Delivery of psychological therapies and interventions: national specification
We want to hear your views on the draft specification for psychological therapies and interventions. We have asked a series of questions, and your answers to these will help us refine the final specification and develop how we will measure if the specification is being met.
Overview
We want to hear your views on the draft specification for psychological therapies and interventions. We have asked a series of questions, and your answers to these will help us refine the final specification and develop how we will measure if the specification is being met.
What are psychological therapies and interventions?
Psychological therapies and interventions are evidence-based approaches (based on facts) that can improve your health by helping you make changes to your thinking, behaviour, and relationships to reduce distress, treat mental health difficulties, help manage emotions, and improve wellbeing.
Psychological therapies and interventions are delivered in a broad range of health, social care, and third sector settings in Scotland; across the age range and for a wide range of need. The range of settings where psychological care may be delivered can be found on Page 2.
Psychological therapies and Interventions are evidence-based techniques used to promote good psychological health, prevent psychological ill health, and provide mental health interventions.
Psychological care refers to all psychological therapies, assessments and interventions delivered through self-help, by individuals or specific psychological teams or services. This care can be delivered in person, in groups and remotely and / or digitally.
We want to make sure that there is a well-functioning psychological care system, which helps you to receive the right information, support, intervention or service appropriate for your needs.
You should be provided with care as quickly as possible if you need it, and with the fewest steps possible. The psychological care you receive will have your needs, and the evidence base at the centre of all decision making. This is to help you feel informed and have choice in your care and support.
We know that currently not everyone has the same experiences or outcomes when they engage with individuals, teams or services when receiving psychological care.
How is psychological care delivered?
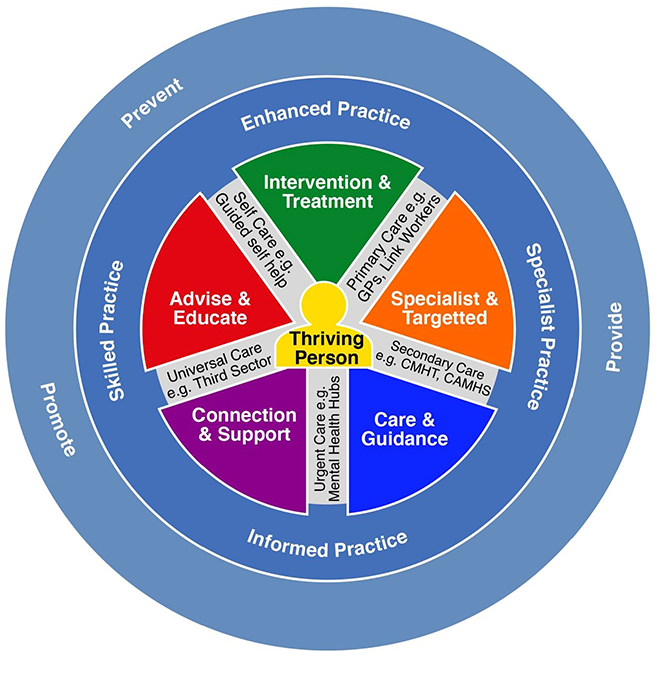
It can be helpful to consider psychological care in the workforce as practice types. A wide range of staff (e.g. Psychologists, Nurses, Allied Health Professionals, Psychotherapists, Doctors and Social Workers) may all deliver psychological care. In Scotland, these practice types are described as:
Informed Practice - this workforce will have knowledge and skills in recognising psychological issues (e.g., a support worker identifying distress through a trauma informed conversation with an in-patient who has cancer, and informing the ward nurse).
Skilled Practice - this workforce will have skills to deliver psychologically based education courses, and have skills in developing good communication and listening skills (e.g., a clinician providing support and education about anxiety and sleep in conversations with adults in a prison setting).
Enhanced Practice – this workforce will provide psychological assessment and treatments that have proven effectiveness as indicated in the Scottish Psychological Therapies Matrix (e.g., an occupational therapist delivering evidence based cognitive rehabilitation with someone in a social care setting).
Specialist Practice - this workforce will have formal training with expertise in at least one psychological therapy (e.g., delivery of trauma focussed Cognitive Behavioural Therapy for people who have Post-Traumatic Stress Disorder and depression by a Clinical Psychologist).
Professionals trained in specialist practice also contribute to wider public sector services through education, training, supervision, consultation, research, and evaluation. The four practice types above are of equal importance and go across sectors, disciplines, and professions.
Where is psychological care delivered?
