COVID-19 mRNA Vaccine BNT162b2 Pfizer/BioNTech Vaccine National Protocol
This protocol is for the supply and administration of COVID-19 mRNA Vaccine BNT162b2 Pfizer/BioNTech to individuals in accordance with the national COVID-19 vaccination programme.
Annex A: Clinical Information
This Annex provides information about the clinical situation or condition and treatment in relation to the National Protocol.
Annex Version history
Version: 1.0
Date: 21/01/21
Summary of changes: Version 1.0 new Annex A
Version: 2.0
Date: 02/02/21
Summary of changes: The following sections have been updated
- Exclusion section updated to align with wording in Green Book on previous systemic allergic reaction (including immediate-onset anaphylaxis and an additional exclusion for those patients with history of systemic reaction to biologics/monoclonals except on the advice an allergy specialist.
- Cautions section updated to include advice from Green Book on second doses following non allergic reactions or localised urticarial skin reactions without systemic symptoms following first dose.
- Form/strength section updated to reflect number of doses in a vial
- Route of administration section updated to align with wording in information for UK health professionals on number of doses in a vial.
- Frequency section updated to align with advice in Green Book on timing of second dose for those commencing immunosuppressive treatment.
- Observation following vaccination section updated with advice on post vaccine observation of second doses in those who had localised urticarial skin rashes (without systemic symptoms to the first dose.
Version: 2.1
Date: 22/02/21
Summary of changes: The following sections have been updated:
- Inclusion section updated to include women who are pregnant where the risk of exposure to SARS-CoV2 infection is high and cannot be avoided, or where the woman has underlying conditions that put them at very high risk of serious complications of COVID-19. And to remove statement not including pregnant women from clinically extremely vulnerable individuals
- Exclusion section updated to remove pregnancy and evolving neurological conditions
- Exclusion section updated to include prior allergic reaction to another mRNA vaccine and highlighting PEG specifically in the vaccine component.
- Exclusion section updated to include those patient characteristics which warrant special precautions as per the Green Book.
- Cautions section updated to include: Management of patients with a history of allergy and Flowchart for managing patients who have allergic reactions to the first dose of COVID-19 vaccine.
- Action if excluded section updated to remove reference to evolving neurological conditions.
- Frequency section updated to align with Green Book advice on scheduling of second dose.
1. Clinical condition or situation to which this Protocol applies
Category: Indication
Description: COVID-19 mRNA Vaccine BNT162b2 is indicated for active immunisation against COVID-19 disease caused by SARS-CoV-2 virus in accordance with Scottish Government COVID-19 immunisation programme and recommendations given in Chapter 14a of the Immunisation Against Infectious Disease: the 'Green Book', JCVI statement on priority groups for COVID-19 vaccination from 30th December 2020 and subsequent correspondence/publications from Scottish Government.
Category: Inclusion criteria
Description: National policy must be followed in relation to the priority groups eligible for vaccination at a particular point in time.
COVID-19 vaccine should be offered to the following individuals:
- Residents in a care home for older adults and their carers
- All those 80 years of age and over
- Frontline health and social care workers (as included in COVID-19 – SARS-Cov-2 chapter of Green Book, JCVI statement and Scottish Government CMO letters)
- All those 75 years of age and over
- All those 70 years of age and over
- Clinically extremely vulnerable (CEV) individuals (not including those under 16 years) as defined by Scottish Government at https://www.gov.scot/publications/covid-shielding/pages/highest-risk-classification/
- All those 65 years of age and over
- Individuals aged 16 years to 64 years with underlying health conditions which puts them at higher risk of serious disease and mortality included in Table 3 COVID-19 – SARS-Cov-2 chapter 14a of Green Book*
- All those 60 years of age and over
- All those 55 years of age and over
- All those 50 years of age and over
- Further guidance for those under age 50 years not included in the above groups will follow in phase 2.
- Women who are pregnant where the risk of exposure to SARS-CoV2 infection is high and cannot be avoided, or where the woman has underlying conditions that put them at very high risk of serious complications of COVID-19, and only after a discussion between the woman and an obstetrician.
*This also includes those who are in receipt of a carer's allowance, or those who are the main carer of an elderly or disabled person whose welfare may be at risk if the carer falls ill.
