Substance misuse services: delivery of psychological interventions
Strategy aimed at increasing access to support for people working to recover from problematic alcohol and drug use.
3. Which interventions should be delivered, and by whom?
Principles of psychological intervention delivery
All psychological interventions should be delivered as part of a recovery care plan, integrating the most appropriate psychological, social, medical and other non-medical interventions for an individual in recovery. Interventions should be based on a comprehensive assessment of need.
The choice of psychological intervention should be based on a formulation of an individual’s difficulties. Psychological formulation is a way of understanding a person’s, couple’s or family’s difficulties; it is developed in collaboration with them, links theory with practice, and provides a roadmap for intervention.
All delivery should be carried out within a clear structure of managerial and clinical supervision to ensure effective delivery and governance. Psychological interventions are delivered via a complex interpersonal interaction. Supervision specifically designed to support delivery is essential at each tier to ensure the safety and integrity of interventions for both service users and practitioners.
Peer support and access to the recovery community should be available at every tier, along with the potential for family and network interventions.
Most interventions will be delivered face to face, but some may be accessed by telephone or via the Internet, particularly in remote areas or as part of ongoing work. Care should be delivered in accordance with the Scottish Government’s Quality Principles. [7]
A matched-care model of delivery is presented in Figure 1. This is based on the Psychological Therapies Matrix, [8] which outlines evidence-based psychological interventions for alcohol problems and substance misuse in Scotland. This model offers ‘tiers’ of care: each step up leads to more intensive interventions for service users with more complex needs, requiring additional competencies, training and supervision structures for providers. Staff with additional training and competencies can provide consultation and liaison to support early recognition and treatment of needs requiring higher-tier interventions.
Treatment may also be understood to move in ‘phases’ of care, recognising that different interventions may be more appropriate at different times in a service user’s treatment journey. Interventions at all times should be based on assessment and review of service users’ changing needs and motivations throughout the recovery journey.
Figure 1: A matched-care model of delivery of psychological interventions ( PI) in substance misuse ( SM) services
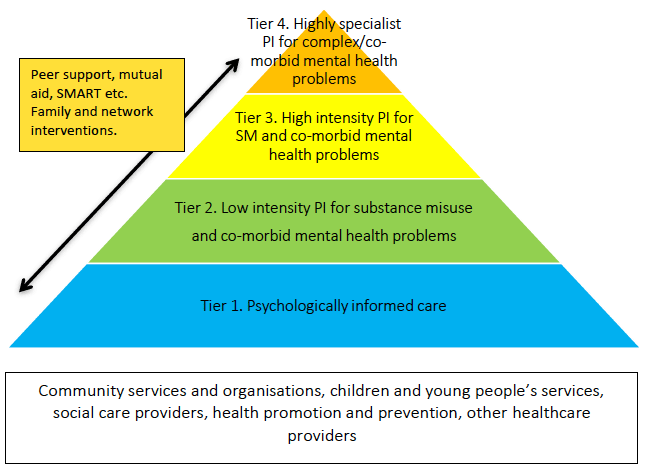
The model in Figure 1 proposes that the foundation for all service delivery in a substance misuse service should be psychologically informed care provided by all clinical and care staff. This guide takes a broad definition of ‘psychologically informed care’ to support adaptation to the range of service settings across Scotland, but is based on the understanding that substance treatment services will be embedded within a recovery-oriented system of care. This should be seen as being complementary to the recommendations that treatments in substance misuse services should also be psychologically informed [9] and trauma-informed. [10]
The competencies required to deliver psychological interventions are outlined further in this section. They build on those described in Supporting the development of Scotland’s drug and alcohol workforce, [11] specifically the learning priorities at levels 2–4, and outline the knowledge and skills required to deliver effective and evidence-based psychological interventions in substance misuse services.
As outlined in the UK guidelines on clinical management of drug misuse and dependence [12] and the Psychological Therapies Matrix, [13] the choice of psychological and psychosocial interventions should depend on their suitability, effectiveness (from the evidence base), appropriateness and acceptability to the individual or group, availability of trained staff and cultural appropriateness. Some approaches and interventions, such as counselling, psychotherapy and therapeutic community approaches, have not been included in the guide as they would not be classified as specific psychological interventions, according to the definition outlined below.