- Adult Mental Health Services
- Child and Adolescent Mental Health Services
- Child and Young People
- Education Settings
- Care homes
- Clinical neuropsychology Services – acute and rehabilitation
- Community settings
- Crisis support
- Digital Therapies
- Early Intervention services to support whole population health
- Early Intervention for Psychosis
- Eating Disorders
- Forensic Mental Health Services
- Gender Identity
- GP Practices
- Infant Mental Health Services
- Justice settings
- Perinatal Mental Health Services
- Prisoner Health care
- Maternity and Neonatal Psychological Intervention Service
- In-patient services
- Intellectual Disabilities
- Neurodevelopmental
- Older Adults including dementia
- Paediatrics
- Physical Health
- Primary Care
- Rehabilitation, both physical and mental health
- Secure Care
- Social care
- Substance use
- Specialist trauma services
- Veterans
- Wellbeing and prevention
Context
Currently, there is no national specification for the delivery of psychological therapies and interventions in Scotland. People with lived experience of accessing psychological therapies and interventions and people who work and volunteer in services, have identified this as a barrier in the delivery of quality care and support. The development of this specification aims to address this gap.
Demand for psychological therapies and interventions in Scotland had been growing gradually before the coronavirus pandemic in 2020. The pandemic has increased the demand. The Mental Health Transition and Recovery Plan, published in October 2020, outlines the Scottish Government's response to the coronavirus pandemic. It addresses the challenges that the pandemic has had, and will continue to have, on the population's mental health and psychological wellbeing. It has a key aim of ensuring safe, effective treatment and care of people living with mental illness. It committed us to the development; implementation and assessment of the National Standards for Adult Secondary Care Mental Health Services and the Minister subsequently announced a commitment to develop a specification for Psychological therapies and interventions.
This specification has been published for consultation in the context of the development of the new Mental Health and Wellbeing Strategy for Scotland. The Strategy provides an opportunity to set out our aims for a high-functioning mental health and wellbeing system and the standards we expect services within that system to deliver. Measurement of the standards will provide indicators that can form part of our evaluation and monitoring of the Strategy and Delivery Plan.
We acknowledge that the work set out in this specification is ambitious and will take time to implement. We recognise that it must compliment other ongoing and interlinking work, such as the creation of the National Care Service (NCS) and the findings from the recently published Mental Health Law Review.
For more information on how the specification fits within the wider landscape of principles, standards and frameworks which impact health and care and mental health services, please see Annex A.
Aims
We want to support the delivery of high-quality psychological therapies and interventions, which enable people to receive the right information, support, care, intervention, or service for their needs, as quickly as possible, with the fewest steps possible.
The aims of the specification are as follows:
- To let individuals, their families and carers know what they can expect when accessing psychological therapies and interventions from preventing poor psychological health through self-help, to care provide by professionals and psychological care services.
- To ensure that person-centred and trauma-informed approaches are embedded within therapies, interventions, and care services.
- To improve experiences and outcomes for people who access psychological therapies and interventions.
- Ensure a consistent, high-quality range of therapies, interventions, and psychological care services are provided to everyone who needs them.
- To be able to measure the quality of services, in line with the specification in order to support improvement.
It will also make it easier for good practice to be shared and for any issues to be identified and addressed, therefore driving improvement in services. This specification is designed to encourage transformational, innovative, high-quality accessible psychological care for you and others.
Process
Throughout the development of this specification, we engaged extensively with people who use psychological care services and mental health services, the psychologically trained workforce and organisations who deliver psychological care. You can find copies of reports on this engagement alongside this consultation.
We worked with the Mental Health and Wellbeing Standards Working Group, which was made up of people from each of these groups and chaired by someone with lived experience. We have also reported regularly to the Mental Health Quality and Safety Board, which is chaired by the Minister for Mental Health and Wellbeing.
Structure of the Specification
The specification is structured around overarching principles, which people with lived experience of accessing psychological therapies and interventions and the workforce were consulted on. The principles are:
- High-quality care and support that is right for me
- I am fully involved in decisions about my care
- High-quality interventions and treatment that are right for me
- My rights are acknowledged, respected, and delivered
- I am fully involved in planning and agreeing my transitions
- We fully involve people, their families, and their carers
- I have confidence in the staff that support me
Each section describes what a person can expect when accessing psychological interventions and therapies and describes how services should be led, managed, designed, and delivered.
Access and Equalities
A key priority in developing the specification has been addressing the inequalities in outcomes and experiences for people accessing psychological therapies and interventions. We know that access to, and experience of psychological care and support is not experienced equally across the population.
We want the specification to support equitable access to psychological care and support, as well as equity in the experiences and outcomes of people using psychological care services. This is a key focus of our consultation on the specification.
We acknowledge that as we continue to shape the specification, there is more we need to do in terms of listening to and learning from people and member-led organisations. In addition, we have undertaken an Equalities Impact Assessment (EQIA) and are using the findings from this to inform our engagement.