The list above is not exhaustive, and clinician should apply clinical judgment to take into account the risk of COVID-19 exacerbating any underlying disease that a patient may have, as well as the risk of serious illness from COVID-19 itself. COVID-19 vaccine should be offered in such cases even if the individual is not in the clinical risk groups specified above, this may be provided under a Patient Specific Direction (PSD).
Category: Exclusion criteria
Description: The vaccine should not be given to:
- Those who have had a previous systemic allergic reaction (including immediate-onset anaphylaxis) to a previous dose of this COVID-19 vaccine
- Those who have had a prior allergic reaction to another mRNA vaccine e.g. Moderna COVID-19 vaccine.
- Those who have had a previous systemic allergic reaction (including immediate-onset anaphylaxis) to any component (excipient) of the COVID-19 vaccine e.g. polyethylene glycol.
- Those with a history of immediate anaphylaxis to multiple, different drug classes, with the trigger unidentified (this may indicate PEG allergy) unless the advice from relevant specialist, local immunisation or health protection team is that vaccination should proceed
- Those with a history of anaphylaxis to a vaccine, injected antibody preparation or a medicine likely to contain PEG (e.g. depot steroid injection, laxative) unless the advice from relevant specialist, local immunisation or health protection team is that vaccination should proceed
- Those with a history of idiopathic (unexplained) anaphylaxis unless the advice from relevant specialist, local immunisation or health protection team is that vaccination should proceed
- Those in whom no valid consent has been received
- Those who are under 16 years of age
- Those with confirmed COVID-19 infection to avoid confusing the differential diagnosis. As clinical deterioration can occur up to two weeks after infection, ideally vaccination should be deferred until around four weeks after onset of symptoms or from the first PCR positive specimen in those who are asymptomatic.
- Those with evidence of current deterioration of COVID-19 symptoms, deferral of vaccination may be considered to avoid incorrect attribution of any change in the person's underlying condition to the vaccine.
- Those who are participating in a clinical trial of COVID-19 vaccines
Those with acute febrile illness – consider postponing immunisation until individual has fully recovered.
Category: Cautions/need for further advice/ circumstances when further advice should be sought from a doctor
Description: The COVID-19 chapter of the Green Book advises that there are very few individuals who cannot receive COVID vaccine. Where there is doubt, rather than withholding vaccination, appropriate advice should be sought from the relevant specialist, or from the local immunisation or health protection team.
The Pfizer BioNTech and Moderna mRNA vaccines contain polyethylene glycol (PEG). PEGs (also known as macrogols) are a group of known allergens commonly found in medicines, many household products and cosmetics. Medicines containing PEG include some tablets, laxatives, depot steroid injections, and some bowel preparations used for colonoscopy. Known allergy to PEG is rare but would contraindicate receipt of mRNA vaccines. It is unclear whether PEG is the only cause of allergic reactions in patients with systemic allergic symptoms after the first dose of Pfizer-BioNTech vaccine.
The rate of anaphylaxis reported to date to the AstraZeneca vaccine is in line with the expected rate of anaphylaxis to non-COVID vaccines. The AstraZeneca vaccine does not contain PEG but does contain a related compound called polysorbate 80. Some people with PEG allergy may also be allergic to polysorbate 80. However, polysorbate 80 is widely used in medicines and foods, and is present in many medicines including monoclonal antibody preparations. Some injected influenza vaccines (including the main vaccine used in over 65 year olds) contain polysorbate 80. Individuals who have tolerated injections that contain polysorbate 80 (such as certain influenza vaccines) are likely to tolerate the AstraZeneca vaccine.
Figure 1 summarises the management of patients with a history of allergy.
