Children and Young People's Mental Health Taskforce: delivery plan
The independent taskforce aims to improve mental health services for young people.
Key Recommendations and Priorities
Audit of Rejected Referrals
The Audit of Rejected Referrals to Child and Adolescent Mental Health Services (CAMHS) was commissioned by the Cabinet Secretary in October 2017 and was undertaken by the Scottish Association for Mental Health (SAMH) and NHS Information Services Division (ISD). The audit provided an opportunity to hear the voices of children, young people and their families.
Some of the material in the report describes a system that does not appear to be joined up and is perceived as unclear and confusing. During the period of the audit, across all Health Boards, nearly 1 in 5 children and young people's referrals to CAMHS were rejected.
The report showed that decisions on rejecting referrals usually happen quickly, with most decisions being made on the basis of paper referrals, without a face to face assessment. While many of the rejected referrals provided signposting to other services, of the 253 people who participated in an online survey of their experiences, just 42% feel they have been signposted. Children, young people and their families reported that signposting is generic, unhelpful and often points to resources they have already explored. Young people whose referral has been rejected often reported a belief that they will not be seen by CAMHS unless they are suicidal or at immediate risk of harm. The report noted that, 'there is a strong indication of a gap in services for children and young people who do not meet the criteria for the most specialist help'.
The report made recommendation for how CAMHS could be improved to resolve the identified issues. The recommendations can be split into four broad categories: further research, meeting the needs of young people and their families, making immediate changes to CAMHS, and improving data collection.
Ministers accepted all of the recommendations in the Audit of Rejected Referrals and commissioned the Children and Young People's Mental Health Taskforce to implement the recommendations.
Annex B lays out how we will help address those recommendations.
Audit Scotland Report
Audit Scotland published their Children and Young People's Mental Health Audit Report on 13 September 2018. The report was critical of current CAMHS services, including structure of provision, data collection and spending commitments. There was also criticism of local and national leadership on children's mental health. The report noted that 'a step change is required to improve children and young people's mental health'. Integration authorities have a major role to play in this change.
The report noted several key concerns around current CAMHS provision. It noted that the Scottish Government's Mental Health Strategy focuses on early intervention and prevention. However, in practice this is limited: mental health services are focused on specialist care and responding to crisis. The system is complex and fragmented, and access to services varies throughout the country.
Audit Scotland found that mental health services for children and young people are under significant pressure. Referrals to specialist services increased by 22% between 2013/14 and 2017/18, and rejected referrals are also increasing. Children and young people are waiting longer for treatment, with 26% waiting over 18 weeks for CAMHS support.
The causes of deteriorating performance in CAMHS waiting times are complex. There is increasing demand for specialist clinical support. There is also pressure on the system through young people being referred to clinical services due to the lack of appropriate pre-clinical support. In some cases we are seeking to medicalise issues that could be dealt with effectively through better support as problems start to emerge. We are seeing some young people referred to CAMHS when a more appropriate service might be centred on specialist neurodevelopmental services.
Rectifying the situation is not straightforward. There is a lack of information available to enable service redesign to take place to improve waits . The report also found that data on mental health services for children and young people is inadequate, and there is a lack of evidence on what difference existing services are making to those who access them. 6% of spending on NHS mental health services is on children and young people, and Boards increased their spending on CAMHS by 11.9% between 2013/14 and 2016/17.
The report concluded that the aims of the Mental Health Strategy will not be achieved unless Scottish Government and COSLA work together with delivery partners to invest in preventative services.
The development of enhanced preventative services will need to involve the workforce currently engaged in CAMHS delivery. Given the pressure on CAMHS as we start that development, additional resources need to be placed in CAMHS teams to help reduce waiting times and the backlog of children and young people awaiting assessment and treatment.
The Taskforce recommends that a significant proportion of the additional £5m allocated to support our work is invested in CAMHS teams to reduce pressure on the system and to support capacity building in early intervention. There should also be investment in some capacity building in prevention and early intervention. This funding should be sustained across the lifetime of the Taskforce and beyond if required.
The shared commitment to improvement
The Scottish Government has made a number of high profile commitments on children and young people's mental health services in the Programme for Government. At a local level there are a number of excellent examples which aim to improve the support for children and young people's mental health. While it is for the Scottish Government and its partners to take forward these commitments, the Taskforce has made the following recommendations on their implementation.
- Invest over £60 million in additional school counselling services across all of Scotland. This will create around 350 counsellors in school education across Scotland ensuring that every secondary school has counselling services. The Taskforce recommends that this new service is integrated with wider services and with other parts of the emerging package of mental health support. The Taskforce's work on generic mental health services can help inform delivery and we will work with education and children's services on this.
- Have an additional 250 school nurses in place by 2022. This will provide a response to mild and moderate emotional and mental health difficulties experienced by young people in the form of local help that is available immediately.
Again the Taskforce will work with the Scottish Government and Local Authorities to provide recommendations around this commitment and recommends that in its implementation it is integrated with wider services.
