Beating cancer: ambition and action
Cancer strategy containing more than 50 actions to improve cancer services across Scotland.
8. Living With, and, Beyond Cancer
Our Ambitions
To help people living with, and after, cancer treatment have access to information, advice and support tailored to their individual needs.
To ensure that, by 2021, everyone in Scotland who needs palliative care will have access to it.
As more people are surviving longer as a result of effective screening programmes, earlier diagnosis and better access to advanced treatment techniques and therapies as set out throughout this plan, it is recognised that some individuals will be cured while others will be living with their disease for years, making cancer, or at least some types, a chronic condition.
Our estimates suggest that for every 1,000 people in Scotland, there may be up to 30 to 35 cancer survivors, eight or more of whom may be experiencing significant consequences of their cancer and its treatment.
We already know that a cancer diagnosis has a considerable psychological impact. The disease itself is often associated with fatigue and other physical effects, but also social, financial and relationship issues which may impact on recovery. There are increasing numbers of people living with multiple co-morbidities, of which cancer may be one. Unlike the management of other chronic diseases, cancer treatments - surgery, radiotherapy and systemic therapies - can have unique and sometimes serious short-medium and long-term consequences.
In an effort to improve our survival deficit, we have been rightly focused on early detection, access to high quality treatment and supporting individuals through their treatment. But as we learn from the experiences of those living with and beyond cancer it is no longer acceptable to focus on these areas alone. We now recognise that more needs to be done to improve the quality of life for people who have been diagnosed with and treated for cancer.
Our focus has widened beyond acute treatment and extends to ensure a good recovery from cancer, acknowledging that improvements in survival must be accompanied by a recognition of the ongoing health and wellbeing needs of survivors and, as appropriate, the consequences of their treatment.
As more people are living longer following diagnosis and treatment of cancer, more are experiencing the consequences of treatment or a second primary cancer. It is essential that such consequences are prevented where possible. We will support efforts to identify and appropriately manage those at risk.
No matter how well existing processes are working in support of people with cancer, there is always more that can be done to improve their care. This means listening to the feedback from individuals and carers/families.
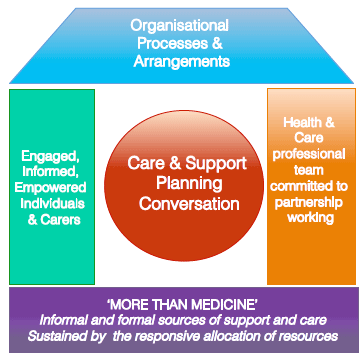
It may require system and organisational change to promote and deliver the roles and skills necessary for true person centred care. Such system change is articulated in models such as the House of Care,[75] which provides a useful representation of the components, all of which are required, to place collaborative, relational decision making and planning at the heart of person-centred care.
In addition, the National Links Worker Programme is working to understand how the primary care team can support people to live well in their community, embedding a dedicated resource - a Link Worker - to make connections between people and sources of support, often drawing upon third sector expertise. When individuals feel supported in their lives, they are more likely to respond to information on ways to improve their health and to live well. If these people are successfully supported sooner rather than later then there is a potential that their risk of developing long term conditions can be reduced.
We also need to ensure that people have the knowledge, understanding, confidence and skills to live well on their own terms and with the health conditions they have. Our health literacy action plan, Making it Easy,[76] sets all of us a challenge as to how we make healthcare simpler and more engaging so that it is responsive, particularly to those with the greatest health literacy needs and those with the least support.
Transforming Care After Treatment
As more and more people are living for longer after a diagnosis of cancer, evidence suggests that their increasingly complex needs are not being met by traditional medically-led follow-up care. It is important that people do not feel a sense of abandonment at the end of treatment.
Work is already well underway, in partnership with Macmillan Cancer Support, through the Transforming Care after Treatment (TCAT) Programme.[77]
We know that people can feel vulnerable and isolated after a period of hospital treatment. We must ensure, through NHS Boards and relevant services, that secondary and tertiary hospital cancer services communicate and work with primary and community health services, social care and our third sector colleagues to ensure the transition from acute care is not only supportive but meets the needs of the individual.