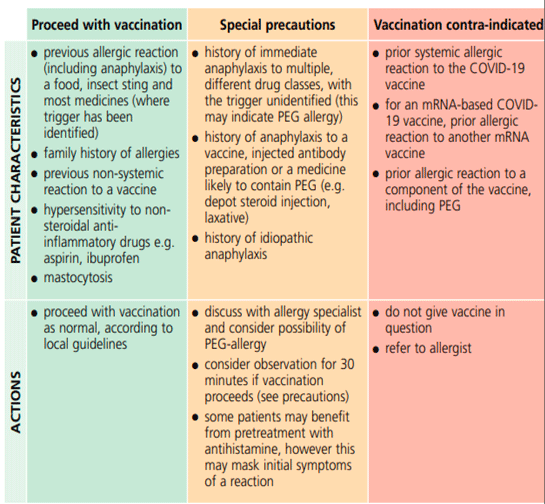
Figure 2 shows the Green Chapter flowchart for managing patients who have allergic reactions to the first dose of COVID-19 vaccine.
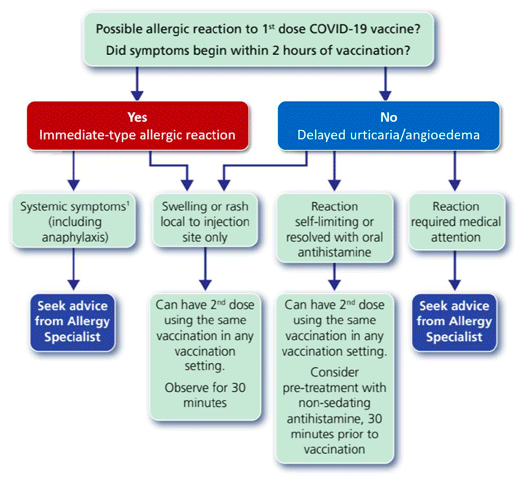
The COVID-19 chapter of the Green Book states individuals with non-allergic reactions (vasovagal episodes, non-urticarial skin reaction or non-specific symptoms) to the first dose of a COVID-19 vaccine can receive the second dose of vaccine in any vaccination setting.
Individuals with a bleeding disorder may develop a haematoma at the injection site (see Route of Administration).
Because of the absence of data on co-administration with COVID-19 vaccines, it should not be routine to offer appointments to give this vaccine at the same time as other vaccines. Based on current information about the first COVID-19 vaccines being deployed, scheduling should ideally be separated by an interval of at least 7 days to avoid incorrect attribution of potential adverse events.
As COVID-19 mRNA Vaccine BNT162b2 is considered inactivated, where individuals in an eligible cohort present having received another inactivated or live vaccine, COVID-19 vaccination should still be considered. The same applies for other live and inactivated vaccines where COVID-19 vaccination has been received first. In many cases, vaccination should proceed to avoid any further delay in protection and to avoid the risk of the patient not returning for a later appointment. In such circumstances, patients should be informed about the likely timing of potential adverse events relating to each vaccine.
Syncope (fainting) can occur following, or even before, any vaccination especially in adolescents as a psychogenic response to the needle injection. This can be accompanied by several neurological signs such as transient visual disturbance, paraesthesia and tonic-clonic limb movements during recovery. It is important that procedures are in place to avoid injury from faints.
JCVI advise there is no known risk associated with giving these types of vaccines during pregnancy. These vaccines cannot replicate, so they cannot cause infection in either the woman or the unborn child.
Although the available data do not indicate any safety concern or harm to pregnancy, there is insufficient evidence to recommend routine use of COVID-19 vaccines during pregnancy.
JCVI advises that, for women who are offered vaccination with the Pfizer-BioNTech or AstraZeneca COVID-19 vaccines, vaccination in pregnancy should be considered where the risk of exposure to Severe Acute Respiratory Syndrome coronavirus 2 (SARS-CoV2) infection is high and cannot be avoided, or where the woman has underlying conditions that put them at very high risk of serious complications of COVID-19. In these circumstances, clinicians should discuss the risks and benefits of vaccination with the woman, who should be told about the absence of safety data for the vaccine in pregnant women.
There is no known risk associated with giving non-live vaccines whilst breastfeeding. JCVI advises that breastfeeding women may be offered vaccination with the Pfizer-BioNTech or AstraZeneca COVID-19 vaccines.
The developmental and health benefits of breastfeeding should be considered along with the woman's clinical need for immunisation against COVID-19, and the woman should be informed about the absence of safety data for the vaccine in breastfeeding women.
Category: Action if excluded
Description: Individuals who are participating in a clinical trial of COVID-19 vaccines who present for vaccination should be referred back to the investigators.
