The Evaluation of the Family Nurse Partnership Programme in Scotland: Phase 1 Report – Intake and Early Pregnancy
The Family Nurse Partnershhip (FNP) is a preventative programme for first time teenage mothers and their babies. FNP is being tested in Scotland for the first time. This is the first interim evaluation report and focuses on the intake and early pregnancy phases of the programmes implementation.
4 ENGAGING AND ENROLLING CLIENTS
4.1 Introduction
This chapter presents information about the recruitment phase of the first Scottish FNP test site in Edinburgh - the nine months of the programme from late January to late October 2010 during which clients were identified, engaged and enrolled with the programme. For individual clients, recruitment to FNP involves several stages. First, potentially eligible clients need to be identified. Next, once their eligibility is confirmed, Family Nurses engage with clients to introduce and explain the programme, and to support them in making a decision about whether or not they wish to participate in FNP. Finally, after this initial engagement clients make a decision on whether or not to opt-in and actually enrol with the programme.
The first section of the chapter (4.2) focuses on analyses of the monitoring data collected by the FNP team, including data about clients' characteristics at enrolment and the extent to which programme fidelity with respect to enrolment was achieved.
The following section (4.3) explores views and experiences of the engagement and enrolment processes from the perspectives of clients and the delivery team, including the Family Nurses, the Supervisor and local FNP Lead in NHS Lothian. The data for clients and the delivery team are drawn from in-depth qualitative interviews. As such, they include the respondents' perceptions of the engagement and enrolment processes. This means that their accounts reflect their experiences and interpretations of events and situations - different respondents' accounts may not always accord with each other, or with what is formally meant to happen. These accounts provide a window on the programme and allow insights into the process of engaging and enrolling clients from the perspectives of those most closely involved in delivering or receiving the programme.
4.2 Monitoring data relating to the recruitment phase
4.2.1 Core Model Elements and fidelity 'stretch' goalsThe FNP is designed to be offered to vulnerable first-time mothers-to-be. The USA National Service Office has determined, based on the USA research evidence and on ongoing USA practice, that maximum impact can be obtained if clients are enrolled early in their pregnancy. To be acceptable, particularly in the British context where there are universal services for all expectant mothers, children and families, it is important that most of those who are offered the service, after being deemed suitable, actually take up the offer. The USA team has also determined the most efficient case-load for a nurse working on this programme. The Core Model Elements for FNP specify a number of requirements relating to client engagement and enrolment, as follows:
- Enrolment and participation in FNP is voluntary
- Eligible clients are first-time mothers only
- Eligible clients include high risk mothers only (during the testing phase, only mothers 19 years and under were eligible - as described above (section 2.4), this specific eligibility criteria was not part of the Core Model Elements, but was agreed with the National Unit at the Department of Health (England), based on the research evidence)
- At least 60% of clients are enrolled by 16 weeks gestation or earlier and 100% no later than 28 weeks
- Each client enrolled is visited by the same Family Nurse throughout her pregnancy and the first 2 years of her child's life.
There are also fidelity 'stretch' goals to:
- enrol 25 families per nurse within 9 months of recruitment commencing, and
- to enrol 75% of eligible clients who are offered the programme.
In addition, the Core Model Elements specify that each full-time Family Nurse should have a caseload of no more than 25 families, and that the Supervisor should have a small caseload of 2 or 3 families.
4.2.2 Identifying eligible clientsEligible women were identified using a NHS Lothian database "Maternity Trak", which records information about all pregnancies to women in Lothian as soon as they become known to the health service. This meant that there was a group of potentially eligible women, who could be offered a Family Nurse very quickly at the start of the recruitment phase, without necessarily having to rely on other health professionals with whom the potential client may have contact. This approach differs from that used in England, where FNP projects were reliant on referrals from other professionals (primarily midwives and GPs).