Every individual should know about their treatment and have the information needed to help put them in control of their own care. To do this a co-operative approach is needed across health and social care.
Promoting the adoption of follow-up that is person-centred and risk-stratified, supported by a holistic needs assessment and individual care plan for everyone following their treatment will lead to improvements in the quality of care delivered.
The Scottish Primary Care Cancer Group, with funding assistance from Macmillan Cancer Support, will examine how best to ensure that everyone is given a Treatment Summary so that they are informed about their own care but also so that this can be used in discussion with clinicians and other professionals throughout the course of their ongoing care and support.
The Improving the Cancer Journey[78] experience in Glasgow is an example of how an integrated approach to implementing the components of the Recovery Package[79] across health and social care can lead to an improvement in quality of life, person-led post-treatment rehabilitation and ability to self-manage.
Palliative Care
Palliative care and care at the end of life needs to be responsive to the changing preferences and priorities of people with advanced illness and those of their carers. All health and care workers require an appropriate level of knowledge and skill in palliative and end of life care. Holistic high quality care must be delivered for everyone in accordance with the appropriate legal, professional, clinical and care standards.
It is not just about care in the last months, days and hours of a person's life about enabling someone to live with a life-threatening condition and maintaining as far as possible the quality of life for people living with cancer and their families. As well as controlling pain and other distressing symptoms, it is about helping individuals and their families cope with the emotional upset and practical problems of their situation and supporting them and their friends in their grief and bereavement. The needs here are the same as those of anyone living with a long-term condition. Many people with cancer can benefit from a palliative care approach delivered across health, social care and community settings.
A person's diagnosis or condition significantly influences the care and support they can access, where they are cared for and funding for their support and accommodation. There can also be inequalities in access, treatment and support arising through socioeconomic and educational disadvantage, and associated with particular individual characteristics such as age, ethnic group, religion or belief and sexual orientation. Particular groups in society may also be disadvantaged, such as people who are in prison or who are part of a travelling community. There are also issues when considering the transition to adult services for young people with palliative care, respite and support needs.
In December 2015 we published our Strategic Framework for Action on Palliative and End of Life Care (2015)[80] which sets out how key stakeholders can apply the 'Three Step Improvement Framework for Scotland Public Services'[81] to support improvement in services.
Through the implementation of the Framework will seek to ensure that people:
- receive health and social care that supports their wellbeing, irrespective of their diagnosis, age, socio-economic background, care setting or proximity to death;
- have opportunities to discuss and plan for future decline in health, preferably before a crisis occurs, and are supported to retain as much independence as possible, for as long as possible; and
- know how to help and support each other at times of increased health need and in bereavement, recognising the importance of families and communities working alongside formal services.
Actions - Living With, and Beyond, Cancer
We will work to ensure that every person with cancer is given a Treatment Summary.
- To ensure that there is capacity in our health and social care services to address any unmet needs of people living with and beyond cancer, the three Regional Cancer Networks and the TCAT Programme Board will develop and implement risk stratified person centred follow-up protocols that will reduce unnecessary and ineffective reviews.
- In an effort to improve health and reduce the risk of secondary disease or a second primary cancer, we will ensure that physical activity advice and services (described in the earlier chapter on cancer prevention) are available for people recovering from cancer.
- We will use the National Cancer Patient Experience Survey and the Patient Experience Quality Performance Indicators to help inform us how unmet need is being addressed.
- We will consider the outcomes from the TCAT programme as it progresses and through its evaluation strategy.
- Invest £9 million over 5 years to support access to health and social care services during and after treatment, via for example, Link Workers to provide support in the most deprived communities and initiatives such as Macmillan's Improving the Cancer Journey.
- We will invest £3. 5 million over 4 years to drive improvements across the palliative care sector and to support targeted action on training and education that support the aims of the Framework.
- With some social security powers being devolved to Scotland we will be founding our action on welfare based on treating people with dignity and respect. This includes giving a rounded assessment of people's needs, streamlining the administrative process, and seeking to fast track for those that qualify and are living with a terminal illness such as cancer.
Contact
Email: Helen Stevens