In case of postponement due to acute illness advise when the individual can be vaccinated and ensure another appointment is arranged.
In case of postponement due to COVID-19 symptoms or positive COVID test in the last four weeks advise when the individual can be vaccinated and how future vaccination may be accessed.
Document the reason for exclusion and any action taken in accordance with local procedures.
Category: Action if patient declines
Description: Advise the individual/carer about the protective effects of the vaccine, the risks of infection and potential complications if not immunised.
Advise how future immunisation may be accessed if they subsequently decide to receive the COVID-19 vaccine
Document patient's declined consent and advice given.
2. Description of treatment
Category: Name of medicine
Description: COVID-19 mRNA Vaccine BNT162b2 concentrate for solution for injection
Category: Form/strength
Description: COVID-19 mRNA Vaccine BNT162b2 30micrograms/0.3ml dose concentrate for solution for injection multi-dose vials
COVID-19 mRNA Vaccine BNT162b2 is a multi-dose vial and must be diluted with 1.8mL of 0.9% sodium chloride before use. 1 vial contains 6 doses of 30 micrograms of BNT162b2 RNA (embedded in lipid nanoparticles).
Category: Route of administration
Description: After dilution, vials of COVID-19 mRNA Vaccine BNT162b2 contain 6 doses of 0.3 mL of vaccine. In order to extract 6 doses from a single vial, low dead-volume syringes and/or needles should be used. If standard syringes and needles are used, there may not be sufficient volume to extract a sixth dose from a single vial. Irrespective of the type of syringe and needle:
Each dose must contain 0.3 mL of vaccine.
If the amount of vaccine remaining in the vial cannot provide a full dose of 0.3mL, discard the vial and any excess volume.
Do not pool excess vaccine from multiple vials
Any unused vaccine should be discarded 6 hours after dilution.
COVID-19 mRNA Vaccine BNT162b2 must be administered by intramuscular (IM) injection preferably into the deltoid area of the upper arm. Where administration into the deltoid is not possible the anterolateral thigh can be considered.
Inspect visually prior to administration and ensure appearance is consistent with the description in the manufacturer's product literature or summary of product characteristics.
Individuals with bleeding disorders may be vaccinated intramuscularly if, in the opinion of a doctor familiar with individual's bleeding risk, vaccines or similar small volume intramuscular injections can be administered with reasonable safety by this route. If the individual receives medication/ treatment to reduce bleeding, for example treatment for haemophilia, intramuscular vaccination can be scheduled shortly after such medication/treatment is administered. Individuals on stable anticoagulation therapy, including individuals on warfarin who are up-to-date with their scheduled INR testing and whose latest INR is below the upper level of the therapeutic range, can receive intramuscular vaccination. A fine needle (23 or 25 gauge) should be used for the vaccination, followed by firm pressure applied to the site without rubbing for at least 2 minutes. The individual/parent/carer should be informed about the risk of haematoma from the injection.
The site at which each vaccine was given should be noted in the individual's records.
Category: Dosage
Description: The dose of COVID-19 mRNA Vaccine BNT162b2 is 30 micrograms contained in 0.3mL of the diluted vaccine.
Category: Frequency
Description: COVID-19 mRNA Vaccine BNT162b2 course consists of two separate doses of 0.3ml each, a minimum of 21 days apart.
Operationally, it is recommended that the second dose of all vaccines should be routinely scheduled between four and 12 weeks after the first dose. This will reduce confusion and allow more people to benefit from the protection provided from the first dose during the roll out phase. Longer term protection will then be provided by the second dose.
Individuals who are about to receive planned immunosuppressive therapy should be considered for vaccination prior to commencing therapy (ideally at least two weeks before), when their immune system is better able to make a response. Where possible, it would also be preferable for the 2-dose schedule to be completed prior to commencing immunosuppression. This would entail offering the second dose at the recommended minimum for that vaccine (three or four weeks from the first dose) to provide maximum benefit that may not be received if the second dose was given during the period of immunosuppression.
If an interval longer than the recommended interval is left between doses, the second dose should still be given (preferably using the same vaccine as was given for the first dose if possible). The course does not need to be restarted.