In total, 396 potentially eligible women were identified using the Maternity Trak system between 25 th January 2010 and the end of October 2010. Of these, 144 women did not - in the end - meet the eligibility criteria, primarily because they had experienced pregnancy loss (miscarriage and termination) after their name was included on the Maternity Trak database, or because they had already had one or more child. In addition, the Family Nurses were unable to contact 13 potential clients, while 26 clients who had been identified as potentially eligible were not in the end offered the programme, because all caseloads were at a maximum (and the recruitment phase was therefore ended). In one case, a potentially eligible client was not offered the programme because her estimated delivery data placed her delivery in a month where all nurses already had 4 clients with due dates.
Of the 185 eligible clients who were offered the programme, just 37 eligible women declined to be part of the programme, giving an acceptance rate of 80% - comfortably above the fidelity 'stretch' goal of 75%. The main reason given for refusal was that the woman already had enough support from friends and family (n = 21). Other reasons given were that they did not want the programme (n = 7) or, for a very small number (n = 2), that they were too busy working full-time. A further seven women gave no reason for declining. The final enrolled number of clients was 148 (See Appendix A for enrolment diagram).
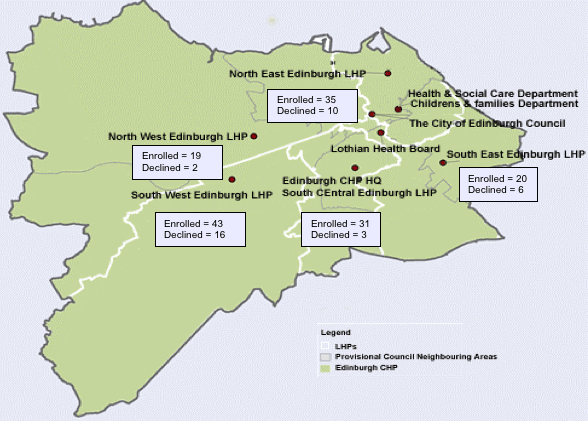
Enrolment varied by area (see Figure 3-A), with South Central and North West Edinburgh having the highest acceptance rates (91% and 90% respectively), and South West Edinburgh having the lowest (73%).
Figure 3-A Enrolment and refusals across Edinburgh CHP
The suggested target for enrolment was 17 women per month. As Figure 3-B shows, 32 women (22% of all clients) were enrolled within the first full month of the recruitment phase. May and September 2010 also saw high rates of enrolment, though both were followed by months of lower enrolment.
Figure 3-B Number of clients enrolled per month (25 th Jan - Oct 2010)
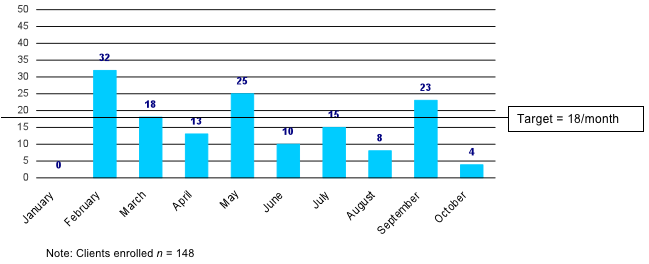
Note: Clients enrolled n = 148
In line with the Core Model Elements, all clients were enrolled by 28 weeks of pregnancy and all were first-time mothers. Almost a third (48 women, 32%) were enrolled by 16 weeks gestation. However, this fell short of the 60% specified in the Core Model Elements and was lower than the figure of 51% achieved for the first 10 pilot sites in England (Barnes et al, 2008).
