shrinking working age population to support it.
According to the latest figures from the National Records of Scotland, Scotland's population is projected to increase by 9 per cent between 2012 and 2037, however this increase is not spread evenly across all age groups of the population. As Figure 1 below shows, the population aged under 60 is projected to remain fairly constant with a small decrease in the 45-59 age group and a small increase in the number of the 0-15 age group whilst the number of older people is projected to increase significantly especially the 75+ age group. The number of people aged 75 and over is projected to increase from 0.42 million in 2012 to 0.53 million in 2022. It is then projected to continue rising, reaching 0.78 million in 2037 - an increase of 86 per cent over the 25 year period. Meanwhile, the number of people of working age is projected to increase from 3.35 million in 2012 to 3.48 million by 2037 (an overall increase of 4 per cent from the 2012 estimate).[2]
Under current law, changes to the State Pension qualifying age will increase to 67 between 2034 and 2036, and 68 between 2044 and 2046.[3] This will in the long term mean that staff in the workforce are likely to be working in the sector for longer, which itself will bring opportunities and challenges.
Figure 1 The projected percentage change in Scotland's population by age group, 2012-2037
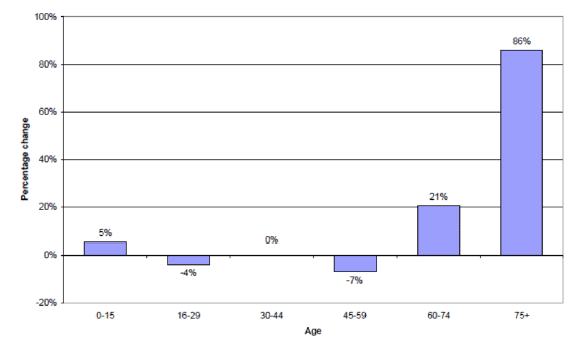
Source : General Register Office for Scotland; Projected Population of Scotland (2012 based)
Analysis and debate is on-going as to what exactly this means for health and social care, but the over-arching message is clear: our residential care sector as it exists at present is unsustainable and in certain cases, un-desirable. Just as the sector has evolved in response to developments in technologies and services over the last few decades, so too it must align itself to meet the needs and desires of our older population in the next twenty years.
The most recently available Scottish Care Home census, which provides information as at the census date of the 31st of March 2012 tells us that at that time there were 916 care homes for older people in Scotland providing 38,465 places to 33,636 residents.[4] Of those residents, at the time of the census, 32,555 (97%) were long stay residents - i.e. had the care home as their permanent residence. Short term and respite residents made up 1,081(3%) of residents.4
The fact that we are living longer can be put down to a range of factors, from perhaps healthier lifestyle choices, advances in medicine and technologies, and a preventative approach to health and social care that has been implemented at national and local levels.
By way of illustration, the gap between Life Expectancy and Healthy Life Expectancy (i.e. the years expected to be spent in a 'not healthy' state during the average lifetime) has been fairly constant for females between 1980 and 2008, but has tended to increase for males. The most recent annual estimates for Scotland are for boys born in 2010 to live 76.3 years on average, 59.5 of these in a 'healthy' state. Girls born in 2010 would be expected to live 80.7 years on average, 61.9 of these years being 'healthy'.[5]
Generally, both Life Expectancy and Healthy Life Expectancy are increasing for males and females across Scotland, allowing people to live independently for longer today compared to the 1980s for example. There has therefore been a marked shift in the demographics of care home residents, and we know that the average age of a resident in a care home is increasing due to the fact that people are moving into care homes at a later stage in life than previously.
Given the age, frailty and multiple morbidities of care home residents they can be defined as one of the most complex and vulnerable group of people in our communities, which has significant implications for the workforce providing their care and support. Added to this we know that 21% of the population over 65 have a care home as place of death so increasingly palliative and end of life needs also require to be met in a residential care setting.
Residents in care homes have increasingly complex and high levels of care and support needs. According to the 2012 census, 1 in 2 long stay residents (i.e. 16,277 people)[4] had a formal diagnosis of dementia. The true level of dementia is likely to be higher than this given that some of those residents will not have had a formal diagnosis but will have been identified as having a dementia.
In recent years, a preference towards caring for older people in their own homes or within the community rather than in a care home has been driven by policy intent in this area. The Scottish Government's vision for older people is that:
"Older people are an asset, their voices are heard and they are supported to enjoy full and positive lives in their own home or in a homely setting."
This vision appears to be taking hold. The number of older people receiving personal care services in their own homes has increased from 33,000 people in 2003-04 to nearly 47,000 people in 2010-11 and 2011-12.[6] This large increase in people receiving services in their own homes reflects an increasing older population and a move away from long-term care in hospital and care homes toward providing care in a person's own home for as long as possible. People receiving personal care services at home received on average nearly 7 hours of care each week in 2003-04. This has risen steadily to over 8 hours of care each week in 2011-12, showing that people receiving care at home have increasing levels of need.
Supporting our older population and their spectrum of needs, whether in a care home or at home, requires a considerable workforce with the right skills.
According to the Scottish Social Services Council's Workforce Report (2012), there are 115,410 people employed as carers delivering care in care homes (54,060), and care at home and housing support services (61,350).[7] To put this into context, 28% of the Scottish Social Services sector is employed in care homes, and 32% in care at home/housing support services.
Social care as a vocation has generally always been viewed as demanding and poorly paid. This has made it difficult to attract the right kind of people with the outlook and behaviours to boost its image, and indeed that image has suffered further recently. Despite the vast majority of the workforce working hard to deliver the best level of care possible, the few instances where the level of care and behaviour of staff has been sub-standard has tarnished the image of social care. Inevitably, this will take time to repair, yet the fact that such instances are coming to light both reassures us that regulation is working, and also underlines the areas we really have to get right within this piece of work.
The integration of Health and Social Care is set to change the landscape in which these services are delivered. Essentially, the Public Bodies Bill will create the framework for strategic planning to take place within partnerships to ensure that energies and resources are focussed on getting the services and placements that meet people's needs.
The manner in which care services are funded is also proving an issue. The main parties in the National Care Home Contract have found it increasingly difficult in recent years to reach consensus on the rates that providers should receive for publicly funded places; debate continues over the contribution of the individual vs. the state; and the difficult economic climate sees the gap between those who have means and those who have little means, continue to grow. Alongside this is the promotion of control and choice for service users via Self Directed Support. This is a hugely positive step towards the personalisation of care in Scotland, and is yet another factor that those responsible for designing, commissioning, purchasing and delivering care need to take into account.
All of this points to the need to consider the future role and function of the care homes market in Scotland.
Contact
Email: George Whitton