JCVI advises that the second vaccine dose should be with the same vaccine as for the first dose. Switching between vaccines or missing the second dose is not advised as this may affect the duration of protection.
There is no evidence on the interchangeability of the COVID-19 vaccines although studies are underway. Therefore, every effort should be made to determine which vaccine the individual received and to complete with the same vaccine. For individuals who started the schedule and who attend for vaccination at a site where the same vaccine is not available, or if the first product received is unknown, it is reasonable to offer a single dose of the locally available product. This option is preferred if the individual is likely to be at immediate high risk or is considered unlikely to attend again.
In these circumstances, as both the vaccines are based on the spike protein, it is likely the second dose will help to boost the response to the first dose. For this reason, until additional information becomes available, further doses are not required.
Category: Duration of treatment
Description: See Dose and frequency of administration above.
Booster doses of COVID-19 vaccine are not yet recommended because the need for, and timing of, boosters has not yet been determined.
Category: Maximum or minimum treatment period
Description: See Frequency of administration above.
Category: Quantity to supply/administer
Description: Administer 30 micrograms in 0.3mL per administration.
Category: ▼ black triangle medicines
Description: COVID-19 mRNA Vaccine BNT162b2 did not have a UK marketing authorisation at the time this protocol was written and is authorised for temporary supply in the UK in accordance with a Regulation 174 authorisation.
All adverse reactions occurring in individuals of any age after vaccination should be reported to the MHRA using the Coronavirus Yellow Card Scheme. Anyone can report a suspected adverse reaction to the MHRA using the Coronavirus Yellow Card reporting scheme
https://coronavirus-yellowcard.mhra.gov.uk/
Category: Legal category
Description: COVID-19 mRNA Vaccine BNT162b2 is provided temporary authorisation by the Medicines & Healthcare products Regulatory Agency (MHRA) for supply in the UK under regulation 174 and 174A, pending UK marketing authorisation.
The regulation 174 authorised product is categorised as a prescription only medicine (POM).
Category: Is the use out with the SPC?
Description: COVID-19 mRNA Vaccine BNT162b2 is supplied in the UK in accordance with regulation 174 and did not have a UK marketing authorisation at the time of writing this protocol.
As part of the consent process, inform the individual/carer that this vaccine does not have a UK marketing authorisation but has been authorised for temporary supply in the UK by the MHRA and that it is being offered in accordance with national guidance.
The vaccine manufacturer's information for UK healthcare professionals states that the vaccine should be given as a series of two doses (0.3mL, each) 21 days apart. This is superseded by the JCVI advice that the second dose of both vaccines should be routinely scheduled between four and 12 weeks after the first dose. This will allow more people to benefit from the protection provided from the first dose during the roll out phase. Longer term protection will then be provided by the second dose.
Category: Storage requirements
Description: COVID-19 mRNA Vaccine BNT162b2 must be stored frozen at ultra-low temperature in accordance with manufacturer's advice.
Once removed from the freezer BNT162b2 vaccine can be stored for 5 days in a fridge between +2 to +8°C prior to dilution.
NHS Board guidance on Storage and Handling of vaccines should be observed.
COVID-19 mRNA Vaccine BNT162b2 should be diluted as close to use as possible. However, reconstituted vaccine which is not required immediately must be used within 6 hours from the time of dilution and stored between +2°C to +25°C.
The vaccine vial has space to write the date and time of dilution; write this on the vial label.
During storage, minimise exposure to room light and avoid exposure to direct sunlight and ultraviolet light.
In the event of an inadvertent or unavoidable deviation of these conditions, vaccine that has been stored outside the conditions stated above should be quarantined and risk assessed for suitability of continued use or appropriate disposal.
The manufacturer may advise of updated storage requirements and product stability as new data becomes available, vaccine may be stored in accordance with updated recommendations from the manufacturer.
Category: Additional information
Description: Minor illnesses without fever or systemic upset are not valid reasons to postpone immunisation. If an individual is acutely unwell, immunisation should be postponed until they have fully recovered.
There is no evidence of any safety concerns from vaccinating individuals with a past history of COVID-19 infection, or with detectable COVID-19 antibody. Inclusion of antibody positive individuals in the Pfizer phase 3 analysis did not give any safety signals.