The short-fall in the number enrolled prior to 16 weeks of pregnancy appears to reflect several issues. First, the programme was offered to all eligible clients who became known to the delivery team - there was no 'cherry picking' of clients under 16 weeks. This decision was in part driven by the need to recruit sufficient numbers within 9 months, but it also reflected a commitment to providing an equitable service and not excluding any women who were eligible to participate. A second, related challenge was associated with the decision taken early in the implementation of FNP in Edinburgh to try and recruit as many eligible women recorded on Maternity Trak at the start of the recruitment phase as possible, rather than simply offering the programme to those who became known to the team at that date. This decision was taken because of concern that the number of women eligible for FNP in Edinburgh over the nine-month recruitment phase might in fact be lower than initially anticipated, because of challenges around estimating numbers of first births to mothers under 20. 6 As the Maternity Trak database included those already at a later stage in pregnancy as at 25 th January, this meant that early on more clients were enrolled further into their pregnancies. Analysis of the monitoring data confirms that average gestation of clients enrolled in February was 130 days (18.5 weeks) and in March was 143 days (20.4 weeks), in contrast to 121 days (17.2 weeks) in April and 118 days (16.8 weeks) in May (there was also a peak in gestation in August due to Nurse holidays in the month before). There were also some inaccuracies in Maternity Trak data (resulting from, for example, pregnancies being more advanced than the client initially thought at their booking in appointment, rather than reflecting any errors in data entry), which again affected the point in the pregnancy at which clients were enrolled. Finally, an additional factor which may have impacted the ease of enrolling women prior to their 16 th week of gestation was the time involved in engaging with clients and introducing the programme to them prior to enrolment. Family Nurses reported that engaging with clients, explaining the programme to them, and ensuring they were able to make an informed decision about whether to not to enrol could take some weeks, particularly where the potential client was unsure about either participating in FNP or about continuing with their pregnancy (see more detailed discussion in Sections 4.3.2 and 4.3.3, below). The need to allow clients to decide in their own time whether or not to enrol was thus viewed as another challenge to recruiting 60% of clients prior to 16 weeks gestation.
Further analysis of the monitoring data showed that 60% of clients were enrolled by 18 weeks and 3 days, which should allow sufficient time to deliver the full programme content for the pregnancy phase before the birth of the baby.
4.2.3 The demographic profile of enrolled clientsThe mean age of clients at conception (based on the date of their last menstrual period) was 17.4 years. The mean age of clients at enrolment was 18.3 years (range 14 - 20 years 7).
Ethnic identity of the enrolled clients was overwhelmingly White (93% were classed a "White British" with a further 3.5% classed as "White Other"). Less than 1 in 20 (3.5%) had a different ethnic background - this is very closely in line with the known ethnic profile for Scotland as a whole (Scottish Government, 2010). The vast majority of clients spoke English as their primary language, with other languages spoken being Arabic and Eastern European languages.
Almost nine in 10 of the clients (88%) had left school, with an average school leaving age of 15 years 10 months (range 14 - 17 years old). The year of leaving school ranged from S3 to S6. Four in five (80%) of the enrolled clients had achieved at least one Standard Grade or equivalent, with over half (57%) achieving five or more Standard Grades. In addition, more than a quarter (29%) of clients had achieved a Grade '2' or above in at least one examination. 8 Clients were, therefore, relatively heterogeneous in terms of their educational attainment at the point of enrolment.
The majority of respondents currently had a partner (79%), although this was not necessarily the biological father of their baby Thirty-five per cent of clients were married, cohabiting or in a civil partnership. Eighty-one percent of respondents said that their current partner 9, husband, or ex-husband was the baby's biological father 10.
4.3 Clients' and the delivery team's experiences of the recruitment phase
4.3.1 Finding out about FNPAs described above, in the England FNP sites, potentially eligible clients are primarily identified by midwives at the booking-in visit, with a Booking Consent Form used to indicate their willingness to meet with a Family Nurse. In Edinburgh, the Maternity Trak database offered a more direct route to engaging clients, which would not necessarily involve midwives.
Clients were asked how they had first heard about the programme. Two routes were mentioned: either through their midwife, who asked if they would like to be "transferred" to the programme and to have their names passed to the Family Nurses, or they were contacted directly by a Family Nurse, either by telephone or a visit. Where the midwife had been the initial source, clients reported that they were given limited information by the midwife about the programme (in line with the agreed protocols) 11.
However clients first heard about the FNP, they all reported that the Family Nurse arranged an appointment to meet with them at home or work to explain the programme. Clients reported that there was a time lag of between 2 and 12 weeks between finding out they were pregnant and first hearing from their Family Nurse, in which time all of the young women in our qualitative panel had seen either their GP or a midwife.