Psychological interventions are delivered by trained practitioners from a wide range of professions, such as nursing, social care, psychology, counselling and psychotherapy, and in various settings, including outpatient, hospital-based and therapeutic communities. It is important to differentiate between the intervention (what work is being delivered), the practitioner (who is delivering it and his or her training background), and the situation (the setting and context).
Evidence-based psychological interventions reflect research that specifically defines the work done in partnership with a service user based on the principles of research methodology. They are operationally defined, often through the use of manuals, worksheets, exercises, protocols, formulation and/or guidelines, which allows the delivery of the specific intervention to be observed and its integrity monitored and progress tracked. Research clearly demonstrates that the therapeutic relationship is essential to the effectiveness of these interventions, with counselling skills establishing the foundation from which evidence-based interventions are delivered. Research also emphasises, however, the importance of defining clearly the intervention being delivered within this therapeutic relationship for effective change to occur.
All staff delivering psychological interventions at every tier should receive regular skills-based supervision and have access to psychological advice when required. While all references have not been included in this section, the interventions presented are drawn from the evidence base for psychological interventions in substance use disorders and co-morbid mental health difficulties. Evidence tables for the delivery of psychological interventions for mental health disorders are available from the Psychological Therapies Matrix, the Scottish Intercollegiate Guidelines Network ( SIGN), and the National Institute for Health and Care Excellence ( NICE).
The model sits on a foundation of community services and organisations that support the pathways into and out of specialist care – social care and voluntary organisations, for example. It should also be seen within the context of wider social and healthcare provision due to shared agendas around, for example, children’s and young people’s care, physical health care and perinatal care.
The model should be understood as being embedded within a recovery-oriented system of care that is trauma-informed, with a commitment to peer recovery support services, access to holistic care, and clear routes for communication between treatment services and the recovery community. Where areas have an established recovery community, this may act as a bridge into services and support those exiting services to reintegrate into the community. This may include organisations and groups such as 12-step fellowships, recovery groups, peer supporters, SMART groups and recovery cafes.
The different tiers of the model are defined below, along with interventions recommended at each tier.
Tier 1. Psychologically informed care
Psychologically informed care uses principles of therapeutic engagement alongside a range of psychological approaches to support service users on their recovery journey. It is key for supporting a service user’s engagement and responsive care planning and is the foundation on which the matched-care model rests. A number of clinical tools, such as self-help materials, node-link maps, websites and apps, may be used to enhance interventions at this tier, which should be available across all teams in a substance misuse service, including integrated, non-statutory and social care partners.
Psychologically informed care should be woven into the fabric of addictions services. All clinical staff in the service should therefore have competencies in these areas to maximise the effectiveness of interventions (both psychological and pharmacological) the service provides. Most staff delivering at this tier are likely to be substance misuse keyworkers and may be supported by treatment protocols and node-link mapping tools. In many services, keyworking is understood as the role that drives and supports service users’ treatment journeys at every tier of the model and at every phase of the journey.
Cross-cutting skills, including crisis and risk management, multi-agency working and liaison with other agencies, and support to access the recovery community and peer support and/or mutual aid, are required at every phase of treatment.
Table 1 is adapted from the Skills Hub developed by the Skills Consortium and supported by the National Treatment Agency for England and Wales. [14]
Table 1. Knowledge and skills required by all staff in substance misuse services
| Phase of treatment |
Knowledge and skills required |
Cross-cutting knowledge and skills |
|
|---|---|---|---|
| Attending to the therapeutic relationship: empathic, collaborative, reflective conversations to guide change |
Engagement Preparation Change Completion Reintegration |
Comprehensive assessment, including:
Building a therapeutic relationship:
Recovery planning:
Reintegration:
|
Psychosocial techniques, supported by clinical tools and resources: Motivational Interviewing techniques, self-monitoring, activity scheduling, relaxation training, mapping techniques Trauma-informed care: trauma awareness, handling disclosure, emotional containment and self-awareness |
Case example: Joanne (1)
Joanne has a 15-year history of polysubstance misuse, including intravenous heroin use for two years. She has a daughter who is currently in the care of her mother.