Vaccination of individuals who may be infected but asymptomatic or incubating COVID-19 infection is unlikely to have a detrimental effect on the illness. Vaccination should be deferred in those with confirmed infection to avoid confusing the differential diagnosis. As clinical deterioration can occur up to two weeks after infection, ideally vaccination should be deferred until around four weeks after onset of symptoms or from the first PCR positive specimen in those who are asymptomatic.
Having prolonged COVID-19 symptoms is not a contraindication to receiving COVID-19 vaccine but if the patient is seriously debilitated, still under active investigation, or has evidence of recent deterioration, deferral of vaccination may be considered to avoid incorrect attribution of any change in the person's underlying condition to the vaccine.
3. Adverse reactions
Category: Warnings including possible adverse reactions and management of these
Description: Local reactions at the injection site are fairly common after COVID-19 mRNA Vaccine BNT162b2 primarily pain at the injection site, usually without redness and swelling. Systemic events reported were generally mild and short lived. In the final safety analysis of over 21,000 participants 16 years and older, the most common events were injection site pain (>80%), fatigue (>60%), and headache (>50%). Myalgia, arthralgia and chills were also common with fever in 10-20%. Most were classified as mild or moderate. Lymphadenopathy was reported in less than 1%.
In an earlier analysis of around 8,000 recipients, severe side effects, defined as those that interfere with daily activity, included fatigue in around 4% and headache in 2%. Older adults tend to report fewer adverse events following vaccination. This earlier analysis also showed no signal for enhanced disease in vaccine recipients with only 1 case of severe COVID in the 8 vaccine failures at that time.
A protocol for the management of anaphylaxis and an anaphylaxis pack must always be available whenever COVID-19 mRNA Vaccine BNT162b2 is given. Immediate treatment should include early treatment with 0.5mg intramuscular adrenaline (0.5ml of 1:1000 or 1mg/ml adrenaline), with an early call for help and further IM adrenaline every 5 minutes. The health professionals overseeing the immunisation service must be trained to recognise an anaphylactic reaction and be familiar with techniques for resuscitation of a patient with anaphylaxis.
In the event of a severe adverse reaction individual should be advised to seek medical advice.
For full details/information on possible adverse reaction, refer to manufacturer's product literature or summary of product characteristics.
Category: Reporting procedure for adverse reactions
Description: Healthcare professionals and individuals/carers should report suspected adverse reactions to the Medicines and Healthcare products Regulatory Agency (MHRA) using the Coronavirus Yellow Card reporting scheme on:https://coronavirus-yellowcard.mhra.gov.uk/
As this vaccine is labelled with a black triangle, all adverse reactions occurring in individuals of any age after vaccination should be reported to the MHRA using the Coronavirus Yellow Card Scheme. Anyone can report a suspected adverse reaction to the MHRA using the Coronavirus Yellow Card reporting scheme https://coronavirus-yellowcard.mhra.gov.uk/
Any adverse reaction to a vaccine should be documented in accordance with locally agreed procedures in the individual's record and the individual's GP should be informed.
Anaphylaxis is a very rare, recognised side effect of most vaccines and suspected cases should be reported via the Coronavirus Yellow Card Scheme. Chapter 8 of the Green Book gives detailed guidance on distinguishing between faints, panic attacks and the signs and symptoms of anaphylaxis. If a case of suspected anaphylaxis meets the clinical features described in Chapter 8, this should be reported via the Yellow Card Scheme as a case of 'anaphylaxis' (or if appropriate 'anaphylactoid reaction'). Cases of less severe allergic reactions (i.e. not including the clinical features of anaphylaxis) should not be reported as anaphylaxis but as 'allergic reaction'.
Programmatic Adverse Events should be recorded in line with local procedures and where appropriate escalated in accordance with the national framework.
Category: Advice to patient or carer including written information
Description: Written information to be given to individual
- Provide manufacturer's consumer information leaflet/patient information leaflet (PIL) provided with the vaccine.
- Provide copy of Public Health Scotland post- vaccination leaflet
- Provide copy of Pregnant, planning a pregnancy or breastfeeding, a guide to COVID-19 vaccine to women of child bearing years
Individual advice / follow up treatment
- Inform the individual/carer of possible side effects and their management.