At their first meeting with a Family Nurse, clients said that they were provided with a general explanation of the FNP and what a Family Nurse might do: they recalled being told that they would get help throughout pregnancy and up to when their child was aged two, and that the programme would be similar to having a Health Visitor, but that the Family Nurse would visit more regularly and they would talk about different things. All clients in the panel felt that they had enough information at this first meeting to enable them to make a decision - there was nothing else they would have liked to have known at that stage:
I thought that she told me everything like. I think I was quite aware o' what it was going to be. Like the first day, she told me loads.
[Pregnancy Interview, Client 13]
Whatever stage of pregnancy they were at when they first heard about FNP, clients appeared to feel that this had been the right time for them. Finding out early in the pregnancy was felt to be helpful because the pregnancy hadn't "sunk in" yet, so it was good to have the Family Nurse there to explain each stage of the pregnancy. Finding out early was also viewed as giving the Family Nurse and client time to build up a relationship during the pregnancy. Those clients who had been enrolled early in their pregnancy felt that it might have been difficult or - as one client expressed it "quite weird" - to meet the Family Nurse at a later point. However, clients who had met their Family Nurse slightly later on in their pregnancy were equally likely to think this was the right time for them, either because it gave them time to settle into their pregnancy first or because, at that later point of the pregnancy, it was seen as a good time to start talking to someone outwith the family.
4.3.2 The engagement processFamily Nurses were understandably anxious about their initial engagement with clients and were anxious that clients would not want to enrol with the programme. In reality, however, the Family Nurses had a very different experience and found that vast majority of the clients they approached decided to take part in the programme, even if the process of engagement was lengthy for some clients. Among the clients in the evaluation's qualitative panel, the amount of time taken to decide whether to accept the programme ranged from an immediate decision to a longer process of hours, days or even weeks to think things through. The decision to sign up was made either alone or in consultation with a parent, partner or midwife.
Family Nurses reported that while some clients were immediately enthusiastic about the programme and signed-up without any hesitations, others - and particularly the more vulnerable young women (for example, those who were in precarious relationships or used drugs) - needed more time. Family Nurses described how they had to 'tread carefully' during their initial engagement with these clients in order to build up a degree of trust. In addition to providing clients with as much information as possible about the programme, the Nurses also talked with clients' families - particularly their mothers and in some cases partners - and provided them with information. Nurses described the importance of taking time to include the mother or partner in the engagement process to answer any questions they may have had. It was suggested that that this helped develop a level of trust and acceptance of the programme among families.
The Family Nurses reported that, in those cases where potential clients did not wish to proceed with the programme, they invariably thanked the Family Nurses for offering it to them. As discussed above, when eligible women declined the programme, a range of reasons were provided. Family Nurses reported that in some instances, the young women who had declined FNP felt that they had enough support structures around them in the form of partners, family and friends or were - as the Family Nurses described them - 'high resource'. These young women may be in full-time employment and were in committed relationships.
In the small number of cases to date where clients withdrew from the programme after enrolling (by the end of October 2010, 2 clients had dropped out during their pregnancy and 2 after giving birth - see Appendix A), reasons cited by the Nurses included clients who felt that the programme was "not for them" or they were young women who did not want any professional involvement. In other cases, clients simply moved out of Edinburgh and could no longer be involved with the programme.
4.3.3 Deciding to sign up to FNPClients were asked about their reasons for enrolling with the programme. On the one hand, there were clients who simply thought the programme "sounded good", that FNP was the best option or that there was no point in saying 'no'. On the other hand, there were clients who provided more clearly defined reasons for enrolling: that it would be good to get practical and emotional support and, in particular, to have someone to talk to who was outside their family and who would keep anything they discussed confidential:
… it's, ken, confidential and that, and just somebody away from the family tae talk tae and just if you needed any information she was always there. I'd just phone her or she was just always there every time I need her.
[Pregnancy interview, Client 11]
A key reason for signing up to the FNP, however, was to obtain information from someone - the Family Nurse - who clients believed would be both informative and responsive. As one client said "I didn't have a clue about anything" [Client 9, Pregnancy Interview]. There was a perception among clients that Family Nurses would be able to provided balanced information which would help clients to decide for themselves what was best for them and their baby. The timing of the programme was an additional reason for enrolling: clients signed up because they would be visited many times before as well as after the birth, whereas a health visitor's support would be more limited and may largely be confined to the post-natal period.