Joanne attends a third sector needle-exchange drop-in and gets talking to the addiction worker on duty. She wants things to be different, and the worker suggests that she attends an assessment clinic later that week (Tier 1: use of Motivational Interviewing to spot motivational hooks, create non-judgemental therapeutic relationship and offer information, alongside harm reduction).
She attends the assessment clinic and says she feels like she is in chaos. She is using daily, and reports that she sometimes harms herself. She is ambivalent, defensive and a little argumentative in the assessment, but the worker responds empathically and agrees with her that her current situation is hard to tolerate (Tier 1: building discrepancy, handling disclosure, managing resistance).
This de-escalates the situation, and Joanne discloses parts of a traumatic history (Tier 1: trauma awareness, managing disclosure). The worker helps Joanne begin to think about next steps and she chooses to be referred to the local drug and alcohol treatment service to titrate onto methadone.
Tier 2. Low intensity psychological interventions for substance misuse and co-morbid mental health problems
Low intensity psychological interventions are aimed at mild-to-moderate addiction difficulties, and mild-to-moderate co-morbid mental health problems. They are delivered by a range of multidisciplinary practitioners trained in specific structured interventions.
Low intensity psychological interventions require additional competencies. [15] They are designed to be delivered alongside medical and pharmacological approaches by selected clinical staff to selected service users to enhance progress.
Staff delivering interventions at this tier will be from a number of professional backgrounds, but will have developed appropriate competencies to deliver low intensity interventions safely and effectively. They are delivered within protected time and to protocols, often based on a cognitive behavioural approach, and can be accessed through 1:1 or group interventions.
Frontline practitioners are likely to use psychological and social techniques and tools (such as motivational techniques, relaxation training, alcohol/drug diaries and self-help materials) as part of their practice within a psychologically minded approach. These techniques do not constitute a psychological intervention, but are invaluable components of routine care.
Practitioners delivering low intensity psychological interventions should have protected time in which to deliver care and attend supervision. This will help to ensure the intervention is delivered as it should be and reduce the likelihood of therapy drift in the face of ongoing emerging difficulties with this complex client group.
A number of low intensity interventions are recommended to address alcohol and drug use: [16]
- Motivational Interviewing ( MI) for drug and alcohol misuse
- Contingency Management for drug misuse
- cognitive behavioural skills-based interventions to enhance coping skills and prevent relapse.
- Community Reinforcement Approach
- Social Behaviour and Network Therapy.
Case example: Joanne (2)
Joanne enters the titration clinic of the treatment service and attends two appointments a week while her dose titrates up. During these appointments, she has access to a peer support service (cross cutting: peer support and recovery community access, building hope and motivation) and agrees to attend Narcotics Anonymous with a peer (cross cutting: access to mutual aid). She also accesses a number of health checks, including for blood-borne viruses and sexual health, and begins to stabilise her use.
She is interested to hear that there are incentives for attending all appointments and begins to work towards clinical privileges, such as take-home doses (Tier 1: harm reduction, health monitoring; Tier 2: contingency management).
Low intensity psychological interventions for common mental health problems such as anxiety and depression are outlined in the Psychological Therapies Matrix and may include interventions such as Cognitive Behavioural Therapy ( CBT)-based guided self-help. They may include:
- behavioural activation
- computerised CBT
- guided self-help
- trauma-informed psychoeducation around developing safety and stability for difficulties relating to complex trauma.
Case example: Joanne (3)
Joanne is allocated to a mental health nurse for ongoing keyworking due to her poor mental health . As her use stabilises, she begins to feel emotionally overwhelmed and her self-harm increases. She discloses this to her keyworker, who normalises her distress and supports her to develop a safety plan, following a protocol to do so over six sessions (Tier 1: trauma awareness, emotional containment, psychoeducation; Tier 2: CBT techniques to support safety and stabilisation, emotion regulation).