- Vaccinated individuals should be advised that it is common to develop a fever after vaccination and that this normally happens within 48 hours after the vaccination and usually goes away within 48 hours. This is a common, expected reaction, and self-isolation and testing for COVID-19 are not required unless the individual has other COVID-19 symptoms; has been told by NHS Test and Protect they are a close contact of someone who has tested positive for COVID-19; they live with someone who has recently tested positive for COVID-19; or they live with someone who has symptoms of COVID-19.
- Vaccinated individuals should be advised that if the fever started 48 hours after the vaccination or lasts longer than 48 hours, they should self-isolate and book a test.
- Vaccinated individuals should be advised that feeling generally unwell, shivery, achy and tired were also symptoms commonly reported by vaccine recipients in the clinical trials. Generally, these symptoms were found to resolve within one to two days without treatment but paracetamol can be taken if necessary to relieve any of these symptoms.
- As has always been recommended, any fever after vaccination should be monitored and if individuals are concerned about their health at any time, they should seek advice from their GP or NHS24
- The individual should be advised to seek medical advice in the event of a severe adverse reaction.
- Inform the individual that they can report suspected adverse reactions to the MHRA using the Yellow Card reporting scheme on: http://yellowcard.mhra.gov.uk.
- Immunosuppressed individuals should be advised that they may not make a full immune response to the vaccine and they should continue to take appropriate measures to protect themselves against this infection.
- When administration is postponed advise the individual how future vaccination may be accessed
- When applicable, advise the individual/carer when to return for vaccination or when a subsequent vaccine dose is due.
Category: Observation following vaccination
Description: Vaccine recipients should be monitored for 15 minutes after vaccination, with a longer observation period when indicated after clinical assessment.
As syncope (fainting) can occur following vaccination, all vaccinees should either be driven by someone else or should not drive for 15 minutes after vaccination.
Individuals with a localised urticarial (itchy) skin reaction (without systemic symptoms) to the first dose of a COVID-19 vaccine should receive the second dose of vaccine with prolonged observation (30 minutes) in any setting.
Category: Follow up
Description: Not applicable
Category: Additional facilities
Description: A protocol for the management of anaphylaxis and an anaphylaxis pack must always be available whenever COVID-19 mRNA Vaccine BNT162b2 is given. Immediate treatment should include early treatment with 0.5mg intramuscular adrenaline (0.5ml of 1:1000 or 1mg/ml adrenaline), with an early call for help and further IM adrenaline every 5 minutes. The health professionals overseeing the immunisation service must be trained to recognise an anaphylactic reaction and be familiar with techniques for resuscitation of a patient with anaphylaxis.
4. Audit Trail/Records
Name: Record/ audit trail
Description:
Record:
- that valid informed consent was given
- name of individual, address, date of birth and GP with whom the individual is registered
- name of person that undertook assessment of individual's clinical suitability for vaccine
- name of person that administered the vaccine
- name and brand of vaccine
- date of administration
- dose, form and route of administration of vaccine
- batch number
- where possible expiry date
- anatomical site of vaccination
- advice given, including advice given if excluded or declines immunisation
- details of any adverse drug reactions and actions taken
- administered under protocol
Records should kept line with local procedures. Ideally records should be kept within the NHS Scotland COVID-19 vaccine administration app.
Local policy should be followed to encourage information sharing with the individual's General Practice.
All records should be clear, legible and contemporaneous.
5. References
Name: Additional references
Description: Immunisation against Infectious Disease [Green Book] https://www.gov.uk/government/organisations/public-health-england/series/immunisation-against-infectious-disease-the-green-book
Immunisation against Infectious Disease [Green Book] COVID-19 https://www.gov.uk/government/publications/covid-19-the-green-book-chapter-14a
JCVI: advice on priority groups for COVID-19 vaccine 30th December 2020
Manufacturer's product information/ Summary of Product Characteristics https://www.gov.uk/government/publications/regulatory-approval-of-pfizer-biontech-vaccine-for-covid-19
Educational resources for registered professionals produced by National Education for Scotland
https://learn.nes.nhs.scot/37676/immunisation/covid-19-vaccines
All relevant Scottish Government advice including the relevant CMO letter(s)