Clients expressed few major concerns about enrolling with the FNP, although there were some initial worries that the Family Nurse "sounded like a social worker" and that enrolling might lead to information being passed to other agencies. Further comments from clients (discussed in section 5.4 below) suggest that this may in part have reflected an underlying fear that their baby might be removed -a concern associated with their young and vulnerable status.
In terms of the topics and issues that might be addressed by the Nurses, clients expected their Family Nurse to provide information, advice and support about the physical aspects of pregnancy and childbirth, ante-natal care and ante-natal classes. There was also an expectation that the Nurse would provide advice and support after the baby was born, including information about their role as a parent - how to be a good mother (or father) and how to take care of a baby. Clients expected that they would gain confidence about being a mother through participating in the programme. More widely, clients hoped that their Family Nurse would have an impact on other aspects of their life, including - for example, providing help with college applications or employment after the birth. Their expectations were, therefore, consistent with what the programme is designed to deliver.
As discussed above, there were suggestions from FNP delivery team members that some potential clients appeared ambivalent about participating in the programme and that this uncertainty may have resulted in their taking longer to make a decision. It was suggested that before 16 weeks, a pregnant teenager may not yet know if she wants to continue her pregnancy and, additionally, may also be unsure or suspicious of the programme that is being offered.
They just haven't made up their mind. They don't know. It's the first time. They don't know what Health Visiting is. They don't know what FNP is. They're testing out the relationship [ ] Teenagers do that, don't they? So it's just teenage behaviour, but it is ... it's as a result of, you know, people always letting them down in life. So I think that maybe that bit of it you can't change either, so you can't make these girls any less ambivalent
[Family Nurse 7]
The critical factor, which Family Nurses and others reiterated, was that every potential client was given time to make their decision about enrolling or not - if necessary, the Family Nurse might revisit them on several occasions, giving the young women time to reflect, to find out more about the programme and to decide if they wished to have a Family Nurse. As indicated in Section 4.2, the net results of this engagement process was that there was a high acceptance rate, but with final enrolment happening beyond the 16 th week of pregnancy for a greater proportion of clients than required to meet this aspect of the Core Model Elements.
4.3.4 The recruitment scheduleIn the early stages of the programme, the Family Nurses felt themselves to be under pressure to enrol clients. It was suggested that this was not a pressure applied by the Supervisor, but was in part a self-imposed demand the Family Nurses placed on themselves. To some extent, this sense of pressure reflected Family Nurses' and others' acute awareness of the need to meet the Core Model Elements and the knowledge that there was a spotlight on their activities.
Nevertheless, there were suggestions that the recruitment phase of FNP could perhaps have been managed differently to ease the pressure on the Family Nurses in the early stages of the programme. The front-loading of engagement and enrolment, described above ( section 4.2), in combination with staff sickness leaving the team a nurse down in the first full month of recruitment, meant that the Family Nurses had rather larger caseloads than they might otherwise have had at an earlier stage in the implementation of the programme in Lothian. The requirement for more frequent visits to clients during the ante-natal period, the time involved in engaging with clients prior to enrolment, and the fact that the Family Nurses were new to the programme and were still attending training sessions all meant that this relatively large early caseload impacted on initial workloads, as well as on the number of clients enrolled before 16 weeks gestation. The Nurses suggested that in hindsight it might have been better to engage with and enrol a cluster of clients, deliver the programme materials to those early clients, consolidate their learning and then engage with and enrol another cluster of clients. There was acknowledgement that there was inevitably a learning phase however enrolment was staggered, but nevertheless there was a view that a somewhat slower pace might have eased the initial sense of pressure and stress that Nurses experienced.
…I think we recruited very, very quickly. That was difficult. I think had the recruitment time been slightly longer then that may not have felt quite so difficult. And it is starting to settle down now, the workload is easing slightly but just a little, but … I think were all beginning to see maybe the light at the end of the tunnel, that things may now start settling as all of our babies are born and things.
[Family Nurse 3]