With Joanne’s consent, the keyworker seeks consultation with the team psychologist, and they develop a joint formulation of Joanne’s difficulties (Tier 4: formulation of complexity, support with treatment planning). The keyworker shares this with Joanne, and she chooses to attend the next Survive and Thrive course – an educational course for survivors of trauma that is run by the psychologist and a nurse therapist.
Joanne is unsure, but speaks to the peer supporter involved with the group and decides to go (Tier 1: building supportive social network; Tier 2: safety and stabilisation educational course; cross cutting: peer support). She attends 8/10 sessions, and learns some strategies for coping with emotions and caring for herself more compassionately. She begins to use healthier strategies for coping, and her self-harm reduces .
Tier 3. High intensity psychological interventions for substance misuse and co-morbid mental health problems
High intensity interventions are aimed at moderate/severe addiction difficulties and co-morbid mental health problems. These are standardised psychological therapies delivered to protocol but may be adapted for specific groups. They are aimed at moderate-to-severe difficulties with significant complexity.
High intensity interventions require specific competencies, accreditation in the particular intervention, and supervision by an appropriately trained supervisor. They are delivered by applied psychologists and CBT therapists trained to certificate and diploma level. High intensity therapies may target mental health difficulties and addictive behaviour change as part of an integrated treatment approach and require protected therapy time.
A number of interventions are recommended for addressing substance misuse at this tier:
- Behavioural Couples Therapy for drug and alcohol misuse
- CBT for alcohol misuse and relapse prevention.
Case example: Joanne (4)
Throughout Joanne’s engagement with the group, her keyworker has supported her to build her recovery capital (Tier 1: building resources, maintaining change), access the recovery community and attend SMART meetings (cross cutting: engagement with mutual aid and recovery community), but she has continued to use heroin weekly. Her keyworker takes her case to the team MI coach for some support, which helps the keyworker use MI skills more consistently (cross cutting: MI; access to practice development).
Joanne realises that she doesn’t believe in her ability to stay drug-free long term and struggles with cravings (cross cutting: MI skills in building discrepancy, functional analysis, confidence in changing). She discusses this with her keyworker, and is offered a place at a local third sector mindfulness group, Life after Addiction, run in conjunction with peers (cross cutting: MI, peer support; Tier 1: building social networks; Tier 3: mindfulness-based relapse prevention).
The third sector organisation has links to college and employability courses, and Joanne begins to make future plans (Tier 1: community reintegration, building recovery capital). She connects with peers she meets through the course and uses the skills she has learned and the confidence she has gained to stop her illicit use completely. Contact with the course offers opportunities around training and mentoring, and Joanne begins volunteering.
High intensity interventions for mental health problems are outlined in the Psychological Therapies Matrix and may include a range of interventions for specific mental health problems.
Much current evidence focuses on single diagnosis studies, rather than including people with complex co-morbidities, which can present a challenge for planning interventions for people with co-occurring mental health and substance misuse problems. An evidence base for interventions designed for co-morbid difficulties is nevertheless emerging: computerised CBT with MI, for example, is recommended for co-morbid depression and alcohol or cannabis misuse. Integrated models of treatment addressing co-occurring needs are recommended, rather than sequential treatments.
Tier 4. Highly specialist psychological interventions for complex/co-morbid mental health problems
Highly specialist interventions for complex and enduring problems are individually tailored interventions based on case formulations drawn from a range of psychological models and identifying the combination of interventions most appropriate for an individual’s needs.
They are most frequently delivered by clinical and counselling psychologists where there is a need to modify standardised approaches or devise a novel approach for a specific presentation. All applied psychologists are trained in at least two models of psychological intervention and should be aware of, and able to draw from, additional therapeutic models.
Tier 4 interventions are designed for service users experiencing severe, complex and co-morbid mental health problems. In substance misuse services, these problems commonly relate to personality disorders (particularly emotionally unstable personality disorders) and the consequences of complex trauma. Interventions are frequently delivered in collaboration with other members of the multidisciplinary team.
Contact
Alcohol and Drug Delivery team: Alcohol_and_Drug_partnerships@gov.scot