- Enhance support and professional learning materials for teachers on good mental health, including ensuring that, by the end of academic year 2019-20, every local authority will be offered training for teachers in mental health first aid, using a 'train the trainer' model to enable dissemination to all schools.
This commitment should be underpinned by Getting It Right For Every Child and link to children's services, education and wider mental health and wellbeing support. Where appropriate consideration should be given to extending training to senior phase school pupils.
- Provide more than 80 additional counsellors in Further and Higher Education over the next four years with an investment of around £20 million.
The Taskforce recommends that this new service is integrated with wider services and with other parts of the emerging package of education mental health support. The Taskforce's work on generic mental health services can help inform delivery and we will work with colleges and universities to this end.
- Put in place systems to fast-track those with serious mental illness to specialist treatment
Through the work of our specialist workstreams we will support the Scottish Government and its partners on the delivery of this commitment.
- Develop services for community mental wellbeing for 5-24 year olds and their parents to provide direct and immediate access to counselling sessions, self-care advice, family support, peer-to-peer support and group work with links to other care settings
The Taskforce recommends that this approach should where appropriate be built around the development at scale of community mental health and family hubs which bring a range of mental health support services with wider children and family services. The mental health third sector has a key role to play in delivery as well as primary care and CAMHS specialist in a supportive role. The Taskforce will provide guidance on commissioning as well as assistance to the commissioning process as required.
- Improve the training and awareness of people working with vulnerable families and deliver improved infant mental health support for those families that need them.
Services to improve infant mental health support are a key element of preventative and early intervention mental health services for children. This is an area requiring significant improvement. The Taskforce's specialist and at risk workstreams will work closely with Scottish Government, Local Government and partners on the implementation of this commitment.
- Launch a new website containing trusted help and information for young people and their families.
The Taskforce's knowledge and information workstream will support the implementation of this commitment with input from each of our workstreams. As part of the work of the Taskforce we draw together advice on digitally enhanced services.
- Expand the Distress Brief Intervention (DBI) programme pilots during 2019 to include people under 18. In essence, DBI, is a form of 'listening with empathy and practical problem solving'. It is currently testing with adults to positive effect in Lanarkshire, Aberdeen, the Highlands and the Borders
As this commitment is taken forward the Taskforce recommends that priority should be given to delivering DBIs in primary care settings as these are where many parents and carers would take young people when they show signs of emotional distress.
- Make mental health and suicide prevention training mandatory for all NHS staff who receive mandatory physical health training. This includes doctors, nurses, psychologists, allied health professionals and pharmacists and will help children, young people and adults
The Taskforce will provide advice on this commitment through its generic mental health services and specialist workstreams.
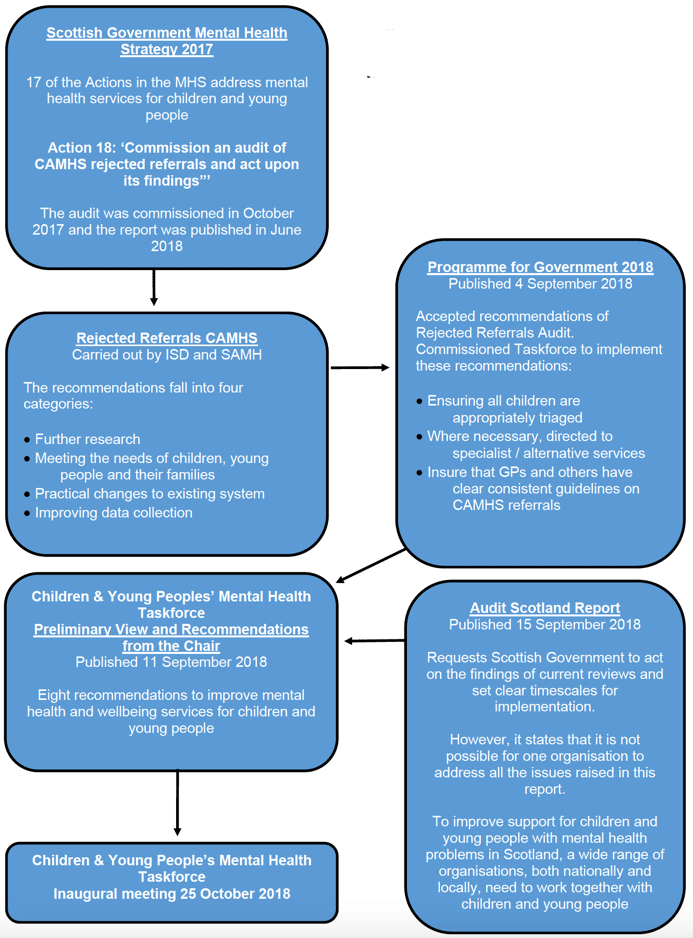
Timeline of recent work on Children and Young People’s Mental Health Services.
Contact
Email: Neil Guy