Groups of people who experience such inequalities include those with protected characteristics such as sex, gender reassignment, sexual orientation, race and ethnicity, and disability. Often these are the same groups in the population that are systematically disadvantaged in many different aspects of their lives. We also know that some people with neurodivergent differences will experience a higher risk of poorer physical health and mental health and difficulty accessing the right support.
In addition, individuals living in the most deprived areas report higher levels of common physical health, mental health problems and mental ill health (including suicidal behaviour), with lower levels of wellbeing than those living in the most affluent areas. People can also experience disadvantage due to adverse childhood events such as being a victim of abuse, poor housing, traumatic events, and poor working conditions. These groups have poorer health and mental health than others and face greater barriers in getting help.
We also know that people with severe and enduring mental illness are themselves more likely to experience poverty, homelessness, incarceration, social isolation and unemployment. They are also at greater risk of poor physical health and reduced life expectancy.
Therefore, it is important that inequality is not only considered in terms of single characteristics or experiences. In reality, people's lives are multi-dimensional and complex. We all have distinct experiences of inequality that need to be understood. This is known as "intersectionality". Whilst we do not have a complete understanding of intersectional inequalities for mental health, we know we need to do more to understand and improve experiences for people across Scotland.
Measurement
A key aim of the specification is to be measurable and to provide assurance that services are delivering for the people that use them. Making the specification measurable will allow us to understand how it is being implemented and whether they are being met. It will also make it easier for good practice to be shared and for any issues to be identified and addressed, therefore driving improvement in services.
Throughout 2022 and 2023, we will work with partners to ensure that we can measure progress against the new specification, developing a validated assessment tool and a set of indicators. We will carry out this work in co-ordination with the development of the Adult Secondary Mental Health Services Standards, Mental Health Strategy and the National Care Service. This will ensure that our approach to data and measurement across mental health is joined up, making best use of the data we already collect and minimising the burden on services.
How you can help us? / Our next steps
In this consultation, we have asked a number of questions about the specification. You can find a copy of the draft specification in its entirety on pages 10 to 19 of the PDF.
Some questions asked will be of more interest to some people than others will. For example, some questions might feel most relevant to people who have experiences of physical issues or mental health issues, while some questions might be of particular interest to people who provide care and support for those with physical health conditions or poor mental wellbeing and mental health conditions.
Part One of the consultation asks questions about the specification overall.
If you have less time to complete the consultation, you may wish to focus on Part One. This contains six questions which will allow you to feedback on the specification overall. This part of the consultation may be of the most interest to people who have experience of accessing psychological therapies using services.
Part Two of the consultation asks more detailed questions on each theme and may take more time to complete.
Part Three contains more detailed and technical questions seeking initial views on how we support services to implement the specification and our plans to measure the specification. While we welcome everyone's views across the whole consultation, this part of the consultation may be of most interest to people with experience of working in or running services.
Whether you answer all of the questions, or only some, your views will be carefully considered by the Scottish Government when writing the final specification.
We will publish a summary of all of the responses to show what people have said. The final specification will be published in 2023.
Mental health and wellbeing support
We want to hear about people's experiences of health and care and mental health and wellbeing, and any support they have received. However, we know that sometimes it can be difficult to talk or write about these experiences, whether they are your own or other people's.
You can respond to any questions in the consultation that you want to. There is no need to respond to them all.
If you are affected by any of the issues covered in this document and need support, help is available.
We have included links to some of those sources of support below:
Breathing Space is Scotland's mental health helpline for individuals experiencing symptoms of low mood, depression, or anxiety, and offers free and confidential advice for individuals over the age of 16. They can be contacted on 0800 83 85 87, 6pm to 2am Monday to Thursday; and from 6pm Friday throughout the weekend to 6am Monday or by visiting their website on https://breathingspace.scot/.
Samaritans provide confidential non-judgemental emotional support 24 hours a day for people who are experiencing feelings of distress or despair. You can contact Samaritans free by phoning 116 123 or via email on jo@samaritans.org
Telephone advice and support on healthcare can be obtained from the NHS24 Mental Health Hub by phoning 111. The Mental Health Hub is open 24/7.
If you're feeling anxious, stressed, or low, or having problems sleeping or dealing with grief - find out how you can improve your mental wellbeing by hearing what others have found helpful by visiting https://www.nhsinform.scot/mind-to-mind
The National Wellbeing Hub helps support the wellbeing of everyone working in Health and Social Care in Scotland. Visit https://wellbeinghub.scot/ to learn more, or call the National Wellbeing Helpline. This compassionate listening service is available 24/7 and is for everyone working in health and social care services in Scotland. You can call on 0800 111 4191.
Contact
Email: ptspecification@gov.scot